https://www.healthcarefinancenews.com/node/139034?mkt_tok=eyJpIjoiWW1OaFpUazJaV1l4TldFeiIsInQiOiJPSUpCQjRXc1E1MTZUUTJIaWFHTWtPWEFTVzRYa0RWTUJ6dFc4ZHNSWlN3aWlKSjlmN3NsajZ0b01PSGkzdHUrQWg1UzR2VUM5QWlSbXdLcG5qUFBIWlVPV1wvWnlKTHlUZ3lNU3JCWG9oM1JLY3hjc3hSRXl3RnBEanlPbUpSZnkifQ%3D%3D

Expanding coverage, lowering healthcare costs, central to Democratic agenda.
Tonight, Joe Biden, Kamala Harris, Cory Booker, Andrew Yang, Julián Castro, Tulsi Gabbard, Michael Bennet, Jay Inslee, Kirsten Gillibrand, Bill de Blasio take the stage for round two of the Democratic presidential debates.
Seven support Medicare for All. The others – Biden, Bennett and Inslee have come out in favor of a public option. Here, in no particular order, is a look at where each candidate stands on healthcare coverage.
Joe Biden
As vice president to President Barack Obama, former Senator Joe Biden carries into this election the legacy of the Affordable Care Act. As president, Biden said he would protect the ACA and prevent further Republican attempts to dismantle it.
Unlike many of his Democratic rivals, Biden does not support full Medicare for All. Instead of getting rid of private insurance, Biden said he would build on the ACA through the Biden Plan to create a public health insurance option. As in Medicare, costs would be reduced through negotiating for lower prices from hospitals and other providers.
He also has a plan to increase the value of the ACA tax credits by eliminating the 400% income cap on tax credit eligibility and lowering the limit on the cost of coverage from 9.86% of income to 8.5%. This means that no one would spend more than 8.5% of their income on health insurance. Additionally, Biden would base the size of tax credits on the cost of the higher-tiered gold plan, rather than silver plan.
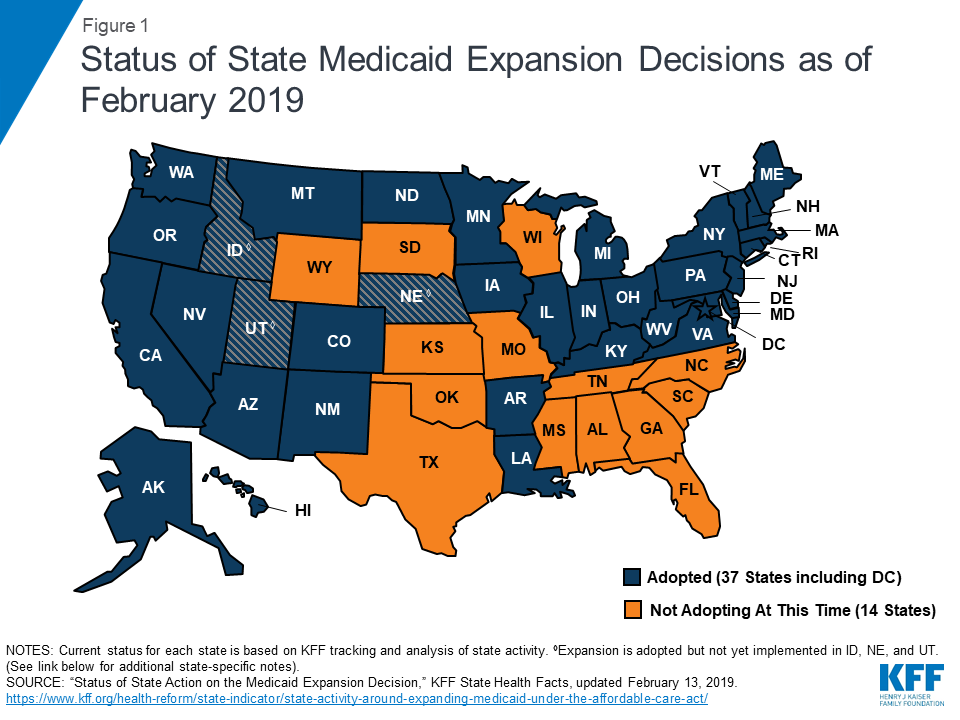
Biden also supports premium-free access to the public option for individuals in the 14 states that have not expanded Medicaid under the ACA. States that have already expanded Medicaid would have the choice of moving the expansion population to the premium-free public option, as long as the states continue to pay their current share of the cost of covering those individuals.
Biden also promises to stop surprise billing, tackle market concentration, repeal the exception allowing drug companies to avoid negotiating with Medicare over drug prices and limiting the launch price for drugs that face no competition, among other actions.
In his words: “When we passed the Affordable Care Act, I told President Obama it was a big deal – or something to that effect.”
Kamala Harris
California Senator Kamala Harris often refers to her mother’s diagnosis of colon cancer and her Medicare coverage for treatment as an example of why all Americans should have Medicare for All.
Harris is looking to eliminate premiums and out-of-pocket costs through government insurance that guarantees comprehensive care including dental and vision and coverage. Harris gives no estimate of the cost of universal healthcare, but says taking profit out of America’s healthcare system would save money.
Her Medicare for All plan, which is similar to Senator Bernie Sanders – would cover all medically necessary services, including emergency room visits, doctor visits, vision, dental, hearing aids, mental health and substance use disorder treatment, telehealth and comprehensive reproductive care services. It would allow the Secretary of Health and Human Services to negotiate for lower prescription drug prices.
As former Attorney General of California who won a $320 million settlment from insurers, Harris said she wants to take on Big Pharma and private insurers to lower the cost of prescription drugs.
She also has strong views on prosecuting opioid makers and for preserving women’s right to healthcare and protecting Planned Parenthood from the financial cuts and policies of the Trump Administration.
She would institute an audit of prescription drug costs to ensure pharmaceutical companies are not charging more than other comparable countries, a comprehensive maternal child health program to reduce deaths among women and infants of color, and rural healthcare reforms, such as increasing residency slots for rural areas with workforce shortages and loan forgiveness for rural healthcare professionals.
In her words on the ACA: “As someone who fought tooth and nail as Attorney General and as Senator to prevent repeal, that’s exactly what I will continue to do.”
Cory Booker
Senator Cory Anthony Booker, first African-American Senator from New Jersey, and former mayor of Newark, is also a Medicare for All proponent.
He also wants to implement universal paid family and medical leave.
He supports lowering costs for prescription drugs by allowing Medicare to negotiate prices and by importing drugs from Canada and other countries, the latter a policy announced today by Health and Human Services Secretary Alex Azar.
He would also invest in ending the maternal mortality rate and work to reduce racial disparities in maternal mortality rates.
One of his big issues is expanding eligibility for long-term services and support for low and middle-income Americans needing care at home. He wants long-term care workers to be paid a minimum of $15 an hour.To limit the impact of the program on state budgets, the new costs associated with the expansion of Medicaid long-term care services and workforce standards would be financed entirely by the federal government in, effectively, a 100% match. The cost would be financed by making the tax code more progressive by reforming the capital gains, estate, and income taxes.
In his words: “Healthcare is a human right.”
Kirsten Gillebrand
Kirsten Gillebrand, U.S. Senator from New York, originally ran for a House seat in that state on a platform that supported the expansion of Medicare, a view she still holds, and in 2017 expressed support for Senator Bernie Sanders’ Medicare for All bill.
In May, Gillebrand reiterated her support, saying the best way to achieve a single-payer system is to let people buy-in over a transition period of about four to five years. She favors allowing a public option to create competition with insurance companies. Medicare needs to be fixed first so that reimbursement rates better reflect costs, she said.
In 2011 she helped pass the James Zadroga 9/11 Health and Compensation Act, which provides treatment to the first responders of the Sept. 11, 2001 terrorist attacks. The law provides health monitoring and services for 9/11-related health issues among those exposed to the debris and tainted air of the attack’s aftermath.
In her words: “Under the healthcare system we have now, too many insurance companies continue to value their profits more than they value the people they are supposed to be helping.”
Bill de Blasio
New York Mayor Bill de Blasio believes everyone, including undocumented immigrants, has a right to receive healthcare, and has repeatedly voiced his support for a national single-payer health plan.
He and rival Elizabeth Warren raised their hands during the first debate when asked if they supported Medicare for All.
One of his accomplishments as mayor was signing a bill into law that established a paid sick leave and safe leave plan for the city.
First unveiled in January, the program NYC Care, guarantees healthcare for the roughly 600,000 New Yorkers who aren’t currently insured, which de Blasio touted as the “most comprehensive health system in the nation.” He has indicated that NYC Care could become a model nationwide.
The plan encompasses primary and specialty care, pediatric and maternity care and mental health services. The idea is that NYC Care works on what de Blasio said was a “sliding scale,” in which people can essentially pay what they can for care. While the city already has a public option for healthcare, de Blasio said NYC Care will pay for direct comprehensive care for people who can’t afford insurance or who aren’t covered by Medicaid.
The program costs $100 million per year for the city — an investment the mayor expects will yield returns.
In his words: “If we don’t help people get their healthcare, we’re going to pay plenty on the back end when people get really sick,” he said recently on MSNBC’s “Morning Joe” broadcast.
Jay Inslee
Washington Governor Jay Inslee has planted a flag as “the climate change candidate” and in many ways he’s all in on that single issue, reasoning that things like healthcare policy “become relatively moot if the entire ecosystem collapses on which human life depends.”
That said, he has a strong case to make on healthcare by virtue of having just recently put his state’s money where his fellow candidates’ mouths are: in May he signed the country’s first public option into law in Washington.
Expect him to bring up that accomplishment — in which the state will contract with private insurers to create a public option that pays at Medicare plus 60 percent — in any conversation about healthcare, as he did in the first debate.
In his words: “We hope this will be a smashing success. We hope that it will give a shot of courage to other governors to move forward toward universal access. We were willing to take the leap and we’re gonna learn as we go along, I’m sure, and there will be some modifications. But we had to get started.”
Michael Bennet
Colorado Senator Michael Bennet supports a public option he calls Medicare-X. But where his plan stands apart from others is a strong focus on the rural-urban divide on access to care. He intends to create a healthcare policy that will ensure that all regions of the country are covered by available health plans, addressing what he calls a failure of the ACA exchanges.
His plan is unusually detailed and includes lowering prescription drug prices, closing existing gaps in care, and, yes, promoting telemedicine and other technology that can bolster rural healthcare. He also has provisions for combatting substance abuse, improving maternal and mental health, and bringing more support to senior caregivers.
In his words: “As president, I would build on the Affordable Care Act to cover everyone, rather than doing away with our current system. My Medicare-X plan gives every family the choice to buy an affordable public option or keep the plan they have today. It starts in rural areas, where there is very little competition and requires the federal government to negotiate drug prices. I have fought for this approach for almost a decade, because it is the most effective and fastest way to cover everyone and drive down costs.”
Julián Castro
The former U.S. Secretary of Housing and Urban Development and San Antonio Mayor favors a Medicare for All, single-payer system.
To pay for the system, Castro has said he would raise taxes on corporations and on the wealthiest Americans — the “0.05, 0.5 or 1%,” he said.
While he favors a single-payer system, Castro said he would allow private insurance, saying that anyone who wants their own private insurance plan should be able to have one.
In his words: Castro said at an event in Iowa that, “The U.S. should be the healthiest nation in the world.”
Andrew Yang
Entrepreneur Andrew Yang of New York is founder of Venture for America, a two-year fellowship program for recent grads who want to work at a startup and create jobs in American cities.
He supports Medicare for All and has called the Affordable Care Act a step in the right direction that didn’t go far enough because access to medicine isn’t guaranteed and the incentives for healthcare providers don’t align with providing quality, efficient care.
Doctors are incentivized to act as factory workers, he has said, churning through patients and prescribing redundant tests, rather than doing what they’d prefer–spending extra time with each patient to ensure overall health.
Medicare for All will increase access to preventive care, bringing overall healthcare costs down. Cost can also be controlled directly by setting prices provided for medical services.
He cites the Cleveland Clinic, where doctors are paid a flat salary instead of by a price-for-service model. Redundant tests are at a minimum, and physician turnover is much lower than at comparable hospitals, he said.
And the Southcentral Foundation which uses a holistic approach to treat native Alaskans with mental and physical problems by referring patients to psychologists during routine physicals.
Also, the current system of employer-sponsored insurance prevents employees from having economic mobility.
In his words: “New technologies – robots, software, artificial intelligence – have already destroyed more than 4 million U.S. jobs, and in the next 5-10 years, they will eliminate millions more.”
Tulsi Gabbard
Rep. Tulsi Gabbard of Hawaii is a military veteran who supports Medicare for All as a cosponsor of H.R.676, the Expanded & Improved Medicare for All Act.
But she is currently getting press for her lawsuit against Google claiming alleged election interference.
Following the first Democratic primary debate on June 26, many people searched her name, but “without any explanation, Google suspended Tulsi’s Google Ads account,” her office said in a statement, according to The Verge.
Tulsi claims the tech giant suspended her campaign’s Google Ads account just after that first debate.
Congress must act to prevent the tech giant from exerting too much influence, she claimed Monday on “Tucker Carlson Tonight.”
In her words: “This is really about the unchecked power these big tech monopolies have over our public discourse and how this is a real threat to our freedom of speech and to our fair elections.”