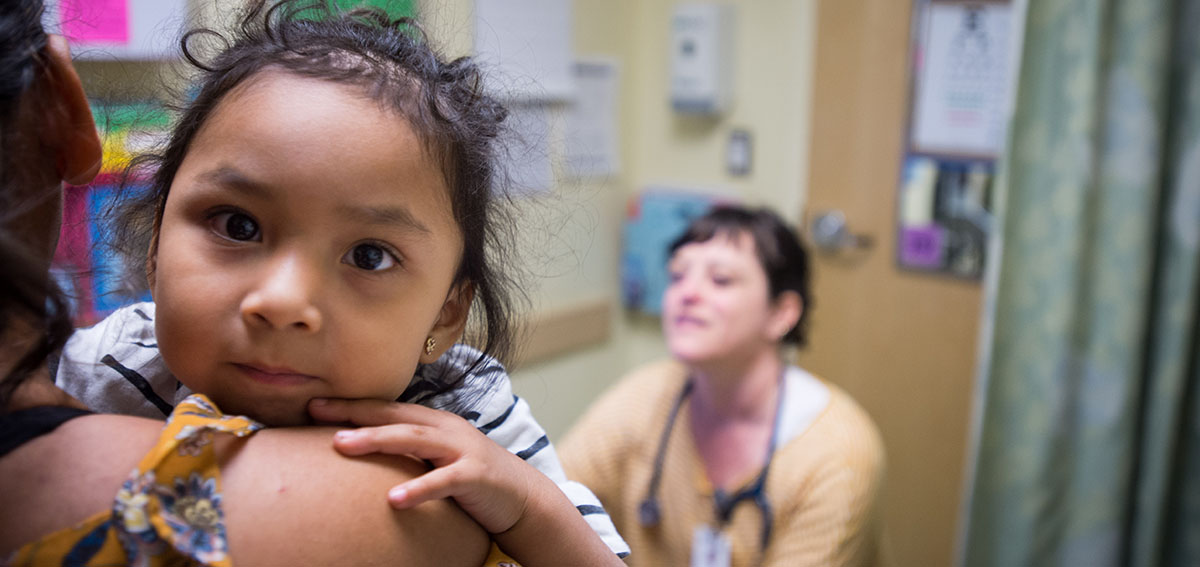Public Charge Rule Could Erode Enrollment in Insurance Coverage
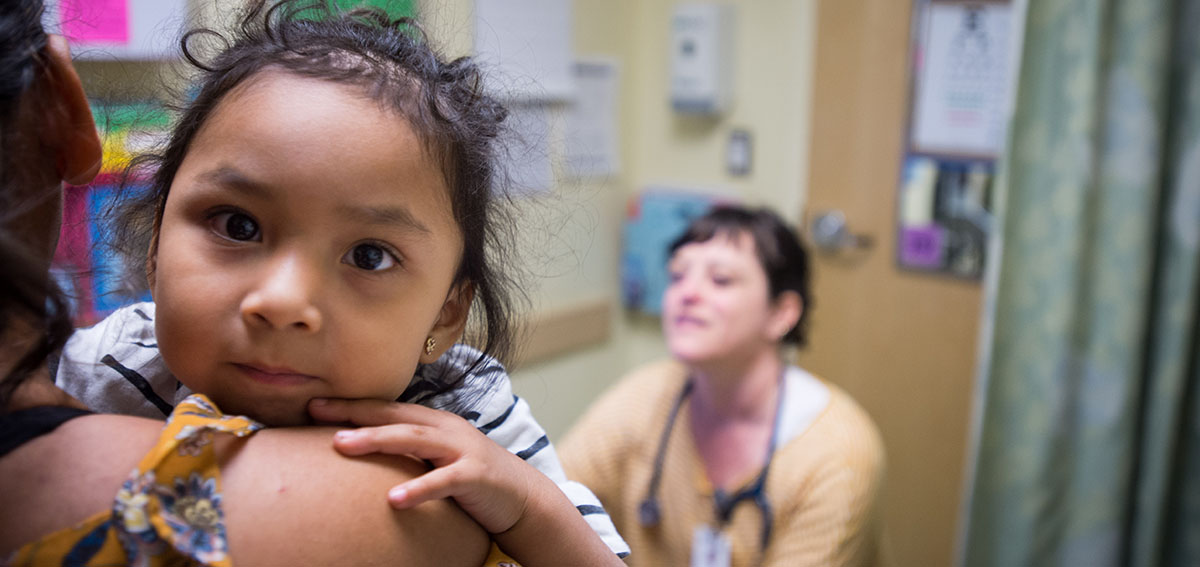
In a 5-4 vote reflecting the ideological split among the justices, the US Supreme Court on January 27 decided to allow the Trump administration to commence enforcement (PDF) of its “public charge” rule nationwide. Only Illinois, where a statewide injunction is currently in effect, will not begin enforcing the rule. The regulation was slated to take effect last October, but federal judges in California, Illinois, Maryland, New York, and Washington blocked its implementation after states and immigrant rights groups challenged its legality. Federal appeals courts later lifted all but New York’s nationwide injunction and Illinois’ statewide injunction. The Supreme Court has now “stayed,” or put on hold, New York’s injunction, allowing the rule to take effect while the litigation continues.
The US Citizenship and Immigration Services agency said the new rule will become effective February 24.
The public charge rule sparked controversy because it “would expand the government’s ability to refuse green cards or visas for legal immigrants determined to be a ‘public charge,’ or dependent on public assistance,” Susannah Luthi explained in Politico. “Those using or likely to use Medicaid, food stamps, and other safety-net programs would face greater scrutiny from immigration officials.”
Experts have warned of a “chilling effect” among immigrant communities, meaning that even those who are not subject to the public charge rule could disenroll or avoid public benefits out of fear. The Institute for Community Health estimated that 195,000 to 455,000 California children in need of medical attention could leave Medi-Cal if the rule takes effect. Including adults, this estimate grows to between 317,000 and 741,000 Californians disenrolling from Medi-Cal, according to researchers from UCLA and UC Berkeley (PDF).
The chilling effect has been documented on a national scale. According to the Urban Institute, in 2018, the year when the Trump administration proposed expanding the public charge rule, about 14% of adults in immigrant families reported that fear prompted them or a family member not to apply for a public benefit program or to disenroll from one. Of the adults who experienced chilling effects, 42% said they or their family members did not participate in Medicaid or the Children’s Health Insurance Program.
Soon after the rule was finalized last year, Eisner Health, a community clinic in Los Angeles, started getting phone calls from patients enrolled in Medi-Cal and CalFresh who wanted to end their families’ coverage, Claudia Boyd-Barrett reported in California Health Report. Many of those patients were not yet permanent residents or were members of mixed immigration status families who feared being penalized for using public benefits.
New Rule Doesn’t Apply to Many Immigrants
It is important to note that many immigrants are not subject to the new public charge rule. “It is urgent that all of us working with immigrant communities — via government, legal aid, health care, and more — have accurate and accessible information for families,” Sandra R. Hernández, president and CEO of CHCF, wrote on Twitter.
Mark Ghaly, California Health and Human Services Agency secretary, released a statement emphasizing that immigrant families should learn their rights. “You can find a list of nonprofit organizations providing free legal immigration services on the California Department of Social Services (CDSS) website, here,” Ghaly said.
CDSS offers a list of legal services providers across California who can assist with public charge questions. Protecting Immigrant Families (a partnership of the National Immigration Law Center and The Center for Law and Social Policy) also has resources on the public charge rule.
Following the Supreme Court’s order to stay the nationwide injunction, California Attorney General Xavier Becerra reiterated his commitment to fighting the rule. “We are a nation of immigrants, so we will lean forward in the face of heartless attacks on working families,” Becerra said in a statement. “Together, we’ll continue our fight to stand up for the right of each and every person who calls the United States their home.”
The legal challenges to the public charge rule will continue to move forward in courts around the nation — including in California — the New York Times’s Adam Liptak reported.
Medicaid Block Grants Could Reduce Access for Many
The Trump administration has announced its plan to let states volunteer to convert a portion of their Medicaid funding into block grants. The program, which has been branded a “Healthy Adult Opportunity,” represents a radical change in financing for Medicaid. Medicaid programs, which are operated by states with significant federal funding and oversight, constitute the nation’s health insurance program for Americans with low incomes. Covering over 75 million people, or one in five Americans, Medicaid programs provide services to 83% of children from low-income families, 48% of children with special health care needs, and 45% of nonelderly adults with disabilities.
On January 30, the administrator of the US Centers for Medicare & Medicaid Services, Seema Verma, sent to state Medicaid directors a letter (PDF) about the new block grant program. Verma gave states “the possibility of trading away an entitlement program that expands and contracts depending on how many poor people need the government health coverage,” Amy Goldstein wrote in the Washington Post. “In exchange, for able-bodied adults in the program, states could apply to receive a fixed federal payment and freedom from many of the program’s rules.”
Additionally, participating states would be allowed to limit the health benefits and drugs offered by their Medicaid programs, Rachel Roubein and Dan Diamond reported for Politico. According to one official, patients with behavioral health needs or HIV would be protected under the new plan.
Criticism from Medicaid advocates was swift. Twenty-seven patient and consumer groups, including the American Lung Association, American Cancer Society, and National Alliance on Mental Illness, issued a statement expressing strong opposition to the new guidance. “Block grants and per capita caps will reduce access to quality and affordable health care for patients with serious and chronic health conditions and are therefore unacceptable to our organizations,” they wrote.
“Worst Medicaid Idea Ever”
Frederick Isasi, executive director of Families USA, said in a statement, “Having spent many years working with governors and Medicaid programs, block grants are possibly the worst Medicaid idea ever presented to states by a federal administration. They would allow the federal government to off-load shared Medicaid responsibility at the expense of deep cuts to state budgets, vital programs supported by states, and the people who rely on those programs.”
Joan Alker, executive director and a cofounder of Georgetown University’s Center for Children and Families, warned in a statement that “if states accept a fixed cap on federal funding to meet their health care needs, they may be able to get by in the short term, but they put the health of their citizens and future state budgets at serious risk down the road.”
The block grant program is unlikely to affect California, which has invested heavily in expanding Medi-Cal access and is not expected to apply to participate.
Nonetheless, the block grant proposal shows that the Trump administration continues to prioritize changes that weaken the foundation of the nation’s health care safety net and could dramatically reduce health coverage for millions of Americans with low incomes.