https://www.healthleadersmedia.com/finance/winners-and-losers-healthcares-q4-earnings-season

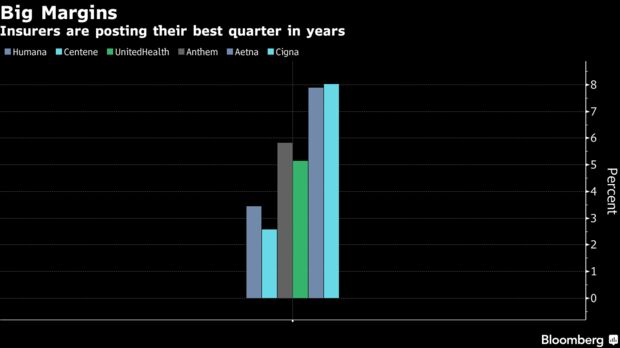
Healthcare companies have reported their earnings from the final quarter of 2018, revealing some success stories and some ongoing struggles.
Earnings season for Q4 2018 has concluded for companies across the healthcare industry, from insurers, for-profit providers, telemedicine companies, and others in between.
Given the challenging market conditions during the final quarter of last year, including the surprise federal ruling that struck down the Affordable Care Act as unconstitutional, many companies reported weaker earnings than they did earlier in 2018.
However, some were buoyed by new intitiatives and product performance that sustained a level of success they intend to carry into 2019.
Below is a list of healthcare’s winners and losers from the 2018 Q4 earnings season:
WINNERS:
- The Minnetonka, Minnesota-based insurer led the pack again, ending 2018 on an upswing thanks to Optum’s record-breaking performance.
- The PBM subsidiary recorded year-end revenues above $100 billion for the first time ever.
- Based United expects to achieve revenues above $240 billion in 2019.
- 2018 was a strong year for the St. Louis-based insurer, finishing with more than $60.1 billion in revenues.
- Managed care membership reached 14 million, an increase of 15% year-over-year.
- Centene’s net earnings for Q4 2018 were $241 million, an increase of $11 million year-over-year.
- IngenioRX, Anthem’s PBM slated for debut in 2020, is now expected to launch in Q2.
- The subsidiary is expected to achieve gross annual savings north of $4 billion, including more than 20% returned to shareholders.
- Anthem added 37,000 medical enrollment members in Q4, and saw its operating gain grow by 30% year-over-year.
MIDDLE:
- The Purchase, New York-based telemedicine company produced revenues of $122 million and saw total visits rise by 70% while net losses fell.
- The company still has sizable net losses to account for, posting a net loss of nearly $25 million in Q4 and $97.1 million for the full year.
- Despite some positive financial metrics, Teladoc’s issued a tepid financial guidance for 2019.
- While we still wait on final federal approval for the megamerger set to drastically change the healthcare landscape, CVS Health posted its earnings report from a difficult Q4.
- The Aetna merger played a role in rising revenues by 12.5% for CVS in the last quarter of 2018, but it also hampered some crucial metrics.
- CVS suffered a net loss of $421 million in Q4 2018 and $596 million during the full year.
- However, CEO Larry Merlo said he believes CVS’ acquisition of Aetna provides the company with “long-term value” in a rapidly transforming market.
- As with CVS, a megamerger couldn’t save Cigna from a down quarter to wrap up 2018.
- The Philadelphia-based insurer produced $14.3 billion in total quarterly revenues and $144 million in net income, but failed to meet earnings estimates after closing its deal with Express Scripts.
- Overall, Cigna capped off 2018 with total adjusted revenues of $48 billion, a 15% year-over-year increase, along with a net income of $3.6 billion.
LOSERS:
- Amidst lingering divestiture activity, CHS posted a net loss of more than $325 million.
- CHS recorded a net loss attributable to shareholders of $328 million in Q4 2018, down from a net loss of more than $2 billion during Q4 2017.
- On one positive note, the the Franklin, Tennessee-based for-profit hospital operator did manage net operating revenues of $3.5 billion, an increase of nearly $400 million year-over-year.
- Tenet experienced a net loss of $5 million in Q4 and saw its full year operating revenues decline 4.5%.
- The Dallas-based company’s quarterly adjusted EBITDA fell 34.6% year-over-year.
- CEO Ron Rittenmeyer praised the “significant progress” Tenet made to “create a more efficient, agile enterprise with new leadership.”
- Segment profit fell to $16 million in Q4, down 83.8% year-over-year, and only reached $228 million in 2018, a 26.7% drop.
- Net revenues for 2018 did increase more than 25%, a lone bright spot for Magellan.
- CEO Barry Smith remains confident despite the significant financial declines over the past year.