Category Archives: Talent Identification
Cartoon – Staffing Today
Cartoon – Next Generation Leadership
Health systems bulk up C-suites ahead of transformation

Faced with tighter margins and continued rising costs, many health system C-suites are restructuring. At least 17 health systems have reorganized executive teams and some eliminated C-suite roles.
The chief operating officer role in particular has been on the chopping block for health systems but not everyone is slimming down.
Some are bulking up amid organizational transformation with an eye on the future.
In June, Sutter Health in Sacramento, Calif., named Todd Smith, MD, its inaugural senior vice president and chief physician executive, responsible for supporting the health system through clinical transformation. Dr. Smith will focus on service line standards, reducing variation and strengthening the system’s relationship with medical group and community physicians.
Sutter isn’t the only system adding clinical leaders to the C-suite. Mass General Brigham in Somerville, Mass., named Erica Shenoy, MD, PhD, its first chief of infection control in June. Her expanded role is accountable for leading the integration of infection control at the system and developing and implementing infection control standards, policies and measurements. She was also appointed to the National Infection Control Advisory Committee to guide HHS earlier this year.
Meritus Health in Hagerstown, Md., added physician leadership to its executive team. Adrian Park, MD, became the system’s first chief surgical officer with responsibility for building a surgical program with advanced technology and minimally invasive procedures to the system. He is known for surgical innovation in laparoscopic techniques, and holds more than 20 patents.
MaineHealth in Portland recently added Chris Thompson, MD, to the C-suite as the system’s first chief medical transformation officer. He is responsible for chief medical officer duties as well as innovating in care delivery.
Richmond, Va.-based VCU Health and OU Health in Oklahoma City named their first chief nursing executives as well earlier this year.
Health systems are also adding strategic experts with expertise in patient experience, transformation and data analytics.
Atlanta-based Emory Healthcare created a new role for Amaka Eneanya, MD, to serve as chief transformation officer, accountable for enhancing patient and clinician experiences. She took on the role in July and is tasked with developing systemwide strategies to boost patient experience, improve access to care, increase community engagement and enrich clinician experience. Dr. Eneanya works with the system’s diversity, equity and inclusion office to prioritize strategies for health equity, diversity and inclusion in care delivery as well.
“Amaka is a forward-thinking leader who is well versed in transformational strategy and operational structure and will help us move Emory Healthcare to the next level,” said Joon S. Lee, MD, CEO of Emory Healthcare. “We look forward to working with her in our continued pursuit to transform and strengthen patient access and the patient experience.”
Last year, Centura Health in Centennial, Colo., also added a chief transformation officer, Scott Lichtenberger, MD, as a new position to balance short-term improvements and long-term value. He is responsible for ensuring the system delivers results quickly.
Finally, Cleveland Clinic has elevated another IT leader into the C-suite in recent weeks. Albert Marinez was named the system’s first chief analytics officer, set to begin his new role Aug. 28. He previously served as chief analytics officer of Intermountain Health in Salt Lake City, and will be responsible for overseeing data strategies for better patient care and lower costs at Cleveland Clinic. He will also have accountability for boosting the system’s growth alongside chief digital officer Rohit Chandra, PhD.
The dawn of the interim CFO

With companies fighting for financial know-how, a spotlight is beginning to shine on leaders who can bring the skill sets and expertise firms need in the moment.
Demand for interim leaders shot up significantly during the past 12 months, a report by Business Talent Group, a Heidrick & Struggles company, found, rising 116% year-over-year. Requests for on-demand finance chiefs in particular saw a considerable spike, increasing by 103% YoY, boosted by both continued economic uncertainty and the growing complexities of the CFO role.
The rising demand for interim CFOs is also partly due to growing awareness of the availability of such short-term expertise, said Sandra Pinnavaia, Chief Innovation Officer for BTG.
“Companies, as they get more comfortable and aware of the fact that there is this on-demand talent world, it allows them to contemplate different kinds of changes and uses than before,” Pinnavaia said. “So I do think there’s an underlying driver here, that is in a sense, supply creates demand.”
The interim CFO’s appeal
For companies, interims can help firms navigate through tricky periods or transitions. Requests for interim CFOs made up half of all interim C-suite requests, according to the BTG report. Companies are specifically searching for financial leadership skilled in financial controls, accounting and audit. Demand for such expertise rose 76% YoY.
For finance leaders, the higher demand coincides with gains in the compensation and benefits that accompany the role, said Jack McCullough, President of the CFO Leadership Council.
There’s better money available for CFOs who do this type of contract or interim work, leading to more executives interested in these types of jobs, McCullough said in an interview. For example, some part-time CFOs have begun to receive stock options, he said, referring to a CFO who received the benefit at three startups.
Taking an interim role can also be a refreshing change for finance leaders who want to apply their skills in new areas, according to Diane Buckley, managing partner of Forte Financial Consulting LLC. Buckley, a veteran of Big Four accounting firm Ernst & Young, was drawn to interim and fractional CFO work because it afforded her the option to share her skills with growing companies and “really be impactful day one,” she said.
“It was like, ‘I can bring value to smaller companies that may not at this point in their growth warrant a full-time CFO, but I can bring that skill set to them,’” she said in an interview.
On the supply side, shifting workforce trends may be prompting more companies to take a second look at what they need from their leadership.
Talent shortages across the accounting and finance space mean companies may be facing a year-long period to find a qualified CFO, making it more necessary to put in an interim “even if it’s not the ideal person,” McCullough said.
Meanwhile, the pandemic has also left a lasting mark: BTG clients have tapped more interims because “they have been forced over the last few years, to redefine their whole way of working,” Pinnavaia said.
“Now obviously we have a huge spectrum — there are companies that are back full-time, in-person every day, and there are companies that have really changed their business model and they’re not in-person at all,” she said. “But I think that has loosened up the aperture for what would be an acceptable solution” when it comes to leadership, she said.
The right talent at the right time
Hiring on-demand talent also allows companies to find a leader who can meet their needs in the moment — and since many interims come into a company to solve a particular problem or meet a specific goal, one’s skills are “kind of by definition matched to what the issues are,” said Reed Malleck, CFO of Ratio Therapeutics.
CFOs often need to operate in “four dimensions,” he said in an interview, including accounting, operational skills, investor relations and the ability to participate in the execution of strategy for the business.
“If you’re a permanent CFO, you have to cover all of those, even though you might be really good at only one of them,” according to Malleck, an experienced interim executive who took on several such roles as an engagement partner with executive talent firm Tatum, a Randstad company. “But as an interim person, it’s more targeted, like, ‘we need a guy who’s really good at operations. We need this thing to be fixed.’”
Being able to slot one’s skills perfectly into the situation can be a huge benefit for CFOs, many of whom are dealing with expanding job creep. While becoming an interim is not necessarily less stressful than a permanent CFO position, “in a way, you get relief when you get to the point where you fix everything, and when you’re in a permanent role that never happens,” Malleck said. “When you’re in a permanent role, there’s always something new that’s a new problem.”
With CFOs taking on more responsibility for areas like digital transformation, keeping up with the books and juggling other operational needs across the organization, “the CFO is blamed for this and blamed for that … increasingly, people get burnt out or there’s a loss of trust,” he said.
“Hundreds of analysts are looking at your stock and your performance, the market and the competitors and the technology and you have to explain things not once a quarter, but like five times a day,” Malleck said.
Succession planning is vital
Another often unexplored benefit of on-demand talent is as a source of expertise for future company leaders. A shortage of talent in the finance and accounting fields is worsening, with potential accountants lured away by shinier fields such as technology.
As a result, building a pipeline for executives with CFO skills is crucial.
Moreover, CFOs who were at the top financial seat the last time the U.S. saw serious inflation in the 1980s have long since retired, McCullough said. Finance leaders today face a “steep learning curve.”
“CFOs, through no fault of their own, they haven’t had to develop the skills” necessary to navigate current economic turmoil, he said.
Many CFOs with decades of experience are also either looking to retire, or seeking promotion rather than lateral opportunities, said Shawn Cole, president of boutique executive search firm Cowen Partners.
The jump from the CFO to the CEO seat is “way more commonplace” today than it was just a few decades ago, Cole said in an interview, opening up more opportunities for finance heads. Promoting internal candidates to an interim chair can be an easier and more affordable way for certain companies — faced with both a dearth of qualified external candidates and shaky succession planning — to fill the seat while they hunt for a long-term replacement, he said.
“For the last decade or so, businesses have been in like a boom or bust kind of scenario,” Cole said. “And so I think there’s just this lack of investment in a future generation.”
Whether an internal or external interim hire, the executive should also be a welcome and engaged part of the search for a long-term candidate, Cole said. It is part of their fiduciary obligations to a company and its shareholders to “do the necessary due diligence to make an informed hire.”
While internal interims can be an affordable choice, there can also be drawbacks: the “most damning issue” being when an internal interim pick is acting both as interim CFO as well as retaining the responsibilities of their original role at the company, Cole said.
“So what they wind up being is CFO in name only and they still are fulfilling the role of financial reporting or something like that,” he said.
Interims and on-demand talent will probably play a greater role in a company as time goes on, Pinnavaia said. She pointed to clients who might think they need an interim CFO, for example, but who are really searching for an expert or CFO who is able to do a specific project with the existing leadership team. In such a scenario, hiring an interim controller or another executive on-demand with the right finance skills would be the best way forward, she said.
“I’m very excited about this as an innovation in how business gets done,” she said. “It is a way of applying … real time alignment of skill and capacity against particular challenges or opportunities in the business.”
Cartoon – Talent Screening
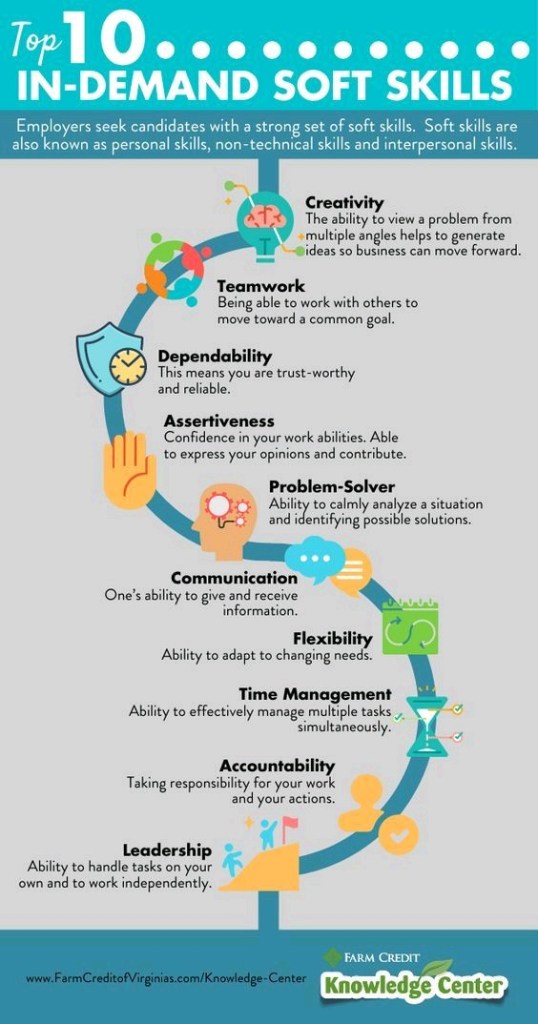
Top 10 In-Demand Soft Skills
Hospitals living paycheck to paycheck, unable to make long-term investments

Healthcare added almost 45,000 jobs in November, but many hospitals and health systems will continue to struggle to meet staffing needs, retain top executives and providers, and foster long-term pipelines for talent, Ted Chien, president and CEO of independent consulting firm SullivanCotter, wrote in a Dec. 15 article for Nasdaq.
Hospitals and health systems are living “paycheck to paycheck” and unable to make long-term investments at the height of the current workforce crisis, Mr. Chien said.
The challenge boils down to a healthcare delivery problem, not a demand problem.
Baby Boomers are the greatest source of care demand on the healthcare system, but are unable to contribute to the provider workforce in the numbers needed to achieve balance, according to Mr. Chien. To compound that issue, burnout is a major factor why “too many” frontline workers have left or plan to exit healthcare, he said.
Last year, an estimated 333,942 healthcare providers dropped out of the workforce, including about 53,000 nurse practitioners, which has led hospitals to spend more on contract labor and feeling more pressure to consolidate, according to an October report published by Definitive Healthcare.
Long term, a continued lack of healthcare workers would force hospitals to operate in a heightened crisis mode, according to Mr. Chien, depriving non-critical patients of sufficient health prevention and demanding too much of providers who are already overly taxed.
Mr. Chien highlighted three key areas to tackle the workforce crisis: smarter technology, resilient teams and excellent leadership.
Technologies that alleviate providers’ administrative burdens will be critical to reduce burnout and keep caregivers focused on patient care, while smarter tech can also forge pipelines for future providers by streamlining clinical experience operations and aligning student placements with existing opportunities.
Building resilient teams begins with competitive pay and robust benefit packages, which fosters trust and demonstrates that a hospital values its staff, according to Mr. Chen. Supporting career growth, including upskilling and redeploying staff when appropriate, empowers employees.
Lastly, capable executive leadership teams, under intense scrutiny from industry stakeholders, must clearly outline their hospital or health system’s strategy and provide the change needed to support their staff. Lack of trust in leaders drives staff out of healthcare, so it is crucial to recruit and retain “modern, strategic thinkers with depth of experience who are prepared to lead,” Mr. Chien wrote.
Click here to read the full article.
Cartoon – Resume Coupon
These are the questions candidates must ask during a job interview

Job seeking is a grueling process, but it is also an opportunity to put your best foot forward in order to find a company that is the best fit for you.
Although it can be nerve wracking to sit through one interview after another, candidates should remind themselves that these interactions are a two-way street, and they have every right to ask challenging questions to make a decision, should the offer come.
Here are the critical questions you as a candidate must ask during a job interview—because remember, you’re interviewing the employer, too.
QUESTIONS TO ASK YOURSELF BEFORE APPLYING FOR THE JOB
Before setting off on your job search, make a list of the types of companies you’re interested in.
- Is this a place you see yourself thriving in?
- Do you believe in the mission?
- Why do you want to work at this place?
- What attracts you about the organization?
Oftentimes, our current situations dictate how we go about making our next move. Perhaps you’re working in an environment that you find suffocating and want out, or you’re seeking more responsibilities, or are looking to become a people manager.
Whatever the case, be sure to keep in mind that in every new workplace, there will be pros and cons, no matter the salary or job description. So be cognizant of all the aspects of a new role that are truly important to you; also, be mindful of what your personal dealbreakers are.
PREPARE A LIST OF STRATEGICALLY PLANNED QUESTIONS
Interviewing is a two-way exchange. While candidates are being scrutinized by the potential employer, the skilled candidate will have an opportunity to evaluate the company based on the flow of the conversation.
Typically, candidates aren’t given the opportunity to ask questions until the very end of the interview. That’s not to say there aren’t ways to integrate specific queries into the conversation, as long as you remember that you’ll get full control of the floor in the grand finale.
In a previous Fast Company story, Patrick Mullane, executive director of Harvard Business School Online, shares how interviewees often will drop the ball when the interviewer tosses out the famous line, “Do you have any questions for me?”
“Candidates forget that when they’re given control of the discussion, it’s an opportunity to do two very important things. First, it’s a chance to learn something genuinely useful about the firm you might be joining. Second, you get to show that you’re thoughtful and conscientious,” he said. “Both are hugely important as you look to make a change. Don’t waste the opportunity.”
When it comes to the questions candidates typically ask companies during an interview, the “big three” revolve around corporate culture, the interviewer’s personal experience (“How have you liked working here?”), and growth.
Rather than default on these inquiries (which interviewers likely receive quite often and may respond in kind with generic answers), Mullane challenged candidates to take these questions and reframe them in a more thoughtful, strategic way:
Culture questions: Rather than asking, “What’s the culture like here,” ask something along the lines of, “Can you share a time when the company’s culture made you excited to work here or helped you during a challenging time?” This bypasses a typical answer like “It’s collaborative,” and dives into the intersection of employees and culture, offering an in-depth look into a specific, and perhaps relatable, scenario.
Personal experience questions: Instead of “How do you like working here?” try, “I noticed you left X company for this one. What convinced you to make the jump?” This reframing achieves two things: It shows the interviewer you did your research and gives you insight into their decision-making, which may help you make your own.
Company growth questions: A question like, “I noticed the company is growing rapidly. Do you expect that to continue?” will often bear a generic, dead-end answer. To get additional, more useful information, put a spin on it. Ask something like, “I noticed the company is expanding rapidly. Is this putting a strain on your customer service team?” Getting information on a company’s financials is not particularly difficult, especially if it is already publicly traded. But asking a question of this nature is especially useful if you are interviewing for a role like Customer Success Manager, as it allows you to get a better sense of how growth impacts the day-to-day of the team.
Overall, it will only work in your favor when you do your due diligence in gathering intelligence on the company you are interviewing for; also, you’ll be setting yourself up for success by having prepared questions that lead to a conversation and present yourself as a thoughtful and conscientious candidate.
“In a hot job market, it’s tempting to be lazy when doing the upfront work to prepare for an interview,” said Mullane. “It’s easy to figure that the interview is over when the person interviewing you gives you the floor. But it’s not. Asking better questions in the right way can significantly increase the chances you’ll not only impress the interviewer, but also gain valuable insights that can help you decide if the position is right for you.”
COVER THE BASICS
It can be easy to get caught up in nerves when interviewing for a company you are extremely attracted to—or even in general. Interviewing is a lot of pressure!
However, when preparing to ask your questions, the areas that you as a candidate must focus on should give you a well-rounded perspective on multiple aspects of the company, not just the specific job description.
This Fast Company article shared a roundup of all the pertinent focus areas that your questions should fall under to get you the best answers, which include:
- The specific role you are interviewing for
- The management style of your would-be boss or team
- Company culture and reputation
- What performance metrics look like
- What kind of colleagues you can expect to work with
- Opportunities for growth
ASK TOUGH BUT FAIR HIGH-LEVEL QUESTIONS
Sometimes it’s not enough to consider the high-level questions, such as salary and work culture. Many of us are in a unique position in life, whether that involves our personal situations, families, health, or other concerns.
When considering your interest in a company, it’s helpful to understand how they can help or support you as an individual beyond your contributions to the job.
On the flip side, you’ll want to know other aspects of internal support for employees. How does this company support internal mobility? How do managers deliver feedback? In other words, what will a day in the life of this role really be like?
Prepare to ask the employer a series of questions tailored to your situation. FlexJobs’ team of career coaches offers guidance in this Fast Company story, including specific inquiries to ask your interviewer, such as:
- Why is this position available? This can give you some insight into the way things are handled at the company. Was someone fired? Are they unable to keep the position filled because of the workload?
- What makes it a great day at work, and what makes it a challenging day? Answers to this question can vary depending on the personal experience of the interviewer, but it’s good to get a sense of how they approach the question.
- How are criticism and feedback handled within the team? Mistakes can happen, and knowing that managers on the team can handle employee errors with grace will offer a sense of relief rather than unnecessary conflict when they do occur.
- Do you have any Employee Resource Groups (ERGs)? How do they support the company’s DEI plans? This question gives you an opportunity to understand where the company stands in terms of diversity, equity, and inclusion (DEI) and how well they support the objectives of ERGs, as well as pushing forward their higher-level strategy.
- How does the company approach salary differences? This can highlight whether the company pays people differently based on location, if they work remotely, in-office, or hybrid. It can also shed light on whether the company has done a pay audit to achieve equity, especially for women and underrepresented groups.
- What’s the company’s approach to supporting work-life balance? Many companies have put forth specific benefits and incentives to support employees in the past two years, including mental health initiatives, fitness classes, therapy, and flexibility. This critical question will help you determine just how the company views employees as individuals and not just by their work output.
An example of a tough conversation to navigate can pertain to how the organization supports employees in specific work situations. If this particular job requires you to relocate, an example of how to navigate the question of moving-cost accommodations might go something like this:
Candidate (C): I noticed this position is based in San Francisco. Is there an option for potential hires to work remotely?
Interviewer (I): I’m afraid our new company policy is to operate on a hybrid schedule. This particular role is based in the Bay Area and requires the individual to come into work three times a week.
C: I understand. Sometimes companies need to make tough decisions based on their needs.
I: Do you think you would be willing to relocate, should we decide to move forward with your application?
C: I think this role is a wonderful opportunity for me, and I truly believe my personal values align with those of this company and its culture. If all goes well, I’d like to learn what the company’s budget is in regards to supporting moving and transition costs.
In this scenario, the interviewer is honest about the new hybrid model their company has adopted. If you, the candidate, are first learning about this aspect during the interview, it’s important to ask direct questions about how the company plans to support potential moving costs, rather than framing the question in a way that offers a loophole or an out.
Organizations are aware that with the plentiful options of remote jobs, finding talent willing to relocate or adopt a hybrid work life will be tougher. Know that the ball is in your court and be straightforward about expensed costs if you are willing to relocate.
WRAP UP THE INTERVIEW WITH THESE KEY QUESTIONS
This will likely be the last time you interact with this team member before either moving onto the next stage or the decision-making process.
In a prior Fast Company story, the founder of executive search firm The Mullings Group shares the best questions to ask when wrapping up.
Don’t let the conversation end without answers to the following questions, so you have enough information to help you reflect on and assess your experience and understanding of the company.
Am I a good fit for this company? The feeling needs to be mutual. Be sure to determine whether your skills, interests, personality, and goals align with the direction of the company.
What are the expected deliverables for this role over the next three months to a year? Depending on the role of the person you are interviewing with, you may get different answers. This is a good question to ask to get a sense of the priorities as it relates to different stakeholders.
How will we both know that I have succeeded in this role? This is another question in which the answers may vary, but it will be helpful for you as a candidate to understand how to work toward specific goals and measure your own impact so that, when it comes time for a raise or promotion in the future, you have the evidence to back it up.
What are the growth opportunities in this role, and what important skills will I learn? It’s not enough to make a lateral move. You need to know how will working for this company enable you to grow and thrive.
Who will I become? Your environment and the people you work with will directly influence your work output, ethic, and your future values. Asking questions about the kind of people you will interact with regularly will help you get a sense of what your day-to-day experiences will look like.
Getting a new job is a big deal. You will be working 40 hours a week in a specific environment that supports a certain culture and hires a certain type of colleague. It’s not just the job description that matters, nor the skill set the company requires to perform in that role. A new job is a combination of your livelihood, a commitment to learn and grow, and contribute.
Remember to be selective in your process because you’re interviewing your next employer, too.