https://mailchi.mp/0d4b1a52108c/the-weekly-gist-april-24-2020?e=d1e747d2d8
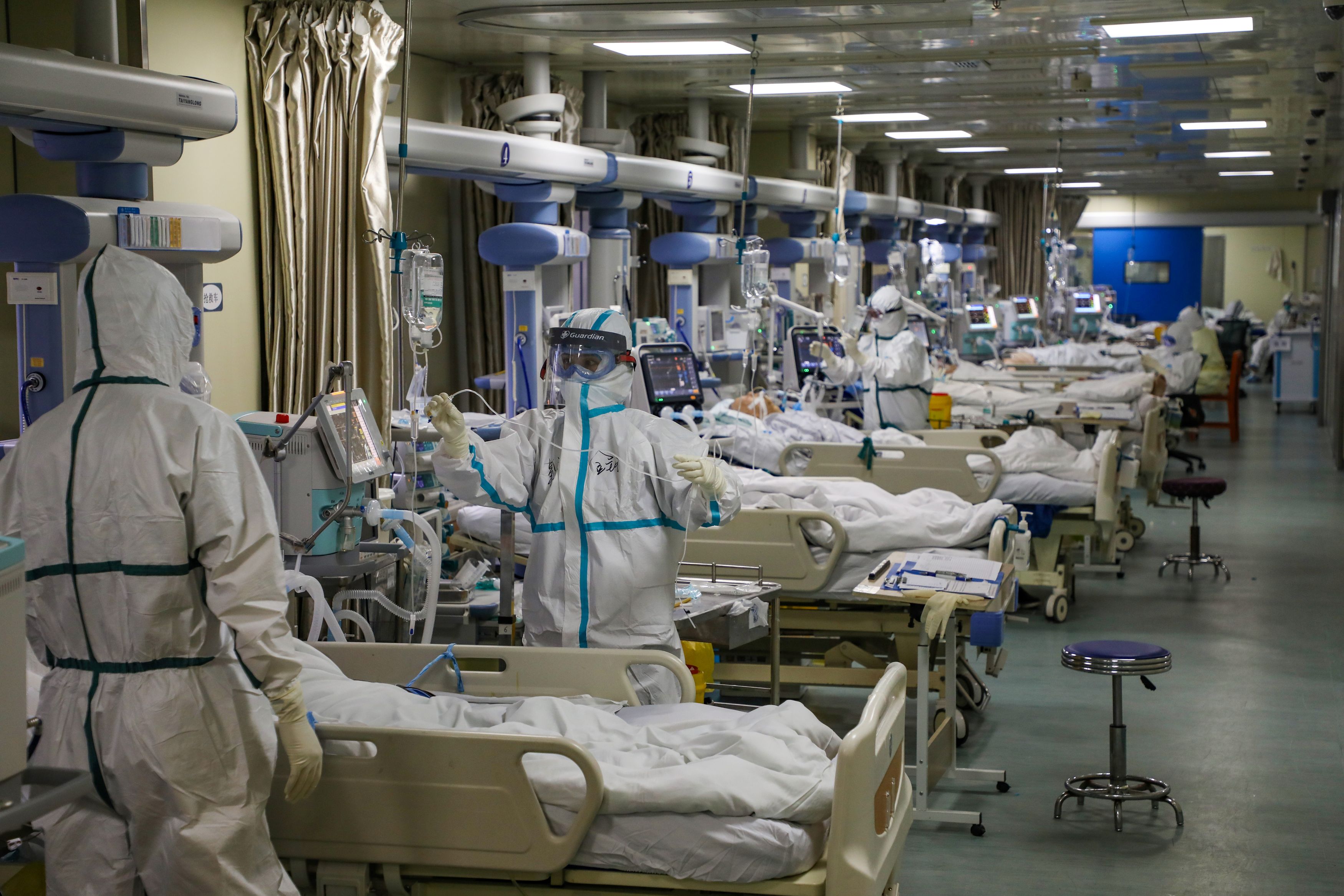
A study published this week in JAMA provides a look at the largest series of COVID-19 hospitalized patients studied to date in the US, reporting that almost all patients treated had at least one underlying condition. Physicians from Northwell Health evaluated the outcomes, comorbidities and clinical course of 5,700 confirmed coronavirus patients hospitalized between March 1st and April 4th across the New York City area. Hospitalized patients, 60 percent of whom were men, had a high burden of chronic disease.
Similar to other reports, older patients, and those with a higher chronic disease burden (especially diabetes) were both more likely to require mechanical ventilation, and more likely to die. Only nine of the 436 patients under age 50 who had no significant cormorbidities (as measured by the Charlson Comorbidity Index) had died. One number received the most press coverage: as reported in the abstract, 88 percent of patients who received mechanical ventilation died. Digging into the details of the series, this may end up being an overestimation, as the statistic is based on a subset of 320 ventilated patients who either died or were discharged by April 4th. At that time, 831 patients remained in the hospital on ventilators, with outcomes still to be determined. Ultimately, the mortality rate of full cohort of ventilated patients could fall nearer to the 50-60 percent range seen in other studies.
Regardless, the rich dataset of the Northwell report adds to the body of evidence that severe COVID-19 infections and deaths involve several organ systems. This Science article provides a thorough (and comprehensible to the non-clinician) review of how the virus invades the body. While the lungs remain “ground zero” for infection, critically ill patients may experience serious kidney, cardiac, or even nervous system involvement. A host of chronic diseases predispose patients for worse outcomes—yet doctors remain puzzled that they aren’t seeing “a huge number of asthmatics” in ICUs. Patients are presenting with dangerously low oxygen levels but less distress than expected, likely because they are able to still “blow off” carbon dioxide, limiting the body’s ability to sense the seriousness of their condition.
Many dying patients are overwhelmed by a “cytokine storm”—an overreaction of the immune system that compounds organ failure. And new evidence suggests that large numbers of critically ill patients may experience abnormal blood clotting, contributing to the high mortality rates of the disease. The more doctors and scientists learn about coronavirus, the more complex the disease process seems—leaving doctors with work to do to understand, manage, and treat the tens of thousands of these seriously ill patients.


