
COVID, RSV and flu cases rising as Americans gather for the holidays

Virus activity is picking up again as millions of Americans crisscross the country for Thanksgiving, taking fewer precautions to protect themselves against illness as concerns about COVID-19 fade away.
Why it matters:
Indoor holiday gatherings are expected to fuel a spike in cases of COVID-19, RSV and the flu — and with vaccinations against all three respiratory viruses lagging, health experts worry hospitals could be slammed again this winter.
What they’re saying:
“The concern here with this vaccination gap is: Could this get worse as the number of transmissions increases from November, December, into January?” Marc Watkins, chief medical officer for Kroger Health, told Axios.
State of play:
Health officials are urging vaccinations to head off a repeat of last winter’s “tripledemic,” when particularly nasty RSV and flu seasons collided with a COVID surge.
- About 15% of adults have received the updated COVID vaccine two months after it became available, according to the Centers for Disease Control and Prevention. That includes about a third of seniors, who are at highest risk from COVID.
- Most adults aren’t planning to get the updated COVID shot, according to a recent KFF survey that also found small shares were worried about COVID affecting their holiday plans.
- About half said they would take at least one precaution this fall and winter to limit their risk of getting COVID, such as avoiding large gatherings (35%) or masking in crowded places (30%).
- The vast majority of Americans have some form of immunity against COVID — from past infection, vaccination or both — but the updated shots can help protect against the latest circulating variants.
Meanwhile, flu vaccinations for adults and kids are slightly behind last year’s pace.
- Experts are hoping that new shots protecting older adults and infants against RSV will help keep patients out of the hospital. However, supplies have been limited, and some patients have run into hurdles getting insurers to pay for them.
- To help ease the supply strain, the CDC last week announced the release of 77,000 additional doses of a monoclonal antibody that protects against RSV in infants.
- 14% of adults 60 and older have received an RSV shot so far, according to the CDC. There isn’t yet data on pediatric vaccination rates.
Zoom in:
Texas is among the states that have been hit particularly hard by RSV early on, as emergency departments filled up with young patients in recent weeks.
- “We really were hoping that after two years of getting hit harder again with these viruses, it would kind of naturally be a milder season,” said Victoria Regan, a pediatrician at Children’s Memorial Hermann Hospital in Houston. “But it hasn’t happened yet.”
- There’s been a sharp rise in RSV cases in the last two weeks, according to CDC data.
- Flu cases rose 4% last week, and there’s high flu activity in several Southeastern states, as well as Washington, D.C., and Puerto Rico, according to CDC tracking.
- Though COVID isn’t being tracked as intensely since the pandemic ended, Midwestern and Western states have recently seen the highest rates of positive tests.
- And nationwide, COVID hospitalizations were up 8.6% in the most recent week for which the CDC has data, but still far below pandemic levels.
Be smart:
Those who are traveling should mask up in crowded areas like airports, have a game plan for getting tested or treated, and skip gatherings if feeling sick, recommended Mary Jacobson, chief medical officer at primary care company Alpha Medical.
The bottom line:
Expect a post-Thanksgiving spike in illness as respiratory virus season picks up and fewer people take precautions.
- “I think people are just fatigued you know, and they just want to go back to pre-COVID,” Jacobson said. “But this is here to stay.”
FDA approves latest weight-loss drug while AMA endorses coverage for obesity treatments
https://mailchi.mp/169732fa4667/the-weekly-gist-november-17-2023?e=d1e747d2d8

Last week, the Food and Drug Administration (FDA) announced the approval of Eli Lilly’s drug tirzepatide for treating obesity. The drug, which will be sold under the name Zepbound for obesity, is already branded as Mounjaro for diabetes treatment.
While Novo Nordisk’s blockbuster semaglutide drug (sold as Wegovy for obesity and Ozempic for diabetes) works only as a GLP-1 agonist, tirzepatide also targets a second receptor and has been shown to elicit greater weight loss.
Spurred by trial results demonstrating significant health benefits beyond weight loss tied to these drugs, the American Medical Association House of Delegates voted this week to adopt a policy advocating for insurance coverage of GLP-1-based obesity treatments, affirming that it regards obesity as a disease, and that patients left untreated for the condition are at greater risk for serious health consequences.
To date, most insurers and self-funded employers have resisted covering weight loss drugs due to their prices: Zepbound has a list price of $1,060 per month, while Wegovy is priced at around $1,300 per month.
The Gist: We have entered a new era in treating obesity.
Even with payers and employers dragging their feet over coverage decisions, and Medicare remaining prohibited from covering weight-loss drugs by law, consumer demand for the drugs has been strong enough to outpace supply. Zepbound’s approval will hopefully both improve availability and exert downward pricing pressure.
While these drugs will undoubtedly contribute to higher healthcare spending in the short term, the long-term benefits of significant weight loss, combined with cardiovascular risk reduction, could lower healthcare costs over the patient’s lifespan—although the payer “holding the bag” for the cost today may not see the return, given that as many as 20 percent of individuals with commercial insurance switch carriers every year.
Cigna’s Express Scripts adopts cost-plus pricing model
https://mailchi.mp/169732fa4667/the-weekly-gist-november-17-2023?e=d1e747d2d8
This week, Express Scripts, the nation’s second-largest pharmacy benefit manager (PBM), which is owned by health insurer Cigna, announced a new pricing model.
It is giving employers and health plans the option to pay pharmacies up to 15 percent over acquisition costs, plus a dispensing fee, for covered drugs. This payment structure was popularized by the Mark Cuban Cost Plus Drugs Company, founded by the billionaire businessman in reaction to the opaque pricing and complicated discounts and rebates common among PBMs.
While Cigna is not promising that this new pricing model will result in lower prices, it says it will improve transparency and should benefit retail pharmacies, who will split the markup with Express Scripts.
Cigna projects that only some employers will lower their healthcare spending through the cost-plus model, and that patient cost-sharing should be similar under both approaches.
The Gist: Between disruptive competitors like Cuban’s venture and increasing scrutiny from Congress, PBMs are facing new pressures to improve transparency and account for their role in rising drug costs.
This move by Cigna is an attempt to address at least one of those concerns, possibly intended to preempt regulatory and legislative action.
After years of complaints surrounding their business practices, it appears that the Congressional tide may be turning toward PBM industry reform. However, patients—who by and large are unaware of what PBMs are or do—won’t be satisfied till they see their out-of-pocket prescription drug costs go down.
Next up on this front: seeing which provisions targeting PBMs, many which have bipartisan support, make it into the Senate’s broad healthcare legislation planned for the end of this year, and in what form that bill ultimately passes.
Taking stock of a decade of Medicare ACOs
https://mailchi.mp/169732fa4667/the-weekly-gist-november-17-2023?e=d1e747d2d8
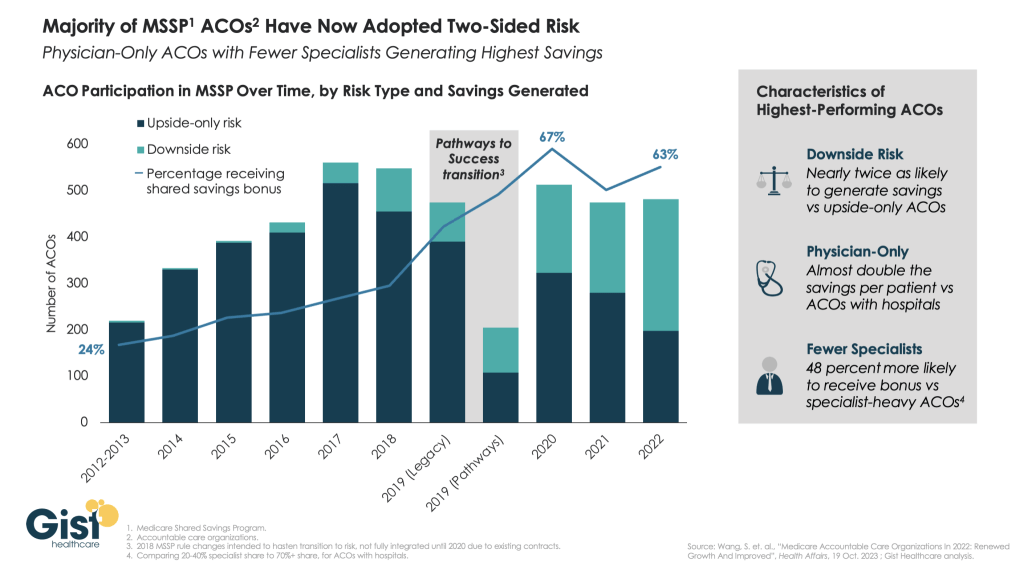
In this week’s graphic, we showcase recent data from Health Affairs highlighting the progress made by the Centers for Medicare and Medicaid Services’ (CMS) flagship value-based payment initiative, the Medicare Shared Savings Program (MSSP).
Ten years into the program, a majority of MSSP accountable care organizations (ACOs) have now adopted downside risk, after a slow start that was accelerated by CMS’s 2018 Pathways to Success program update. With more ACOs in downside risk, over 60 percent of program participants received shared savings bonuses in 2022, as MSSP ACOs with two-sided risk are twice as likely as ones with upside-only risk to receive a bonus.
Beyond taking downside risk, the highest-performing ACOs in the program have been smaller, physician-only ACOs with relatively more primary care doctors and fewer specialists.
While the MSSP program has seen improved growth and savings coming out of the pandemic, the $1.8B in Medicare savings that it generated in 2022 represents only 0.2 percent of total Medicare spending last year.
UnitedHealth Group AI algorithm cutting off patient care
https://mailchi.mp/169732fa4667/the-weekly-gist-november-17-2023?e=d1e747d2d8

This week, Stat published a scathing investigation into the way UnitedHealth Group subsidiary NaviHealth uses an algorithm, nH Predict, to deny Medicare Advantage (MA) patients access to rehabilitation services and long-term care. United set a target to keep rehab stays within one percent of nH Predict’s projection for the year.
Interviews with former case managers and access to internal documents reveal that NaviHealth employees faced disciplinary action and even termination if they approved care that strayed from these algorithmic recommendations.
UnitedHealthcare, the nation’s largest insurer, is now subject to a class-action lawsuit filed this week over these practices. But NaviHealth’s impact extends beyond just United beneficiaries, as other insurers, covering around 15M MA enrollees, also use its services.
The Gist: This article provides a stark example of what can happen when an artificial intelligence (AI) algorithm is used not to complement, but to replace, clinical judgment.
While profit incentives in US healthcare are nothing new, what’s pernicious about an algorithm like nH Predict is how it replaces individual patients, whose needs vary, with a theoretical “average patient”, whose health and life needs can be easily predicted by the handful of data points available to the insurer.
When patients fail to recover along expected timelines—that are imperfectly calculated by incomplete datasets—they’re the ones who suffer.
Thought of the Day: On Which Path to Take
Thanksgiving Wishes
Private Equity’s Role in Health Care

Concerns over how private equity is affecting health care access, quality, and costs in the United States have exploded in the past few years, reflecting the growing activity of private investors in health care markets.
Private equity investors spent more than $200 billion on health care acquisitions in 2021 alone, and $1 trillion in the past decade. Private equity firms have long been active in hospital, nursing home, and home care settings. But recently, acquisitions of physician practices have skyrocketed, especially in high-margin specialties like dermatology, urology, gastroenterology, and cardiology. A recent study showed that in 13 percent of metropolitan areas, a single private equity firm owns more than half of the physician market for certain specialties.
Given their potential impact on the cost, quality, and access to health care in the U.S., these developments have generated considerable interest among federal and state policymakers.
What is private equity?
Strictly speaking, private equity in health care is a form of for-profit ownership reflecting investment in health care facilities by private parties. In general, for-profit health care organizations can take two forms: private or public.
- Public, investor-owned organizations sell shares to the public that trade on a stock exchange. UnitedHealth Group, which now owns thousands of physician practices, is one example. Another is Hospital Corporation of America. These organizations are regulated by multiple federal laws and agencies, including the U.S. Securities and Exchange Commission.
- Shares of private, investor-owned organizations — such as private equity–owned firms — are not traded on public markets. As such, they aren’t required to follow the same regulations as public companies.
As a form of ownership, private equity is not new to health care. A variety of private investors have invested in and owned health care facilities in the past. These have included individual physicians who invest in and own their for-profit private practices and pay taxes on their earnings. Physicians and other private investors have long owned health care facilities, such as specialty hospitals, dialysis units, ambulatory surgical centers, and imaging units.
What’s different now about private equity in health care?
There have been two key shifts in recent years. The first is in who’s doing the investing. Instead of physicians or small groups of investors using their own funds, investors now also include firms that manage funds for large groups of wealthy individuals or institutions. Fund managers and their investors may have little knowledge of health care, viewing it as just another market opportunity.
The second change relates to how they’re investing. Aggressively pursuing quick profits, some private equity firms are taking out loans, using their newly acquired health care facilities as collateral. The loans are used to pay back investors quickly and handsomely, while the health care organizations carry the debt. Another strategy is to sell the health care organization’s land, facilities, and other capital assets to other investors. The proceeds from the sales generate returns for fund managers and their investors. Health care organizations then rent those assets back from the new owners.
A third approach to getting a quick return is to flip the asset — selling the newly purchased health care organization to another buyer, such as a publicly traded company like CVS or Amazon, for a large multiple of the original price. To attract such a buyer, however, the private equity firm must boost the organization’s profits, which usually requires rapidly cutting costs, raising prices, or increasing the number of services provided.
All these strategies are legal, but until recently they hadn’t been deployed as widely or intensively in health care.
How does private equity impact health care costs, quality, and access?
More research is needed on how private equity ownership affects health care costs, quality, access, and equity. So far, the results on cost are clearest. Given its short-term financial focus, private equity tends to increase health care prices and utilization — and thus costs — to both patients and the larger society. Some new private owners of health care facilities may adopt reforms that make care more efficient and reduce costs, thus improving value. And there are examples of promising innovations, such as CareMore, a privately funded organization that reengineered care for high-risk elderly individuals. But in general, it’s much easier, and more common, for private owners to raise prices and volumes and to focus on high-margin services.
Regarding quality, there is no evidence that private equity ownership leads to systematic improvements in care. In fact, a widely cited study of nursing homes acquired by private equity owners showed a 10 percent increase in mortality among Medicare patients. However, there haven’t been additional studies demonstrating such dramatic, harmful effects.
In terms of access to care and equity, the financial pressures on acquired facilities to pay rent or repay loans are raising alarms about possible bankruptcies and closures of hospitals, nursing homes, and other health care facilities. This is especially concerning for those serving poor and rural communities, since these entities tend to be less lucrative financially.
Why are private equity firms investing in health care?
Several factors have driven private equity’s attraction to health care in recent years. One has been the low cost of capital resulting from low interest rates, which has spurred an influx of investors seeking to earn a piece of the $4 trillion health care economy.
A second factor has been the increasing commercialization of health care, which has made it more acceptable for private investors to treat health care — traditionally a nonprofit sector — like other markets. In fact, some nonprofit health care organizations have begun to look more and more like their for-profit brethren. Nonprofits have sought near-monopoly power in local markets through widespread mergers and acquisitions, which have enabled them to raise prices sharply. Compensation for nonprofit executives has also skyrocketed, as have their organizations’ capital reserves.
A third factor has been the ongoing failure of the U.S. health care system to deliver value and keep Americans healthy. With falling life expectancy, increasing maternal mortality, glaring inequities, soaring costs, and punishing medical debt, our health system is ripe for disruption. Private investors — with their energy, fresh perspective, and capital — offer hope for change.
What’s next for private equity in health care?
As interest rates rise and investors pick the low-hanging fruit in health care, it seems unlikely that private equity will maintain its current rate of expansion into the sector, at least for the short term. Public scrutiny of private investment in the health sector is also increasing, as concerns grow about the effects on costs, quality, equity, and access.
Policymakers’ first step in addressing these concerns will likely include new transparency rules to make it clear who owns private, for-profit health care organizations. Congress is considering such requirements, and the Security and Exchange Commission has issued a new rule requiring increased transparency about the identity of investors in private equity arrangements. It seems doubtful, however, that greater transparency rules alone could slow private equity’s penetration of health care markets.
Other potential changes include reforming antitrust laws to open the sale of local physician practices to scrutiny. The Federal Trade Commission recently sued a private equity firm that has been trying to dominate the anesthesia market in areas of Texas.
Some scholars believe that private equity serves as a divining rod for failures in our current health care market. Investors, they believe, are simply exploiting the system’s weaknesses for profit. In this sense, the growth of private equity is a symptom, not the cause, of our health system’s failure to meet the needs of Americans.
CommonSpirit reports Q1 $291M operating loss, $738M net loss

Chicago-based CommonSpirit Health, one of the largest nonprofit healthcare systems in the country, reported an adjusted operating loss of $291 million on revenue of $8.9 billion for the first quarter of fiscal 2024, ending Sept. 30.
The adjusted figure reflects the effects of the California provider fee program. Without such an adjustment, the system reported an operating loss of $441 million versus a $23 million gain the previous year.
The adjusted figures compared with an operating loss of $227 million in the same period last year with revenue of $8.5 billion. Salaries and benefits increased $174 million over the prior year period, or 3.9%.
The overall net loss for the 142-hospital system totaled $738 million as CommonSpirit reported net investment losses of $289 million.
“Despite significant industry and economic headwinds, CommonSpirit was able to extend the momentum achieved in the previous quarter,” CFO Dan Morissette said in a statement. “While this is encouraging, we take nothing for granted. More efforts are underway to provide the strong financial foundation this health ministry needs to provide care to everyone in the communities we serve, including the most vulnerable.”



