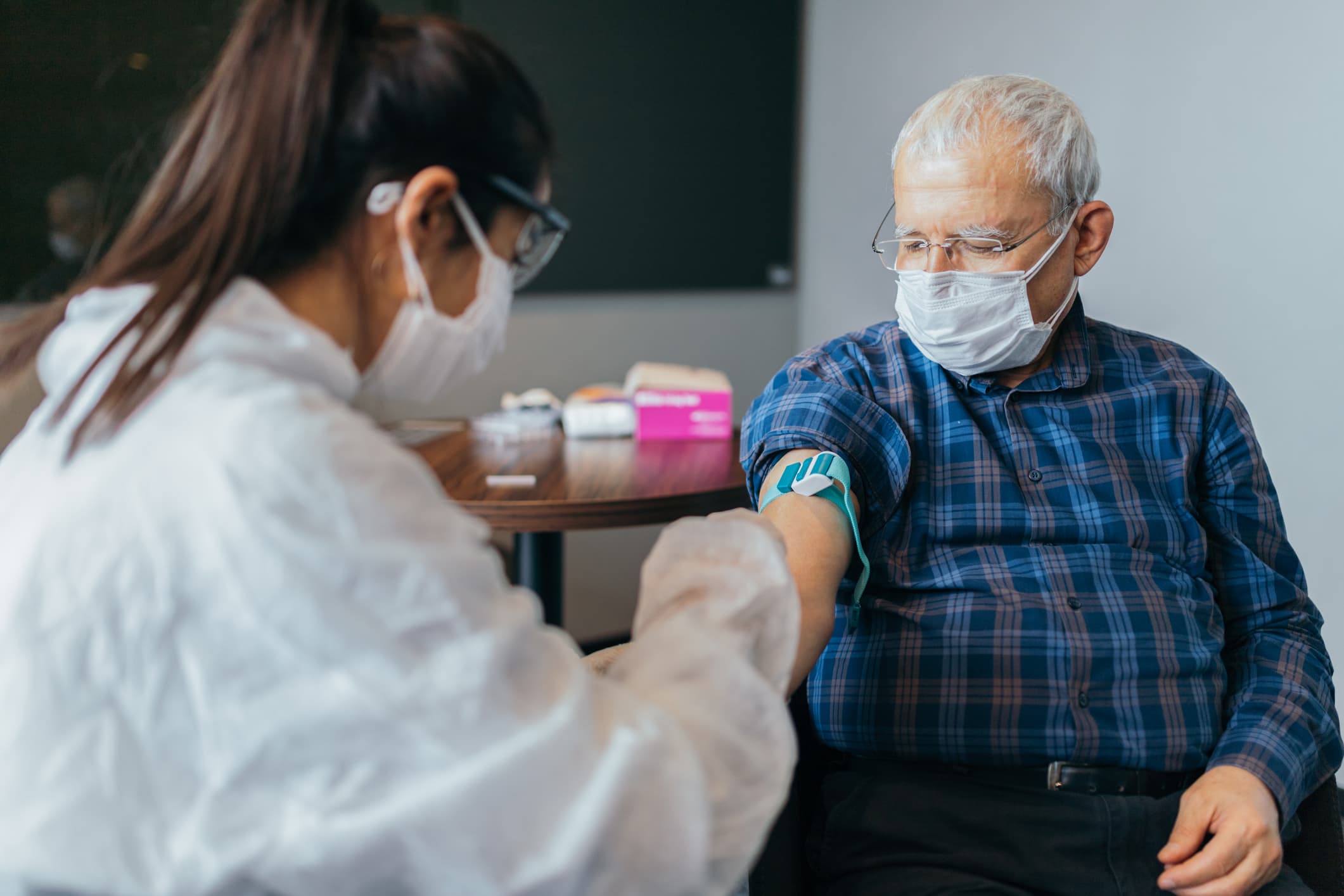
Most seniors have not gotten a COVID-19 vaccine yet, according to an analysis from the Kaiser Family Foundation.
Why it matters: There’s simply not enough vaccine available right now to take on every priority, Axios’ Marisa Fernandez writes.
- Even as states eye the next phase of the process and additional high-risk groups clamor for access, there’s still a long way to go just in protecting most vulnerable.
By the numbers: In the first month of vaccinations, about 29% of recipients were 65 or older, per KFF.
- The first round of vaccines was directed primarily at health care workers and the residents of long-term care facilities.
Where it stands: West Virginia has vaccinated the most seniors at 34%, thanks to a focused effort in nursing homes.
- Nine states — West Virginia, North Carolina, Florida, Mississippi, Delaware, Texas, Michigan, New Jersey, and Wisconsin and Washington, D.C. — report vaccinating at least 20% of seniors.
Yes, but: Demographic data aren’t available in some states and cities, which will make it hard to track how well the U.S. is addressing high-risk groups as more people become eligible.









