
Author Archives: henrykotula
Cartoon – Feeling Better
The Bill That Never Ends

Even with insurance, millions of Americans with serious illnesses are trapped in a cycle of deductibles, debt collectors and annually resetting medical bills.
Jeni Rae Peters was a single mother and mental health counselor in Rapid City, South Dakota, when she was diagnosed with stage 2 breast cancer in 2020. She had health insurance through her employer. She kept working through surgery and chemotherapy because she knew that losing her job meant losing her coverage, and losing her coverage meant losing everything.
As KFF Health News reported in its landmark “Diagnosis: Debt” investigation, the bills came anyway. Her deductible and out-of-pocket limit reset every Jan. 1 — as they do for most health plans. When she switched jobs and her insurance changed, the clock reset again. In 2021 it reset once more, and when she slipped on the ice and broke her wrist — a fracture likely made worse by chemotherapy that had weakened her bones — she was charged thousands more. Surgeries, radiation and chemotherapy left her with at least $30,000 in debt. She couldn’t tell you exactly how much she owed anymore. The bills kept coming.
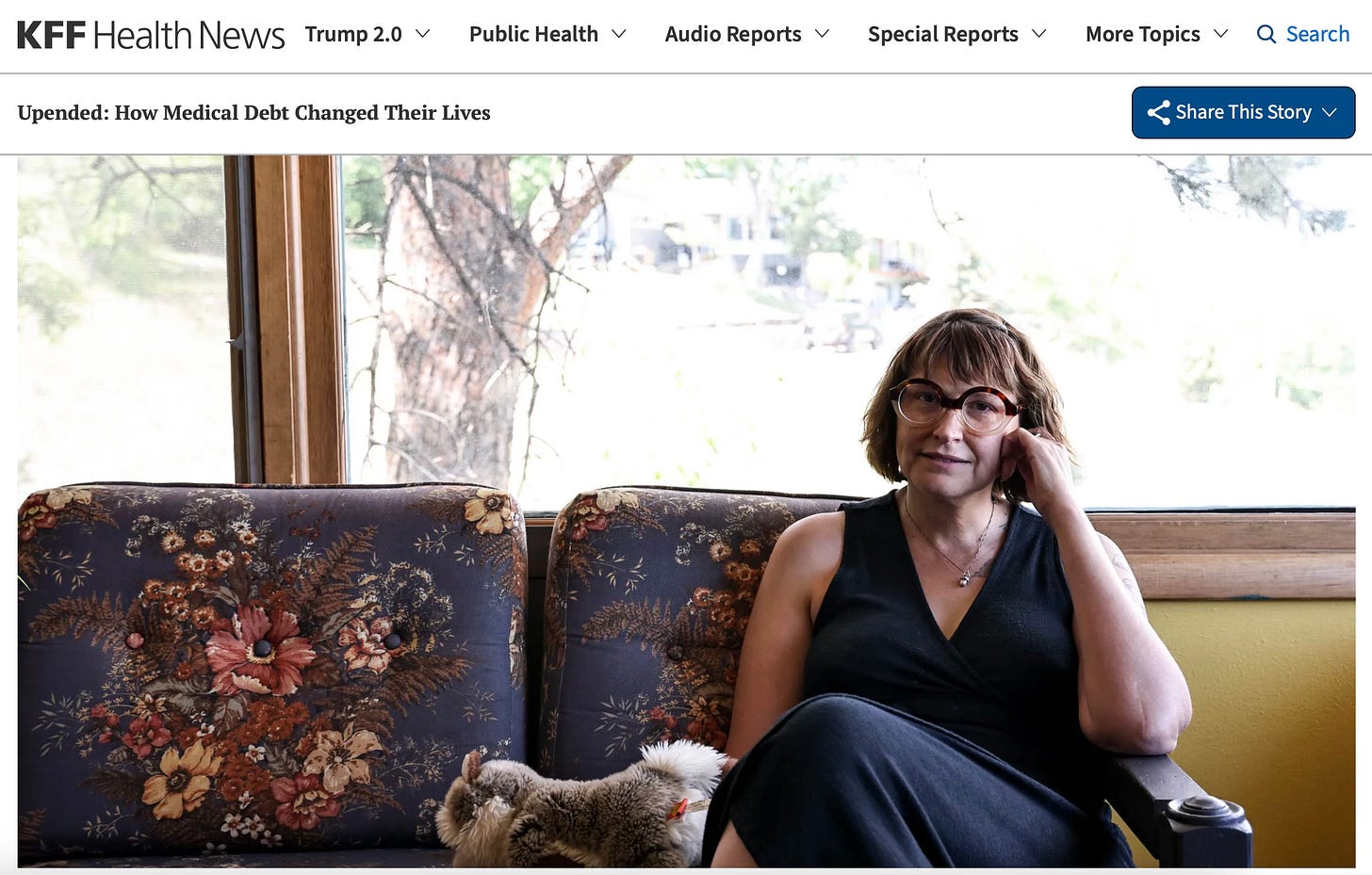
One of the debt collection calls came while she was lying in the recovery room after her double mastectomy. She was still half-delirious from anesthesia. She thought it was her kids calling. It was someone asking her to pay a medical bill.
Jeni Rae Peters’ story is not unusual. In the brutal current version of American health insurance, it is practically routine.
A 2024 survey by the American Cancer Society Cancer Action Network found that nearly half of cancer patients and survivors — 49% — have incurred medical debt to pay for their cancer care, with another 13% expecting to incur debt as they begin or continue treatment. We’re not talking about uninsured Americans here. In fact, nearly all of them — 98% — had health care coverage at the time they accumulated that debt. What they had in common is that most of them were enrolled in a high-deductible health plan.
Having insurance, in other words, did not protect them. In many cases, the insurance plan itself was the mechanism of their financial destruction.
Over the past two decades, the insurance industry — with the quiet approval of employers eager to cut their own costs — systematically shifted financial risk onto patients. The gears of the mechanism are familiar to anyone who has ever tried to read an Explanation of Benefits: deductibles, copayments, coinsurance, out-of-pocket maximums. These instruments were designed, in theory, to discourage unnecessary care. In practice, they have become a second billing system — one that activates precisely when a person is most sick, most frightened and least equipped to fight back.
The numbers have grown staggering. The average deductible for a single worker in employer-sponsored coverage now exceeds $1,700 — and that figure masks the reality for workers at smaller firms or in lower-wage jobs, where deductibles of $3,000, $5,000 or more are common. The Affordable Care Act limits the amount of money Americans with commercial insurance have to pay out of pocket, but the cap was unreasonably high from the start, it increases every year – and it resets every year. This year the out-of-pocket maximum is $10,600 for an individual and $21,200 for a family. For a cancer patient like Jeni Rae Peters, hitting that cap wasn’t a worst-case scenario. It was the first-year scenario. And then the calendar flipped to Jan. 1. And it all reset.
This is the particular cruelty that most Americans don’t fully understand until they get sick: the out-of-pocket maximum isn’t a lifetime protection. It’s an annual one. Every January, the counter goes back to zero. The deductible resets. The coinsurance begins again.
For someone managing cancer — or diabetes, or multiple sclerosis, or heart disease — this isn’t a one-time financial hit. It’s a recurring one, year after year, for as long as the disease persists. Oncologists have a term for it: financial toxicity. The treatment harms the body. The bills harm everything else.
The harm is measurable and well documented. Among cancer patients who accumulate medical debt: 60% are unable to put money into savings; 49% have their credit score damaged; 46% report being harassed by creditors and debt collectors. Eighteen percent consider filing for bankruptcy. Six percent actually do. Eight percent lose their home or are forced to live somewhere they don’t feel safe.
Researchers have also found that cancer patients who go bankrupt are more likely to die than cancer patients who don’t. Financial toxicity is not a metaphor. It is a cause of death.
There is a philosophical argument, still advanced in insurance industry testimony and in certain policy circles, that requiring patients to pay something for care makes them more cost-conscious consumers. I used to help make that argument when I was an insurance industry communications executive. It is one of the things I regret most about that career.
What that argument leaves out is that no one rations chemotherapy because it seems unnecessary. No one decides their insulin isn’t worth the cost because they’re being “judicious.” The cost-sharing model punishes the sick for being sick. It was designed to shift costs, not to improve health. And it has worked spectacularly well for health insurers. Forcing health plan enrollees to pay hundreds and often thousands of dollars out of their own pockets before their coverage kicks in enables insurers to pay far fewer claims today than they did before they began pushing Americans into high-deductible plans two decades ago.
In the coming weeks, I’m going to tell more stories like Jeni Rae Peters’. I’ll be writing about what’s happening to people who buy coverage through the ACA Marketplace and discover that “covered” doesn’t mean what they thought it meant, about how our employers have become the primary architects of most Americans’ financial exposure when they get sick, and what we can do about it.
It’s The End of the Independent Hospital. Here’s What Comes Next for Community Care

An unforgiving financial climate is forcing many community hospitals to choose between preserving independence and pursuing consolidation. But the path forward doesn’t have to be strictly binary.
KEY TAKEAWAYS
The financial pressure facing community hospitals is driven by widespread underpayment that makes sustaining independence difficult.
Consolidation can provide stability, but it often brings higher costs, workforce disruption, and reduced local control over decision-making.
Hospitals that act early have more strategic options, while delayed action leads to fewer choices and diminished leverage in shaping their future.
Independent hospitals have survived reimbursement cuts, labor shortages, and waves of consolidation before. But according to the executives in this month’s HealthLeaders cover story, this time may be different.
In a sweeping look at the financial and political pressures reshaping healthcare, our CEO editor Jay Asser examines why leaders at independent and regional health systems increasingly believe the traditional hospital business model is reaching its breaking point.
The story features candid conversations with Russ Ranallo, CFO of Owensboro Health; Pat Charmel, President and CEO of Griffin Health; Scott Rathgaber, MD, CEO of Emplify Health; and longtime healthcare executive Peter Wright, all of whom argue that the combination of Medicaid cuts, collapsing public trust, political gridlock, and rising operational costs is forcing hospitals into a new era of survival.
Their message is blunt: the old playbook no longer works.
For decades, hospitals found ways to absorb federal payment reductions through cost-shifting, consolidation, and commercial payer leverage. But as Jay reports, leaders now say those escape valves are closing all at once. Rural and independent systems are confronting impossible math, policymakers are demanding accountability without offering solutions, and communities still expect hospitals to provide care regardless of financial reality.
The story dives into the uncomfortable questions many executives are now asking privately:
- Is fee-for-service finally collapsing under its own weight?
- Have hospitals lost the political and public trust needed to defend themselves?
- And if the current model is no longer sustainable, what replaces it?
Forget reimbursement cuts. Now the conversation centers around whether independent hospitals can survive the next decade at all.
Read the full cover story to see why healthcare leaders say the industry is heading toward a reckoning it can no longer avoid.
Congress, Hospital CEOs Clash Over What’s Behind Rising Costs

At a House Ways and Means Committee hearing, lawmakers targeted pricing and market power while executives pointed to cost pressures and reimbursement gaps.
KEY TAKEAWAYS
House Ways and Means Committee members cast hospitals as central figures contributing to increased costs for patients.
CEOs from major health systems highlighted labor costs, Medicare Advantage delays, and uneven reimbursement.
Ongoing disconnect between lawmakers and hospital leaders continues to affect affordability policy and provider strategy.
A hearing before the House Ways and Means Committee brought hospital finances into focus as lawmakers questioned the drivers of healthcare spending and health system CEOs described the reality facing providers.
The discussion centered on pricing, profit margins, and consolidation, with members of Congress pressing for accountability, while CEOs of HCA Healthcare, CommonSpirit Health, New York-Presbyterian, and ECU Health pointed to cost pressures and reimbursement challenges impacting business decisions.
Though both sides agreed that rising costs remain a significant issue, the hearing illustrated a divide in how those costs are understood. That tension continues to influence both policy proposals and provider strategy as the debate over affordability moves forward.
Committee chairman Jason Smith, R-Mo., opened the hearing by comparing hospital profitability with major corporations and tying that performance to what patients pay for care.
“Hospitals with more than 100 beds have a higher profit margin than Delta Air Lines, Target, or Disney,” Smith said. “Turns out charging an arm and a leg for health care is more lucrative than the Happiest Place on Earth.”
Smith placed responsibility on the entire healthcare system and highlighted insurers, which also faced the committee in January, but stressed that hospitals must answer for their role.
“This committee isn’t interested in hearing about how the high prices your businesses charge are someone else’s fault,” Smith said. “The blame game didn’t work with insurers, and it won’t work today. Simply put, hospitals are charging an insane amount for care. Hospital prices have skyrocketed 300 percent in just over two decades – more than any other sector of our economy.”
That line of questioning reflects a growing focus in Washington on hospital pricing as a central factor in affordability, and a push to rein in price increases through policymaking.
During the hearing, lawmakers raised concerns about the impact of consolidation on negotiated rates, the role of large systems in shaping local markets, and the degree to which higher commercial prices ripple through employers and households.
Executives described a more complex financial picture that extends beyond headline margins.
Sam Hazen, CEO of HCA, acknowledged elements of the committee’s concerns while emphasizing that hospital reimbursement varies widely based on factors like patient mix and acuity.
“There are certain aspects of your discussion here that have merit,” Hazen said. “I think there’s also merit to the hospitals receiving a premium in certain circumstances, so we would be more than willing to work with you on that.”
Payment friction emerged as a recurring theme, particularly in relation to Medicare Advantage. Wright Lassiter III, CEO of CommonSpirit, pointed to delays and denials as a source of strain for large nonprofit systems.
“Medicare Advantage plans are the most challenging today,” he said. “We have $4.3 billion in unpaid Medicare Advantage claims, with nearly $1 billion of that being more than 150 days past due for care that CommonSpirit has delivered to patients and communities that you represent.”
The conversation also turned to consolidation and access in regional markets. Michael Waldrum, CEO of ECU Health, described consolidation as a response to shifting market dynamics rather than a strategy aimed at expanding pricing leverage.
“Consolidation in our market is not driven by preference, it is how we survive,” he said. “As some exit and others enter with profit-driven agendas, systems like ECU Health are left to serve as a safety-net. The result is reduced access, worsening outcomes and increasing costs.”
A statement submitted by the AHA for the hearing reiterated the current pressures facing hospitals, but noted an effort to reduce the cost of care by “improving efficiency, embracing innovative technologies and redesigning how services are delivered.”
The AHA called on insurers, purchasers, drug and supply manufacturers, and policymakers to work together with hospitals on four key areas of the healthcare system: improving the health of individuals and communities, advancing value through care transformation, reducing regulatory and administrative waste, and innovating to improve care quality and outcomes.
However, the gap between how lawmakers view hospital pricing and how health system leaders contend with rising costs and uneven reimbursement continues to limit alignment on policies aimed at improving affordability.
Fixing a System That Can Deny Health Coverage: Miranda Yaver on Insurance Reforms (Part II)

“Comprehensive health insurance reform really needs to happen at the federal level.”
Last issue we shared the first part of my Q&A with Miranda Yaver, author of the new book Coverage Denied: How Health Insurers Drive Inequality in the United States, where we discussed the ins and outs of health insurance coverage denials and how we ended up with such a system.
In part two of our conversation below, we discuss potential reforms and policy solutions and how to achieve them.
Miranda is a health policy professor at the University of Pittsburgh and was the Roosevelt Institute’s 2025 author-in-residence.
Stephen Nuñez: You wrote the book before HR1 (the “One Big Beautiful Bill Act,” or OBBBA) was passed. There are myriad ways this bill will make health care worse for people. Is there anything that you’re particularly focused on, given your research into the causes and consequences of this (quasi-)managed-care system we seem to have backed ourselves into?
Miranda Yaver: In addition to the broad coverage losses and increases in administrative burdens associated with enrolling and staying enrolled in health insurance, a couple of things happened. First, with the expiration of the enhanced premium tax credits, those with Affordable Care Act (ACA) marketplace insurance saw their premiums jump up dramatically. That means denials of coverage that do arise may be more harmful because people have less financial wiggle room with which to get creative with stopgap measures.
With both premium increases and new administrative complexity around eligibility verification, there’s also greater potential for patient churn among health insurers, which creates a setting that can lead to myopic coverage decisions from insurers who feel they can pass the buck rather than make up-front investments in patient health. For example, an insurer might deny coverage for a diabetic’s continuous glucose monitor with the expectation that by the time the patient faces costly complications from poorly managed glucose, they’ll be with another insurer.
I think whenever we’re introducing new fiscal pressures in the insurance market, we need to worry about private insurers turning to prior authorization as one way to make up some of that financial deficit.
Stephen: I was joking on social media the other day that if you ask an ordinary person about the American Medical Association (AMA), you’re likely to get positive comments (“doctors are the good guys!”), but if you ask a social scientist you might get a tirade or perhaps a hissing sound. The AMA has since the time of President Franklin D. Roosevelt worked to prevent the expansion of “socialized medicine” and has been a large lobbying barrier to several attempts over the decades to expand public insurance and push industry reform. And yet pre-authorization (and post-procedure coverage denial) undermines doctors’ autonomy and bandwidth in ways that seem to really irk them. Politics can make strange bedfellows, so I’m wondering if you see any fruitful avenues for collaboration with the AMA on this issue?
Miranda: I think that’s absolutely right, and in Coverage Denied, I certainly highlight both perspectives: In chapter one, I walk through the political origins of prior authorization and its entrenchment. It’s hard to talk about the origins of this managed-care tool without reflecting on the yearslong outcry over socialized medicine, but I also highlight the AMA’s more contemporary work around prior authorization and physician burden reduction, as well as broader issues of professional autonomy. The AMA’s physician surveys call attention to the sweeping impact (or at least, perceived impact) of prior authorization—from time and staffing demands to adverse effects on patients. The organization has also led the charge in advocacy and model legislation to do things like regulate the qualifications of reviewing physicians, promote transparency concerning prior authorization requirements, require more timely processing, and reduce the volume of prior authorizations. None of those issues address the broader philosophical objections to prior authorization—that is, that health coverage decisions are being made by companies with fiduciary responsibilities to shareholders rather than by treating physicians—but they do reduce the extent to which patients and their physicians are dealing with the constant headaches of these processes.
The AMA rightly frames these prior authorization headaches as sources of physician burden and burnout. Even if physicians might prefer to do away with prior authorization, and even though promoting transparency and timeliness won’t necessarily result in fewer denials, these reforms could take the guesswork, “black-box” feeling out of prescribing. In turn, physicians could more easily assess whether and when to move on to a plan B rather than endure the protracted delays common under the current system. Regulation of the qualifications of reviewing physicians could (at least on the margins) reduce the odds of erroneous denials that reflect lack of familiarity with more recent treatment protocols outside a doctor’s field of specialty, and which necessitate burdensome appeals to rectify. And even in this highly polarized and gridlocked political climate, some of these measures are passing at the state level with unanimous or near-unanimous support.
But this does not disrupt the reliance on prior authorization or confront the philosophical objections. A larger-scale intervention into this facet of the US health-care system would require more sweeping health reform from Congress than is feasible in the foreseeable future given *gesticulates wildly at the world.* Although the AMA continues to oppose single-payer, over the decades they have become more conciliatory toward issues of health coverage expansion and now support a public option. A public option would certainly move our health insurance system forward because private health insurers (which have been heavily reliant on prior authorization, delays, and denials) would have to compete with a government plan. Still, my money is very much on single-payer—which would extract the profit focus—for delivering the most relief for those in need of health care. But politics is complex and often much more a dynamic of incrementalism than waving a magic wand, and I’m a big believer in moving the needle where we can and when we can, even if the bigger philosophical issues of health insurance delivery will have to wait a few years.
My money is very much on single-payer—which would extract the profit focus—for delivering the most relief for those in need of health care.
Stephen: So we have path dependence, we have a health-care system that is for-profit and generates poor outcomes (for hospitals, doctors, patients, even insurance companies alike), we have a host of actors, and we have the complexities of federalism on top of that. Things feel pretty dire! What are some things we could do at the state and/or federal level to solve or at least mitigate the problems you detail in the book?
Miranda: One area where states have begun to take action is the role of AI, which health insurers are increasingly using to bulk-process claims and prior authorizations. California’s SB 1120, which went into effect this year, stipulates that when insurers’ AI programs recommend denials, they must be reviewed by physicians in the appropriate specialty. These technologies are advancing faster than regulatory oversight tools can keep up with, and unlike the relatively low-stakes penalty assessed when, say, a student uses AI for a paper and hallucinates a citation, when AI programs get health coverage decisions wrong, the consequences can be dire. And especially amid the ongoing litigation against Medicare Advantage plans’ use of AI to deny (with reversal rates of 80–90 percent), this could be a valuable shift.
When AI programs get health coverage decisions wrong, the consequences can be dire.
Some states are doing things that I’m not as fond of: Gold card laws, under which physicians who secure around 92 percent or more approval for their prior authorizations become exempt from these processes. It sounds good at face value, but it’s really replacing one form of physician burden with another because it’s assessed at the plan-service level, such that one might have a wallet full of gold cards to keep track of—a gold card for head CT scans with Aetna and abdominal CTs with Cigna, and so on. Texas’s law was so restrictive that just 3 percent of physicians qualified as “high performing” under its terms, so its impact has proven quite limited.
There are other options worth thinking about that are highly feasible and don’t require revisiting big philosophical questions about the US health care system. For example, plain-language rules in health insurance communication could help prevent patients from falling through the cracks due to complex and technical explanations of denials and appeal processes. The average American adult reads at around the 8th grade level, but most health insurance materials are written in at least the 10th grade level. Lower-income and lower-educational attainment patients and non-native English speakers are especially vulnerable in this system. This would also be relatively simple to administer and enforce. The Washington State Office of the Insurance Commissioner is a great model of guiding patients through appeal processes—from an accessible YouTube video to template appeal letters for different types of denials. Of course, this doesn’t address the propensity to deny in the first place, but it can mitigate the ensuing patient burden.
It would also be relatively feasible for states to limit prior authorization’s application to only domains of health care where there are at least relatively recent evidence bases of abuse or overprescribing. All too often, prior authorization is applied to areas of medicine where this overuse is not a documented concern. Lower lumbar spine MRIs are a commonly cited example of overprescribing, such that health insurers will often require a few weeks of physical therapy before being able to proceed with the scheduling of the MRI. That might not necessarily be an inappropriate use of prior authorization, whereas applying this process to a drug like PReP is far less logical, since it is life-saving and there is no evidence of abuse. States could, at the least, require insurers to justify the use of prior authorization for these types of procedures with data and evidence.
At the federal level, the House of Representatives approved by a voice vote the Improving Seniors’ Timely Access to Care Act in 2022, but despite bipartisan support, the legislation died in the Senate. This bill was centrally aimed at streamlining existing prior authorization requirements. It would require Medicare Advantage plans to deliver timelier decisions through electronic processes. This wouldn’t increase the odds of approval, but it would mitigate delays before either initiating appeal or moving on to a plan B.
In the background of all of these state efforts is the reality that state reforms cannot touch the majority of employer-sponsored health insurance plans. This quirk, which deviates from the federalism embedded into so many other areas of health policymaking and beyond, is due to the constraints of the Employee Retirement Income Security Act (ERISA). ERISA preempts state laws that “relate to” self-insured health plans, which cover most workers in employer-sponsored insurance. Because of the limits of what states can do to move the needle on equitable coverage, comprehensive health insurance reform really needs to happen at the federal level, which presents obvious challenges in the current political environment.
Because of the limits of what states can do to move the needle on equitable coverage, comprehensive health insurance reform really needs to happen at the federal level.
Stephen: Cost control/overutilization is a fundamental problem, even if the way the US “solves” for it is particularly awful. I can think of a variety of ways single-payer public health insurance helps: no insurance churn so no short-termism; deductibles, copays, and coverage are subject to a democratic process; and the government has monopsony power to negotiate down provider rates. And yet the fee-for-service conundrum and responses to it still exist in other countries with models closer to single-payer.
Are there any models or policies from the international context that you find promising, even if not politically feasible in the US right now? I’m thinking of things like New Zealand’s no-fault compensation system for medical injury, which means doctors don’t have to run tests simply to avoid lawsuits, or Pay-for-Performance/Value-Based Care models that could base payment on health-care outcomes and not just volume of services.
Miranda: My work is very US-centric, but I’ve grown increasingly interested in Switzerland. Even though traditional Medicare is immensely efficient, spending vastly less on overhead than do private insurers, Americans largely maintain the perception that the private sector is comparatively more efficient in policy delivery. That constrains our political choices (though this preference is becoming weaker over time, as more Americans are open to a government-run system). Given this underlying preference, are there ways that we can make private health insurance work? I think Switzerland shows that the answer is “yes, but.”
Even though traditional Medicare is immensely efficient, spending vastly less on overhead than do private insurers, Americans largely maintain the perception that the private sector is comparatively more efficient in policy delivery.
The Swiss health insurance system is actually more privatized than ours, and like our system, there’s a great deal of decentralization across localities. Where it diverges is its coupling of privatization with significant regulation as opposed to a broader embrace of free-market principles. The Swiss are legally required to be insured (though they have many options from which to choose), and on top of the standard but comprehensive insurance package, people can purchase supplemental private insurance to fill in any gaps or gain access to better hospital accommodations (e.g., a private room) or to see additional health-care providers. Consequently, nearly everyone in Switzerland is insured. In contrast with the relatively consolidated insurance market we have—with UnitedHealthcare, Cigna, CVS Health/Aetna, Elevance, Centene, Humana, and Kaiser Permanente dominating the markets, especially in certain regions—the Swiss have 56 insurers from which to choose. But the Swiss government exerts considerable regulatory oversight over both quality and prices.
So, you’ve got nearly universal coverage, market competition, regulation of pricing so as to mitigate exploitative charges to patients and the system writ large, and privatization. But all of these elements are in combination with enough regulation that you’d be unlikely to run into the insurance barriers that are such a dominant American experience and that make up the focus of my book.
The challenge, of course, is that to get this better coverage (which unsurprisingly produces better health outcomes), the Swiss both accept a higher tax rate than US politics tends to find palatable, and they accept the insurance mandate (whereas there was public consternation, driven by conservative political leaders, over the ACA’s individual mandate). To be sure, Americans’ attitudes could shift: We’ve certainly seen significant growth in support for the ACA, and the share of Americans who see it as the federal government’s responsibility to ensure health-care access has increased significantly over recent years. To the extent that these trends continue, that could facilitate a broader menu of health reform options.
But there are also some questions about scalability given that Switzerland has roughly the same population as New Jersey, is quite homogeneous, and invests more broadly into addressing social determinants of health. All too often in the US, we ignore those social determinants, which are truly in the driver’s seat of our health, while pouring money at health-care delivery. This leaves us with high health spending but a suboptimal return on investment. Switzerland can serve as some inspiration to right-size US reliance on private industry, though the extension may be difficult amid political preference for lower tax rates and deregulation.
Stephen: Is there anything else we haven’t discussed that you’d like to highlight?
Miranda: One elephant in the room amid discussions of health insurance barriers—their proliferation and their persistence—is why health insurers have been able to remain so largely unaccountable. At least part of this answer comes back to ERISA. To begin with, it preempts states’ efforts at comprehensive coverage reforms. This means that when political conditions aren’t well-suited to federal reforms, while we can often turn to the states to advance progress where they can, ERISA prevents comprehensive prior authorization reforms or the broader reduction of administrative burden in insurance. Further, it denies meaningful legal recourse to patients enrolled in self-insured health plans, which is about two-thirds of covered workers. Under ERISA, denied patients cannot obtain monetary damages (e.g., punitive damages, or damages for pain and suffering) and attorney’s fee recovery is left to the discretion of the judge. All that patients are entitled to receive is the benefit owed, which may be cold comfort to someone whose condition has worsened. And needless to say, less affluent patients will be risk-averse in taking legal action with this vulnerability to being left to cover their own legal costs.
The lack of meaningful remedies is where it becomes really clear that health care was an afterthought in ERISA, which was motivated by pension concerns. If your employer tries to screw you out of your pension, you can sue and get your pension back, but health conditions can change and make this enforcement apparatus ill-suited. Further, lawyers will likely be reluctant to take on cases that lack a monetary value. And if insurers know that patients are especially unlikely to sue insurers under these conditions, effective control over these entities can be harder to come by because wrongful denials are virtually costless. So, ERISA’s denial of meaningful remedies for wrongful coverage denials can not only be harmful to the patients when such denials arise, but insurers may have less incentive to exercise caution when deciding whether to cover costly care because they won’t face a meaningful penalty. In the worst case scenario for them, they eventually cover the treatment if the patient challenges the denial, which they rarely do. This design can thus increase the probability that insurance barriers arise in the first place. Congress tried to fix this problem in the late 1990s with the Patients’ Bill of Rights, but it didn’t come close to enactment. That bill is a critical issue for legislators to revisit. I’m currently writing another book that looks squarely at what accounts for the entrenchment of this feature of our health insurance system and the ways it disrupts equitable access to health care.
When Health Insurers Decide: Miranda Yaver on Coverage Denials (Part I)
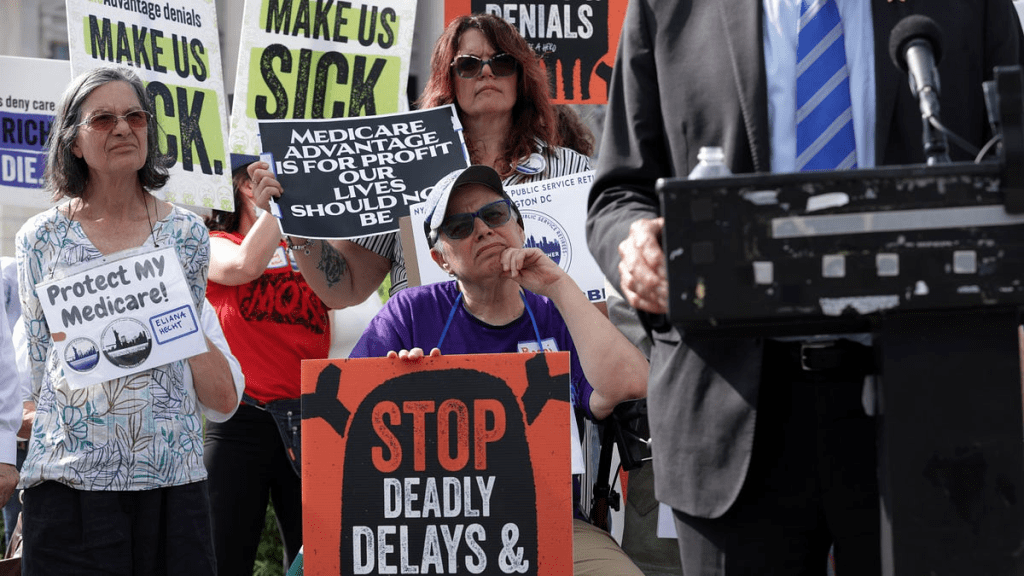
“There are more ways people can be denied by their health insurer than they realize.”
It’s not news to any of us that the US health insurance system needs massive change. The sheer scale of administrative and financial burden on patients and providers is untenable. I spoke with Miranda Yaver about her research on one underdiscussed aspect of the insurance maze: coverage denials.
Miranda is a health policy professor at the University of Pittsburgh and was the Roosevelt Institute’s 2025 author-in-residence. Her book Coverage Denied is out today, April 23, from Cambridge University Press.
Health insurance coverage denials and how they affect patients
Stephen Nuñez: In my own recent research on health-care policy, I detailed the consequences of our broken system for patients: medical debt, bankruptcy, and delayed or forgone treatments that often lead to worse health outcomes down the road. I focused on some of the better-known aspects of American health care, like underinsurance through high premiums, high deductibles, co-pays, and gaps in coverage (such as being between jobs).
In your new book, you focus on another aspect of the health-care system: denial of coverage among people who think they are insured against injury and illness. Could you explain the different ways this plays out?
Miranda Yaver: When we talk about problems like underinsurance in America, we’re typically referring to high out-of-pocket medical costs within the plan terms (such as high deductibles or high cost sharing). What I work to do in Coverage Denied is show that there’s this additional, less-discussed dimension of underinsurance: inadequate protection by health benefits in which one is enrolled, not due to plan terms, but rather due to insurer decision-making about what is actually medically necessary. Strikingly, there are more ways people can be denied by their health insurer than they realize.
Prior authorization, or required health insurer preapproval for prescribed care (typically costlier care, though it has certainly extended to lower and even low-cost care in recent years), is the realm of denials with which Americans are likely the most familiar. This is when your health-care provider wants you to get a CT scan, but you can’t proceed with scheduling until it gets cleared by your health insurer—and it might get denied. When people are denied prior authorization for health-care services, they face delays or denials of medical tests or treatments, potentially risking worsening health, unless they can afford to pay out of pocket (but health care in the United States is notably expensive, so that is rarely an option).
There are appeal processes in place that a patient denied prior authorization and their physician can pursue, though it can take time to submit additional information and receive a redetermination, and physicians might only be given hours to respond to a request to avoid a patient being denied again. This might mean that the patient cannot proceed with scheduling a diagnostic test. In the case of, say, a prescription medication, the patient may go unmedicated—potentially leading to worsening of symptoms —or be on a second-choice regimen to avoid an entire gap in care, pending the insurer processes that will take an unknown period of time to resolve. And if the patient’s conditions worsen, they may eventually require higher-level (and consequently, more expensive) medical care.
The irony here is that prior authorization is partly a measure aimed at cost containment, but if denials are ultimately delays that necessitate more pronounced medical intervention (whether receipt of medication in the emergency department, or even getting admitted), then this practice can undercut insurers’ underlying profit objectives.
People can also receive concurrent denials, which occur when the insurer decides during the course of a medical treatment that it will decline coverage for further care. The result of this mid-treatment decision can be treatment disruption, if not altogether discontinuation, that can undercut optimal health outcomes for the patient.
Retrospective denials occur when the insurer denies payment for health care that was already provided to the patient. While this does not leave the patient vulnerable to declining health with respect to that condition, it does raise the prospect that they will have to take on medical debt and potentially forgo other care so as to avoid risking accruing additional medical expenses. Additionally, though infrequently, one may be vulnerable to a retroactive denial, which occurs when an insurer retracts payment for a service that they already approved, leaving the patient themselves responsible for the payment (e.g., because the insurer determined that they should not have approved it previously). This can also render the patient vulnerable to assuming new medical debt that can be financially destabilizing and foregoing further health-care expenses. While this may be an appropriate error correction on the part of the health insurer, it can drive significant uncertainty and destabilization for the patient, who might not have continued to pursue the care if they had better information at the outset.
These types of claim denials (i.e., denials post-treatment) operate quite differently from prior authorization denials. The good news is that they shouldn’t result in a patient’s worsening condition per se (though anxiety about a denial of coverage for test A may lead to reluctance to pursue test B). The bad news is that this can contribute to the patient’s financial destabilization, potentially leading to medical debt that hurts their credit and thus broader economic opportunity. And of course, we know that medical debt is unevenly distributed across racial and socioeconomic groups, and health insurance barriers constitute another driver of those inequities.
Given that patients are often making these decisions with informational disadvantages—we don’t have a good sense of what care is in fact medically necessary, let alone the criteria with which our insurers are evaluating this—this multitude of ways that patients can be left both medically and financially vulnerable lays bare just why accessing health care in the US can be so anxiety-provoking (not to mention inequitable). And while analyses have shown that some providers do prescribe medical care that is of low or questionable value (in turn, running up quite a tab), all too often, the burden falls on patients, who get caught in between their prescribers and their insurers.
Stephen: What remedies are there for patients when denials happen, and do people even know about them or how to obtain them?
Miranda: As I mentioned, there are appeal processes in place, which insurers are legally required to provide patients with information about when they are issuing a notice of a denial. Some insurers are especially transparent about their process—UnitedHealthcare, for example, publishes online its detailed description of the three-layered standard appeal process and three-layered expedited appeal process. But there are a few things that can and often do get in the way of patients understanding and acting on this right, so that fewer than 1 percent of denied marketplace claims and less than 12 percent of Medicare Advantage (the privatized version of Medicare) prior authorization denials are appealed.
For starters, appeal explanations are already complicated processes that are often written in a way that is difficult for the average reader to understand. That means many people don’t even know what their rights even are. Additionally, people may underestimate the value of appealing. “I’m just one person going about their day. How could I possibly stand a chance going up against a health insurance giant?” And in fact, when I asked 1,340 people to guess how often health insurance appeals are won, most survey respondents thought patients win less than 20 percent of the time. In truth, it’s closer to a coin flip, with various estimates lying in the 40–60 percent range, and 52 percent of my survey respondents winning their appeals if they appealed. But if you think that this endeavor of appealing is likely to be fruitless, it makes sense that one wouldn’t exert the time and energy—the burden—of appealing.
I asked all of my survey respondents who were denied by their insurer but did not appeal why they chose not to do so. The two most common reasons were that (a) they didn’t realize they could appeal (often because the information was in fine print or not conveyed in plain language, or they saw the denial and got so discouraged that they didn’t read further) and (b) they didn’t think they stood a chance at winning (though many said that if they had known it was a coin flip, they’d have been more likely to appeal their own denial). Respondents also cited confusion about how to navigate the red tape of this insurance process. So, on the one hand, there’s a lot of evidence that coverage denials are not only destabilizing to health and finances, but that administrative burden gets in the way of patients pursuing appeals to reverse these adverse decisions. On the other hand, my findings point to the possibility of some simple information interventions to improve patient knowledge and, in turn, improve access to health benefits, even if we can’t tackle (yet) the complexity of the appeal processes themselves.
But the underlying reality is that insurers expect that patients are unlikely to go through the appeal process, which is difficult enough on a good day (and we’re rarely having our best day when we need to appeal to insurers). In fact, one person I interviewed, who reviews claims for a major health insurer, said they were told that denying is perfectly fine because there is an appeal process—even though they have the data to confirm that most patients don’t go through with them. This is why I characterize these processes not as rationing care through denial, but rather rationing by inconvenience, or accumulations of inconveniences.
Stephen: This sort of thing seems even crueler than high premiums and deductibles, where at least you know what you’re (not) getting. The uncertainty and arbitrary and almost Kafkaesque conditions experienced by patients who suddenly find themselves without the safety net they thought they had purchased is really striking.
You did a lot of interviews for this book. Are there any cases that stand out to you, that really illustrate the absurdity of it all?
Miranda: It is absolutely the case that this uncertainty and apparent arbitrariness—the “song and dance”—is overwhelming and heart-wrenching for patients (as well as for their providers) in a way that goes beyond the broader but more predictable frustrations about care being unattainable due to, for example, a high-deductible health plan. One physician interviewee told me about his experience with prior authorization burdens:
“It feels like there are people sitting around a room conspiring to figure out how to delay care further. And every day that they can delay your care is money kept in their pocket longer.”
One patient story that stuck out was surely an administrative error, but nevertheless burdensome for both patient and physician to correct. This patient was getting a wrist MRI with contrast: First, the patient had radioactive dye injected, and then the scan was to be performed. Her insurer approved the radioactive injection but not the scan that made that exposure necessary. Now, at face value, that sounds silly—and it is. But what it took to correct it was a recognition that this was absurd (when a lot of patients don’t read itemized medical bills, let alone understand them), and a degree of health insurance literacy and administrative capital that enabled her to successfully navigate the complexity of the health insurance appeal process.
But there were some really heart-wrenching stories. One was from a low-income woman in the South who had taken time away from a years-long nursing career due to medical complications following the birth of her daughter. Amid prolonged severe lower abdominal pain and vaginal bleeding, she was ordered a CT scan and spent months navigating insurance complexity to get prior authorization, to no avail. When the insurer asked for additional documentation of medical necessity, she brought to bear all of her skills as a nurse, using not only technical medical terminology to document her symptoms but indicating numeric pain ratings based on exacerbating factors, ameliorating factors, and the like—things that the average individual can’t do, because most people have limited medical knowledge. “I’m a nurse. I know how to document stuff. I’ve been doing it for 15 years,” she recounted. But it was to no avail that she described her condition as clinically and as elaborately as possible when seeking insurer approval. “I got specific, they denied it, and they picked a different reason.”
Then, the hospital erroneously said that the prior authorization was approved, but this patient ended up stuck with such a big bill that not only did she have to put off necessary home repairs amid a failing roof, but she even contemplated divorcing her husband and the father of her daughter in order to have an income that would qualify for Medicaid. This level of financial and family devastation wasn’t anomalous. The average American can’t accommodate an emergency $1,000 expense without going into debt, and as most people can attest to, it’s not hard to accrue a $1,000 medical expense.
And alongside all of this was a real loss of trust in the system and feeling of inadequacy amid the navigation of red tape. One diabetic lawyer said of his battle to get a continuous glucose monitor,
“Is there something wrong with me? Do I not deserve this? Do I think my need is more important than it really is? The process makes you feel so small.”
Diabetes treatment was an area in which coverage barriers were very common. After one interviewee battled her insurer to get on a more sustainable insulin regimen, she said,
“It colored the way I interacted with insurance for the rest of my life.”
Relatedly, it was striking to see the prevalence of prior authorization requirements in corners of health-care delivery where there is not evidence of overutilization and abuse, the mitigation of which is ostensibly a central goal underlying the administration of prior authorization. PrEP is one such medication, which is critical in preventing HIV transmission and thus an important aspect of LGBTQ health. This isn’t a medication that people just take “for fun,” nor is it a medication that is abused or overprescribed—but there can be prior authorization attached to it nevertheless. Another example is insulin, which is literally lifesaving for millions of Americans, but can still have onerous prior authorization and formulary restrictions attached to it. As I spoke with these patients who felt like they were constantly playing the role of Sisyphus pushing the boulder up the hill, it is little wonder why they lost trust in, and felt betrayed by, the insurers to whom they had been paying monthly premiums for years.
How we got here: Why US health insurance is the way it is
Stephen: It seems that there’s a fundamental issue in health care around constraining costs and preventing overtreatment in the form of unnecessary/low-value/wasteful care. Doctors want to be thorough (and don’t want to be sued for malpractice), patients don’t know how to distinguish between necessary and unnecessary care, and insurers don’t want to pay, for example, to run an endless battery of useless tests. But while this might be a fundamental problem in health care, the ways in which it plays out in the United States are unique and tied to our for-profit insurance system.
Can you describe some of the features of our system that have contributed to “managed care” (plans that cut costs via pre-authorizations, drug tiers, step therapy, etc.)?
Miranda: During the New Deal, there was some hope that amid this expansion of national power to lift the US out of the Great Depression, there might be sufficient support to carry national health insurance across the finish line. But even Franklin D. Roosevelt’s immense popularity wasn’t enough to get this done, and it became clear pretty quickly that trying to tie health insurance to Social Security was going to compromise both, and Social Security was an absolute must-have. Harry Truman then spent his presidency fighting tirelessly, albeit unsuccessfully, for national health insurance, but faced immense opposition campaigns from organizations like the American Medical Association (AMA), which used the slogan “The Voluntary Way is the American Way” in an effort to curb movement toward a compulsory insurance program that they likened to “socialized medicine.” In the background of all of this, employer-sponsored insurance had just gained prominence during World War II and further advanced through the labor movement: The Stabilization Act of 1942 precluded raising wages to attract much-needed workers, so health insurance became the perk of choice.
Eisenhower didn’t unravel the New Deal, but he did favor privatization over national insurance. When the 1960s rolled around, the previous ambitions of national health insurance were scaled down to prioritize targeting two vulnerable populations, the indigent (who would get Medicaid) and the elderly (who would get Medicare). Amendments to the Social Security Act in 1965 ultimately secured this new coverage. And in fact, LBJ signed these into law at the Harry S. Truman Presidential Library in Independence, Missouri, as a nod to his long-fought efforts toward this expansion.
But of course, these programs cost money, in part thanks to the fee-for-service arrangements according to which they were designed, such that there was little oversight over billing and the physicians could earn more by ordering more tests and treatments. So, it’s around this time that we see the introduction of some very narrowly circumscribed utilization management, such as certifying hospital lengths of stay. Of course, having a physician tell an insurer, “Yes, this patient does still need to be in the hospital to treat X” is a far cry from its current sweep. But the rising health-care costs also fueled the enactment of the Health Maintenance Organization (HMO) Act of 1973, which encouraged the development of HMOs, which are private insurance plans. What would later follow was the more flexible preferred provider organizations (PPOs). Ironically, with this latter, more flexible mechanism of health insurance delivery came the loss of a key cost-control mechanism, giving rise to the set of concerns that led to the proliferation of prior authorization.
The Balanced Budget Act of 1997 further cemented the United States’ reliance on privatization, bringing Medicare Advantage onto the scene and escalating the privatization of Medicaid. It’s in this moment that we see at a large scale the privatization of traditionally public health insurance programs whose enrollees would now come to experience managed care plans’ cost-containment tools like prior authorization. And as health-care innovation—from new drugs to new technologies—flourished in the US, both quality and cost increased, spreading prior authorization into new corners of health-care delivery. Today, if you’re being prescribed a higher-cost drug, high-tech imaging, a surgery, a major procedure, and even some less costly drugs, you can bet on prior authorization or some form of step therapy (in which a patient must try lower-cost drugs before “stepping up” to what was initially prescribed).
At the end of the day, it’s a tough issue of politics, economics, medicine, and law all wrapped up in one. We don’t have unlimited amounts of money to spend on health care without making very hard (and likely politically unpalatable) choices in other areas of policy delivery, so we need to find ways to contain costs, hopefully without compromising quality of care. We often misperceive more care as equating to better care (sometimes it is, but it certainly isn’t a guarantee), which then places demands on physicians who need to be mindful of patient satisfaction ratings as well as malpractice liability. That can in turn drive some degree of defensive medicine (or ordering unnecessary tests and procedures) that comes with a price tag.
And in the background of all of this is the reality that health insurers don’t have a ton of incentive to make up-front investments in our health—even those that have a good return on investment—because people change health insurers so frequently. This means that while it may seem like poor financial planning for Cigna to deny a patient Drug A, by the time a costly complication manifests for the patient, they may no longer be on Cigna, but rather UnitedHealthcare, or they may have aged onto Medicare. So, in addition to concerns about privatization, cost containment (as well as profit maximization given the need to report quarterly growth), and overutilization (which can undercut those cost-containment objectives), there’s also some passing of the buck that may not yield great patient outcomes and may even drive up costs in the system writ large, but not for the insurer that issued the initial denial.
So, then we get to the question of whether there are better alternatives to contain costs. One way to make up the deficit is that insurers could raise premiums, but we know that’s untenable for most people and would drive problems of adverse selection. Negotiating down the cost of health-care delivery by providers would certainly be a nonstarter with the AMA as well as with the broader physician community, especially given the high cost of medical training and recent politics around loan forgiveness. Improving drug price negotiation with the pharmaceutical industry is important, and we’ve moved in that direction narrowly, but that still won’t touch a lot of the problems here.
Another very underdiscussed aspect of this problem is the reality that while overutilization is a commonly cited concern driving the implementation of prior authorization, physician burdens associated with prior authorization and the appeals it can necessitate can actually drive issues of underprescribing to avoid these challenges.
Stephen: A big theme of the book is path dependence, the idea that each legal or regulatory decision sets us down a path and makes it harder to reach other outcomes. For example, I was struck by the fact that the backlash against narrow networks implemented by HMO plans probably made pre-authorization more common.
Maybe a bigger surprise was the ways that the Affordable Care Act (ACA) may have inadvertently contributed to the current situation. Could you explain more?
Miranda: I’ll preface this by saying that I’m a huge fan of the ACA, but a few aspects of it are relevant to the story I’m telling here. First, it directly built on the private health insurance framework (the setting in which delays and denials of coverage are the most common) and left prior authorization largely undisturbed, with the exemption of emergency department care and in-network OB-GYN care. So, overall, there’s increased patient participation in private health insurance plans, which come with more prior authorization except in some narrowly circumscribed areas. But there’s also the possibility that when Congress told these private health insurers to cover all these people they’d done a very good job of finding ways to avoid covering—those with what had been declinable preexisting medical conditions (around 27 percent of non-elderly US adults, according to a 2019 KFF estimate)—the insurers look for other ways to curb costs. They can’t deny patients anymore, so it’s possible that denial of payment for prescribed care became the attractive alternative.
Stephen: When doing research on medical debt, I found that the debt problem was a lot worse for people on employer-sponsored insurance plans or ACA marketplace plans than for folks on Medicaid and Medicare (though a substantial portion of Medicare recipients are still carrying debt from their time uninsured and underinsured prior to aging into Medicare.)
You quote health-care expert Jacob Hacker in the book, who said, “Medicare should be the model for health security.” But a large part of the book details how both Medicaid and Medicare are also increasingly becoming managed-care systems. Can you explain what is happening and why?
Miranda: The US health insurance system is definitely made far more complex through its fragmentation, as well as its entwining of public and private programs, which can culminate in contradictory popular sentiment like “keep your government hands off my Medicare” and what Suzanne Mettler has characterized as the “submerged state.” And of course, Medicare is not the only government insurance program that has become heavily privatized. Not only are about 54 percent of seniors in Medicare Advantage, but about three-quarters of Medicaid is privatized.
Privatization of these two critical health insurance programs, which combine to cover roughly 4 in 10 Americans, is problematic for many reasons, but in the context of this book, it means adding a lot of prior authorization—and the delays and denials that come with it—for a population that has generally lower health-insurance literacy and is consequently less well-equipped to navigate the burdensome repercussions of these processes. Unlike Medicare Advantage, where 99 percent of enrollees have prior authorization, traditional Medicare has historically used prior authorization sparingly and denies care infrequently, though Centers for Medicare and Medicaid administrator Mehmet Oz’s introduction of the WISeR model that experts agree may lead to more denials. Medicare has been a game changer in enabling seniors to have quality coverage at a time in their lives when they generally have greater health needs but limited disposable income—and it provides this coverage with low administrative spending relative to private insurance and outside the confines of means-testing that can be stigmatizing and thus dampen policy take-up. But its privatization over the last three decades has produced outcomes that look a lot more like the broader private health insurance landscape (whether employer-sponsored insurance or the ACA marketplace) in terms of prior authorization, delays and denials of coverage, and burdensome and inequitable processes to appeal those adverse decisions.
On the managed Medicaid side, we also see frequent reliance on prior authorization and high incidence of delays and denials. Not only is this a population that has generally low health insurance literacy (raising the burdens of appealing barriers to coverage), but it is also generally less healthy (raising the stakes of these barriers to coverage). Moreover, due to their low income, they’re especially unlikely to be able to front the cost of medical treatment in order to avoid a gap in care pending an insurance appeal.
The Convenient Narrative Letting Insurers Off the Hook

Blaming hospitals isn’t wrong. But it’s incomplete—and it’s exactly the story insurers want told.
Zack Cooper argued this week in The New York Times that Americans may be blaming the wrong culprit for rising premiums. In his view, the bigger driver is hospital market power—fueled by years of consolidation that policymakers have done little to stop. On that point, he’s on solid ground saying that hospital prices have climbed steadily, and oversight has lagged.
Where the argument falls short is in how it portrays insurers. It suggests they are largely on the defensive—unable to push back on powerful hospital systems and left to rely on tools like prior authorization and claim denials as a workaround. In that telling, insurers come across less as drivers of the problem and more as constrained players navigating a difficult market.
That’s not consistent with what I saw working inside the industry, or with how the business is structured to operate.
Cooper’s academic work on hospital consolidation is serious and worth engaging with. But the argument he made in the Times—whether intended or not—tracks closely with a line the insurance industry has advanced for years. It’s a familiar frame, and one I recognize because I helped design it.
The industry’s oldest trick
When I was head of corporate communications at Cigna, one of my core job responsibilities was to ensure that the public and policymakers understood what we called the “true drivers” of medical inflation. Those drivers were never us. They were hospitals charging too much, drug companies gouging patients, and — when we needed a villain closer to home — ordinary Americans overusing the health care system. The finger-pointing was deliberate, coordinated, and effective. As any magician will tell you, misdirection is the oldest trick in the book.
AHIP, the industry’s trade and lobbying group, is running that same playbook today with the full force of the industry behind it. In recent months it has blanketed Washington with the message that “hospital costs account for more than 40 cents of every premium dollar” and that hospitals should “stop looking around for someone else to blame.” This is not an inaccurate claim. It is an incomplete one, deployed with the precision of a public relations campaign rather than the rigor of a policy argument. The fact that Cooper’s op-ed reinforces that message — even from an independent and credentialed source — is a gift to an industry that has been under unprecedented scrutiny since the murder of a UnitedHealthcare CEO in late 2024.
I am not suggesting Cooper wrote his piece on AHIP’s behalf. I am suggesting that a structurally incomplete argument, published in arguably the country’s most influential newspaper at this precise moment, serves the insurance industry’s interests whether or not that was anyone’s intention.
Who started the consolidation arms race?
Cooper’s framing also elides a crucial piece of history. Hospital consolidation did not happen in a vacuum. Hospitals began merging in significant part as a defensive response to the growing bargaining power of large insurers. Providers seeking to consolidate often cited a desire to acquire bargaining leverage with market-dominant payers, arguing that their own consolidation could counter the consolidation of increasingly powerful insurers.
Insurer consolidation begat hospital consolidation, which begat higher prices, which begat higher premiums. It is an arms race in which the only losers are patients and employers.
WATCH NOW:

WATCH NOW: Prior Authorization: Care, Delayed | EP 3
Copy link
Prior Authorization: Care, Delayed | EP 3
In the third episode of the HEALTH CARE un-covered Show, we take a deep dive into prior authorization’s toll — from doctors to federal policy — featuring Dr. Wendy Dean, Dr. Seth Glickman and Rep. Suzan DelBene (D-WA) on CMS’s new AI-driven WISeR model.
Watch the full episode here.
Cooper is right that hospital market power is now the dominant force driving costs. But the insurers that consolidated first — and that benefited by squeezing providers in the short run — helped create the conditions for the hospital consolidation wave that followed. Neither side’s hands are clean. The arms race, which dates back to the rapid horizontal consolidation that occurred in the insurance industry in the 1990s and early 2000s, is what patients are now paying for.
Now to the incentive problem Cooper’s framing obscures. In commercial insurance — particularly the self-funded arrangements that now cover most large employers — the insurer often earns fees tied to the total size of claims processed. Higher hospital prices mean larger claims. Larger claims can mean higher revenue for the insurer administering the plan. This is not a conspiracy. It is arithmetic. The incentive to hold the line on hospital prices is weaker than Cooper suggests because in many arrangements, higher costs flow through to the insurer’s bottom line.
The Affordable Care Act’s medical loss ratio rules were supposed to fix this by requiring insurers to spend 80% to 85% of premiums on care. What those rules actually do, in a rising-cost environment, is allow absolute profits to grow even as the percentage stays fixed. If the pie gets bigger, the insurer’s slice gets bigger too — even at the same ratio.
The network access trap
In markets where a single hospital system controls the majority of beds, the insurer faces a problem that has nothing to do with negotiating skill. It cannot exclude that hospital from its network and still have a product to sell. Employers and individuals will not buy a plan that locks them out of the dominant regional provider. The hospital knows this. The insurer knows this. What gets called “negotiation” in these markets is often closer to ratification.
The insurer’s response to this trap — when it cannot win at the hospital price table — is not to fight harder. It is to redirect. Costs that cannot be controlled at the source get shifted somewhere more manageable: onto patients, through higher deductibles and narrower benefits; onto providers, through prior authorization burdens and claims denials; onto employers, through premium increases framed as the inevitable result of “medical trend.”
This is the point Cooper comes closest to and doesn’t quite reach. He writes that insurers “are incentivized to lower health spending, but in many markets don’t have the ability to put meaningful pressure on hospital prices.” That’s true. What is also true is that they put pressure on everything else, which all too often has the effect of reducing access to medically necessary care.
Prior authorization, step therapy, utilization management — these are not crude approximations of cost control. They are the rational corporate adaptation to a problem the insurer has decided not to solve at its source. They extract value from the system by making care harder to access rather than cheaper to provide. And they do so in a way that is largely invisible to the public as a cost-shifting mechanism, because each individual denial looks like a clinical decision rather than a financial one.
Big Insurance Q1 2026 Earnings Round Up

In Q1 2026, 7 Big Insurers did what their shareholders demanded: hike premiums, slash benefits and dump the sick.
The most recent numbers the nation’s largest for-profit health insurers have shared with investors tell a story the industry is eager to tell Wall Street: the worst is over. After two brutal years of earnings misses, executive firings, and stock price collapses driven by unexpectedly high medical spending, the seven biggest publicly traded health insurers have now completed their first-quarter earnings reports for 2026 and their shareholders are cheering.
Every one of them beat analysts’ expectations in various ways, and most raised their full-year 2026 guidance. But before you read the company-by-company results, it is worth examining the mechanisms behind that recovery because the story the earnings releases tell is not quite the same as the story they leave out.
To get back into Wall Street’s good graces, insurers have:
- raised premiums
- cut benefits
- narrowed their provider networks
- exited markets that weren’t meeting investors’ profit expectations, and
- shed members they deemed too costly to cover.
Across the seven companies, total medical membership fell by roughly four million people between the first quarter of 2025 and the first quarter of 2026, and from what executives signaled to investors, many more people likely will be dumped by the end of the year. The patients who already have lost coverage through market exits or who found their benefits reduced this year do not appear as line items in an earnings release. They appear in the year-over-year membership declines and skimpier benefits that analysts note with approval.
WATCH NOW

Inside Big Insurance’s $1.7 Trillion Year | EP 2
Copy link
Inside Big Insurance’s $1.7 Trillion Year | EP 2
In second episode of the HEALTH CARE un-covered Show, we walk you through the full year 2025 earnings reports of seven of the largest for-profit health insurance corporations in the country.
The key metric driving the recovery is the medical loss ratio — the percentage of premium revenue that insurers actually spend on medical care. When that number falls, profits rise and investors get richer. Across the sector, medical loss ratios came down in the first quarter, or at least came in lower than Wall Street feared. Insurers credited tighter cost management, a milder flu season, and “repricing” — the practice of raising premiums and cutting benefits, particularly in Medicare Advantage plans, to close the gap between what they collect and what they pay out. (Financial analysts’ term for this is benefit buydown, which is unique among American industries.) Higher revenue coupled with devalued benefits produces better medical loss ratios from investors’ perspective.
The stock market has responded — but the picture is more complicated than a simple sector rebound. Most of these stocks are up year to date, measured from deeply depressed December 31 baselines. But look back a full year and a different story emerges: four of the seven companies are still worth less today than they were a year ago. Molina is down 43% over that period. Cigna and Elevance are each down about 6%. The “recovery” is real in the sense that stocks have bounced off their bottoms.
For much of the sector, it is not yet a return to full health, but the companies clearly are making good on their assurances to investors that they will do whatever it takes to improve their profit margins, regardless of the consequences to patients.
Here is what each of the seven reported — and what each report left out.
UnitedHealth Group
UNH Close (May 11): $384.44 YTD: +17.4% 1-year: +4.4% Dec 31: $327.56 | May 12, 2025: $368.36
UnitedHealth Group, the nation’s largest health insurer, reported first-quarter 2026 revenues of $111.7 billion, with adjusted earnings of $7.23 per share and a medical loss ratio of 83.9% — well below the 85.5% analysts had expected. The company raised its full-year adjusted earnings guidance to more than $18.25 per share.
UnitedHealth attributed the year-over-year declinedecline in its medical loss ratio to strong medical cost management and favorable reserve development, while acknowledging “consistently elevated utilization and unit cost trends.” In plain terms: patients are still using more care than the company would prefer, but UnitedHealth is getting better at managing around it.
The stock’s 17% year-to-date gain requires context. UnitedHealth ended 2025 at $327.56 — the result of a punishing year that included the Change Healthcare cyberattack, the killing of its insurance CEO, and mounting federal scrutiny of its Medicare Advantage risk-scoring practices. Then this past January, a disappointing fourth-quarter 2025 earnings report sent shares plunging nearly 20% in a single session, pushing the stock to its recent lows before the partial recovery began to take hold. The May 11 close of $384.44 leaves the stock about 4% above where it was a year ago — a modest gain that reflects recovery from a deep hole rather than a return to anything resembling its former heights.
CVS Health / Aetna
CVS Close (May 11): $92.23 YTD: +18.2% 1-year: +47.5% Dec 31: $78.03 | May 12, 2025: $62.52
CVS Health reported first-quarter net income of more than $2.9 billion as costs slowed for subscribers of its Aetna health plans. The company’s medical loss ratio fell to 84.6%, compared to 87.3% in the same period a year ago.
CVS attributed the decline primarily to better underlying performance in its government business and the absence of a premium deficiency reserve recorded in the prior year — a liability an insurer must set aside when anticipated claims are expected to exceed the premiums it has collected. Its absence is itself a sign of improved financial positioning.
Total revenue grew more than 6% to $100.4 billion. CVS raised its diluted earnings per share guidance and confirmed it is exiting the individual Affordable Care Act marketplace after this year. Total medical enrollment fell by roughly 600,000 members compared to year-end 2024, and more than one million year-over-year. This marked CVS’s fifth consecutive quarterly earnings beat.
CVS tells the clearest turnaround story in the group. Its stock is up 18% year to date and up nearly 48% from where it traded a year ago, when the company was in the depths of its earnings crisis and had just replaced its CEO. The trajectory is unambiguous — and so is the strategy behind it.
“Margins over membership”
That recovery was not an accident. It was a stated strategy. CVS CEO David Joyner has said repeatedly over the past year that the company is prioritizing “margins over membership” in its Medicare Advantage business. That means exactly what it says: CVS would rather have fewer, more profitable enrollees than a larger membership it cannot price to break even. On the commercial side, Joyner made the same calculus equally plain. “We do see elevated trends. We took a disciplined pricing approach to that in 2025, which has pressured membership, but we’re going to stay disciplined in our pricing approach,” he told investors last August.
“Pressured membership” is the corporate euphemism. What it describes is people being priced out of their plans, and what it means is that Aetna is once again purging customers it considers a drag on profit margins. (It has done that frequently over the past 25 years.)
The membership losses CVS reported this quarter — roughly 600,000 members gone, more than a million year-over-year — are the direct result of that strategy. Wall Street loved it.
Cigna
CI Close (May 11): $289.00 YTD: +5.6% 1-year: −6.5% Dec 31: $273.72 | May 12, 2025: $309.20
Cigna beat analysts on both earnings and revenue in the first quarter, posting $1.65 billion in profit. Its medical loss ratio came in at 79.8%, a favorable shift from the 82.2% posted a year earlier.
Cigna’s unusually low medical loss ratio reflects both aggressive cost management and a significant structural change. The MLR decline is partly attributable to the removal of its Medicare Advantage business, following Cigna’s sale of that book of business to Health Care Service Corporation. Medicare Advantage has been the primary driver of elevated medical costs across the industry. Cigna’s complete exit from MA made the numbers look cleaner.
Cigna also announced it will exit the individual ACA exchange market beginning in 2027. The company raised its full-year 2026 adjusted earnings guidance to at least $30.35 per share.
Evernorth, Cigna’s pharmacy benefit management and health services arm, generated $58.4 billion in revenue for the quarter, far more than the company’s health plan division. Like its peers, Cigna is increasingly a pharmacy and services company that also sells health insurance — not the other way around. (CVS now takes in more revenue from its PBM, Caremark, than from Aetna’s health plans and the company’s 9,000 retail stores.) Cigna’s stock has recovered to a 5.6% year-to-date gain but remains down about 6.5% from a year ago. A strong quarter has not answered the underlying question investors are asking: now that Cigna has exited Medicare Advantage and is exiting the ACA market, where does future growth come from?
Elevance
ELV Close (May 11): $381.84 YTD: +9.6% 1-year: −6.4% Dec 31: $348.40 | May 12, 2025: $407.98
Elevance Health (previously known as Anthem) reported $1.8 billion in first-quarter profit, down about 19% from the same period a year earlier, though the results exceeded Wall Street expectations. The company, which operates Blue Cross plans in 14 states, posted a medical loss ratio of 86.8% — slightly higher than a year ago, reflecting elevated costs in its Medicaid business, but better than analysts had feared.
Adjusted earnings per share came in at $12.58, above analysts’ consensus expectations. Elevance also raised its full-year 2026 adjusted earnings guidance.
One significant complication: Elevance’s results included a $935 million accrual tied to Medicare Advantage risk-adjustment data the company had previously submitted to federal regulators, where the ultimate liability remains uncertain. Risk-adjustment data — the system by which Medicare Advantage plans submit diagnosis codes to justify higher payments — has come under increasing regulatory scrutiny as a driver of what federal analysts estimate are tens of billions of dollars in annual overpayments to private insurers.
CEO Gail Boudreaux told investors that the company saw “moderately stronger retention” in its ACA segment and attributed better-than-expected results partly to a shift by remaining enrollees toward bronze-tier coverage — lower-premium, higher-deductible plans that tend to see lower utilization in the early months of the year. The stock is up nearly 10% year to date but remains about 6% below where it traded a year ago, with the risk-adjustment liability an unresolved overhang.
Humana
HUM Close (May 11): $274.24 YTD: +7.6% 1-year: +10.2% Dec 31: $254.84 | May 12, 2025: $248.93
Humana’s first-quarter results were the most complicated of the group — a beat on paper, but with enough asterisks to keep analysts cautious.
The company’s insurance segment MLR came in at 89.4%, edging out its own target of just under 90%, with medical and pharmacy cost trends running somewhat lower than anticipated. Revenue for the quarter reached $39.6 billion, up sharply from $32.1 billion a year earlier, driven largely by a 25% surge in Medicare Advantage enrollment.
But Humana did not raise its full-year guidance, unlike most of its peers. The company said it expects its second-quarter medical loss ratio to come in slightly above 91%, a deterioration from the first quarter — a signal that the cost pressures driving last year’s sector-wide crisis have not fully abated – and the expectation that Humana picked up many of the more costly MA enrollees that its competitors dropped.
Humana confirmed it expects to earn at least $9 per share for the full year and projects a full-year medical loss ratio of 92.75%, far higher than its rivals. Humana executives said the company’s primary objective is returning to a sustainable individual Medicare Advantage margin of at least 3% by 2028. Getting there will require continued benefit cuts, premium increases, and geographic retreats — all of which bear directly on the Medicare beneficiaries enrolled in Humana’s plans. What that means is that Humana likely will purge many of its new MA enrollees in the same way it did in 2025 after it disappointed Wall Street the year before.
Humana’s stock recovered sharply after the Q1 report, closing Monday at $274.24 — up nearly 8% year to date and up about 10% from a year ago. But investors’ enthusiasm should be tempered by one number: Humana’s aggressive Medicare Advantage membership growth this quarter mirrors exactly what CVS did in 2024, just before badly missing its cost targets as expenses came in far higher than expected. If that pattern repeats, the recovery will be short-lived.
Centene
CNC Close (May 11): $56.35 YTD: +36.9% 1-year: −10.4% Dec 31: $41.15 | May 12, 2025: $62.87
Centene kicked off the year with better-than-expected revenue and adjusted earnings, signaling a recovery from a rough 2025. Its stock rose more than 13% the day after its earnings call — and at nearly 37% year to date, it is the strongest year-to-date performer in the sector so far in 2026.
The company posted total revenues of $49.9 billion, with its consolidated medical loss ratio falling slightly to 87.3%. Adjusted diluted earnings per share came in at $3.37, and Centene raised its full-year adjusted EPS guidance to above $3.40.
Centene is primarily a Medicaid and ACA marketplace insurer, and its recovery story is rooted in those markets. The company’s Medicaid medical loss ratio fell half a percentage point — driven by rate increases from states and continued cost management.
The ACA marketplace, however, remains a source of volatility. Centene’s ACA enrollment fell sharply as the expiration of enhanced premium tax credits pushed many lower-income consumers out of the market — a policy shift that, for Centene, paradoxically helped near-term financial results by reducing exposure to a segment that had been generating losses.
As with the rest of the sector, context matters. Centene ended 2025 at $41.15, deeply depressed from its year-ago price of $62.87. The stock has bounced hard off that bottom but remains down more than 10% from where it stood a year ago. The recovery is real but the hole it is recovering from is also real.
Molina
MOH Close (May 11): $185.17 YTD: +6.7% 1-year: −43.5% Dec 31: $173.54 | May 12, 2025: $327.69
Molina is the outlier in the sector’s recovery narrative — the one company whose headline numbers looked genuinely bad, even as management insisted the underlying story was better than it appeared.
Molina reported a 95% year-over-year drop in net income for the first quarter, falling to just $14 million from $298 million in the same period last year. The collapse was driven primarily by a one-time charge: a $93 million impairment of intangible assets tied to the company’s planned 2027 exit from the Medicare Advantage–Part D market.
Total revenue was $10.8 billion, with premium revenue down about 4% year over year. The consolidated medical loss ratio rose to 91.1%, up from 89.2% in the first quarter of 2025.
The company’s executives reaffirmed full-year guidance for about $42 billion in premium revenue and at least $5 in adjusted earnings per share, and CEO Joe Zubretsky called the quarter “solid under the circumstances.” Molina has described 2026 as a “trough year” for its Medicaid margins, with the expectation that new contracts and the exit from unprofitable Medicare lines will improve results in 2027.
The stock market has rendered a harsher verdict. Molina’s shares are down 43% from where they traded a year ago — by far the worst one-year performance in the sector. The 7% year-to-date gain is recovery from a floor, not a foundation. Investors who held the stock through 2025 have lost nearly half their money.
The Second Quarter Will Be the Real Test
From Wall Street’s perspective, the industry has stabilized. Whether the companies’ management teams have learned anything different is a question the second quarter will begin to answer.
Analysts have flagged Q2 as especially critical — particularly for Humana, whose aggressive Medicare Advantage membership growth while holding benefits stable mirrors a pattern CVS followed in 2024, before badly missing its medical loss ratio targets. If that pattern repeats, the stock gains of recent months will not hold.
More broadly, the mechanisms driving this quarter’s “recovery” — premium hikes, benefit cuts, member shedding, and structural exits from unprofitable markets — are not cost reductions. They are cost shifts. The medical spending did not go away. It was simply transferred: onto patients through higher out-of-pocket costs, onto states through Medicaid pressure, and onto the federal government through the ongoing overpayment dynamics in Medicare Advantage that regulators have not yet fully addressed.
Wall Street calls this a recovery but it is worth being precise about what has actually been recovered and what has simply been moved off the balance sheet and onto someone else’s.
Five Ways to Start Fixing America’s Health Care System

Identifying what’s broken in American health care is easy. The harder part is disarming the ticking time bomb before soaring costs, consolidation and coverage gaps explode into something worse.
I saw an interview with a bomb disposal technician. He made the comment; “Identifying a bomb is easy, disarming it is the hard part.” It made me think about the debate around our current health care problems. It’s easy to point to all the things that are wrong or to throw stones at big insurance companies or Big Pharma.
Even though the finger pointing may be warranted, the harder part is coming up with a solution to this ticking time bomb. If we don’t figure out how to disarm this bomb it’s going to take us all with it when it goes off. I am as guilty as anyone of focusing on the problems we have, so, here is my attempt at some real solutions. I don’t pretend that these five things will solve all our problems, but I think they are a good start. So here we go.
- Pass the Break Up Big Medicine Act. We need to pass this bill right away. Much of our problems with cost and insurance intervention in health care comes from the fact that they have been allowed to create mammoth vertically integrated companies that not only finance health care but also control much of how health care is delivered. These massive health care companies have done nothing to control costs. Their focus is on maximizing profits. Case in point. A recent study showed that UnitedHealth Group pays its own doctors an average of 17% more than independent doctors in the same specialty and market. This is just one example of how this vertical integration is increasing costs to increase profit for UnitedHealth. I could write a whole book on why this much vertical integration creates problems but the long and short of it is, insurance industry vertical integration is like having a for-profit fire department that is also an arsonist. If you are going to be an insurance company then you need to focus on that business and not be allowed to own doctors, PBMs, etc.
- Pass a law that makes the actions performed by insurance company medical directors fall under the legal definition of “practicing medicine”. This would mean that when an insurance company medical director decides that a patient can’t have a study or a specific drug or when they deny a claim as not medically necessary, they are practicing medicine. They would then have all the responsibilities and accountabilities that the treating physician has. They would have to have a valid license in that state. They would have to be practicing in their specialty. They would have to document their decision making in an electronic medical record that belongs to the patient, and they could be sued for malpractice. You know all the same things that the actual treating physician must do. No more hiding behind the shield of “I’m not saying you can’t have it, just that we won’t pay for it.” If this were done it would eliminate most of the delays and care denials that plague our current system.
- Deal with the highly concentrated health insurance marketplace with existing monopoly rules and enforcement. In almost every other industry the Federal Trade Commission protects consumers and makes sure that competition is present by looking at highly concentrated industries. They use a long-standing mathematical measure called the Herfindahl-Hirschman Index (HHI). Under this index any industry with a score higher than 2,500 is considered highly concentrated and as such ripe for review and possible action by the FTC. When it comes to health insurance if you look at the HHI by state you come up with some alarming results. In 2024 there were only 3 states and the District of Columbia that had HHI scores below 2,500. Further, there were eight states with a score of over 7,000. In any other industry those situations would have been reviewed by the FTC long ago. These monopolies should be broken up to increase competition and protect consumers and doctors from this kind of unbalanced market power.
- We need to pass legislation that will create a process for universal clinical coverage policies. The care you receive should not be decided by the company name on your insurance card but rather on your clinical situation and evidence-based coverage guidelines. These guidelines should be approved by a group of clinical experts who are not financially incentivized to deny care. Right now, insurers that have a vested interest in denying expensive treatments decide when something is covered or not covered. We need to change that. Coverage policies should be universal. Doctors shouldn’t be asked to play the game of trying to figure out which drug or which treatment option is covered by each insurance company and rather should be recommending care based on what is best for the patient with the best evidence based medical research available at the time.
- Finally, we need to address one of the biggest travesties in our current health care environment. The fact that the richest country in the world does not have universal coverage for all its citizens should be problem number one. We should be embarrassed that a country of riches has failed and continues to fail such a large portion of our citizens when it comes to health coverage. We should require all insurance companies to sell insurance to anyone who wants to buy it either as an individual or an employer regardless of size. We need to make those premiums community rated with rates that are approved at the state level. We also need to finance or subsidize coverage for small businesses and people who don’t qualify for Medicare or Medicaid. This can be done by giving small businesses tax incentives to provide coverage under their business and to provide subsidies to individuals who are not able to get coverage from their employer and whose income is such that they can’t afford to purchase that coverage themselves. Paying for this universal coverage could be accomplished in several ways including, among other options, a small national sales tax or a small increase in the corporate or high-income tax rate. Again, we live in a country with an annual GDP of over $32 trillion dollars. Paying for universal health coverage for our citizens is not a heavy lift.
These five actions won’t solve all our problems. We still need to put more focus on wellness and prevention. We still have issues with mental health and substance use in this country. We need to work on providing better care and access for rural America.
Yes, there will still be plenty of work to be done even if we enacted each of these suggestions. These five things aren’t a full solution, but they are a very good start. Let’s start disarming this time bomb before it goes off.


