https://mailchi.mp/0622acf09daa/the-weekly-gist-december-2-2022?e=d1e747d2d8
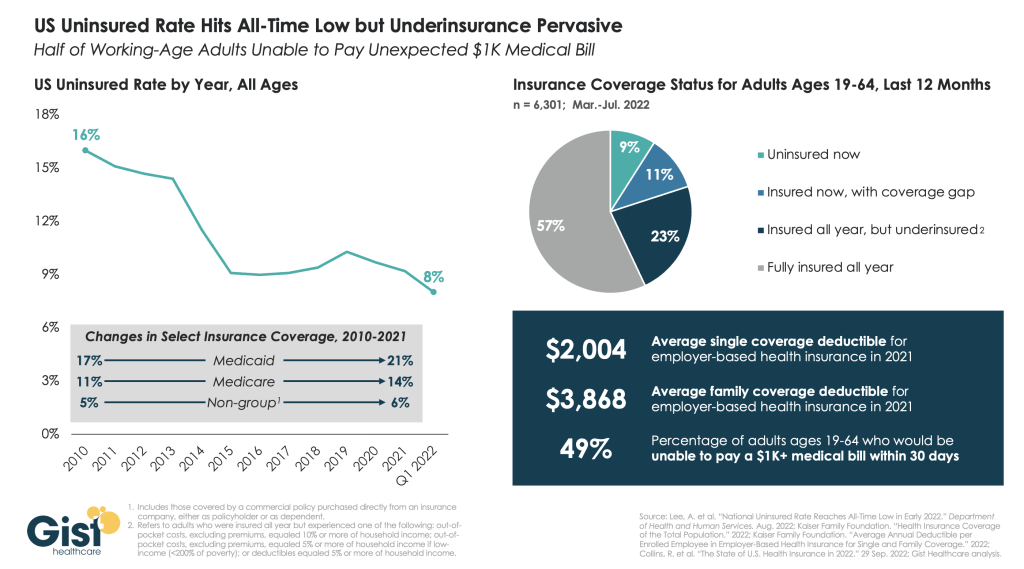
Driven by the steady progress of Medicaid expansion and pandemic-era policies to ensure access to health insurance coverage, the US uninsured rate hit an all-time low of 8 percent in early 2022. Since the Affordable Care Act passed in 2010, the US uninsured rate has been cut in half, with the largest gains coming from Medicaid expansion.
However, using data from Commonwealth Fund, the graphic below illustrates how this noteworthy achievement is undermined by widespread underinsurance, defined as coverage that fails to protect enrollees from significant healthcare cost burdens. A recent survey of working-age adults found that eleven percent of Americans experienced a coverage gap during the year, and nearly a quarter had continuous insurance, but with inadequate coverage.
High deductibles are a key driver of underinsurance, with average deductibles for employer-sponsored plans around $2,000 for individuals and $4,000 for families.
Roughly half of Americans are unable to afford a $1,000 unexpected medical bill. Americans’ healthcare affordability challenges will surely worsen once the federal COVID public health emergency ends, because between 5M and 14M Medicaid recipients could lose coverage once the federal government ends the program that has guaranteed continuous Medicaid eligibility.
The process of eligibility redeterminations is sure to be messy—while some Medicaid recipients will be able to turn to other coverage options, the ranks of uninsured and underinsured are likely to swell.

