Monkeypox cases in women and non-binary people may be getting misdiagnosed as sexually transmitted infections (STIs), daily Covid-19 hospital admissions are expected to increase for the first time since July, and more in this week’s roundup of monkeypox and Covid-19 news.
Monkeypox:
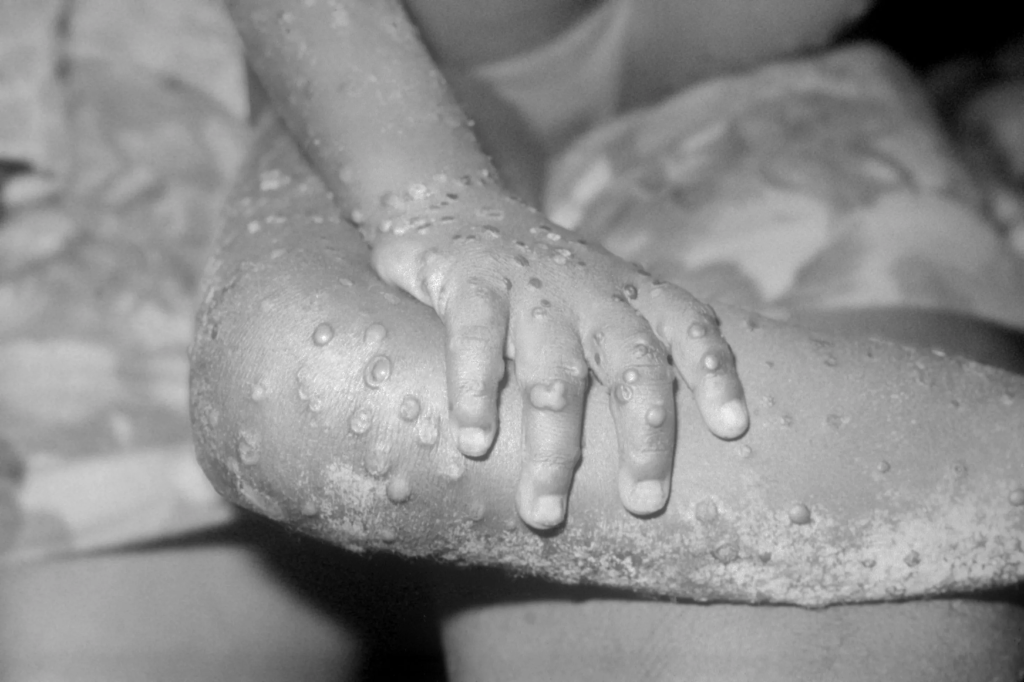
- Monkeypox may be getting misdiagnosed as STIs in women and non-binary people, according to a new study published in The Lancet. For the study, researchers gathered data from 69 cisgender women, 62 transgender women, and five nonbinary people assigned female at birth with confirmed monkeypox cases between May 11 and Oct. 4 across 15 countries. The study found that 73% of monkeypox infections among this group were likely acquired from sexual contact. While nearly all monkeypox infections among trans women were likely acquired through sexual contact, roughly 24% of cis women and nonbinary people were believed to have acquired an infection outside of sexual contact, such as household or occupational exposure, according to the researchers. In addition, the researchers found that around 33% of cisgender women were misdiagnosed before being diagnosed with monkeypox—and almost half received a delayed diagnosis. “It’s very likely that infections have been missed and not picked up at all,” said Chloe Orkin, a physician and researcher at Queen Mary University of London. “The lesson here is that everybody needs to know about this,” Orkin noted. While public health messages have been primarily directed toward men who have sex with men, “it’s important to recognize this is not the only group,” she added. (Mandavilli, New York Times, 11/21; Hart, Forbes, 11/17)
Covid-19:
- CDC is forecasting an uptick in Covid-19 hospitalizations for the first time since July, according to national disease modeling. In the coming weeks, CDC’s ensemble forecast from 15 modeling groups is projecting a nationwide increase in daily Covid-19 hospital admissions, with a forecasted 2,000 to 9,000 new daily admissions on Dec. 9. As of Nov. 11, the seven-day average of new hospital admissions for Covid-19 was 3,330—a slight decrease from 3,374 the previous week. In addition, modeling from Mayo Clinic is projecting a 51.5% increase in daily Covid-19 cases over next two weeks, with average daily cases projected to increase from 37,912.7 cases on Nov. 18 to 57,441 on Dec. 2. However, CDC’s ensemble forecast from 13 modeling groups projects that Covid-19 deaths will remain stable or follow an uncertain pattern over the next month. (Bean, Becker’s Hospital Review, 11/21)
- Earlier this month, omicron subvariants BQ.1 and BQ.1.1 surpassed BA.5 as the dominant strains of the coronavirus in the United States. Currently, BA.5 accounts for roughly 25% of new Covid-19 cases, and BQ.1 and BQ.1.1 account for an equal proportion of around 48% of cases. As BQ.1 and BQ.1.1 become more dominant, many experts are voicing concern over low vaccine uptake and evidence that suggests the dominant strains are not as susceptible to current treatments. For instance, FDA earlier this month updated its guidance for two monoclonal antibody treatments—bebtelovimab and Evusheld—warning that BQ.1 and BQ.1.1 showed significant declines in susceptibility to the treatments. (Choi, The Hill, 11/18)
- A new study published in JAMA Network Open found that almost 15% of 62,525 hospitalized Covid-19 patients had a medical contradindication after taking Paxlovid’s antiviral combination of nirmatrelvir and ritonavir. To evaluate Paxlovid eligibility among hospitalized Covid-19 patients, researchers used a list of individual contraindications created by FDA. The patients were hospitalized in Paris University hospitals between Jan. 24, 2020, and Nov. 30, 2021. In total, over 9,100 patients—or 14.6%—experienced a medical contraindication to Paxlovid, making the treatment inadvisable. Notably, contraindication rates were higher among men (18%) than in women (11.3%). Among older patients, contradiction rates were 26.9%. “The most prevalent contraindications were severe kidney impairment and use of medications dependent on CYP3A for clearance,” researchers said.