
As of Sunday, there are 35 confirmed cases of measles in the state of Washington — an outbreak that has already prompted Gov. Jay Inslee to declare a state of emergency.

As of Sunday, there are 35 confirmed cases of measles in the state of Washington — an outbreak that has already prompted Gov. Jay Inslee to declare a state of emergency.
Healthcare Triage: The 2017 Flu Killed 80,000 in the US. Get a Flu Shot!

Influenza killed 80,000 people last year in the United States. That is the highest number of deaths since the CDC started keeping records in the 1970s. Help protect yourself and those around you. Get a flu shot!

Duluth, Minn.-based Essentia Health rolled out a mandatory flu shot policy last year, and the health system will continue the program this year.
Under the program, employees had until Nov. 20, 2017, to receive a flu shot, obtain a medical/religious exemption or face termination. Essentia reported more than 99.5 percent compliance with the program.
For 2018, Essentia will continue its mandatory flu shot program, which also applies to students who train and vendors who operate at the health system’s facilities, as well as people who volunteer through Essentia programs.
To ensure there is plenty of time to review medical/religious exemptions before this year’s Nov. 20 compliance deadline, Essentia moved up the deadline to submit exemption requests.
“The first year [is] the most difficult because everyone [is] doing first-time medical and religious exemption requests,” said Rajesh Prabhu, MD, infectious disease and chief patient quality and safety officer for the system. “Those granted medical exemptions last year still [have their medical exemptions] in place. For religious exemptions, they just have to confirm their belief hasn’t changed from last year.”
He expects compliance to increase this year since fewer people need to request medical exemptions for the first time. Essentia now has 14,700 employees and began its flu shot campaign Oct. 2.
Dr. Prabhu encouraged other systems or hospitals considering a mandatory flu shot program to focus on the reasoning behind beginning the program.
“It’s not just a technical change. You have to get everyone to feel why this is important for not only our employees but [also] the patients we serve. We focus a lot of efforts on that end,” he said.
Dr. Prabhu said support from leadership helped make the first year of Essentia’s mandatory flu shot program a success.
“We had support from our CEO and everyone in leadership,” he said. “[They had] direct, in-person communication with some of those hesitant to get vaccinated because sometimes it’s good to talk to people to understand their concerns and barriers.”
Lessons learned
Essentia announced its mandatory flu shot program in September 2017 and some employees felt they didn’t get enough notice to comply. However, Dr. Prabhu said he believes some employees would not have complied with the program even if they were given more time.
“No matter how much lead time you give, I don’t think it will change the minds of people who are resistant to get the influenza vaccine,” he said.
Essentia’s flu shot policy encountered opposition from unions as well. The Minnesota Nurses Association and some other labor groups that represent Essentia employees continue to challenge the flu shot policy. In July, an arbitrator sided with Essentia over the United Steelworkers Union regarding the policy.
Despite the opposition and a few challenges in the initial rollout, Dr. Prabhu said Essentia needed the policy. He said the system was not going to get to where it wanted to be with its previous voluntary policy, which had 82 percent compliance. And, after evaluating the first year, Essentia decided it was necessary to continue the policy into the 2018-19 flu season.
2018-19 flu season
For this flu season, the CDC recommends everyone 6 months and older receive a flu vaccine by the end of October. Nasal spray FluMist was not recommended last season, but it is recommended for 2018-19 as an option for flu vaccination of nonpregnant individuals age 2 to 49.
It’s unclear how severe the 2018-19 flu season will be. Last year’s flu season was particularly severe, with about 900,000 people hospitalized and about 80,000 people dead due to the virus.
Dr. Prabhu said the flu season hasn’t hit the Duluth area yet, but Essentia is trying to do everything possible to prevent the spread of the virus among patients and staff.
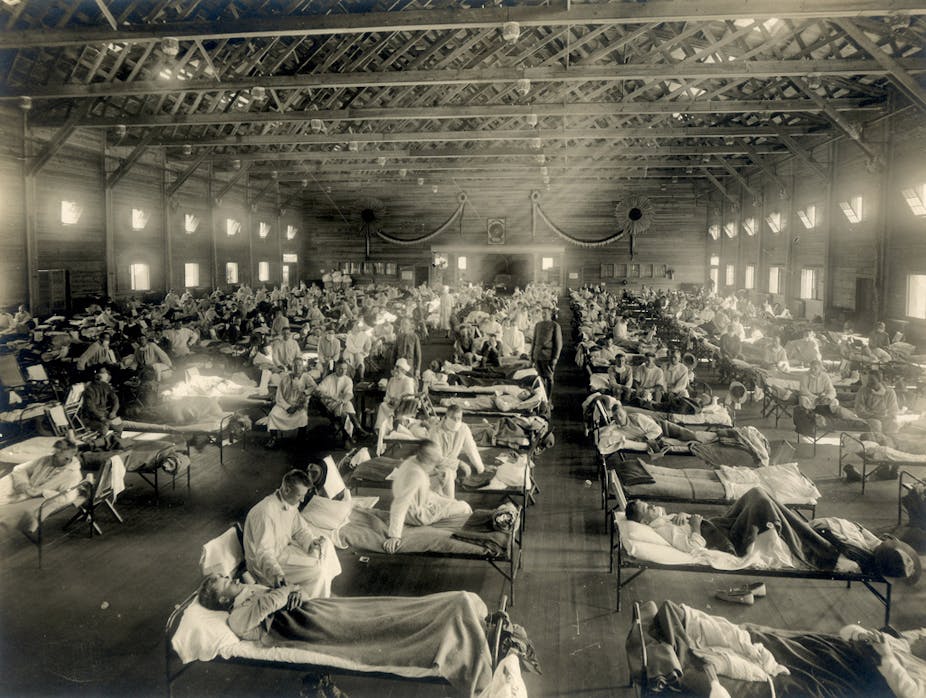
Vaccination is underway for the 2017-2018 seasonal flu, and next year will mark the 100-year anniversary of the 1918 flu pandemic, which killed roughly 40 million people. It is an opportune time to consider the possibility of pandemics – infections that go global and affect many people – and the importance of measures aimed at curbing them.
The 1918 pandemic was unusual in that it killed many healthy 20- to 40-year-olds, including millions of World War I soldiers. In contrast, people who die of the flu are usually under five years old or over 75.
The factors underlying the virulence of the 1918 flu are still unclear. Modern-day scientists sequenced the DNA of the 1918 virus from lung samples preserved from victims. However, this did not solve the mystery of why so many healthy young adults were killed.
I started investigating what happened to a young man who immigrated to the U.S. and was lost during World War I. Uncovering his story also brought me up to speed on hypotheses about why the immune systems of young adults in 1918 did not protect them from the flu.
Certificates picturing the goddess Columbia as a personification of the U.S. were awarded to men and women who died in service during World War I. One such certificate surfaced many decades later. This one honored Adolfo Sartini and was found by grandnephews who had never known him: Thomas, Richard and Robert Sartini.
The certificate was a message from the past. It called out to me, as I had just received the credential of certified genealogist and had spent most of my career as a scientist tracing a gene that regulates immune cells. What had happened to Adolfo?
To follow up, I posted a query on the “U.S. Militaria Forum.” Here, military history enthusiasts explained that the Army Corps of Engineers had trained men at Camp A. A. Humphreys in Virginia. Perhaps Adolfo had gone to this camp?A bit of sleuthing identified Adolfo’s ship listing, which showed that he was born in 1889 in Italy and immigrated to Boston in 1913. His draft card revealed that he worked at a country club in the Boston suburb of Newton. To learn more, Robert Sartini bought a 1930 book entitled “Newton War Memorial” on eBay. The book provided clues: Adolfo was drafted and ordered to report to Camp Devens, 35 miles from Boston, in March of 1918. He was later transferred to an engineer training regiment.
While a mild flu circulated during the spring of 1918, the deadly strain appeared on U.S. soil on Tuesday, Aug. 27, when three Navy dockworkers at Commonwealth Pier in Boston fell ill. Within 48 hours, dozens more men were infected. Ten days later, the flu was decimating Camp Devens. A renowned pathologist from Johns Hopkins, William Welch, was brought in. He realized that “this must be some new kind of infection or plague.” Viruses, minuscule agents that can pass through fine filters, were poorly understood.
With men mobilizing for World War I, the flu spread to military installations throughout the U.S. and to the general population. It hit Camp Humphreys in mid-September and killed more than 400 men there over the next month. This included Adolfo Sartini, age 29½. Adolfo’s body was brought back to Boston.
His grave is marked by a sculpture of the lower half of a toppled column, epitomizing his premature death.
The quest to understand the 1918 flu fueled many scientific advances, including the discovery of the influenza virus. However, the virus itself did not cause most of the deaths. Instead, a fraction of individuals infected by the virus were susceptible to pneumonia due to secondary infection by bacteria. In an era before antibiotics, pneumonia could be fatal.
Recent analyses revealed that deaths in 1918 were highest among individuals born in the years around 1889, like Adolfo. An earlier flu pandemic emerged then, and involved a virus that was likely of a different subtype than the 1918 strain. These analyses engendered a novel hypothesis, discussed below, about the susceptibility of healthy young adults in 1918.
Support for this hypothesis was seen with the emergence of the Hong Kong flu virus in 1968. It was in “Group 2” and had severe effects on people who had been children around the time of the 1918 “Group 1” flu.Exposure to an influenza virus at a young age increases resistance to a subsequent infection with the same or a similar virus. On the flip side, a person who is a child around the time of a pandemic may not be resistant to other, dissimilar viruses. Flu viruses fall into groups that are related evolutionarily. The virus that circulated when Adolfo was a baby was likely in what is called “Group 2,” whereas the 1918 virus was in “Group 1.” Adolfo would therefore not be expected to have a good ability to respond to this “Group 1” virus. In fact, exposure to the “Group 2” virus as a young child may have resulted in a dysfunctional response to the “Group 1” virus in 1918, exacerbating his condition.
What causes a common recurring illness to convert to a pandemic that is massively lethal to healthy individuals? Could it happen again? Until the reason for the death of young adults in 1918 is better understood, a similar scenario could reoccur. Experts fear that a new pandemic, of influenza or another infectious agent, could kill millions. Bill Gates is leading the funding effort to prevent this.
Flu vaccines are generated each year by monitoring the strains circulating months before flu season. A time lag of months allows for vaccine production. Unfortunately, because the influenza virus mutates rapidly, the lag also allows for the appearance of virus variants that are poorly targeted by the vaccine. In addition, flu pandemics often arise upon virus gene reassortment. This involves the joining together of genetic material from different viruses, which can occur suddenly and unpredictably.
An influenza virus is currently killing chickens in Asia, and has recently killed humans who had contact with chickens. This virus is of a subtype that has not been known to cause pandemics. It has not yet demonstrated the ability to be transmitted from person to person. However, whether this ability will arise during ongoing virus evolution cannot be predicted.
The chicken virus is in “Group 2.” Therefore, if it went pandemic, people who were children around the time of the 1968 “Group 2” Hong Kong flu might have some protection. I was born much earlier, and “Group 1” viruses were circulating when I was a child. If the next pandemic virus is in “Group 2,” I would probably not be resistant.
It’s early days for understanding how prior exposure affects flu susceptibility, especially for people born in the last three to four decades. Since 1977, viruses of both “Group 1” and “Group 2” have been in circulation. People born since then probably developed resistance to one or the other based on their initial virus exposures. This is good news for the near future since, if either a “Group 1” or a “Group 2” virus develops pandemic potential, some people should be protected. At the same time, if you are under 40 and another pandemic is identified, more information would be needed to hazard a guess as to whether you might be susceptible or resistant.
http://www.businessinsider.com/pandemic-risk-to-humanity-2017-9
http://www.globalgoals.org/goalkeepers/datareport/

As hurricanes and other natural disasters ravage the world and the threat of nuclear war looms, it’s hard to assess which risks for humanity are really the scariest right now.
But one of the biggest threats out there is one of the oldest: infectious disease, which can emerge naturally or be human-made, as in a case of bioterrorism.
As Bill and Melinda Gates wrote in their recently released “Goalkeepers” report, disease — both infectious and chronic — is the biggest public health threat the world faces in the next decade. And although Gates said on a press call that “you can be pretty hopeful there’ll be big progress” on chronic disease, we are still unprepared to deal with the infectious variety.
Gates has repeatedly stated that he sees a pandemic as the greatest immediate threat to humanity on the planet.
“Whether it occurs by a quirk of nature or at the hand of a terrorist, epidemiologists say a fast-moving airborne pathogen could kill more than 30 million people in less than a year,” Gates wrote in an op-ed for Business Insider earlier this year. “And they say there is a reasonable probability the world will experience such an outbreak in the next 10-15 years.”
Gates is right about the gravity of that threat, according to experts in the field.
George Poste is an ex officio member of the Blue Ribbon Study Panel on Biodefense, a group created to assess the state of biodefense in the US,.
“We are coming up on the centenary of the 1918 influenza pandemic,” he told Business Insider. “We’ve been fortunately spared anything on that scale for the past 100 years, but it is inevitable that a pandemic strain of equal virulence will emerge.”
The 1918 pandemic killed approximately 50 million people around the globe, making it one of the deadliest events in human history.
David Rakestraw, a program manager overseeing chemical, biological and explosives security at Lawrence Livermore National Laboratory, and Tom Slezak, the laboratory’s associate program leader for bioinformatics, also agree with Gates.
“Both natural and intentional biological threats pose significant threats and merit our nation’s attention to mitigate their impact,” they told Business Insider in an email.
It’s possible that a major outbreak could be intentionally created as the result of a biological weapon, but Poste thinks a serious bioterrorism attack is unlikely due to the complexity of pulling something like that off.
It’s very likely, however, that a highly dangerous disease would naturally emerge — and the consequences of that pandemic would be just as severe.
Regardless of how a disease starts to spread, preparedness efforts for pandemics are the same, according to Poste. And the recent outbreaks of Zika and Ebola have highlighted the need for more heightened disease surveillance capabilities. We’re still getting a handle on the health effects of Zika — and it seems like the mosquito-borne disease may be even more severe than we thought.
Experts have long advocated for better ways to recognize emerging threats before they become epidemics or pandemics. Poste also said we need to improve rapid diagnostic tests and get better at developing new therapeutics and vaccines — something Gates highlighted as a weakness in the “Goalkeepers” report as well.
Until that happens, that threat remains far more real than many of us realize.
http://www.latimes.com/nation/nationnow/la-na-houston-chemical-plant-20170831-story.html
The pounding rains of Hurricane Harvey washed over the conduits, cooling towers, ethylene crackers and other esoteric equipment of the nation’s largest complex of chemical plants and petroleum refineries, leaving behind small lakes of brown, foul-smelling water whose contents are a mystery.
Broken tanks, factory fires and ruptured pipes are thought to have released a cocktail of toxic chemicals into the waters. Explosions that released thick black smoke were reported at the Arkema Inc. chemical plant, where floods knocked out the electricity, leaving the facility outside Houston without refrigeration needed to protect volatile chemicals.
Meanwhile, emissions into the air have soared as the petrochemical industry shut down and then started up chemical operations, a cycle that causes an uptick in releases.
The potential health problems were magnified by overflowing sewers, inoperative treatment plants and the residues of animal waste, including carcasses.
Nobody is sure how much long-term health impact, if any, will result from the tidal wave of toxins and bacteria that swept through the nation’s fourth largest city.
Exhaustive investigations by the Environmental Protection Agency and the National Academy of Engineering after Hurricane Katrina, in which floodwaters languished in New Orleans for about six weeks, showed that toxic concentrations and the resulting exposures were too low to cause significant long-term health problems.
That festering flood caused a stench for weeks that left soldiers gagging for air as they flew helicopters 2,000 feet over the city. The Army Corps of Engineers had to pump the water out of New Orleans, much of which lies below sea level.
A report by the National Academy of Engineering in March 2006 said the floodwaters contained elevated levels of contaminants. The inorganic compounds were below drinking-water standards, while arsenic levels, attributed in part to lawn fertilizer, were above those standards.
The EPA took 1,800 samples of residue and soil from across the New Orleans area after Hurricanes Katrina and Rita and found that generally “the sediments left behind by the flooding from the hurricanes are not expected to cause adverse health impacts to individuals returning to New Orleans.”
The situation is far different in Houston, where the floodwaters are receding much faster.
But because Houston is far more industrialized, Harvey could have a much larger potential for leaving a toxic trail.
Without question, air emissions rose significantly during and after the storm, said Elena Craft, a toxicologist and senior scientist at the Texas branch of the Environmental Defense Fund.
The industry shutdown and startup cycle released 2 million pounds of pollutants, equal to 40% of all the emissions from 2016, Craft said, based on reports the industry made to the Texas Commission on Environmental Quality.
“In a few days, we have had months of exposure,” Craft said.
Marathon Oil, for example, reported to the state that heavy rain had pounded the roof of a storage tank so hard that it tilted, exposing gasoline to the air.
The emissions reports also included such carcinogens and suspected carcinogens as benzene and butadiene.
Craft said that sewage treatment plants in Beaumont went off line. A pipe carrying anhydrous hydrogen chloride was compromised in La Porte. Harris County’s 26 federal Superfund toxic waste sites may have been affected, including one that contains dioxins from a former paper mill along the San Jacinto River.
The fire at the Arkema chemical plant in Crosby released organic hydrogen peroxide, which officials said is an irritant but not toxic.
Tommy Newsom, who lives about 7 miles from the plant, said he felt fine but wondered what other chemicals might be involved. “Who knows how much of what they’re telling us is true?” he said.
“I think the wind’s in my favor,” said Newsom, a 60-year-old port worker, pointing to Texas state and U.S. flags at the entrance to his housing development.
Jennifer Sass, a senior scientist with the Natural Resources Defense Council’s health program, said the situation in Houston is a perfect breeding ground for hepatitis and tetanus.
“The flood is so large and slow-moving and the area is packed with dirty industries that are poorly regulated. Because the oil and gas industries down here are not as safe, we are concerned those toxins and chemicals are leaking,” she said.
Texas regulators urged caution. “Floodwaters may contain many hazards, including infectious organisms, intestinal bacteria, and other disease agents,” the Texas Commission on Environmental Quality said in a statement. “Precautions should be taken by anyone involved in cleanup activities or any others who may be exposed to floodwaters.”
The American Chemistry Council said its members are in constant communication with state and federal regulators about the status of their operations.
“Hurricane Harvey has presented extreme and unique challenges for the city of Houston and the surrounding areas in southeast Texas and Louisiana, warranting an unprecedented response effort, including that by local industry,” the trade group said in a statement.

Where Medicaid is concerned, the most notable thing about the latest version of the Better Care Reconciliation Act (BCRA) is that despite the drama of the past two weeks—the flood of news coverage regarding the potential impact of the losses; mounting concerns raised by Senators from expansion and non-expansion states alike; and the massive outcry from hospitals, physicians, insurers, and health care organizations—the new iteration leaves untouched the fundamental Medicaid contours of the earlier version.
The new draft retains the federal funding bar for Planned Parenthood (§ 123) as well as the earlier version’s limit on states’ ability to fund their programs through lawful, broad-based provider taxes (§ 131). The new bill does virtually nothing to lessen the financial losses to states that will flow from the prior iteration. According to the Congressional Budget Office (CBO), these losses would surpass $770 billion over 10 years as a result of provisions that eliminate the enhanced funding for the adult expansion population and superimpose flat annual growth restrictions on Medicaid’s historic federal funding formula (§124 and §132).
By 2036, CBO reports, federal Medicaid funding would be about 35 percent below current law, a catastrophe of epic proportions. According to one study that sought to translate BCRA’s Medicaid provisions into state-by-state loss estimates, California alone would lose between $37 and $52 billionbetween 2020 and 2027, depending on how the cap’s arbitrary growth limits play out over time. Indeed, depending on how the cap, which is tied to a general economic inflation rate that cannot be known with certainty, plays out against actual state spending needs—triggered by everything from new vaccines to long-term services and supports to address the opioid crisis or the consequences of Zika—the federal funding losses could grow from catastrophic to unimaginable.
Perhaps Congressional leaders have sought to convince their colleagues to disregard the CBO estimates and these studies, arguing that Congress, in fact, will never allow the bottom to fall out on states and will come through with additional funding. But the newest version of the bill underscores the fundamentally meaningless nature of such assurances.
Small crumbs of Medicaid give-backs can be found at various places in the new version. One that might be thought of as the Louisiana Purchase is designed to help one state cope with massive loss; over the long term, however, the adjustment washes out in the far larger picture of declining federal funding for an exceptionally poor state.
For purposes of setting the arbitrary growth limits over time, the original bill relied on per capita spending data from the 2014-2015 time period. The new draft would allow a late-expanding state (i.e., Louisiana) to use 2016 as its base period (§ 132). But regardless of whether it is tied to 2014-2015 or 2016, nothing can mask the fact that the base period is part of a growth formula unrelated to the real world of Medicaid spending. All state programs will be tied to the distant past where federal Medicaid funding is concerned.
Furthermore, the new version does not exempt the state from the bill’s exceptionally clumsy rate-setting procedures, which lack adjustments for volume and intensity or new technology and that allow the Health and Human Services (HHS) Secretary’s power to unilaterally alter what he considers to be unreliable state data. The measure continues to permit the Secretary to claw back what he determines to be “excessive” funding by reducing later payments without a prior hearing; in the event of state evidence of underpayment, the Secretary can withhold federal funds owed until a lengthy appeals system is exhausted.
As was the case with the prior version, the new draft tips its hat toward non-expansion states, further sweetening the pot by tweaking the disproportionate share hospital payment formula in ways that favor payments to states with the highest uninsured populations (§ 126, Restoring Fairness in DSH Allotments). Like its predecessor, the new version thus rewards states that have refused to insure their poorest residents and harshly penalizes struggling hospitals serving the remaining uninsured in those that have.
As an additional lure, the new version expands the block grant option in the earlier measure to enable states to use block grants for the ACA expansion population as well as for traditional low-income adults (§ 133). Like the earlier version, state block grant funding would remain virtually frozen, leaving states increasingly on the hook for care for millions of grievously under-funded adults.
One of Medicaid’s most important dimensions is its irreplaceable role in addressing the immediate and long-term effects of public health crises. Medicaid is by far the nation’s biggest single source of health care financing for dealing with critical public health threats. These threats may begin with an initial, recognized period of a formally declared emergency. They then can morph into events with very long-term effects felt for years or decades after. This was the case with the World Trade Center attacks, which led to an immediate surge in health care spending, followed by years of elevated spending to address the long-term health fallout triggered by the emergency itself. One need think only about Zika or the opioid crisis now gripping the nation to understand the near-term/long-term nature of public health threats.
Medicaid enrollees are disproportionately likely to live in poor communities, and poor communities are disproportionately likely to face public health threats ranging from environmental hazards to infectious disease. These communities also are inherently less likely to have fewer resources to cope with the effects of an emergency. Thus, a program such as Medicaid is crucial in its ability to deploy health care financing resources to the hardest-hit populations. Indeed, two thirds of all Louisiana Medicaid beneficiaries lived in the parishes affected by Hurricane Katrina.
Section 319 of the Public Health Service Act authorizes the HHS Secretary to declare the existence of a public health emergency arising from events such as a “disease or disorder,” “significant outbreaks of infectious diseases or bioterrorist attacks,” or other events identified as public health emergencies by the HHS Secretary. Whether to declare an emergency is entrusted to the Secretary’s judgment, and during the immediate emergency period, the Secretary enjoys expanded powers to deploy resources to designated populations or geographic areas. These special powers end when the declared emergency period ends. In the aftermath, states and local communities effectively are on their own, relying on the resources they have.
In and of itself, a loss of federal health funding as large as that imposed by BCRA elevates the threat risk. This risk grows exponentially when a true crisis hits, if Medicaid is crippled in its ability to provide a large-scale surge in public health care spending both during the emergency and thereafter. To understand how little the revised bill does to mitigate the crippling impact of the initial draft one need only look carefully at what the revisions would do when a true emergency strikes.
The press release accompanying the new draft states that “if a public health emergency is declared, state medical assistance expenditures in a particular part of the state will not be counted toward the per capita caps or block grant allocations for the declared period of the emergency.” But a close read of the actual bill text reveals its fundamental inadequacy.
First, the period of exemption lasts only five years, from January 1, 2020 through December 31, 2024. Emergencies happening after this date won’t qualify for the spending adjustment. Second, the bill provides no additional federal spending during the period of a declared emergency. The draft simply allows states to eventually qualify for additional federal funding in the years following the emergency if they can prove to the Secretary that their spending on the affected population went up compared to prior years and then only for immediate emergency costs. What state will have the money in advance? And what state will be able to take a chance on spending more given the purely speculative nature of whether an emergency will be declared and emergency expenditures recognized?
Third, states would receive no additional funding ever unless the HHS Secretary actually declares an emergency in the affected portion of the state or for the state’s affected populations. Many public health threats may not rise to a level that triggers a formal Secretarial determination, and the Secretary may be inclined not to make such a determination because of other, spillover effects that come with such a determination, such as the elevated demand for other types of resources.
Fourth, the additional amount of federal funding made available would be limited to the difference between what the state spent on the population in connection with the emergency and the state’s previous expenditures for the same population. Expenditures to cope with the emergency aftermath would not count, and of course these expenditures likely would not occur simultaneously with the emergency expenditures. For example, Zika has triggered emergency expenditures aimed at preventing the spread of the virus, but the true costs of Zika will roll out slowly in the form of babies left permanently and severely disabled by the virus.
And here is where the public health implications of BCRA become clear: other than exempting state expenditures on children classified as disabled from the caps, the revised bill, like its predecessor, makes no adjustment for long-term consequences. To be sure, as just mentioned, BCRA does exempt state expenditures on severely disabled children from the federal cap. But because the vast majority of children qualify for Medicaid based on poverty, this type of cramped classification system for measuring exemptions is sure to exclude spending for millions of children in severely compromised health from the exemption process.
Fifth, the bill allows only $5 billion in the aggregate for all additional federal funding over the five-year time period covered by the emergency exemption. In other words, the bill essentially creates a five-year, $5 billion mini-block grant to help all states address Medicaid spending for all emergencies occurring during this time period. The incredibly small size of the block grant alone would be likely to incentivize the HHS Secretary to avoid declaring emergencies out of concern that the money won’t be there to cover them.
In the end, the newest iteration of BCRA does nothing to alleviate the catastrophic effects of its predecessor: the difference in magnitude between what Medicaid can do today and what it will be capable of doing in the future is incalculable.

What goes on the chopping block: Research into cancer or Alzheimer’s? A Zika vaccine or a treatment for superbugs?
Health groups say President Donald Trump’s proposal to slash funds for the nation’s engine of biomedical research would be devastating for patients with all kinds of diseases — and for jobs.
“It is possible that the next cure for some cancer is sitting there waiting to be discovered, and it won’t get to the table,” said Dr. Georges Benjamin, executive director of the American Public Health Association.
In his budget blueprint Thursday, Trump called for a cut of $5.8 billion from the National Institutes of Health. That’s a staggering 18 percent drop for the $32 billion agency that funds much of the nation’s research into what causes different diseases and what it will take to treat them.
It comes despite Trump recently telling Congress about the need to find “cures to the illnesses that have always plagued us.”
“All of us woke up this morning in a state of shock about this number,” said Dr. Blase Polite, a cancer specialist at the University of Chicago who chairs the American Society for Clinical Oncology’s government relations committee.
Trump’s proposal would roll back NIH’s 2018 budget to about what it was in 2003. The president called for a “major reorganization” of NIH to stress the “highest priority research,” but only specifically targeted for elimination the $69 million Fogarty International Center that focuses on global health and has played a big role in HIV research abroad.
Drops in deaths from cancer and heart disease, breakthroughs in genetics, and new ways to treat and prevent HIV and other infectious diseases all are credited to decades of NIH-funded basic research.
http://www.healthcarefinancenews.com/news/superbug-infection-kills-patient-reno

A superbug infection resistant to all 27 available antibiotics killed a woman in Reno, Nevada, the Centers for Disease Control and Prevention reported Friday, in issuing a precaution to hospitals nationwide.
While this superbug case was rare, sepsis blood infections reportedly kill an estimated 258,000 Americans each year.
Medical experts have been warning for years of the dangers of overprescribing antibiotics because of the potential for antibiotic-resistant superbugs.
The female patient who died this September from the superbug infection was a Washoe County, Nevada resident in her 70s who arrived in the United States in early August 2016 after an extended visit to India, the CDC said.
On August 18, she was admitted to an acute care hospital with a primary diagnosis of an infection called systemic inflammatory response syndrome, which likely resulted from an infected right hip.
A week after she was admitted, the hospital notified the Washoe County Health District in Nevada that the patient had a bacterial infection of carbapenem-resistant Enterobacteriaceae, called CRE.

The number of cases of a sexually transmitted disease reported in the U.S. reached an all-time high last year, the CDC is reporting.
The combined total of reported chlamydia, gonorrhea, and syphilis cases was more than 1.8 million in 2015, the agency said in its annual Sexually Transmitted Disease Surveillance Report.
Those numbers are probably an underestimate, the agency said in a release, since most STD cases are undiagnosed and untreated. But the treated cases have reached an all-time — and expensive — high: the agency said it estimates the annual cost of therapy at nearly $16 billion.
The reported incidence of all three conditions rose from 2014 — by 5.9% for chlamydia, 12.8% for gonorrhea, and a whopping 19% for primary and secondary syphilis.