https://mailchi.mp/72a9d343926a/the-weekly-gist-september-24-2021?e=d1e747d2d8
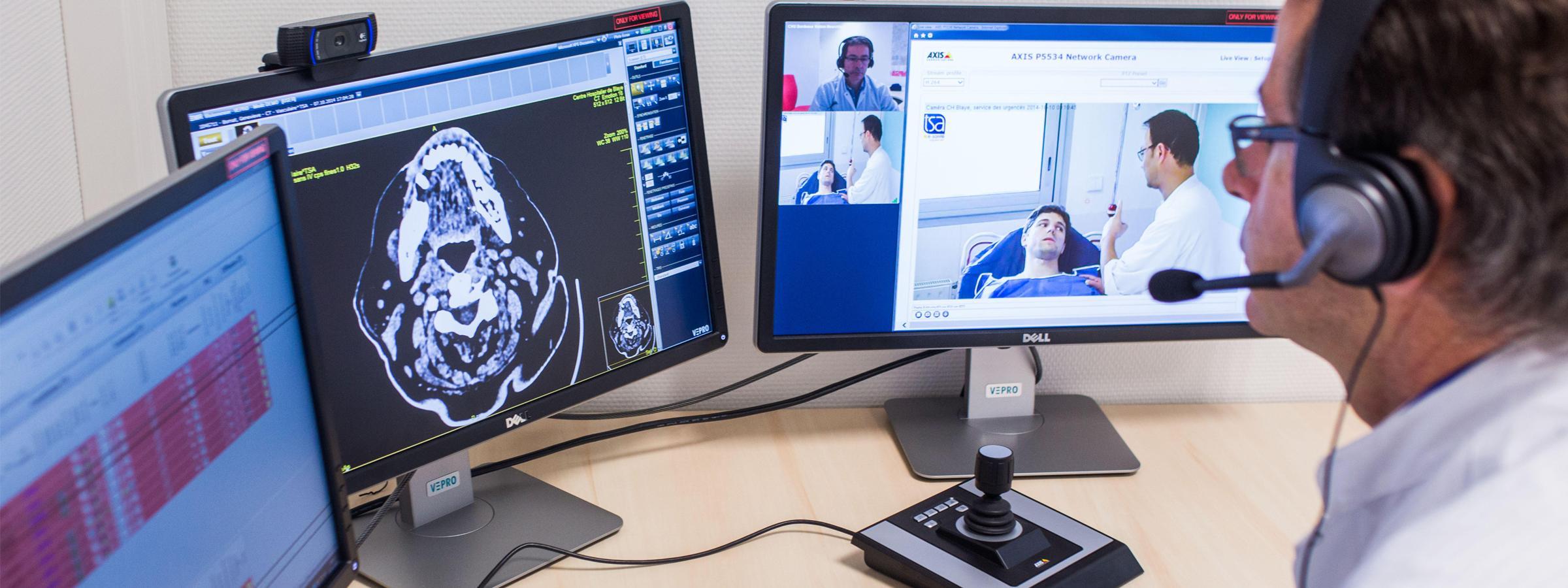
Every health system and physician group is now focused on strategies to make telemedicine more scalable across their networks. When we spoke recently with a chief medical information officer (CMIO) leading his system’s telemedicine strategy, he shared, “If there is one thing I wish executives would understand about telemedicine, it’s that it will never make doctors more efficient.”
His data show the average video visit takes just as long as an in-person encounter. True, there is no physical exam, but the virtual conversations can be lengthy. And adding in time lost to helping patients troubleshoot technology, some of his colleagues report that virtual visits may actually take a little longer.
He went on to explain that other kinds of virtual encounters, specifically asynchronous communication with a provider, sometimes supported by automated symptom triage engines like Zipnosis, are far more time-efficient ways to communicate with patients. Certain clinical situations may better lend themselves to these types of “e-visits”. Take dermatology, where sending a high-resolution picture of a rash to the clinician is more valuable than trying to view the problem live on a Zoom call.
Of course, video visits can be far more convenient for patients—and there is huge value in in providing access to patients wherever they are. But delivering telemedicine “at scale” to meet rising consumer expectations will require finding the right balance of asynchronous communication, telemedicine, and in-person visits to best fit specific clinical circumstances.
And we’ll need to rethink clinical workflow—centralizing some telemedicine delivery at the system level across individual practices.

