
Monthly Archives: December 2022
Cartoon – Employee Engagement
Cartoon – Growing the Top Line
Cartoon – Important to Note
Operating Margins Among the Largest For-Profit Health Systems Have Exceeded 2019 Levels for the Majority of the COVID-19 Pandemic
Recent reports have raised concerns about the financial stability of hospitals amidst disruptions caused by the COVID-19 pandemic and the looming prospect of an economic recession.
Large amounts of government relief helped prop up hospital margins in 2020 and 2021. However, industry reports suggest that the outlook for hospitals and health systems has deteriorated in 2022 due to the ongoing effects of the pandemic (such as labor shortages), decreases in government relief, and broader economic trends that have led to rising prices and investment losses. According to at least one account, 2022 may be the worst financial year for hospitals in decades. These challenges could force hospitals to take steps to increase efficiency but may also result in price increases or cost-cutting measures that impair patient access or care quality. Against this backdrop, industry stakeholders have asked Congress to provide additional fiscal relief to hospitals and to stop scheduled Medicare payment reductions.
To provide context for these policy discussions, we evaluated the financial performance of the three largest for-profit health systems in the country—HCA Healthcare (“HCA”), Tenet Healthcare Corporation (“Tenet”), and Community Health Systems (CHS)—which collectively accounted for about 8 percent of community hospital beds in the US in 2020.1 These three systems are publicly traded, meaning that we were able to acquire timely financial data about these systems through their reports to the Securities and Exchange Commission (SEC), as well as data on their stock prices (see Methods for additional details).
Operating margins among all three large health systems were positive and exceeded pre-pandemic levels for the majority of the pandemic, including most recently in the third quarter of 2022.
Operating margins reflect the profit margins earned on patient care and other operations of a given health system—such as from gift shops, parking, and cafeterias—and incorporate government COVID-19 relief funds.2 Our definition of operating margins excludes income taxes and nonrecurring revenues and expenses, such as from the sale of facilities. HCA and Tenet had positive operating margins throughout the pandemic, and CHS had positive operating margins in all but two quarters of the pandemic (with one of those quarters being at the very beginning of the pandemic). HCA has had operating margins of at least 10 percent during the majority of the pandemic (9 out of 11 quarters). In other words, HCA’s revenue from patient care and other operations exceeded operating expenses by at least 10 percent for most of the pandemic. Tenet has had operating margins of at least 5 percent for the majority of the pandemic (9 out of 11 quarters), while CHS’s operating margins have been lower (less than 5% for 9 out of 11 quarters). CHS had lower margins than the other systems before the pandemic as well.
For all three systems, operating margins have exceeded pre-pandemic (2019) levels for most of the pandemic (9 out of 11 quarters), including the last quarter of our analysis (the third quarter of 2022), despite recent decreases in operating margins. HCA and Tenet dipped below their 2019 operating margins during two quarters of 2020, and CHS fell below their 2019 operating margins during the first quarter of 2020 and the second quarter of 2022 before increasing again. As of the third quarter of 2022, operating margins were 11.4 percent for HCA, 8.4 percent for Tenet, and 1.2 percent for CHS.
Stock prices increased and then decreased during the pandemic; HCA and Tenet stock prices have increased overall since January 2020 while CHS stock prices have decreased.
Stock prices generally reflect investors’ evaluation of the future earnings potential of a given company. Stock prices increased dramatically during the first 1.5 to 2 years of the pandemic. At their heights, HCA stock prices had increased by 87.9 percent, Tenet stock prices had increased by 153.8 percent, and CHS stock prices had increased by 383.1 percent relative to January 2020.
Stock prices have also decreased substantially in 2022—in line with broader economic trends—and especially so among Tenet and CHS. As of November 8, 2022, HCA and Tenet stock prices have increased overall relative to January 2020 (by 44.6% and 12.6%, respectively).3 CHS stock prices have decreased by 11.5% since January 2020, though CHS has also experienced longstanding financial challenges that predate the pandemic. For purposes of comparison, HCA stock prices increased by a much greater amount than the S&P 500 during this period (44.6% versus 16.8%), while the S&P 500 slightly outperformed Tenet stock (16.8% versus 12.6%) and significantly outperformed CHS stock (16.8% versus -11.5%).
As of December 2, 2022, the majority of market analysts followed by MarketWatch were bullish on HCA and Tenet stock (with 18 buy, 3 overweight, and 5 hold recommendations for HCA stock and 14 buy, 2 overweight, and 4 hold recommendations for Tenet stock) and neutral about CHS stock (with 8 hold and 4 buy recommendations); none of the analysts rated these stocks as “sell” or “underweight.”
Discussion
Industry reports have suggested that hospitals had high margins in 2020 and 2021 but have faced significant financial challenges in 2022. Our analysis adds nuance to this discussion. So far this year, operating margins among the three largest for-profit health systems in the country have met or exceeded pre-pandemic levels. HCA and Tenet in particular have had high operating margins. CHS had negative operating margins in the second quarter of 2022, and its stock prices decreased overall from January 2020 to November 2022, but its financial challenges precede the pandemic. While some hospitals are struggling in the current environment—with high inflation and the ongoing burdens posed by COVID-19, flu, and respiratory syncytial virus (RSV)—our results indicate that the largest for-profit systems have had operating margins that exceed pre-pandemic levels.
Physical and Occupational Therapy Are on the Medicare Chopping Block

Americans expect the best care from their doctors. Decades of experience, thoughtful interdisciplinary planning, and evidence-based research mean providers are treating them based on widely accepted standards of care.
For example, someone who has experienced a heart attack would never be discharged from a hospital without being prescribed medications to mitigate future cardiac events. A patient with acute pulmonary issues would receive medications and resources for oxygen therapy, if appropriate. Stroke patients receive the acute hospital-based care they need to save their lives, as well as a constellation of other types of care and services to decrease complications and enhance recovery — pharmacological, dietary, and rehabilitative.
Physical therapy and occupational therapy are among the critical standards of care that would be included for all of these patients. These services help form the bedrock of ensuring good outcomes, decreasing secondary injury and complications, and reducing rehospitalizations.
In addition to serving as an important part of post-acute care, physical and occupational therapy provided by licensed therapists can help improve balance and mobility, improve cardiovascular function, reduce pain, and decrease falls. In fact, healthcare associated with falls costs the healthcare system tens of billions of dollars each year — and exercise interventions by physical therapists have helped to lower the risk of falls by 31%.
Eliminating or reducing access to physical and occupational therapy due to Medicare cuts would be devastating to patients’ health outcomes. Not only would it undermine the standards of care for many conditions, it would also complicate the lives and tenuous health situations of the millions of Americans who depend upon it.
Seniors nationwide, therefore, are extremely concerned about the 4.5% cut to their therapy providers in 2023 under the Medicare Physician Fee Schedule. If this cut is implemented, the physical and occupational therapy community will experience cuts totaling approximately 9% by 2024. The continued practice of annual Medicare cuts threatens the sustainability of the country’s physical and occupational providers, especially in rural and underserved areas where they are needed most.
Our nation’s Medicare beneficiaries understand how integral physical and occupational therapy are to standards of care — and they value it deeply. According to a recent survey, 9 out of 10 Americans over the age of 65 have favorable views of physical therapists, and the majority see considerable value in the services they provide. Nearly the same number (88%) expressed concerns that proposed Medicare payment cuts may eliminate alternatives for therapy outside of nursing homes and eliminate seniors’ ability to age in place. More than three in four respondents (76%) say it is important for them to be able to access their physical therapist when they cannot come into the office for an in-person appointment.
Care professionals across the healthcare continuum — from skilled therapists to physicians to nurse practitioners and physicians’ assistants — recognize the negative impact these cuts would have on their patients, and support efforts in Congress to address these cuts in the year ahead.
Bipartisan lawmakers in Congress have introduced legislation to block these harmful cuts from taking effect in 2023, an essential step toward ensuring all Americans can access quality physical therapy and other specialty services. The Supporting Medicare Providers Act of 2022 (H.R. 8800) would block Medicare’s Physician Fee Schedule cuts by providing an additional 4.42% to the conversion factor for 2023.
It’s inconceivable to think we can continue to provide thorough care without one of the most essential elements — therapy. We hope that Congress will act — and quickly before the end of the year — so that our critically important healthcare standards for patients suffering from a multitude of diseases, injuries, and conditions are not irrevocably undermined.
Does Coffee Increase Lifespan?

A 2022 observational study publicized by Harvard Health claimed that drinking coffee could significantly lower your risk of dying.
Is that true?
Wasn’t there a study (or ten) in recent memory claiming that coffee would give you cancer?
Well, it turns out observational studies are not very good for studying things like this.
Inflation cools in November for the second-straight month
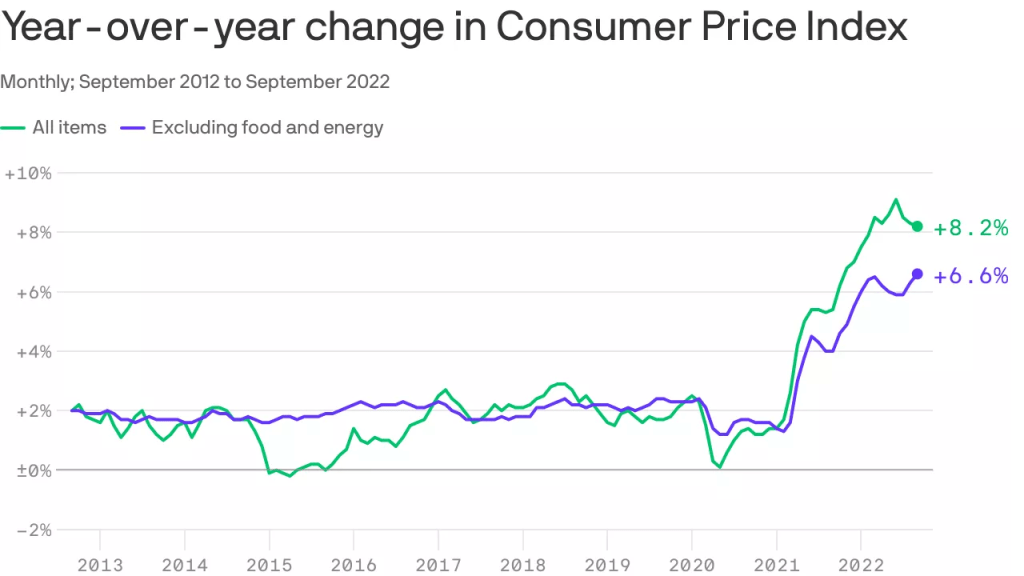
Following a cooler-than-expected inflation reading in October, consumer price gains slowed even further last month: the Consumer Price Index rose 7.1% in the year ending in November, down from 7.7% the prior month, the Labor Department said on Tuesday.
Why it matters: Inflation is still way too high, but the data offers some hope that it can ease alongside a still-healthy economy.
By the numbers: On a monthly basis, CPI rose 0.1%, slower than the 0.4% in October.
- Core CPI, which strips out volatile food and energy costs, also continued to ease. On a monthly basis, it rose 0.2% — up 6% over the 12 months ending in November.
- In October, those figures were 0.3% and 6.3%, respectively.
Where it stands: The Federal Reserve has raced to try to get inflation under control, raising interest rates at a historic clip — moves that risk throwing the economy into a recession.
- Officials will likely raise rates by a smaller (but still historically huge) amount following a two-day policy meeting that concludes on Wednesday.
- That will come after surprisingly cooler inflation readings, though officials have warned that its war on inflation is far from over.
Atrium and Advocate Aurora complete merger
https://mailchi.mp/3a7244145206/the-weekly-gist-december-9-2022?e=d1e747d2d8
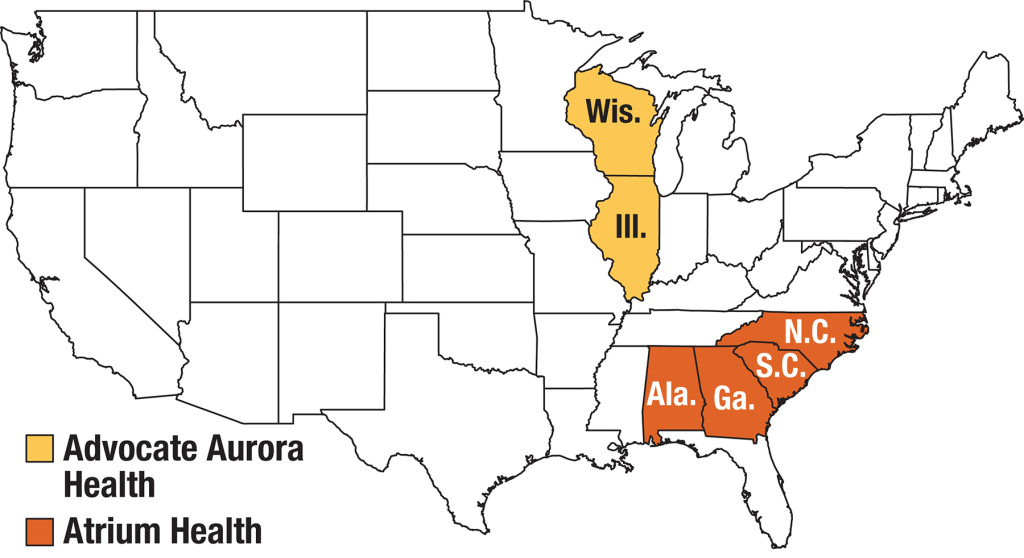
Charlotte, NC-based Atrium Health and Downers Grove, IL- and Milwaukee, WI-based Advocate Aurora Health have formally combined to become the nation’s fifth-largest nonprofit health system. Taking the name Advocate Health, the $27B system will control 67 hospitals across six states in the Midwest and Southeast. The merger, announced in May of this year, unites the systems on even footing, with equal representation on a new board of directors, and a co-CEO arrangement for the first 18 months. The Atrium, Advocate, and Aurora brands will continue to be used in their respective local markets.
The Gist: Structuring Advocate Health as a joint operating agreement, and creating a new superstructure atop the two legacy systems, should allow the combined entity more flexibility in local decision-making, while still potentially generating cost savings from back-office efficiencies.
While we expect these kinds of mega-mergers between large regional systems to continue, it remains to be seen whether the newly combined systems can successfully create value by building larger “platforms” of care to win consumer loyalty, deploying digital capabilities, attracting talent, and becoming more desirable partners for nontraditional players.
Workplace violence continues to strain hospitals
https://mailchi.mp/3a7244145206/the-weekly-gist-december-9-2022?e=d1e747d2d8

Even before the pandemic, healthcare workers accounted for nearly three quarters of non-fatal injuries from violence in the workplace. Given the level of emotion and stress experienced in hospitals, that’s not surprising. But during the pandemic, once-sporadic violent outbursts became routine, leaving many healthcare workers fearful for their safety.
According to several health systems we’ve recently spoken with, violent events haven’t waned as the number of COVID admissions has fallen. One hospital CEO recently told us, “I never would’ve imagined that security would consume so much of my time. We keep looking for a great solution, but despite a ton of effort and a lot of money, it’s barely made a dent.” The cost of additional security—more personnel, metal detectors, restricted access—can run into millions annually for the average hospital.
Another CEO shared, “We want the hospital to be a healing environment, not feel like a prison, so we were looking for less-threatening alternatives. But those were even more expensive. Placing a canine team in the ED would run over $1M per year!” And violent episodes are not limited to hospitals, with systems reporting an increase in incidents at outpatient and clinic sites where it’s not feasible to place onsite security, given the number of smaller-scale locations.
Human resource leaders report that experiencing workplace violence, either personally or through a colleague, has been a tipping point for those considering leaving the field. According to one CHRO, workers experiencing repeat violence has been increasingly common: “We recognized the importance of having someone very senior—CEO, COO, or CMO—personally reach out to staff who have been assaulted in the workplace. But there are people who we’ve now had to call two or even three times. It’s hard to even know what to say in those situations.”
In addition to visible security and constant staff communication, providers must lobby state and federal lawmakers for legislation that requires tracking and reporting of healthcare workplace violence, and increases penalties. The Workplace Violence Prevention for Health Care and Social Service Workers Act was passed by the US House of Representatives in 2021, and was recently introduced into the Senate, so it’s time to contact your representatives and urge them to move this bill forward.




