
With efforts to repeal the Affordable Care Act dead in Congress for now, a critical test for the law’s future is playing out in one small, conservative-leaning state.
Iowa is anxiously waiting for the Trump administration to rule on a request that is loaded with implications for the law’s survival. If approved by the federal Centers for Medicare and Medicaid Services, it would allow the state to jettison some of Obamacare’s main features next year — its federally run insurance marketplace, its system for providing subsidies, its focus on helping poorer people afford insurance and medical care — and could open the door for other states to do the same.
Iowa’s Republican leaders think their plan would save the state’s individual insurance market by making premiums cheaper for everyone. But critics say the lower prices come at the expense of much higher deductibles for many with modest incomes, and that approval of the plan would amount to another way of undermining the law. Already the administration has slashed funding for advertising and outreach to help people sign up for insurance, and President Trump is preparing to issue an executive order allowing more access to plans that don’t meet the law’s standards.
Adding to the uncertainty, the Washington Post reported last week that Mr. Trump in August asked Seema Verma, the federal official in charge of reviewing Iowa’s plan, to reject it. Some supporters of the law saw that as a deliberate effort to keep premiums high; Mr. Trump frequently cites sharply rising premiums as proof that the health law is failing.
Neither C.M.S. nor the White House would comment on whether Mr. Trump had pushed for the application to be denied. A spokeswoman for C.M.S. said only that the plan remains under review.
In Des Moines on Tuesday, Gov. Kim Reynolds told reporters that her team was in constant contact with the White House and C.M.S. about the plan, including a call with Ms. Verma this week, trying “to get to yes.” She said the administration has been “very receptive” to the plan as a solution to the “unaffordable,” “unworkable” health law until it can be repealed.
Iowa calls its request a stopgap plan that would allow the state to opt out of the federal health insurance marketplace, HealthCare.gov, for 2018 and create a state-run system that its insurance commissioner says would lower premiums for the 72,000 Iowans who currently have Obamacare health plans, including 28,000 who earn too much to get subsidies to help with the cost.
But the cheaper premiums would come with a big trade-off: higher out-of-pocket costs. The only option for customers would be a plan with deductibles of $7,350 for a single person and $14,700 for a family. The proposal would also reallocate millions of federal dollars that the health law dedicates to lowering costs for people with modest incomes and use the money for premium assistance to those with higher incomes, no matter how much money they make.
The individual insurance market is particularly fragile in Iowa, partly because the state has allowed tens of thousands of people to keep old plans that do not meet the health law’s standards. Aetna and Wellmark Blue Cross & Blue Shield, the state’s most popular insurer, are both withdrawing at the end of the year. The only insurer planning to remain, Medica, is seeking premium increases that average 56 percent, blaming Mr. Trump’s ongoing threats to stop paying subsidies known as cost-sharing reductions that lower many people’s deductibles and other out-of-pocket costs. Wellmark has said it will stay if the stopgap plan is approved.
“What we are trying to address is a really large number of people being priced out,” said Doug Ommen, the state’s Republican insurance commissioner.
Two other states, Alaska and Minnesota, have already won permission to shore up their Obamacare markets with waivers allowed under the law; they will use federal money to help insurers cover the claims of their most expensive customers next year. But Oklahoma abruptly withdrew a similar request in late September — one that state officials said would have reduced premiums by an average of 30 percent — saying that the Trump administration had reneged on a promise to approve it by Sept. 25 and they were out of time. (A C.M.S. spokeswoman said, “At no time was an approval package or an approval date ever agreed upon.”)
Iowa’s waiver request is more far-reaching, providing what Timothy S. Jost, an emeritus professor of health law at Washington and Lee University, has called a “watershed moment” for Obamacare.
“It’s a decision to abandon a number of key principles of the Affordable Care Act,” he said.
Under the law, people who don’t get insurance through work can buy it through the online marketplace. They get federal subsidies to help with the cost if their income is below 400 percent of the poverty level, or about $65,000 a year for a couple. Those whose incomes are below 250 percent of the poverty level — $40,600 a year for a couple — also get cost-sharing reductions.
Iowa’s plan would reallocate much of that federal assistance, using it to provide premium subsidies based on age and income for even the wealthiest individual market customers. It would also be used to create a “reinsurance” program, like Alaska’s and Minnesota’s, to help insurers cover their sickest customers. The law’s essential health benefits and protections for people with pre-existing conditions would remain in place, but every individual market customer would get the same standardized high-deductible plan.
Mr. Jost and other supporters of the law say Iowa’s proposal does not meet the requirements for so-called innovation waivers, including that the coverage they provide must be at least as comprehensive and affordable as Obamacare plans, because poorer people would face higher deductibles and other out-of-pocket costs. That, they say, leaves the plan open to almost-certain legal challenges.
Seemingly acknowledging that problem, Mr. Ommen has tweaked Iowa’s proposal — including with a supplemental filing to the Trump administration on Thursday — to preserve subsidies that reduce out-of-pocket costs for roughly 21,000 low-income Iowans.
But those at slightly higher income levels would lose cost-sharing assistance completely, facing the $7,350 deductible and other out-of-pocket expenses.
“You still have some real problems from the perspective of making sure low-income people can afford coverage,” said Joel Ario, a managing director at Manatt Health who worked on the Affordable Care Act at the Department of Health and Human Services during the Obama administration.
But for the roughly 28,000 Iowans who have Obamacare coverage but earn too much to get subsidies, the need for a shake-up is urgent. And with open enrollment starting in about three weeks, time is of the essence.
Dozens of them, including many farmers, submitted comments to Mr. Ommen or testified at public hearings in favor of the stopgap plan, with many saying they would be forced to drop their insurance next year if it were not approved.
“Fortunately both my husband and I have already prepaid our funeral expenses,” write a woman identified as Nancy K., of Bellevue, who said she could no longer afford her coverage. “Every single item, even our cemetery marker, is paid for or covered for my death in the event that we cannot afford insurance to pay for any so-called catastrophic health care.”
Landi Livingston, whose family raises beef cattle in rural southern Iowa, said she was paying almost $500 a month for a Wellmark plan and dreaded having to switch to Medica next year, with what she assumed would be significantly higher prices.
If the Trump administration approves the state’s request, Ms. Livingston’s premium would likely drop to around $350 a month, according to estimates from the state, saving her $1,800 next year. But her $3,000 deductible would more than double, meaning that if she had high medical expenses she could end up paying more toward those bills.
“I still think it’s the best thing on the table right now,” she said of the stopgap plan. “It’s high time the people in power get this figured out.”
For Tony Ross, a retired paralegal in Des Moines who has a subsidized marketplace plan from Aetna, the stopgap plan would lower his premiums to about $85 a month, from $220, according to the state estimates. But his deductible – currently $750 because his low income qualifies him for cost-sharing reductions – would balloon by almost tenfold. That would mean paying thousands more each year for his expensive blood pressure medication, he said.
“Obviously I need a way lower deductible than $7,350,” said Mr. Ross, 63. “This doesn’t seem like a fair way of fixing things.”


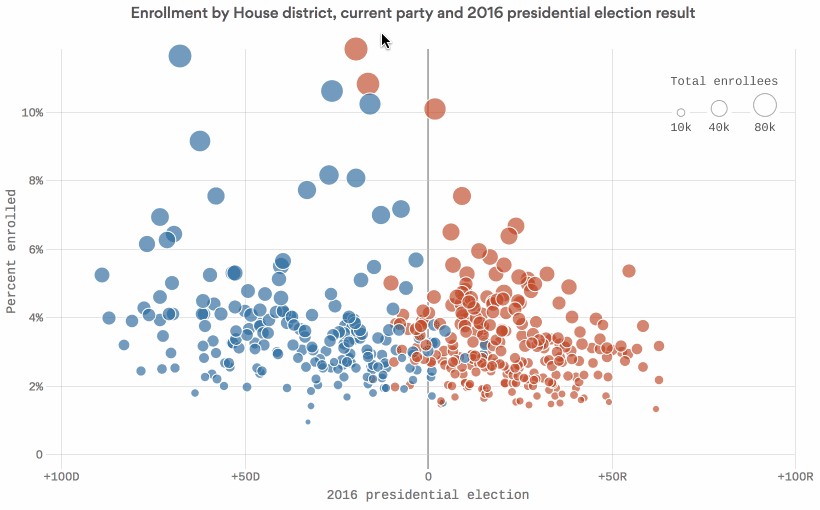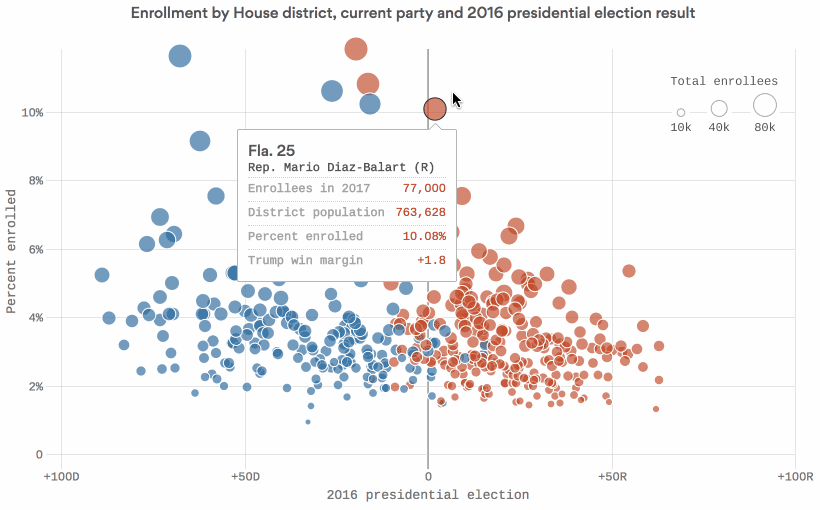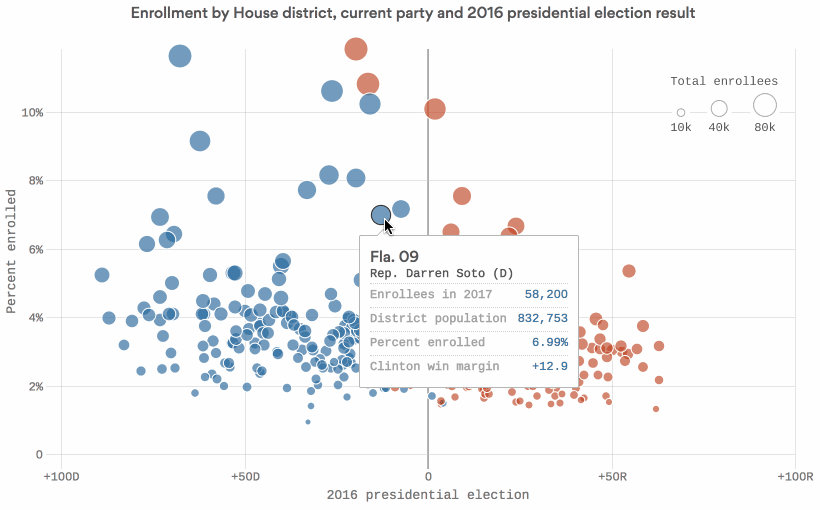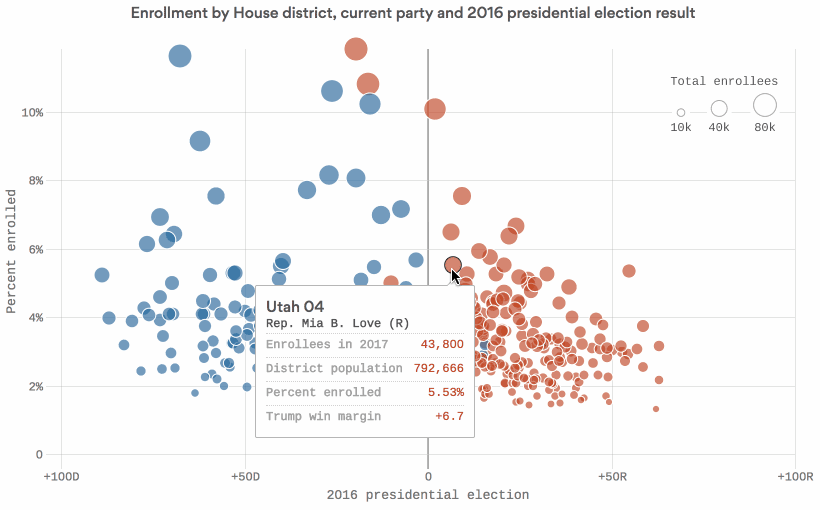 Data: Kaiser Family Foundation; Daily Kos Elections; Census Bureau; Chart: Chris Canipe / Axios
Data: Kaiser Family Foundation; Daily Kos Elections; Census Bureau; Chart: Chris Canipe / Axios





