http://www.healthleadersmedia.com/health-plans/cbo-alexander-murray-bill-would-trim-deficit-keep-americans-insured?spMailingID=12228675&spUserID=MTY3ODg4NTg1MzQ4S0&spJobID=1262308916&spReportId=MTI2MjMwODkxNgS2#

Is the Senate’s bipartisan compromise a workable fix or a ‘futile’ stopgap?
The bipartisan Alexander-Murray bill aimed at propping up the Affordable Care Act long enough for more substantial changes to be made is receiving a mixed response from lobbying groups and legislators, with some saying the bill only extends the life of a system that should be allowed to die.
Supporters say the bill would stabilize a volatile healthcare insurance market and preserve coverage for millions of Americans by continuing the cost sharing reduction (CSR) payments that health plans say are essential to helping them survive the ACA.
The Congressional Budget Office (CBO) and Joint Committee on Taxation (JCT) released an assessment Wednesday of the measure, finding that the deal would reduce the deficit by $3.8 billion over the next decade “without substantially changing the number of people with health insurance coverage, on net.” By contrast, earlier proposals to overhaul the ACA lost steam this year after CBO scores indicated that they would likely drive down the number of insured Americans by tens of millions.
“This nonpartisan analysis shows that our bill provides savings and ensures that funding two years of cost-sharing payments will benefit taxpayers and low-income Americans, not insurance companies,” Sen. Lamar Alexander (R-TN) and Sen. Patty Murray (D-WA) said Wednesday in a joint statement.
The CSR payments are intended to compensate insurers for providing coverage to lower-income consumers at below cost, and many say losing those payments will drive premiums higher and force some insurers to leave certain markets.
The compromise
Alexander and Murray developed the compromise bill in a bid to maintain the CSR subsidies that the Trump administration announced October 12 it would halt. The White House argues the CSRs were never authorized by Congress.
California is leading the charge in a legal challenge of President Trump’s stated intention to stop the payments, and the American Hospital Association, along with several other groups representing hospitals and other healthcare organizations, has filed a brief in support of the CSRs. But a federal judge in California sided Wednesday with the White House, ruling that the government doesn’t have to continue making the payments while states challenge the move in court, Reuters reported.
A bipartisan coalition of 24 senators—12 Republicans and 12 Democrats—have signed on to the healthcare legislation as cosponsors. Preserving the CSRs was a major priority of the Democrats, who compromised by agreeing to the Republican push to allow states to seek waivers of ACA requirements in their own states.
Ending the subsidies is expected to result in healthcare plans raising premiums even higher than otherwise planned. But the Alexander-Murray bill would authorize the CSR payments for two years and tie them to the changes in the ACA that give states more flexibility to seek waivers from the law’s requirements.
The proposed legislation also would allow insurance companies to sell less comprehensive plans to all consumers. Republican leaders say the allowance would make more affordable plans available, which, in turn, would encourage more people to buy coverage and help the insurers remain profitable.
“This is a first step: Improve it, and pass it sooner rather than later. Our purpose is to stabilize and then lower the cost of premiums in the individual insurance market for the year 2018 and 2019,” Alexander said.
Bill opposition
The Association of American Physicians and Surgeons (AAPS) opposes the bill, saying it seeks to stabilize the insurance marketplace by forcing taxpayers to pay insurers to lower out-of-pocket costs for certain plan members.
Jane M. Orient, MD, executive director of AAPS, says the ACA actually makes insurance unaffordable.
“The deceitfully named Affordable Care Act did not just destabilize the individual insurance market; it destroyed it by outlawing genuine, voluntary insurance,” Orient says. “ACA-compliant plans are not true insurance, but coercive prepayment schemes for a federally dictated package that might be rejected by most subscribers.”
Orient says the bill being considered should be seen as an inappropriate form of legislative life support.
“Resuscitating Obamacare with Alexander-Murray would only prolong its dying process, but at great expense,” Orient says.
“Instead of running a futile Code Blue on Obamacare, we should be attending to American medicine and the American economy,” she adds.
Bill ‘provides critical stability’
American College of Emergency Physicians (ACEP) President Becky Parker, MD, FACEP, disagrees.
She says ACEP supports the Alexander-Murray legislation because it will provide critical stability for the individual health insurance marketplace, ensuring that millions of Americans have continued access to the health coverage they need and deserve.
“This legislation is a good-faith bipartisan effort that will help limit increases in health insurance premiums and preserve important consumer protections, such as the Essential Health Benefits package that includes emergency services, while also providing additional flexibility for states to implement innovative approaches to coverage,” Parker says.









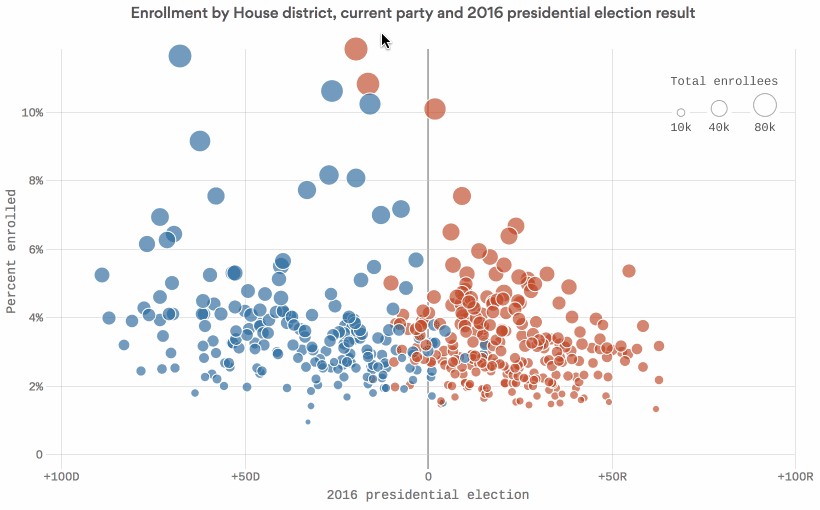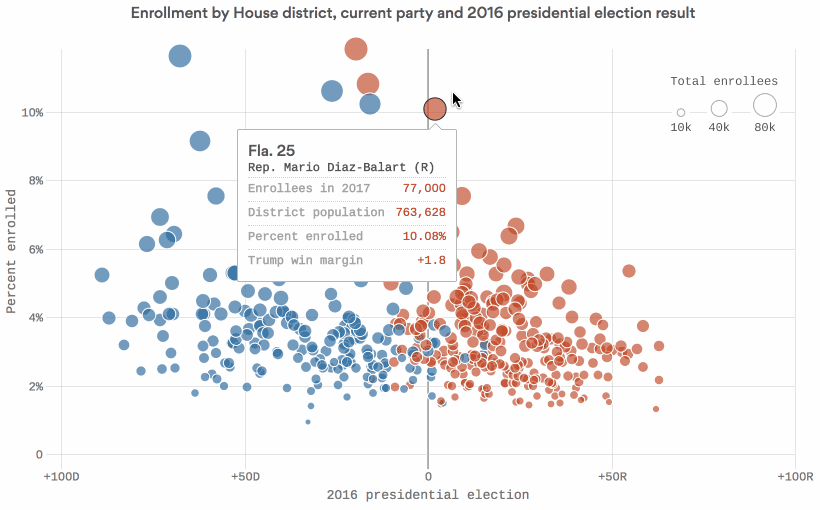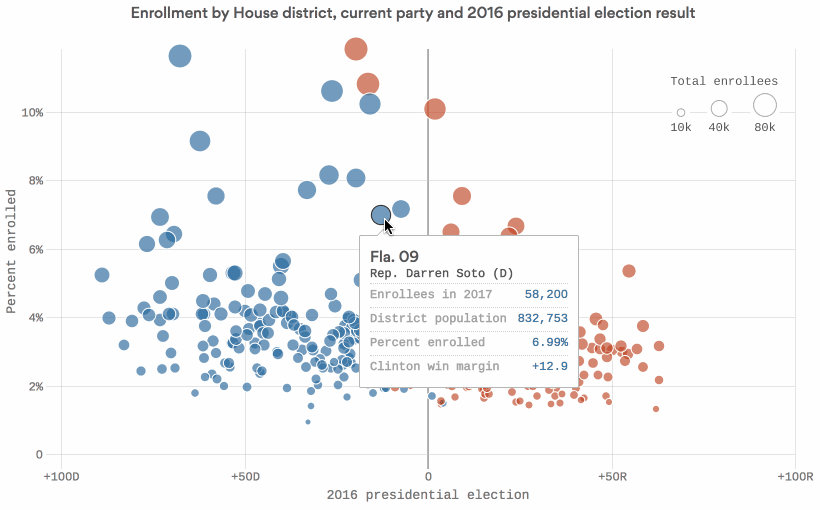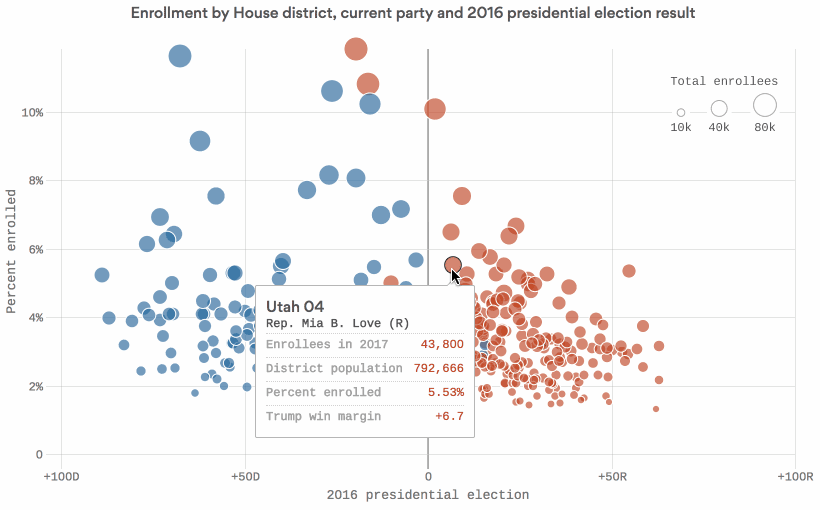 Data: Kaiser Family Foundation; Daily Kos Elections; Census Bureau; Chart: Chris Canipe / Axios
Data: Kaiser Family Foundation; Daily Kos Elections; Census Bureau; Chart: Chris Canipe / Axios