
Category Archives: Uncategorized
Cartoon – Bad Decisions
Health System Mega-Mergers Keep on Coming

I wrote an Industry Insights article last year about large health system mergers
on the heels of the announcement that behemoths Advocate Aurora and Atrium
Health were coming together. That transaction closed in December of 2022
and since then, we have witnessed numerous other “mega-mergers,” creating health systems with
well over $5 billion in revenue.
With the operating environment for hospitals becoming even more challenging, is getting bigger the solution?
Before we answer that though, let’s take a brief look at the large mergers that have occurred over the past few years.
In 2021, Spectrum and Beaumont in Michigan announced they were coming together to create a $15
billion revenue system now known as Corewell Health. Intermountain and SCL Health came together
to create a $15B system; Illinois systems NorthShore University Health and Edward-Elmhurst
Healthcare ($5B); in Pennsylvania, Jefferson Health closed on its merger with Einstein Healthcare
Network ($8B); Piedmont Healthcare + University Health Care + 4 HCA hospitals in Georgia ($5B);
and North Carolina-based Novant Health closed on its merger with New Hanover Regional ($6B).
In 2022, the keynote merger was Advocate Aurora and Atrium Health coming together to create a
$27 billion multi-state system. There were also other sizeable combinations such as the University of
Michigan Health and Sparrow Health ($7B), South Dakota-based Sanford Health and Minnesota-based Fairview Health ($14B), though that merger has since been called off, Wisconsin’s Marshfield
Clinic and Minnesota’s Essentia Health ($5B), and Wellstar Health and August University Health in
Georgia ($6B).
So far in 2023, the most notable is Kaiser Permanente’s acquisition of PA-based Geisinger Health,
which will take the combined system to over $100 billion in revenue. Other mega-mergers include
BJC Health and St. Luke’s Health System in Missouri ($10B), Froedert Health and ThedaCare in
Wisconsin ($5B), and most recently, Oregon Health & Science University and Legacy Health ($7B).
So why are these systems merging?
For starters, there is the benefit of geographic and revenue diversification. Some markets are more
challenging than others, with diversification across a larger footprint helping to balance the combined
systems. Plus, scale allows the systems to more effectively manage risk. With the need to compete
in a value-based care world, health systems must operate in markets that are large enough to be
effective.
Of critical importance, and another key driver behind these mergers, is the enhanced ability to invest
in technological capabilities. It is important to note technology investments cannot be funded through
traditional tax-exempt debt and as technology plays a more important role in the delivery of
healthcare, not-for-profit systems must make investments to remain competitive. AI, data security,
revenue cycle, innovation, information sharing, etc. are all necessary for the successful delivery of healthcare. Furthermore, not every health system can source, invest, or build the right technology on its own. By combining, systems improve upon their ability to lower their per unit cost of investment in technology.
There is also the people. Human talent is a sought-after resource for hospitals these days and the business of running hospitals has
only gotten tougher. Not every health system can attract the best leaders. By merging, health systems can leverage the capability set
from across the organization to more effectively manage the business.
Another reason is the enhanced capital access. As rates rise and lenders tighten standards, bigger is better; and larger balance sheets
with greater assets and security enhances borrowing capabilities. However, capital access does depend on financial performance, so it
requires earnings creation. The jury is still out on the back-office savings created by these mega-mergers, but over time, with effective
leadership, the right technology, and the necessary scale, achieving synergies must be a motivating factor.
But do mergers actually achieve these goals? I have not yet found an independent study to answer this question as many megamergers are recent and there are many variables that influence the analysis. While an n of 1 would not be acceptable to my actuarial
wife, there are examples that show promising signs. In my home state of NJ, the 2016 merger between Hackensack and Meridian is
notable. Leading up to the merger, Hackensack had $1.7 billion in revenue and was averaging 9% operating EBIDA margins, 150 days
cash on hand, and 1x cash to debt. Meridian had $1.6 billion in revenue and was averaging just over 11% operating EBIDA margins,
240 days cash, and 1.4x cash to debt. Post-merger, the combined system now has $6.6 billion of revenue and not taking into the
account the recent swings during and post-COVID, was averaging 11% EBIDA margins, 270 days cash, and 1.6x cash to debt. For the
combined Hackensack Meridian Health System, 1+1 > 2. They have grown faster, plugged weaknesses, improved their balance sheet,
all while continuing to make investments.
There are many reasons why large systems are pursuing mergers and why we expect to see more. And one of these mega-mergers
could create another competitor to the national for-profit operators like HCA or the large catholic systems like Ascension,
CommonSpirit, Providence, or Trinity.
Medicare starts a long road to cutting prices for drugs

Medicare starts a long road to cutting prices for drugs, starting with 10 costing it $50.5 billion annually – a health policy analyst explains why negotiations are promising but will take years.
The Biden administration released on Aug. 29, 2023, a list of the first 10 drugs that will be up for negotiations with pharmaceutical companies over their Medicare prices.
The drugs are purchased through Medicare Part D, a prescription drug coverage program for Americans ages 65 and older. The 10 medications accounted for more than US$50.5 billion in gross costs between June 1, 2022, and May 31, 2023.
Provisions authorizing these negotiations were part of the Inflation Reduction Act which Congress passed in 2022, allowing Medicare to negotiate drug prices for the first time. Pending successful negotiations, these changes would amount to what researchers estimated to be net savings of about $1.8 billion in 2026. The Congressional Budget Office projected an even bigger savings of $3.7 billion.
The top 10 list includes such drugs as Johnson & Johnson’s Xarelto, which treats blood clots, and Amgen’s Enbrel, which treats rheumatoid arthritis and psoriasis.
Negotiations are expected to begin in October and continue until August 2024, with lower prices going into effect in 2026.
Democrats have hailed the new law’s drug pricing provisions as game-changing. They’re likely to make the issue a centerpiece of their 2024 election campaigns. Democrats are further emboldened as public opinion polls show overwhelming support for the policy among Americans.
As a scholar who researches the politics of health policy, I’m skeptical that Medicare drug price negotiations will end up making as big a difference as Democrats have promised, at least in the near future. While U.S. prescription drug prices are excessive, the true potential of the policy is unclear, as it remains muddled in lawsuits and industry opposition. However, if it can withstand the ongoing attacks and become settled law, Americans ages 65 and up could see real financial relief down the line.
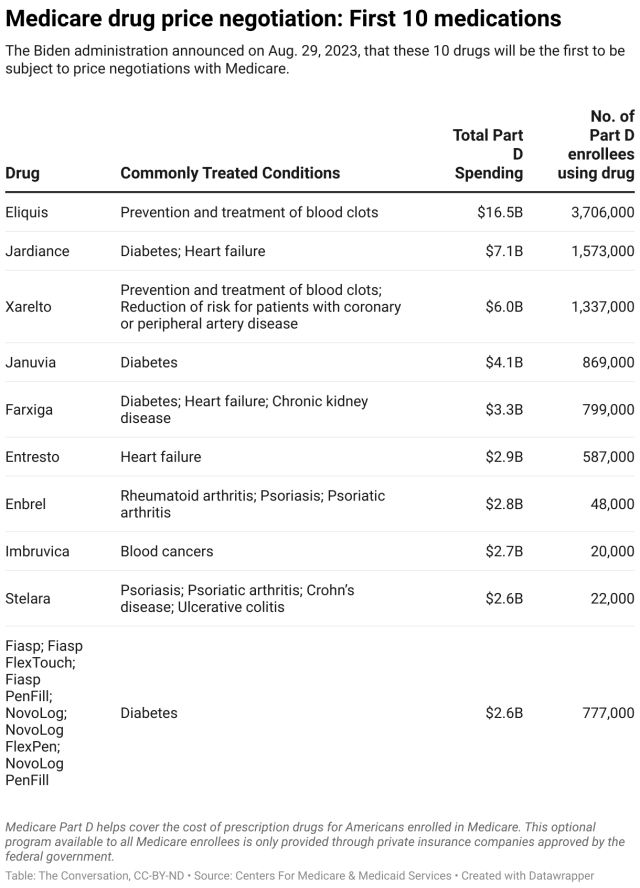
Cutting drug costs for Medicare enrollees
The Inflation Reduction Act allows the Centers for Medicare & Medicaid Services to negotiate prices with the companies that make some of the most expensive drugs in the Medicare program, including life-saving cancer and diabetes treatments like Imbruvica and Januvia.
If the negotiations proceed as planned, the drug-price-negotiation provision is expected to save the U.S. government about $98.5 billion by 2031 by allowing it to pay less on prescription drugs for Americans on Medicare – nearly 66 million people. The Biden administration hopes that these cost savings will be passed down to Americans 65 and older through reduced Medicare Part D premiums and lower out-of-pocket costs.
The Inflation Reduction Act provides additional benefits for older Americans, including limiting their out-of-pocket expenses for prescription drugs to no more than $2,000 annually, limiting the growth of Medicare Part D premiums, eliminating out-of-pocket costs for vaccines and providing premium subsidies to low-income people ages 65 and older.
The Inflation Reduction Act also includes a separate provision that requires drugmakers, under certain conditions, to provide the Medicare program with rebates if drug price increases outpace inflation, starting in January of 2023. That measure is expected to yield $71 billion in savings over a decade.
Penalties for companies that won’t negotiate
The 10 drugs that the Centers for Medicare & Medicaid Services have selected accounted for $3.4 billion in out-of-pocket spending in 2022 for Americans ages 65 and older and $50.5 billion, or about 20%, of total Part D gross prescription drug costs from June 1, 2022, to May 31, 2023.
Pharmaceutical companies have to sign agreements to participate in the upcoming negotiations by October 2023. Based on criteria such as public feedback and consultation, as well as the clinical value of the drug, the Centers for Medicare & Medicaid Services will make an initial price offer in early 2024, with the potential to further negotiate the price until August 2024. Going forward, additional drugs will be subject to negotiations.
If drugmakers don’t negotiate, they will face stiff penalties in the form of a tax, reaching as high as 95% of U.S. pharmaceutical product sales. Alternatively, the companies may pull their drugs from the Medicare and Medicaid markets, meaning that seniors on Medicare would lose access to them.
Why US drug prices are so high
Americans pay substantially more for prescription drugs compared with people who live in countries with similar economies, like Germany, the U.K. and Australia. While Americans spent more than $1,100 a year in 2019, Germans paid $825, the British paid $285 and Australians paid $434 per person.
The reasons for this disparity are multilayered and include the overall complexity of the U.S. health care system and the lack of transparency in the drug supply chain. Of course, many other countries also directly set prices for drugs or use their monopoly on health services to drive down costs.
For example, Dulera, an asthma drug, costs 50 times more in the U.S. than the international average. Januvia, a diabetes drug that is among the first 10 drugs up for price negotiation, and Combigan, a glaucoma drug, cost about 10 times more.
These costs impose a big burden on Americans – 1 in 5 of whom skip at least some of their prescribed medications due to the expense. Those 65 and older are particularly affected by these problems.
Strong resistance
It’s too soon to say how big the impact of the drug pricing provisions will be and whether this policy will be sustained.
Drugmakers have opposed any governmental regulation of drug prices for decades. They are fighting the measure in court and running a public relations campaign that warns of reduced investments in life-saving cures because their financial incentives are reduced.
Even if the drug price negotiations survive the industry’s legal challenges, it’s possible that future Republican administrations won’t embrace or enforce this policy. This is because potential Republican wins in the 2024 presidential and congressional elections could unravel or severely curtail the new drug negotiation policy. Indeed, Republicans have been working feverishly on designing a strategy to use the negotiations against Democrats in the upcoming elections.
Weighing the prospects
In my view, the government’s efforts to cut prices for prescription drugs that Part D enrollees obtain are a step in the right direction. For now, the effect will likely be small because patients already receive discounts on the listed drugs, bringing the net savings down substantially. However, the potential for real savings for Americans ages 65 and older will undoubtedly grow as more drugs become subject to negotiation.
At the same time, drug manufacturers have indicated that they are willing to take their legal battles against the Medicare drug pricing reform all the way to the Supreme Court. If that happens, there’s a good chance they will prevail because the arguments made in their lawsuits are likely to appeal to the Supreme Court’s conservative majority, which has been favorable to many of the arguments made by drugmakers in their lawsuits.
Moreover, drugmakers could also simply pull their drugs from Medicare and Medicaid to force the government’s hand. The Centers for Medicare & Medicaid Services seems to have deliberately chosen drugs that make up a high percentage of manufacturers’ drug sales to counter this possibility. The industry has a history of skillfully exploiting loopholes and possesses a vast lobbying apparatus.
It’s also too soon to know if this is going to be a win for American patients overall. It’s possible that Americans who aren’t covered by Medicare may actually see prices go up. That’s because if drugmakers do make less money on drugs for people enrolled in Part D, they might make up for those lost profits by charging more for drugs that other people depend on.
And lastly, it’s possible that there will be fewer new prescription drugs – as an indirect result of this policy that’s supposed to improve access to health care – because it may reduce drugmakers incentives. While the number of cases is likely small, it would potentially take a toll on patients who might have seen a cure to their disease – or some relief from their symptoms.
Thought of the Day: On Finishing
The Three Major Challenges for Private Equity Investors in Healthcare Services

Healthcare is a capital intense industry: facilities, technologies, workforces, infrastructures and clinical breakthroughs require access to funding from banks willing to lend and investors willing to bet.
For most, being a limited partner in a private equity fund is an attractive hedge against inflation, especially a fund that targets healthcare wherein demand is increasing and shifting, costs are soaring and consumers are receptive to new alternatives.
Private equity is big business:
Private equity funds have nearly $2 trillion in dry powder to invest. The Securities and Exchange Commission (SEC) recently reported that private funds’ gross assets now surpass those of the commercial banking sector at more than $25 trillion–up from $9 trillion in 2012. And the American Investment Council reports that…
· 12 million are employed at Private Equity-Backed Companies.
· 32,041 Private Equity-Backed Businesses have been funded since 2017.
· 34 million Americans Depend on Private Equity to Support Their Retirements.
And healthcare is a prime target:
According to data compiled by Pitchbook, “private equity invested more than $206 billion in U.S. health care throughout 2021 to fund research into deadly diseases like Alzheimer’s and Parkinson’s, expand and renovate facilities, modernize medical records and health care data, and make other needed investments.” Bain reported “Despite the slowdown in healthcare private equity deal flow in the second half of 2022, firms continued to create healthcare-focused funds and raise near-record levels of capital in 2022. Data from Preqin suggests that firms raised more than $15 billion in new buyout capital for funds where healthcare is the exclusive or core focus, which has happened in only two other years in the last two decades—2019 and 2021.”
In 2021, the Medicare Payment Advisory Commission (MedPAC) released a report affirming that private equity investments “play an important role providing hospitals, nursing homes, and physician practices with capital and expertise to navigate an increasingly complex health care landscape” but offered Congress no recommendations about how to navigate its growing role.
The playbook for PE investing in healthcare services is widely-known:
· Thesis: Healthcare is expensive, wasteful and unsustainable in its current structure: Incumbents in healthcare services, especially hospitals and physicians, need capital to survive and are receptive to private money.
· Strategy: Land, Expand, and Exit in 5-7 years: Leverage debt at competitive rates to fund most of the deal; operate aggressively by lowering operating costs; grow revenue aggressively thru adjacency acquisitions and partnerships; price aggressively and avoid compliance penalties associated with safety or quality issues.
· Keys to success: Timing, attractive deal terms, a scalable operating platform, exceptional CEO and dispassionate exit strategy. And for navigating expectations of limited partners (high net worth individuals, pension funds, et al), the General Partner gets a 2% management fee and 20% of the value created in the enterprise at exit.
My take:
For the past decade, PE investments in distressed hospitals, medical specialties (radiology, dentistry, dermatology et al), outpatient surgery/ diagnostic facilities and logistics solutions have been popular targets. Going forward, opportunities in services will increasingly center on business models that produce significant, near-term cost-reduction compared to alternative solutions as issues around affordability and employer health costs mount. But three issues will impact the role and success of PE investing in healthcare services looking ahead:
1-Heightened Regulatory Scrutiny: There’s growing concern in Congress and among regulatory agencies about the role of private equity in healthcare services.
· In Congress and in some states, ownership restrictions and added disclosure requirements are being considered.
· The SEC is advancing changes to require added protections for investors in PE funds.
· The FTC is examining the correlation between PE ownership and business practices and consumer choices.
· CMS is considering analyzing the association between PE ownership and prices.
2-The Maturity Wall: “A maturity wall is fast approaching for PE funds that are nearing the end of their term life to distribute their capital back to investors through exits. PE investors will need to pick up their exit pace or will be confronted with 20% to 26% of the capital initially invested by funds to hit the maturity wall. The cumulative amount of still- held investments could grow to over $360 billion in the next 12 years.” (Pitchbook June 30, 2023). The maturity wall will be especially problematic in communities where medical practices and/ancillary services providers acquired thru PE-sponsored deals are forced to switch owners necessitating possible disruptions in care.
3-Heightened Competition among PE Funds: PE funds compete for good deals and satisfied investors. Bigger funds have advantages over smaller funds i.e., domain expertise, analytic models and access to effective executive talent. The deal landscape in healthcare services has slowed though opportunities remain. It’s a buyer’s market prompting intensified competition between funds and aggressive negotiations between buyers and sellers. Qualified investors are comparing fund performance and moving funds to the most successful.
The healthcare services market in the U.S. is worth $3.5 trillion and is forecast to increase at 5%/yr. for the next decade. It’s traditionally dominated by nonprofit operators and market conditions that favor incumbents over newbies, bigger over smaller and business to business (B2B) models over business to consumer (B2C). That’s changing. Investor-ownership in healthcare services is increasing. Distinctions between privately operated PE owned hospitals and services providers and investor-owned publicly traded operators are being scrutinized by regulators even as the tax-exempt status enjoyed by not-for-profits is under the microscope.
Access to capital that’s cost-effective is critical to the future of health services providers. PE will be increasingly part of that discussion and with it, added risk.







