An estimated 2 percent of the increase will be due to the return on the health insurance tax.
Insurers are projected to submit rate increases in the Affordable Care Act market of about 10 percent, which is higher than the roughly 6 percent increase for 2019, according to Dave Dillon, a fellow of the Society of Actuaries and senior vice president of Lewis & Ellis, Actuaries and Consultants.
An estimated 2 percent of the increase will be due to the return on the health insurance tax. Medical inflation will account for 4-8 percent of the increase, which Dillon called a normal annual trend reflecting the underlying growth in healthcare costs.
Another 1 to 2 percent will be due to the decrease in the level of the premium tax credits. A reduction in the exchange user fee for federal and state-based exchanges will allow for a .5 to 1 percent decrease in rates.
Many factors play a role in rate setting, making predictions somewhat of an educated guess. But Dillon believes one issue that won’t be a factor, unless the court hands up a decision very soon, is the question of the constitutionality of the ACA being weighed in the Fifth Circuit Court of Appeals in Texas.
The Department of Justice recently said the ACA in its entirety should be struck down, now that the individual mandate is gone.
“While there’s a lot of topics going on, they’re not necessary ones that affect 2020 rates,” Dillon said. “The Texas case hangs over everybody but not as an actionable item right now.”
Neither is the Medicare for All debate likely to influence premiums for 2020, he said.
WHY THIS MATTERS
Insurers are getting ready to file their 2020 premium rates for the on-exchange market of the ACA.
Depending on the state, such as Vermont and the District of Columbia, which have deadlines this month, the filing season kicks into high gear during the first and second weeks of June. Other states, such as Arkansas, have a deadline in July, said Dillon, who works with about 10 states on rates.
Off-exchange rates are due later in summer.
Rates will vary by state and would be influenced by a state’s implementation of 1332 waivers to allow for less expansive plans. So far, no state has taken advantage of the waivers that the Centers for Medicare and Medicaid Services began offering last fall, according to The Washington Post.
TREND
ACA premium rates stabilized for 2019 and insurers returned to the market or expanded their coverage areas.
In making his prediction for rates for 2020, Dillon looked at medical loss ratios and profit margins from the 2018 season. These were stable compared to 2017 when insurers were filing two sets of rates depending on whether cost-sharing reduction payments would be continued under the Trump Administration.
President Trump did end the CSRs. However, to make up for the loss to insurers and to lower premium increases, the Department of Health and Human Services allowed insurers in the 2019 season and again for 2020, to silver load premium increases onto silver level plans. Since most beneficiaries get the benefit of federal subsidies for health insurance through the ACA, the federal government is still bearing the cost of allowing insurers to offer lower rates.
Unlike other years, Dillon said he’s not hearing a lot about the market, which he interprets as a stabilizing trend. Insurers aren’t coming in and out of the markets as much. Regional companies may be expanding into other states, but there’s been no talk of another large insurer getting in, he said.
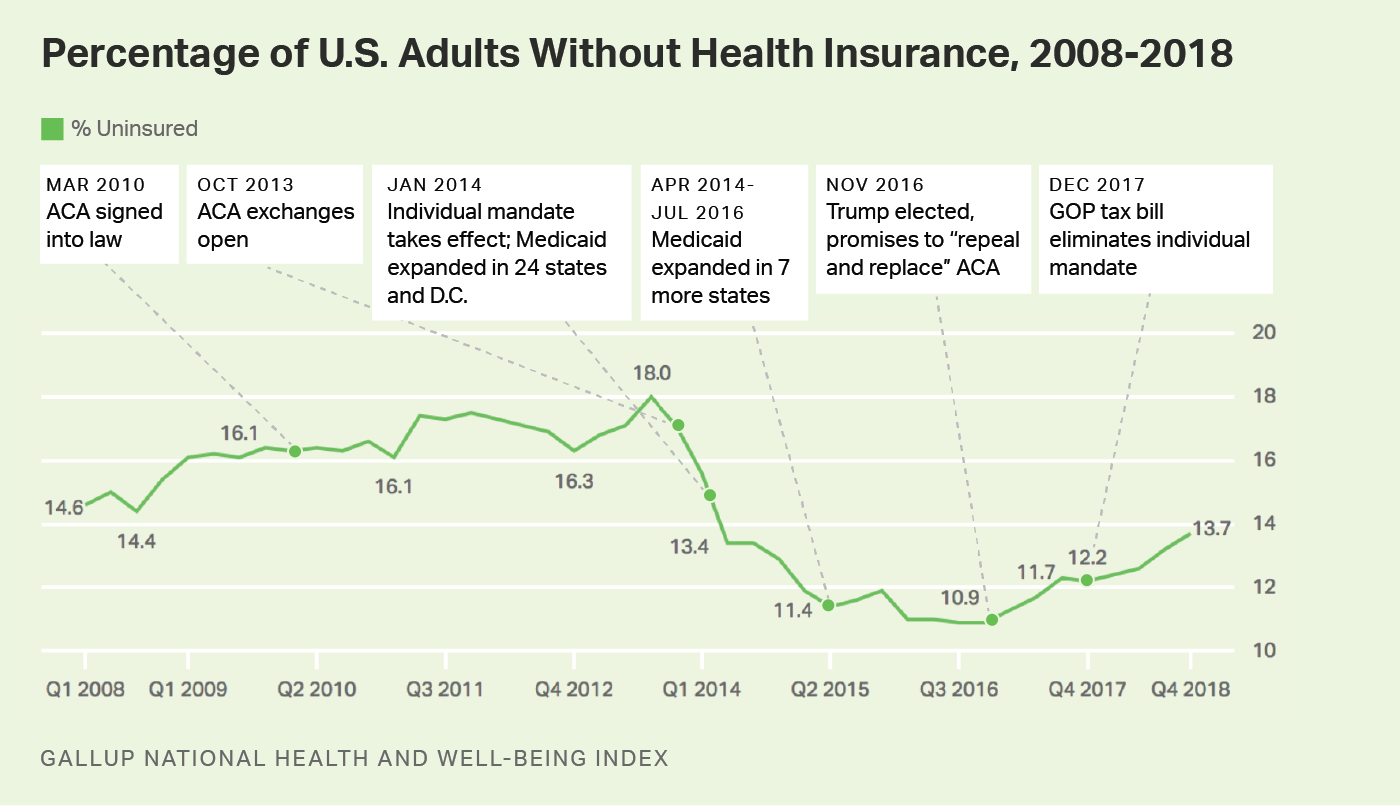
“I think we’re on the path to gaining some traction and stability,” Dillon said. “Obviously the ACA has put us at lowest uninsured rate ever.”
ON THE RECORD
“Consistent with previous years, insurance rates will vary widely across individual states and marketplaces,” Dillon said.