https://mailchi.mp/377fb3b9ea0c/the-weekly-gist-august-4-2023?e=d1e747d2d8

A physician who has led the primary care enterprise for a large health system for over twenty years told us he’s never seen physician morale as low as it is now:
“Burnout is bad across the board for all specialties, but I’m having a really hard time finding the bright spots for primary care”.
We recalled a recent survey of primary care physicians that confirmed his observations, with 61 percent of doctors stating that primary care is “crumbling”. But it struck us that we’ve been seeing these kinds of dire surveys about the state of primary care for the entire quarter-century we’ve been doing this work.
What’s different now?
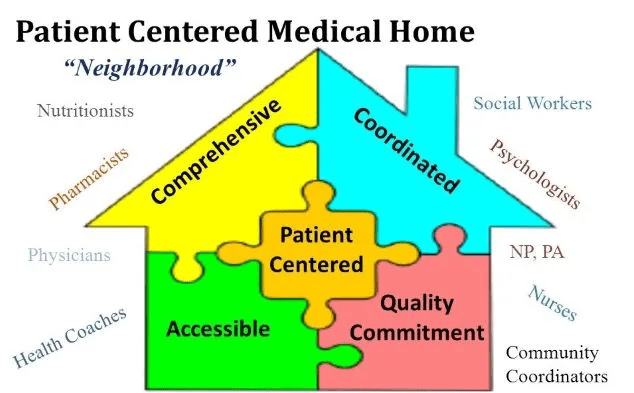
He posited one critical change. Ten years ago, during the heyday of accountable care, primary care was central to health system strategy. Systems were devoting resources to converting practices to patient-centered medical homes. “We felt like primary care was at the heart of transforming health systems, and that we were finally getting resources to help patients,” he shared.
“Now it feels like the health system has moved away from ‘value’, the focus is all on specialists and growing procedure volume again, and we’re being treated as a cost center and told to cut staff and up our referral targets.”
We agree. Although large independent primary care groups continue to command record valuations, overall, the transition to value has slowed, and work burden has increased given staffing shortages.
Where could optimism come from now?
We both agreed that workflow innovations to ease documentation burden and help the transition to virtual care appear closer to reality than ever before.
And the increased focus on “consumerism” has many systems recognizing that primary care is the first—and principal—touchpoint for most patients and will be key to winning consumer loyalty.