
Cartoon – Thank God for these curtains



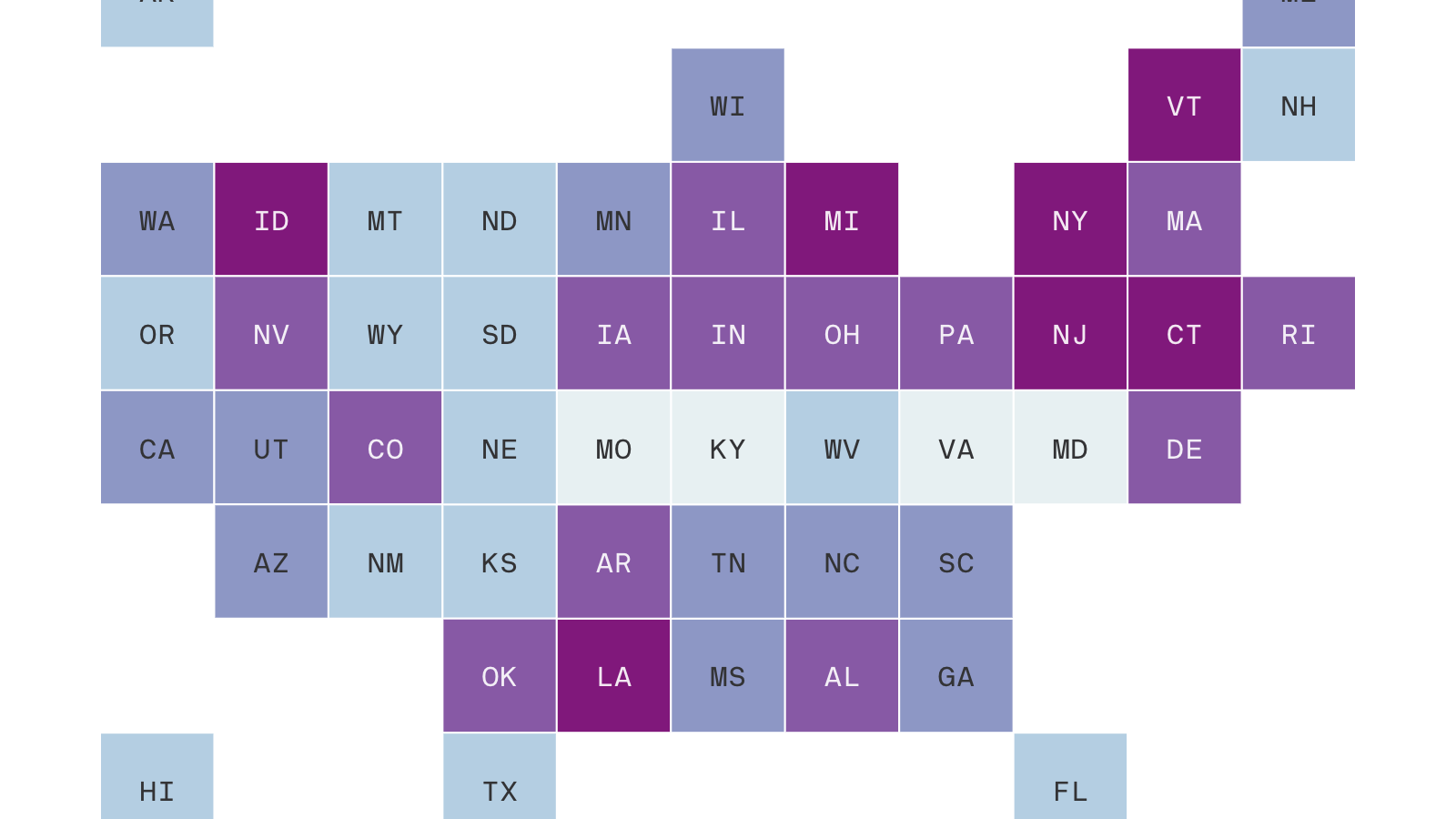
Although the coronavirus is expected to peak in the U.S. in two weeks, many states will see their individual peaks well after that, according to a model by the University of Washington’s Institute for Health Metrics and Evaluation.
Why it matters: States like Virginia and Maryland have more time to prepare for their systems to be maximally strained — if they make good use of that time.
States’ coronavirus peaks are defined as the point at which there is the most demand for resources, namely hospital beds and ventilators.
Some experts warn that states expected to face the hardest hit later in the year aren’t using their lead time well.
The bottom line: Coronavirus outbreaks, both globally and in the U.S., have seemed manageable until it’s too late. For states that so far aren’t hit hard, there’s no such thing as over-preparing.

At least 60 inmates at the Oakdale prison are in quarantine and an unknown number of staff are self-quarantining at home, said Corey Trammel, a union representative for correctional officers at the 1,700-inmate facility about 110 miles northwest of Baton Rouge.
“It’s been simultaneous, just people getting sick back to back to back to back,” Trammel said. “We don’t know how to protect ourselves. Staff are working 36-hour shifts — there’s no way we can keep going on like this.”
The prison bureau is not releasing the names of other infected inmates or staff, citing medical and privacy concerns. Jones complained of a “persistent cough” on March 19, the prison bureau said, and was transported to a hospital where he was diagnosed and placed on a ventilator.
The prison bureau also said Jones had “long-term, preexisting medical conditions” that increased his risk of developing the disease. Jones was convicted in 2017 of possession with intent to distribute crack cocaine within 1,000 feet of a junior college. He was serving a 27-year sentence.
Louisiana ranks 10th highest among states for reported coronavirus cases, with more than 3,300 people who have tested positive and another 137 who have died, government reports show. A week before the Oakdale prison had its first positive case, Gov. John Bel Edwards (D) issued a stay-at-home order and closed all public schools.
Trammel said the prison bureau has been slow to respond to the crisis across the country. The bureau last week banned family and friends from visiting inmates, but the officers’ union had lobbied the federal prison system to take this action for weeks to keep the disease from infiltrating the prison walls.
The Bureau of Prisons updates confirmed coronavirus cases most afternoons on its website, but there has been a lag between cases reported by the officers’ union and prison officials. As of Sunday afternoon, the prison system had only confirmed 14 inmates and 13 staff have tested positive.
At Oakdale, Trammel said staff also asked prison officials — weeks before the first coronavirus case — to shut down a prison labor program within the facility, where more than 100 prisoners make inmate clothing. The program, Trammel said, was not shut down until after the first inmate tested positive.
The Bureau of Prisons — which operates 122 prisons with more than 175,000 inmates — did not immediately respond Sunday to a request for comment. Oakdale Warden Rod Myers could also not be reached for comment.
Trammel said he asked the prison bureau on Saturday to send specialized medical teams to the facility to help with staffing shortages. He’s also asking for hazard pay, which would increase their salaries by 25 percent as they respond to the crisis. And he’s asking for more robust protective gear, including masks with respirators and perhaps face shields.
“We are bringing inmates to the hospitals and are staying right beside them around the clock,” Trammel said. “All we have is these itty bitty masks — a piece of towel over our faces — and nurses are coming into the room for a few minutes and they are all suited up.”
He also said he believes all Oakdale prison staff have now been exposed to the virus. Days ago, he interacted with an inmate who had a fever and still doesn’t know if the prisoner has received a test.
“We should all be in quarantine,” Trammel said. “We should not be going in to spread this monster of a virus.”
Prison reform advocates, who have been pushing for the early release of elderly and severely ill inmates due to covid-19, said the death of a federal inmate illustrates why government officials need to be doing a better job of protecting people like Jones.
“The conditions and reality of incarceration make prisons and jails tinderboxes for the spread of disease,” said Udi Ofer, director of the American Civil Liberties Union’s Justice Division. “A prison sentence should not become a death sentence. Our leaders must immediately take steps to release those identified by the CDC as most vulnerable to covid-19. With every hour of inaction that passes, the greater the human tragedy.”
https://www.yahoo.com/huffpost/amazon-fires-worker-chris-smalls-033240313.html

Amazon fired an employee who helped organize a walkout at one of its fulfillment centers over the company’s response to the ongoing coronavirus pandemic on Monday.
Chris Smalls, the employee who helped organize the demonstration, said he felt Amazon had failed to enact adequate measures to protect workers at the facility as many Americans turn to online shopping as stay-at-home mandates expand around the country. Smalls was one of a small group who walked out at a fulfillment center on Staten Island, demanding the company close the site and sanitize it before reopening. He said Amazon had notified employees at the warehouse of one confirmed case of the virus but claimed there were several others that hadn’t yet been reported.
Shortly after the strike, Smalls was terminated after working at Amazon for five years.
“Amazon would rather fire workers than face up to its total failure to do what it should to keep us, our families, and our communities safe,” Smalls said in a statement obtained by HuffPost. “I am outraged and disappointed, but I’m not shocked. As usual, Amazon would rather sweep a problem under the rug than act to keep workers and working communities safe.”
Amazon disputed Smalls’ account in a statement on Monday, saying he had been warned several times for “violating social distancing guidelines” and had been fired after failing to stay home. The company said Smalls’ claims were “simply unfounded.”
“He was also found to have had close contact with a diagnosed associate with a confirmed case of COVID-19 and was asked to remain home with pay for 14 days, which is a measure we’re taking at sites around the world,” a company spokesperson told HuffPost. “Despite that instruction to stay home with pay, he came onsite today, March 30, further putting the teams at risk. This is unacceptable and we have terminated his employment as a result of these multiple safety issues.”
The company also said just 15 employees out of 5,000 at its Staten Island location had participated in the demonstration.
“Our employees are heroes fighting for their communities and helping people get critical items they need in this crisis,” the spokesperson said. “Like all businesses grappling with the ongoing coronavirus pandemic, we are working hard to keep employees safe while serving communities and the most vulnerable.”
The Washington Post notes workers in at least 21 Amazon warehouses and shipping facilities in the U.S. have tested positive for the virus.
Employees at several other major companies staged walkouts on Monday. Workers at Instacart, the grocery delivery company, went on strike nationwide to demand better protections, including hazard pay and expanded paid sick leave. And employees at Whole Foods, owned by Amazon, said they planned to hold a nationwide “sick out” on Tuesday.
Workers at the Staten Island warehouse were first told last week that an employee had tested positive for the novel coronavirus, but they told HuffPost’s Emily Peck that business was “normal” and “running just as it had been” after the declaration. Others said they were afraid of getting sick at work, saying there wasn’t enough protection equipment on site, such as hand sanitizer or masks.
Amazon said it has extended a range of benefits to help protect workers during the pandemic, including extended paid leave options for some employees and increased health and safety measures. Employees diagnosed with COVID-19 are entitled to up to two weeks of paid leave, and Amazon says it notifies workers at sites with infected individuals.
The ongoing efforts by warehouse workers throughout the coronavirus pandemic have garnered support from several lawmakers. Rep. Alexandria Ocasio-Cortez (D-N.Y.) wrote Monday that the employees were simply “demanding dignity.”
“When people work an hourly job, it’s suggested in many ways that you‘re unimportant or expendable,” she wrote on Twitter. “Except you aren’t. Everyone deserves safe work, paid leave, & a living wage.”
https://www.yahoo.com/news/dr-birx-predicts-200-000-115800421.html

The White House coronavirus response coordinator said Monday that she is “very worried about every city in the United States” and projects 100,000 to 200,000 American deaths as a best case scenario.
In an interview on “TODAY,” Dr. Deborah Birx painted a grim message about the expected fatalities, echoing that they could hit more than 2 million without any measures, as coronavirus cases continue to climb throughout the country.
“I think everyone understands now that you can go from five to 50 to 500 to 5,000 cases very quickly,” Birx said.
“I think in some of the metro areas we were late in getting people to follow the 15-day guidelines,” she added.
Birx said the projections by Dr. Anthony Fauci that U.S. deaths could range from 1.6 million to 2.2 million is a worst case scenario if the country did “nothing” to contain the outbreak, but said even “if we do things almost perfectly,” she still predicts up to 200,000 U.S. deaths.
Fauci, the director of the National Institute of Allergy and Infectious Diseases, reiterated Monday on CNN that “I don’t want to see it, I’d like to avoid it, but I wouldn’t be surprised if we saw 100,000 deaths.”
Politics
Birx said the best case scenario would be for “100 percent of Americans doing precisely what is required, but we’re not sure that all of America is responding in a uniform way to protect one another,” referencing images circulating online of people still congregating in big groups and ignoring guidelines from the Centers for Disease Control and Prevention.
Birx was also on “Meet the Press” on Sunday warning that “no state, no metro area will be spared,” a message she repeated Monday. Even if metro or rural areas don’t see the virus in the community now, by the time it does appear, the outbreak will be significant, she added.
How long Americans will be expected to comply with measures, including socially distancing and sheltering in place, remains unclear in this growing pandemic after several states and larger cities began implementing measures over the past couple of weeks.
President Trump announced Sunday that the administration’s guidelines on social distancing have been extended until April 30. Trump said last week that he wanted to see much of the country return to normal by Easter, April 12, despite warnings from top health experts that easing guidelines early could cause mass deaths. Now, Trump said he expects “great things to be happening” by June 1.
Birx said on Sunday that the choice to extend the guidelines had not been made lightly.
“We know it’s a huge sacrifice for everyone,” she added.

Amazon warehouse workers in Staten Island, N.Y., and Instacart’s grocery delivery workers nationwide plan to walk off their jobs on Monday. They are demanding stepped-up protection and pay as they continue to work while much of the country is asked to isolate as a safeguard against the coronavirus.
The strikes come as both Amazon and Instacart have said they plan to hire tens of thousands of new workers. Online shopping and grocery home delivery are skyrocketing as much of the nation hunkers down and people stay at home, following orders and recommendations from the federal and local governments.
This has put a spotlight on workers who shop, pack and deliver these high-demand supplies. Companies refer to the workers as “heroes,” but workers say their employers aren’t doing enough to keep them safe.
The workers are asking for a variety of changes:
Workers at Amazon’s Staten Island facility have said that multiple people at the warehouse have been diagnosed with COVID-19. Some of them plan to walk off the job on Monday to pressure the company to close the warehouse for an extended deep cleaning.
At Amazon, which employs some 800,000 people, workers have diagnosed positively for COVID-19 in at least 11 warehouses, forcing a prolonged closure of at least one warehouse in Kentucky. The company says it has “taken extreme measures to keep people safe,” including allowing unlimited unpaid leave time for employees who feel uncomfortable working.
Amazon says its decision on whether to close a warehouse for cleaning or for how long depends on where the sick workers were in the building, for how long, how long ago and other assessments. The company has also temporarily raised its pay by $2 an hour through April.
Instacart’s army of grocery delivery workers are not employees, but independent contractors. They say the company has not provided them with proper protective items like disinfectants, hazard pay of an extra $5 per order and a higher default tip in the settings of the app.
Instacart on Sunday said it would distribute supplies, including hand sanitizer, to more workers and that it would change some tipping settings, but did not address paid sick leave for its contractors.
“Actions speak louder than words,” Instacart worker Sarah Polito told NPR. “You can tell us that we’re these household heroes and that you appreciate us. But you’re not actually, they’re not showing it. They’re not taking these steps to give us the precautions. They’re not giving us hazard pay.”
A nurse at Mount Sinai Hospital in New York died from COVID-19 after learning he was infected by the novel coronavirus almost two weeks ago. Protective medical gowns are in such short supply in the Mount Sinai system that some nurses have started to use Hefty-brand garbage bags instead, according to photos on social media.
The New York Post reported that Kious Kelly, an assistant nursing manager at Mount Sinai Hospital in Manhattan, died Tuesday. He was 48 years old.
His sister confirmed his death to the Post, saying that she was told he had been in the intensive-care unit but that he did not think it was serious. The Post did not specify how he contracted the virus.
“We are deeply saddened by the passing of a beloved member of our nursing staff,” Renatt Brodsky, a representative for the Mount Sinai Health System, told Business Insider in a statement. Brodsky did not provide any further details.
New York state has become the epicenter for the US’s coronavirus outbreak, with more than 33,000 infections and more than 360 deaths. In New York and other areas in the US with large outbreaks, healthcare workers are reporting shortages of personal protective equipment like masks, gowns, face shields, and gloves.
At Mount Sinai West, in the same hospital system where Kelly worked, nurses published a photo on social media showing them fashioning plastic trash bags into protective outfits, according to the Post.
“NO MORE GOWNS IN THE WHOLE HOSPITAL,” they wrote on Facebook. “NO MORE MASKS AND REUSING THE DISPOSABLE ONES … NURSES FIGURING IT OUT DURING COVID-19 CRISIS.” One nurse is seen holding a box of Hefty Strong 33-gallon bags, more commonly used for lining household trash cans.
https://www.axios.com/coronavirus-lessons-other-countries-24794264-1653-4500-922c-7f1c66efa011.html
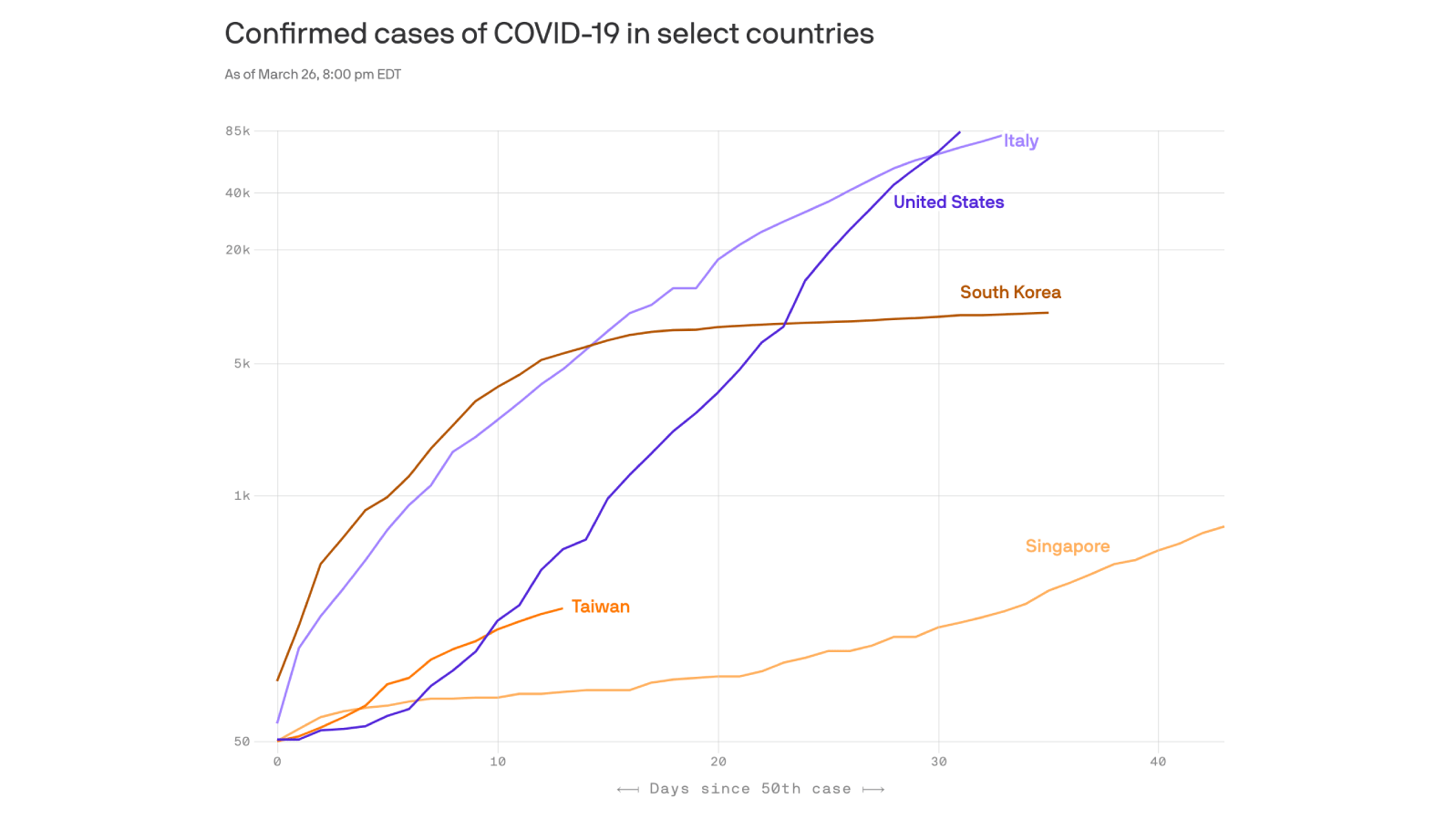
The countries that have most successfully fended off the novel coronavirus have mainly done it with a combination of new technology and old-school principles.
Why it matters: There’s a lot the U.S. can learn from the way other countries have handled this global pandemic — although we may not be able to apply those lessons as quickly as we’d like.
The big picture: A handful of Asian countries, including South Korea, Singapore and Taiwan, have succeeded where the U.S. and Europe have failed.
The bad news: It’s too late for the U.S. to simply do what worked in those countries. We’ve already made too many mistakes.
As a new infection begins to spread, you want to quickly test the people who might have it, and quarantine the ones who do. Then you want to figure out who else they might have infected, and test those people, and quarantine the ones who are indeed sick. This process gets repeated.
This test-and-trace process is nothing new. It’s the standard playbook. South Korea, Singapore and Taiwan just executed it a lot better than the United States.
Next time a mysterious virus starts spreading abroad, better testing and a much faster response will be imperative.
Singapore has gotten pretty draconian with its track-and-trace process.
That might be too Big Brother for the U.S., but a voluntary version of it might work — we already consent to a whole lot of location tracking for much less important ends.
Taiwan, meanwhile, aided its coronavirus response by making better use of data it already had. It quickly merged its immigration and health care databases, giving authorities a real-time view of who was getting sick and where they had traveled.
Public communication is one of the big things Italy — a leading example of what not to do — got wrong.
Singapore, by contrast, came out early with a clear message: This was going to be bad for a while, and people needed to stick together and do their part.
The U.S., so far, looks a lot more like Italy.
The U.S. can’t go back in time to get things right at the beginning. So we can’t match the success of places like South Korea.
The bottom line: “If we had got on top of this thing two months ago, America would look very, very different,” Ashish Jha, director of Harvard’s Global Health Institute, said in a recent interview with the New Yorker.

The pandemic has begun to sweep through New York City’s medical ranks, and anxiety is growing among normally dispassionate medical professionals.
A supervisor urged surgeons at Columbia University Irving Medical Center in Manhattan to volunteer for the front lines because half the intensive-care staff had already been sickened by coronavirus.
“ICU is EXPLODING,” she wrote in an email.
A doctor at Weill Cornell Medical Center in Manhattan described the unnerving experience of walking daily past an intubated, critically ill colleague in her 30s, wondering who would be next.
Another doctor at a major New York City hospital described it as “a petri dish,” where more than 200 workers had fallen sick.
Two nurses in city hospitals have died.
The coronavirus pandemic, which has infected more than 30,000 people in New York City, is beginning to take a toll on those who are most needed to combat it: the doctors, nurses and other workers at hospitals and clinics. In emergency rooms and intensive care units, typically dispassionate medical professionals are feeling panicked as increasing numbers of colleagues get sick.
“I feel like we’re all just being sent to slaughter,” said Thomas Riley, a nurse at Jacobi Medical Center in the Bronx, who has contracted the virus, along with his husband.
Medical workers are still showing up day after day to face overflowing emergency rooms, earning them praise as heroes. Thousands of volunteers have signed up to join their colleagues.
But doctors and nurses said they can look overseas for a dark glimpse of the risk they are facing, especially when protective gear has been in short supply.
In China, more than 3,000 doctors were infected, nearly half of them in Wuhan, where the pandemic began, according to Chinese government statistics. Li Wenliang, the Chinese doctor who first tried to raise the alarm about Covid-19, eventually died of it.
In Italy, the number of infected heath care workers is now twice the Chinese total, and the National Federation of Orders of Surgeons and Dentists has compiled a list of 50 who have died. Nearly 14 percent of Spain’s confirmed coronavirus cases are medical professionals.
New York City’s health care system is sprawling and disjointed, making precise infection rates among medical workers difficult to calculate. A spokesman for the Health and Hospitals Corporation, which runs New York City’s public hospitals, said the agency would not share data about sick medical workers “at this time.”
William P. Jaquis, president of the American College of Emergency Physicians, said the situation across the country was too fluid to begin tracking such data, but he said he expected the danger to intensify.
“Doctors are getting sick everywhere,” he said.
Last week, two nurses in New York, including Kious Kelly, a 48-year-old assistant nurse manager at Mount Sinai West, died from the disease; they are believed to be the first known victims among the city’s medical workers. Health care workers across the city said they feared many more would follow.
Mr. Riley, the nurse at Jacobi, said when he looked at the emergency room recently, he realized he and his colleagues would never avoid being infected. Patients struggling to breathe with lungs that sounded like sandpaper had crowded the hospital. Masks and protective gowns were in short supply.
“I’m swimming in this,” he said he thought. “I’m pretty sure I’m getting this.”
His symptoms began with a cough, then a fever, then nausea and diarrhea. Days later, his husband became ill. Mr. Riley said both he and his husband appear to be getting better, but are still experiencing symptoms.
Like generals steadying their troops before battle, hospital supervisors in New York have had to rally, cajole and sometimes threaten workers.
“Our health care systems are at war with a pandemic virus,” Craig R. Smith, the surgeon-in-chief at NewYork-Presbyterian Hospital, wrote in an email to staff on March 16, the day after New York City shut down its school system to contain the virus. “You are expected to keep fighting with whatever weapons you’re capable of working.”
“Sick is relative,” he wrote, adding that workers would not even be tested for the virus unless they were “unequivocally exposed and symptomatic to the point of needing admission to the hospital.”
“That means you come to work,” he wrote. “Period.”
Arriving to work each day, doctors and nurses are met with confusion and chaos.
At a branch of the Montefiore hospital system in the Bronx, nurses wear their winter coats in an unheated tent set up to triage patients with symptoms, while at Elmhurst Hospital Center in Queens, patients are sometimes dying before they can be moved into beds.
The inviolable rules that once gave a sense of rhythm and harmony to even the busiest emergency rooms have in some cases been cast aside. Few things have caused more anxiety than shifting protocols meant to preserve a dwindling supply of protective gear.
When the pandemic first hit New York, medical workers changed gowns and masks each time they visited an infected patient. Then, they were told to keep their protective gear on until the end of their shift. As supplies became even more scarce, one doctor working on an intensive care unit said he was asked to turn in his mask and face shield at the end of his shift to be sterilized for future use. Others are being told to store their masks in a paper bag between shifts.
“It puts us in danger, it puts our patients in danger. I can’t believe in the United States that’s what’s happening,” said Kelley Cabrera, an emergency room nurse at Jacobi Medical Center.
An emergency room doctor at Long Island Jewish Medical Center put it more bluntly: “It’s literally, wash your hands a lot, cross your fingers, pray.”
Doctors and nurses fear they could be transmitting the virus to their patients, compounding the crisis by transforming hospitals into incubators for the virus. That has happened in Italy, in part because infected doctors struggle through their shifts, according to an article published by physicians at a hospital in Bergamo, a city in one of the hardest-hit regions.
Frontline hospital workers in New York are now required to take their temperature every 12 hours, though many doctors and nurses fear they could contract the disease and spread it to patients before they become symptomatic.
They also say it is a challenge to know when to come back to work after being sick. All medical workers who show symptoms, even if they are not tested, must quarantine for at least seven days and must be asymptomatic for three days before coming back to work.
But some employers have been more demanding than others, workers said.
Lillian Udell, a nurse at Lincoln Medical Center, another public hospital in the Bronx, said she was still weak and experiencing symptoms when she was pressured to return to work. She powered through a long shift that was so chaotic she could not remember how many patients she attended. By the time she returned home, the chills and the cough had returned.
“I knew it was still in me,” she said. “I knew I wasn’t myself.”
Christopher Miller, a spokesman for the Health and Hospitals Corporation, said the agency could not comment on Ms. Udell’s claim, but said its hospitals had “never asked health care workers who are sick and have symptoms of Covid-19 to continue to work or to come back to work.”
There is also the fear of bringing the disease home to spouses and children. Some medical workers said they were sleeping in different rooms from their partners and even wearing surgical masks at home. Others have chosen to isolate themselves from their families completely, sending spouses and children to live outside the city, or moving into hotels.
“I come home, I strip naked, put clothes in a bag and put them in the washer and take a shower,” one New York City doctor at a large public hospital said.
Because the pathogen has spread so widely, even medical workers not assigned directly to work with infected patients risk contracting the disease.
A gynecologist who works for the Mount Sinai hospital system said she had begun seeing women in labor who were positive for the coronavirus. Because she is not considered a front-line worker, she said, restrictions on protective gear are even more stringent than on Covid-19 units. She said she was not aware of any patients who had tested positive after contact with doctors or nurses, but felt it was only a matter of time.
“We’re definitely contaminating pregnant mothers that we’re assessing and possibly discharging home,” said the doctor, who spoke on condition on anonymity because her hospital had not authorized her to speak.
Mount Sinai said in a statement that it had faced equipment shortages like other hospitals, but added the issues had been solved in part by a large shipment of masks that arrived from China over the weekend. The hospital “moved mountains” to get the shipment, the statement said.
This week, the Health and Hospitals Corporation recommended transferring doctors and nurses at higher risk of infection — such as those who are older or with underlying medical conditions — from jobs interacting with patients to more administrative positions.
But Kimberly Marsh, a nurse at Westchester Medical Center outside New York City, said she has no intention of leaving the fight, even though she is a 53-year-old smoker with multiple sclerosis and on a medication that warns against getting near people with infections.
“It almost feels selfish,” she said, though she acknowledged that with two years before retirement she could not afford leave if she wanted to.
Even so, she said, the fear is palpable each time she steps into the emergency room. A nurse on her unit has already contracted the virus and one doctor is so scared he affixes an N95 mask to his face with tape at the beginning of each shift. Ms. Marsh said she sweats profusely in her protective gear because she is going through menopause and suffers from hot flashes.
“We all think we’re screwed,” she said. “I know without any doubt that I’m going to lose colleagues. There’s just no way around it.”

Hahnemann University Hospital could hold 500 patients with the coronavirus. But city officials said the cost was too steep.
A hospital with room for nearly 500 beds has been closed for months in the center of Philadelphia, a city bracing for the spread of the coronavirus and a crush of sick patients.
But the facility will remain empty, city officials said, because they cannot accept the owner’s offer: buy the hospital or lease it for almost $1 million a month, including utilities and other costs.
“We don’t have the need to own it nor the resources to buy it. So we are done and we are moving on,” Mayor Jim Kenney told reporters on Thursday during the city’s daily briefing.
The next day, he said that Temple University would let the city use a music and sports venue for free. The city would no longer pursue the closed facility, Hahnemann University Hospital.
The abrupt end of the dispute underscored the frantic search for more hospital beds as cities try to prepare for a crisis that is overwhelming medical facilities in New York, and highlighted the tensions between government officials and businesses in responding to the pandemic. This week, the Trump administration backed away from announcing a $1 billion deal with General Motors and Ventec Life Systems to produce ventilators, after officials said they needed more time to assess the estimated cost.
In Philadelphia, coronavirus infections are quickly rising. On Friday, the city health commissioner, Dr. Thomas Farley, reported 154 new cases, for a total of 637 cases across every ZIP code of the city, and three deaths. “This virus is everywhere in Philadelphia,” he said.
The owner of the hospital, Joel Freedman of Broad Street Healthcare Properties, a real estate company, said he had offered to sell the facility to the city well below market price, or to lease it for $60 a bed a day, far less than what two other hospitals in California agreed to charge to lease their facilities.
“Anyone looking at the apples-to-apples comparison can see that Mr. Freedman not only desired to be helpful to the city of Philadelphia and its leaders, but he was very reasonable,” said Sam Singer, a spokesman for Mr. Freedman, who is based in Los Angeles. “We’re disappointed that they didn’t accept what we offered, but we stand ready to be helpful to the city or the state if they want to reopen discussions.”
Hahnemann Hospital, which once served the city’s poorest patients, closed in September 2019. The hospital had been suffering millions of dollars in losses a month, Mr. Freedman told The Philadelphia Business Journal last June.
“We relentlessly pursued numerous strategic options to keep Hahnemann in operation, and have been uncompromising in our commitment to our staff, patients and community,” Mr. Freedman said at the time. “We are faced with the heartbreaking reality that Hahnemann cannot continue to lose millions of dollars each month and remain in business.”
The decision to close the hospital last year infuriated local leaders and led Senator Bernie Sanders, the Vermont independent running to be the Democratic nominee for president, to hold a rally outside the hospital. He described the closure as a consequence of greed, and an example of the need for a better health care system.
Mr. Singer said Mr. Freedman had been unfairly maligned throughout the recent dispute, and that his obligations included maintenance, compensating his staff and paying off the loan he took out to buy the property.
“They’ve wrongly been critical of Mr. Freedman,” Mr. Singer said of his detractors. “We understand that emotions are high. We don’t want in any way to hold that against them.”
He added, “Even with those harsh words, our doors, our ears, our minds are still open. We want to help.”
Since last fall, the hospital has sat empty and fallen into disrepair, Mayor Kenney said on Thursday. “It has no beds and would require extensive work to make it usable again,” he said.
Mr. Kenney said the city had offered to lease the hospital for a “nominal” amount and pay for its maintenance and expenses, a deal that would have meant “hundreds of thousands of dollars a month” for Mr. Freedman and made the property more marketable in the future.
“Yet the owner would not agree to our offer,” he said.
Instead, Mr. Freedman wanted the city to pay $400,000 a month in rent in addition to making improvements and paying for other expenses, Mr. Kenney said. “I’ll let others decide whether that’s reasonable or not,” Mr. Kenney said.
Mr. Singer said the city contacted Mr. Freedman around March 11 about leasing the property. “We responded immediately and said, ‘Yes, we would like to help in any manner,’” he said.
Mr. Freedman offered to sell the property below market price or lease it for $27 a bed a day. The city would have to pay an additional $33 a bed a day to cover the costs of utilities and taxes, he said. The full amount came to about $910,000 a month, Mr. Singer said.
“They just decided, ‘We’re not going to pursue Hahnemann,’” he said.
City officials had signaled that negotiations were breaking down earlier this week. On Tuesday, the city’s managing director, Brian Abernathy, told reporters that what Mr. Freedman wanted was “unreasonable.”
“I think he’s looking at this as a business transaction rather than providing an imminent and important aid to the city and our residents,” Mr. Abernathy said.
City Councilor Helen Gym said on Twitter that day that Philadelphia should not let “unconscionable greed to get in the way of saving lives,” and called for acquiring the property through eminent domain. Mr. Kenny said city officials had explored that option but determined it was too time-consuming and would require them to purchase the building at market price.
Mr. Kenney said in a news conference Friday that the city would use the Liacouras Center, a concert and sports venue at Temple University, for additional hospital space. The university will let the center be used for free and the space can fit up to 250 beds, officials said.