http://www.healthcarefinancenews.com/news/cigna-teams-cvs-health-collaboration-rival-urgent-care-clinics?mkt_tok=eyJpIjoiTXpVelkyRXhZMkpqTmpKaSIsInQiOiJFVjFscVRVVDdXZmZqek02STNMSVNjelwvREEwMmZmckZrWmNyZjNrQnVcL0szTGZuNXA4ZGdrOGRhT1V5bnREanBwWitPbTNkQllLZW5BTmd4VDk5TDg0ak1NNStnTllqdEllQlNpQmRZbDUwcm5JdVNaZ1lJcmpVVXJNYWxcL0JcL28ifQ%3D%3D

Cigna expects to save money on urgent care and emergency room visits through a new collaboration with CVS Health called Cigna Health Works..
In June, the insurer and CVS Health announced the initiative for Cigna’s self-funded employer-sponsored health plans.
Retail pharmacies are competing against traditional providers by offering convenient walk-in clinics.
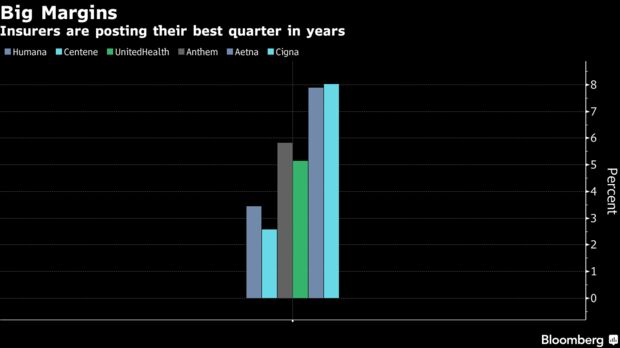
Cigna Health Works offers patients an alternative to urgent care and emergency room visits, the insurer said. Roughy 45 percent of urgent care facility visits by its members could be conducted at retail clinics, potentially reducing healthcare costs by 81 percent per visit, Cigna said.
The collaboration aligns Cigna-administered health benefits with CVS Pharmacyand CVS MinuteClinic retail healthcare services.
“This new model is based on how the customer wants to consume health care — it’s about creating value and a new way for healthcare consumers to get more from their health plan, by ensuring that we are there for them at the places they prefer to go for convenient care,” said Michele Paige, vice president and general manager of Cigna Onsite Health.
“As the popularity of retail health care continues to rise, Cigna Health Works is designed to help improve healthcare quality and address potential gaps in care. In some markets, up to one-third of Cigna customers have used some form of retail health care within a year’s time.”
Cigna Health Works can help patients who do not have a primary care doctor to find one by providing a list of Cigna-contract physicians from the health plan’s provider network.
CVS MinuteClinic nurse practitioners can offer pre-diabetic health screening, acute episodic care at discounted rates, as well as low cost A1C blood sugar testing, with the drugs available at CVS.
The nurse practitioner can ensure that an electronic record of each visit to CVS MinuteClinic is sent to the PCP‘s office.
“This new level of collaboration with Cigna is a part of the growing trend toward consumer-directed care,” said Helena Foulkes, president of CVS Pharmacy. CVS Health, a pharmacy benefit manager, has nearly 9,700 retail locations and more than 1,100 walk-in medical clinics nationwide.
It is among the country’s top pharmacies that also include Walgreens, Walmart, Rite Aid and Kroger.
In November, CVS Health partnered with OptumRx, UnitedHealth’s pharmacy benefit manager business. OptumRx consumers are able to fill 90-day prescriptions at CVS for prices that compete with home delivery copays.
Walgreens formed a similar deal with OptumRx.
Cigna Health Works beneficiaries get personalized pharmacy support through Health Tag Messages on the prescription bag to advise patients of needed health actions by the pharmacist or clinician, and provide information on available Cigna health and wellness coaching services included in their Cigna plan at no additional cost.
They get contracted discounts at CVS MinuteClinic for select preventive and acute care, including biometric screenings for blood pressure, cholesterol and blood sugar as well as diagnosis and treatment for minor illnesses such as bronchitis, ear infections and strep throat.
Consumers get an exclusive 20 percent discount on CVS health brand over-the-counter products through the CVS ExtraCare Health card. This program can be coupled with Cigna 90 Now, which offers 90-day refills for maintenance prescriptions to help improve patient adherence to their medication regimen.
The personalized health and wellness program is being offered in select markets for U.S. Cigna-administered employer-sponsored medical plans.