
Cartoon – I finished your performance review





Amid the evacuation of approximately 1,500 patients from Houston-area hospitals, officials are commending the emergency response by health providers — while also cautioning that it may be weeks before the facilities are back to business as usual.
The SouthEast Texas Regional Advisory Council — which has overseen catastrophic medical operations since Hurricane Harvey as part of Houston’s emergency command center — estimates that nearly two dozen hospitals have evacuated patients by ambulance and airplane over the course of the past week.
“The storm was so huge it was uncertain what hospitals might be in harm’s way,” said Darrell Pile, chief executive officer of SETRAC. Had they known Harvey would grow into a Category 4 storm, Pile said, they would have staged evacuations three days in advance. But Harvey was unpredictable from the start — and grew stronger without much warning.
Evacuations have been slow not only because of the perils involved in moving patients but also because it has taken time to find other hospitals to accept them. “Some patients may have had gone to Dallas, San Antonio, Austin, or even Waco,” Pile said. “You’ve got to find the hospital to handle the unique needs of the patients you want to transfer.”
Evacuation numbers continued to climb on Tuesday. But Pile said numerous hospitals also scaled back or suspended plans for evacuations. One such facility was Ben Taub, one of Houston’s major safety-net hospitals, which only evacuated three patients after originally seeking to move all 350 patients after flooding occurred inside the hospital basement.
“In the case of Ben Taub, as the waters went down, and additional staff were able to arrive, they whittled down their list,” Pile said, speaking Wednesday. “They may even open back up to full service later today.”
Bryan McLeod, director of external and online communications at Harris Health System, said in a statement Tuesday afternoon that Ben Taub, the system’s largest hospital, is now seeking to “offload some of the patients that we currently have” in anticipation of a “surge of patients” expected as roads clear.
“I can only imagine the burden is going to increase,” said Vivian Ho, a health care economist with Rice University. “It’s going to get tough on them.”
Pile praised the coordination of hospitals, first responders, and civic leaders. In other major storms elsewhere, he said, some hospitals have failed to communicate effectively; ambulances would bring patients to their doors even though the facilities might be unable to meet their needs.
By contrast, Pile said, roughly 25 hospitals affected by Harvey declared an “internal disaster” — a status that reflects a hospital facing problems in carrying out normal daily operations — that allowed SETRAC to pass along timely information along to first responders who could, in turn, divert patients toward care at hospitals capable of treating them.
“The majority of our hospitals stayed open,” Pile said. “The teamwork of hospitals and EMS agencies through our coalition kept it from becoming an even a bigger disaster.”
Pile hasn’t heard of any hospitals in the Houston area devastated to the point of shuttering — something that’s also occurred in other storm-ravaged cities. It’s because of that he believes nearly all Houston-area hospitals will be fully up and running by the end of September.
“This storm was paralyzing,” Pile said. “Within a month, [I expect] 90 to 95 percent of hospitals will be back in full service. That’s a first.”
https://www.cbsnews.com/news/obamacare-repeal-has-never-been-more-popular/
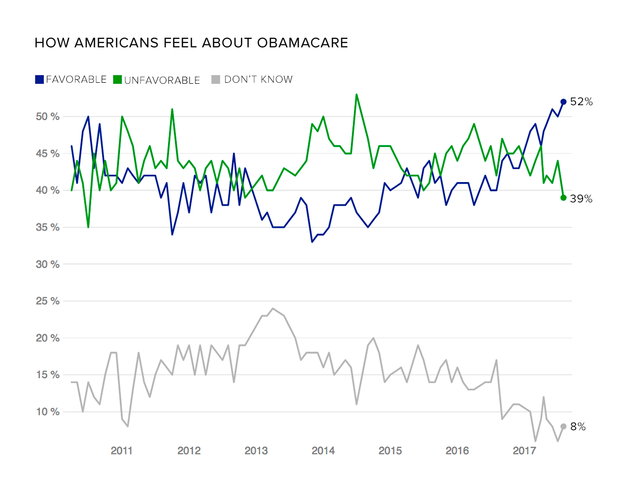
Underscoring the adage that you don’t know what you’ve got until it’s (almost) gone, the popularity of Obamacare is surging.
Only weeks after Republicans in Congress failed to repeal the landmark health reform law, 52 percent of respondents hold a favorable view of the Affordable Care Act (ACA), according to a recent Kaiser Family Foundation August poll. That’s up 10 percentage points since June of last year and nearly 20 points since November 2013, when public support for the ACA was at its nadir.
A July poll by CBS News after the repeal effort collapsed found that a plurality of Americans favor a bipartisan push in Congress to improve Obamacare.
The shift in sentiment coincides with other positive developments for Obamacare following its close call in Washington. With several large, and some smaller, insurers pulling out of the program over the past year or so, until recently it looked as if more than 92,000 participants spread out over 82 counties would have no insurer in their local health care exchanges, Cynthia Cox, associate director of Kaiser Family Foundation, said. But state insurance commissioners and other officials in states in jeopardy of losing Obamacare coverage have worked closely with insurers to negotiate continued coverage.
In Ohio, for instance, there were 20 counties without insurers, but officials ultimately convinced five health plans to cover all but one. Then, on August 24, the Ohio Department of Insurance announced that Paulding County, the last “bare county” in the country, would be covered by insurer CareSource.
In addition, the exchange marketplace overall has shown signs of stabilizing. After big financial losses in 2014 and 2015, individual market insurers saw improved performance in 2016, a trend that has continued this year, according to a different Kaiser Family Foundation study.
If Obamacare’s popularity is up, the program’s shortcomings remain clear. At last count, more than 2.6 million enrollees across 1,300 counties were expected to have only one insurer in their exchanges. More insurers also could pull out or move to sharply increase their premiums. The deadline for insurance companies to commit to participate in an exchange is September 27.
Until then, many insurers are watching closely to see if the Trump Administration will continue funding the federal cost-sharing subsidies that help low-income members pay for deductibles, co-pays and other out-of-pocket costs. Industry players are also waiting or Senate hearings to start after Labor Day in which which insurance commissioners, lawmakers and state governors are expected to testify about what can be done to stabilize the individual marketplace.
Meanwhile, some states are beginning to take matters into their own hands, moving to rewrite the ACA rules by applying for what’s known as a “Section 1332” waiver. Oklahoma is asking for a waiver to establish its own reinsurance program using some federal funds, which would cover the highest-cost individual marketplace cases. Alaska recently received approval for a similar reinsurance waiver. Oklahoma, however, is also looking ahead to more major structural changes that may spur debate.
Iowa, which is undergoing huge premium increases in its individual marketplace, has submitted a waiver that would overhaul the state’s insurance marketplace by redistributing federal tax credit money. The plan would create a single standard health plan and offer a flat tax credit based on age and income.
Critics argue this would increase health care costs significantly for Iowa’s low-income population, putting coverage out of reach for many. Proponents argue that increasing Iowa’s pool of healthy insured people is the best way to stabilize Iowa’s individual market and lower premiums for everyone.
https://www.theatlantic.com/health/archive/2017/08/mold-city/538224/
Flooding means health issues that unfold for years.
The flooding of Houston is a health catastrophe unfolding publicly in slow motion. Much of the country is watching as 50 inches of water rise around the chairs of residents in nursing homes and submerge semitrucks. Some 20 trillion gallons of water are pouring onto the urban plain, where developers have paved over the wetlands that would drain the water.
The toll on human life and health so far has been small relative to what the images suggest. Authorities have cited thirty known deaths as of Tuesday night, while 13,000 people have been rescued. President Donald Trump—who this month undid an Obama-era requirement that infrastructure projects be constructed to endure rising sea levels—offered swift reassurance on Twitter: “Major rescue operations underway!” and “Spirit of the people is incredible. Thanks!”
But the impact of hurricanes on health is not captured in the mortality and morbidity numbers in the days after the rain. This is typified by the inglorious problem of mold.

Healthcare spending growth slowed in 2016, and the trend appears to be continuing, according to the August 2017 Altarum Institute Center Health Sector Trend report.
According to the report, spending grew by only 4.6 percent in 2016 and estimates based on new data have the downward trend continuing with growth for the first half of 2017 at 4.4 percent. Altarum said the estimates illustrate the impact of expanded coverage, and its subsequent leveling off, on healthcare utilization. Coverage expansion was concentrated in 2014 and 2015, leading to a jump in health services utilization. That peaked at at 5.1 percent in 2015.
“Coverage leveled off in 2016 and, in response, the growth in health services utilization has been trending back toward pre-expanded coverage rates,” Altarum said.
Healthcare price growth has also dropped in 2017, from 2 percent in the first quarter to 1.6 percent in the second quarter.
Though much higher than healthcare services, prescription drug price growth slowed to 3.6 percent in the second quarter 2017. However it is important to note that the impact of rebates are not reflected in these data, and that drug pricing controversies like the one surrounding Mylan’s EpiPen were recently resolved and some generic alternatives have been made available at lower prices.
Finally, health employment grew an average of 21,000 jobs per month during the first 5 months of 2017 then unexpectedly rebounded to 38,000 in June and July. The jump in June and July was a surprise, and was focused mainly in ambulatory settings.
“Growth averaged 32,000 during 2015 and 2016, and the decline in monthly growth during the first 5 months of 2017 was expected due to slower growth in health care utilization driven by the leveling off in expanded coverage,” Altarum said.
The American Hospital Association’s February 2017 Cost of Caring report also illustrated the increased utilization in 2014 and 2015, due to expanded healthcare coverage and more intense utilization of services like chronic disease management.
However, the report mentioned that statistics also suggested that hospitals are trying to hold costs down. For instance, hospital price growth in 2015, as measured by the Hospital Producer Price Index, was .9 percent, a 13-year low and a notable drop from the rate of 4.4 percent in 2006, the report said.
Growth in Medicare spending for all hospital services, both inpatient and outpatient, is at a 17-year low, and inpatient spending dropped 1.9 percent in 2015.
So it is possible that along with a leveling off of coverage and utilization, successful hospital attempts at stabilizing or reducing cost of care could be responsible for the lower spending. The slowing in hospital price growth in the Altarum report is also illustrative of these theories.
However, the hospital industry faces serious challenges that can slow efforts to reduce costs, including drug prices and regulatory compliance, the AHA report said.
Electronic health records have also proven to be big resource absorbers for providers. AHA estimates show that from 2010 to 2014 hospitals spent over $47 billion annually on IT. Increasing regulatory requirements are also fueling increases in administrative expenses and compliance staffing demands, the AHA report said.
Click to access Altarum%20RWJF%20Trend%20Report%20Aug%202017_1.pdf
https://www.axios.com/aca-markets-narrow-problem-2479649219.html
The problem: Premiums in the Affordable Care Act marketplaces have been rising sharply, with the average increase for the benchmark “silver plan” up 21% this year. Proposed rates for next year will range from a 49% increase in Wilmington, Delaware to a 5% decrease in Providence, Rhode Island.
But the non-group market is actually fairly small, covering about 18 million people, with about 10 million of them in the ACA marketplaces which have received so much attention.
The perception: A Kaiser Family Foundation poll this month found that when people read headlines or hear about “premiums soaring” in the ACA marketplaces, most Americans — 76% — they think they are hearing about their own premiums, even though the vast majority of Americans are not in the individual insurance market and are not affected. (A smaller but sizeable percentage believe they are affected when they hear about counties with no or limited insurance options in the ACA marketplaces.)
There are several reasons for this, and the media bears some of the responsibility. Health journalists have generally done an outstanding job covering the issue, but sloppy cable headlines, commentary from pundits, and spin from politicians have too often implied that everyone in America is affected when they are not.
For context: In fact, the rest of the health system where most Americans get their coverage looks very different from the non-group market. As the chart shows:
The back story: Insurers and regulators have been struggling with a unique set of issues in the non-group market, most especially a sicker than expected risk pool and the uncertainty surrounding Trump administration policies. The most important areas of uncertainty have been whether the administration will continue to pay out the $7 billion in cost sharing subsidies and enforce the individual mandate.
But even before the ACA, the non-group market was also the weak link of the insurance system, with sick people priced out or excluded from coverage altogether.
What to watch: Some think a deal on stabilizing the non-group market could be as narrow as an agreement to appropriate the $7 billion in federal cost sharing subsidies in exchange for greater flexibility for states under the ACA. That might not be a slam dunk if that flexibility trips over third rail issues, such as endangering coverage for people with pre-existing conditions.
But whether the formula for a bipartisan deal is that one or another one, policymakers will have a better chance of addressing the problems in the marketplaces if they forge a narrow agreement. And the debate stands a better chance of not spinning out of control if the news media works overtime to help the public understand who is affected and who is not.

An old saying from Six Sigma and other process improvement regimes is that “what gets measured gets done.” That’s important for senior healthcare executives to remember. But that truth leaves out the critical question of what should be measured.
The options are literally endless, but determining the most important metrics to measure in an era in which healthcare is transforming is no trivial decision.
The move toward reimbursement based on the value the healthcare organization provides to the patient and the payer, which is happening at vastly different rates in some geographical areas compared to others, means that asking and answering that question at regular intervals is crucial.
If that’s the case, what are the metrics that leaders need to watch to ensure clinical, financial, and strategic success?
This special issue of HealthLeaders examines how high-performing organizations are instilling and adapting to new performance measures that healthcare leaders need to track to “get value done.”
Our editorial team talked with more than a dozen organizations in a variety of sectors, from leaders of hospital inpatient organizations to payer leaders, from leaders of postacute care organizations to information technology, nursing, and finance leaders; all have measurements they find useful to achieve value in a rapidly transforming healthcare business environment.
Some metrics may be familiar, such as admissions or readmissions per thousand patients. Other metrics may be unfamiliar, such as a “user resource metric,” part of which incorporates the speed with which patient calls are answered at a call center.
Many more important metrics are clinical in nature, but are often monitored and reported by the financial arms of the organization, as they provide a proxy for customer satisfaction, a growing component of the value equation.
Also critical is the latency of such measurements. For example, it’s less valuable to learn about line infection rates and sepsis diagnoses after the patient has been discharged, because little can be done to influence the statistics by that time.