Category Archives: Uncategorized
Cartoon- Losing Management Momentum
Cartoon – Working on a Highly Confidential Project
Cartoon – The Reality of False Hope
Cartoon – EMR’s have done Wonders for Patient Care

In health care, it’s still about the prices

Health care executives gave no indication to bankers and investors at this year’s J.P. Morgan Healthcare Conference that their pricing practices would change any time soon.
Why it matters: That sentiment comes the same week when three of the original authors of an influential 2003 article — which studied why health care is so expensive in the U.S.— published an update. Their conclusion was the same: “It’s still the prices, stupid.”
48% of CFOs don’t have a succession plan

Though CFOs are usually known for their careful attention to detail, 48 percent of them have not identified a successor, according to a study in The Wall Street Journal.
Robert Half Management Resources surveyed 1,100 CFOs in various industries. Of those respondents who have not created a succession plan, nearly two-thirds said they had no plan because they did not intend to step down soon. They also cited the need to focus on other priorities and the absence of qualified candidates.
Jenna Fisher, head of the global corporate sector at executive search firm Russell Reynolds Associates, said the percentage of CFOs with succession plans represents a dramatic improvement from five years ago, when she estimated less than 10 percent of her clients had CFO succession plans.
“The role of CFO has become more salient,” Ms. Fisher said.
Fifth Circuit Hits Pause on ACA Lawsuit Over Government Shutdown

At the urging of the Trump administration, an appellate judge put legal wrangling over the Obama-era law’s constitutionality on hold until the partial government shutdown ends.
The appeals process to review a ruling that declared the entire Affordable Care Act invalid will have to wait until attorneys for the federal government have funding to proceed.
Fifth Circuit Court Judge Leslie H. Southwick issued a stay in the case Friday, granting a request filed earlier in the week by the U.S. Department of Justice.
The pause comes three weeks into a partial government shutdown that’s poised to become this weekend the longest in U.S. history, as President Donald Trump insists that Congress authorize $5.7 billion for a wall along the U.S. border with Mexico and Democrats refuse to do so.
While most of the federal government was funded by earlier legislation, this shutdown affects about 800,000 federal workers and inhibits the work of several agencies that handle health-related tasks.
Both the plaintiffs and federal defendants agreed that a stay would be appropriate. But the California-led coalition of Democratic state attorneys general challenging the lower court’s decision and the U.S. House of Representatives—which, newly under Democratic control, is seeking to intervene in the case to defend the ACA—opposed the stay request.
2019 Healthcare Industry Outlook
Scaling the “specialty care business” across the health system
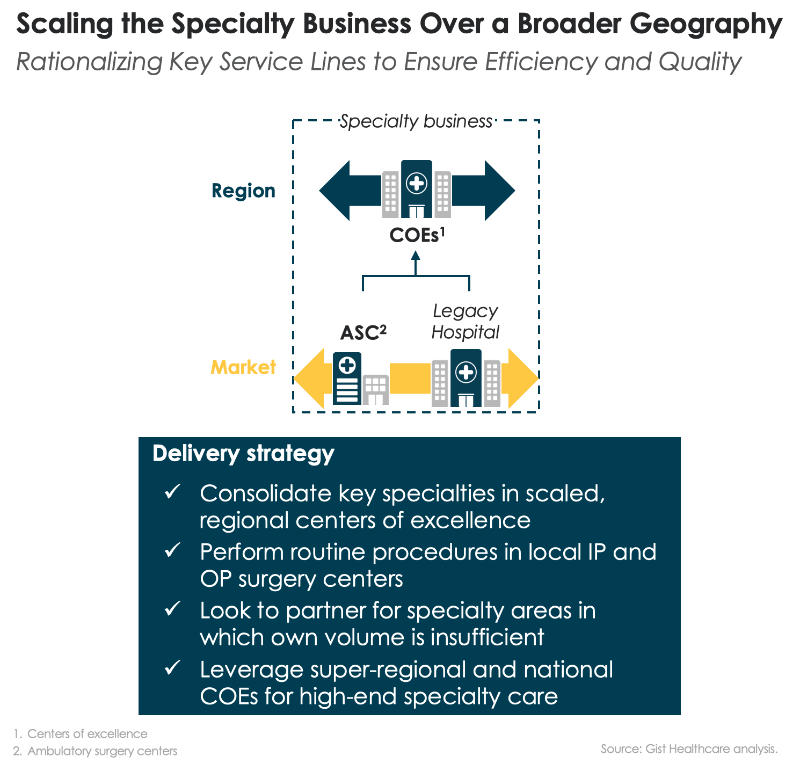
Over the past month we’ve been sharing our framework for helping health systems rethink their approach to investment in delivery assets, built around a functional view of the enterprise. We’ve encouraged providers to take a consumer-oriented approach to planning, starting by asking what consumers need and working backward to what services, programs and facilities are required to meet those needs. That led us to break the enterprise into component parts that perform different “jobs” for the people they serve. We think of each of those parts as a “business”, located at either the market, regional or national level depending on where the best returns to scale are found (and on the geographic scale of any particular system). So far we have described how a consumer-oriented health system should be organized at the market level, with expanded access and senior-care businesses providing lower-cost care in an outpatient setting for many services that were previously delivered in an acute-care hospital, and how the profile of the local hospital needs to change in response.
This week we shift our attention to health system services that can be scaled at the regional level, starting with specialty care, the medical and surgical specialty services that comprise many hospital service lines. Today nearly every community hospital is a “jack of all trades” with the same portfolio of services: obstetrics, cardiac care, orthopedics, and cancer care are the marquee service lines. Incentives, both market-based and internal to the health system, have encouraged this. Hospitals build services aimed at capturing the same handful of profitable (and usually procedurally-focused) DRGs. And many health systems reward local hospital leaders on the profitability of the hospitals they run, creating no incentive for those leaders to shift profitable volume to other hospitals in the system, and often resulting in redundant, inefficient, and sub-scale specialty care services.
We believe many specialty care services could be improved by moving care “up and out” of the community hospital. As we described before, a large portion of routine surgical care could be moved “out” of the hospital to lower-cost outpatient centers, supported by short-stay capabilities and expanded home health. At the same time, more complex specialty care should move “up” in the health system and be concentrated in regional “centers of excellence”, where expensive talent and expertise can be scaled, and systems can aggregate the volume needed for highly-efficient operations that lower the cost of delivering complex specialty care.
While the center of excellence model is not new, it’s often little more than a marketing slogan. Few systems have deployed it for operational efficiency, redirecting specialty care patients to high-volume-centers—and shuttering their low-volume or sub-standard local programs. Even fewer have invested in the infrastructure needed to effectively coordinate care between a regional center and local providers: telemedicine for effective provider collaboration and consultation, effective information sharing, and strong local care management support. One question inevitably arises: will patients travel for care? As individuals bear a larger portion of the cost of care, they do seem to be willing to travel longer distances in pursuit of better value. Understanding how the consumer “travel radius” changes with higher levels of financial accountability, and how that radius differs among services, ought to rank high on the priority list of systems looking to determine what business to consolidate at regional centers.






