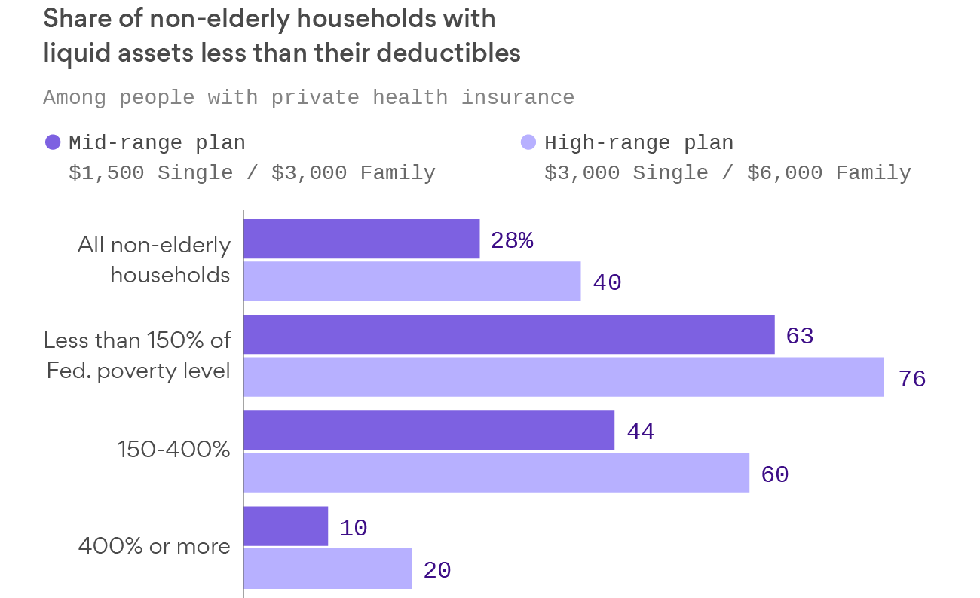https://www.healthcaredive.com/news/middle-income-americans-paying-more-for-health-insurance/543903/

Dive Brief:
- Middle-income families are spending more of their incomes on health insurance as average premiums skyrocketed in 2017 after modest rate increases earlier this decade, The Commonwealth Fund found in a new report.
- Average employee contributions rose to nearly 7% of median income for single and family plans compared to 5.1% a decade ago. Premium contributions were 8% of median income or more in 11 states, including Louisiana, which had the highest percentage (10.2%).
- The contributions and potential out-of-pocket spending for single and family policies was $7,240 in 2017. That was 11.7% of median income and an increase from 7.8% a decade ago.
Dive Insight:
Cost and price variations between areas aren’t anything new. A recent Network for Regional Healthcare Improvement found healthcare usage and pricing drive variation between states’ total healthcare costs. The report also found vast differences in costs between five states studied.
Overall, national health spending has slowed in recent years. The CMS Office of the Actuary reported this month that national health spending grew 3.9% ($10,739 per person) in 2017. It was the second consecutive year of slower healthcare spending growth. The slower cost growth is connected to fewer people receiving care.
The Commonwealth Fund found large differences between states. For instance, the average annual premium contributions for single-person plans ranged from $675 in Hawaii to $1,747 in Massachusetts. Michigan saw the cheapest premiums in family plans at $3,646 while Delaware had the highest at $6,533.
The average annual deductible for single-person policies increased to more than $1,800 in 2017. The gap was between $863 (Hawaii) and about $2,300 (Maine and New Hampshire). Three states (Florida, Mississippi and Tennessee) had average deductibles more than 6% of median income.
Premiums for employer health plans, which is how most Americans get coverage, increased 4.4% for single plans and 5.5% for family plans in 2017. All but five states saw higher single-person premiums with eight states averaging more than $7,000 (Alaska, Connecticut, Delaware, Massachusetts, New Jersey, New York, Rhode Island and Wyoming).
Meanwhile, family premiums increased in 44 states and were $20,000 or more in seven states (Alaska, Connecticut, Massachusetts, New Jersey, New York, West Virginia and Wyoming) and the District of Columbia.
The cost of health insurance is increasing faster than wage growth — and the Commonwealth Fund found that the added cost isn’t leading to higher-quality health insurance. The issue is especially a problem in southern states with lower median incomes, such as Mississippi.
The group suggested policymakers could tackle the problem of rising healthcare costs in a couple of ways.
Congress could provide more tax credits to people with employer-sponsored insurance, require businesses to improve plan benefit design to cover more services before employees reach their deductibles and offer refundable tax credits to offset out-of-pocket costs.
Other potential efforts include connecting provider payments to value and outcomes, addressing the concentration of payer and provider markets and slowing prescription drug cost growth. “Policymakers will need to recognize that the increasing economic strain of healthcare costs facing middle-income and poor Americans is driven by multiple interrelated factors and will require a comprehensive solution,” according to the report.