
Cartoon – Fee Explanation Fee



When Sen. Tom Carper was shopping for votes to block GOP health care bills, he didn’t just turn to his fellow senators. He turned to their governors.
A self-described “recovering governor,” himself, the Delaware Democrat carried out a communications blitz – calling, texting, emailing – and made contact with up to half of them. He skipped out on a Democratic campaign retreat to make a case at the National Governors Association summer meeting in Rhode Island.
His message: The legislation will hurt your states. Put your opposition in writing so the Senate can pause, work together to stabilize the insurance exchanges, and return to “regular order,” with hearings, bipartisan amendments — and input from governors, he said.
Delaware’s senators are bullish that debate over health care will turn to fixing the Affordable Care Act after the Senate early Friday morning defeated a proposal to repeal parts of the landmark law. 7/28/17 Damian Giletto/The News Journal
“He came up and spent a morning discussing the ins and outs, the details of health care changes,” Colorado Gov. John Hickenlooper, a Democrat, said on CBS’s “Face the Nation” Sunday.
Ohio Gov. John Kasich, a Republican, speaking on the same show, said, “Tom Carper from Delaware has been unbelievable in terms of his looking at trying to solve this problem.”
Carper believed that governors’ objections would be key to blocking the GOP effort to repeal and replace Obamacare, and it turned out they were. Even Sen. John McCain of Arizona, one of three Republicans who helped sink the GOP’s last-ditch effort, repeatedly highlighted his governor’s concerns.
Senate Minority Leader Charles Schumer of New York tapped Carper to lead outreach efforts to governors in early July when Carper complained that their voices weren’t being heard. In the health care drama, where there were many players, Democrats’ casting of Carper as the lead governors’ lobbyist made sense. He’s a former NGA chairman who loves the organization (and is prone to gushing about it).
“Tom Carper was really our point person with the governors, he kind of managed it,” said Sen. Tim Kaine, a former Democratic governor of Virginia. “He played a very important role in all of this. And the governors themselves, their voices were very important.”
Several days before the NGA summer meeting, Carper learned administration officials would discuss GOP health care proposals with the governors and was alarmed to discover that no one was scheduled to present the opposing view. He wangled an invitation to speak on a closed-door panel on July 15 alongside Seema Verma, administrator of the Centers for Medicare and Medicaid Services, and Secretary of Health and Human Services Tom Price.
“(Carper) was spreading this word that we should do this together, that people shouldn’t be hurt who are not in a position of being able to help themselves,” Kasich, an opponent of the GOP health care bills, said in an interview with USA TODAY. “And it was a message of slow down and let’s get this right. At no time did he ever say we should do nothing.After that, Carper kept contact information for every governor by his side, calling them during free moments between hearings and meetings. They discussed how the legislation would impact states’ Medicaid expansions, for example, or how a straight repeal of Obamacare would impact the states.
When he couldn’t reach Arizona Gov. Doug Ducey, a Republican, he said he talked several times to his Medicaid director and to his chief of staff. He said he spoke with Kasich “a dozen times or more.”
“One night he called me and it was like 10:30 at night,” Kasich said. “He was relentless in terms of what he did. And do I think he made a difference? I have no doubt that he did. Did he switch anybody? You don’t know. Did he have some people that would have not voted for this had McCain not voted ‘no,’ I just can’t tell you. But he deserves a lot of credit for being a really good public servant, keeping in mind the people that he serves.”
Carper said his outreach efforts helped him develop trust with governors “and just to let them know if they are interested in finding a path forward, they have a number of Democratic senators… who want to find common ground.”
Three days after Carper’s pitch at the NGA meeting, Kasich, Hickenlooper and nine other bipartisan governors who had been vocal about their concerns issued a statement opposing efforts to repeal the current system and replace it later. The statement, which Kasich said had been in the works for a while, called for governors to be included in the next steps.
“The best next step is for both parties to come together and do what we can all agree on: fix our unstable insurance markets,” they wrote.
They may be getting their wish, and so may Carper.
After the GOP’s three legislative failures, the Senate Health, Education, Labor and Pensions Committee announced it would begin hearings in September on ways to stabilize the individual health insurance market. The committee will hear from a wide range of stakeholders, including governors.
Moving forward, Carper said “the stage has been set” for better, more affordable health care coverage. Though he isn’t on the HELP Committee, he believes he can play a role in bipartisan discussions on health care.
“The key now is for the Senate to do its job,” Carper said.
https://www.axios.com/the-different-ways-your-health-care-costs-are-going-up-2471186113.html
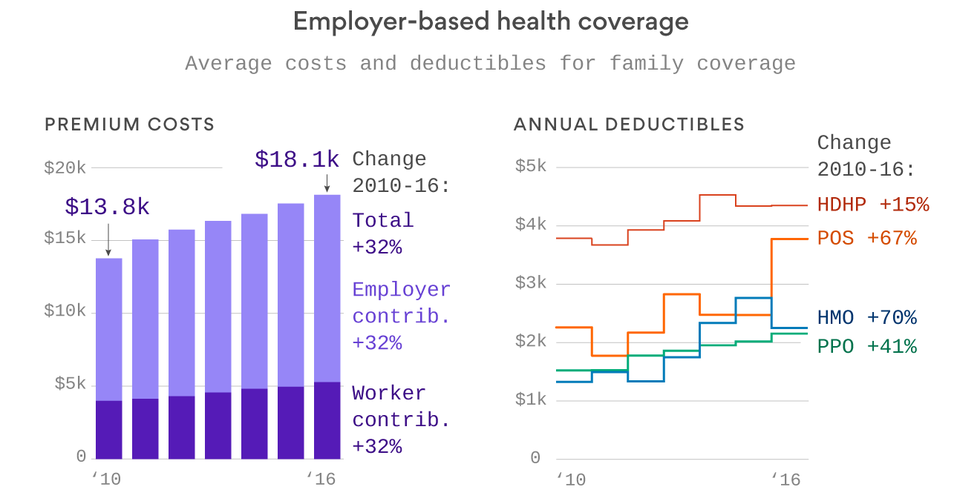
We’ve spent so much time talking about Affordable Care Act costs this year that it’s easy to forget what most people are actually paying for health care — the 156 million Americans who get their health coverage through the workplace. Turns out, most of us aren’t seeing sky-high premium increases. But it’s also worth remembering that deductibles matter too — because that’s what we pay out of pocket before insurance kicks in.
Take a look at these two graphics from Axios datavisuals genius Chris Canipe. The premium increases between 2010 and 2016 weren’t that bad — they’re single digits each year, and just add up over time. But you can see some big increases in deductibles, especially in point-of-service plans and HMOs.
Why it matters: That’s a big reason why people feel their health care costs going up, because it means they’re paying more out of pocket. And when prescription drug prices rise, they’re more likely to feel it directly.

Global investment firm Kohlberg Kravis Roberts & Co has announced they will buy Covenant Surgical Partners. Financial details were not disclosed.
Covenant buys and operates ambulatory surgery centers and physician practices, and touts 37 facilities located across 17 states.
The deal is expected to close in the third quarter of FY 2017.
The announcement comes just a day after another major, much-anticipated deal was unveiled. KKR’s Air Medical Group Holdings will merge with Envision Healthcare’s transportation subsidiary American Medical Response to form an entirely new medical transportation company, a transaction worth $2.4 billion, KKR said.
The combined company is expected to transport more than five million patients per year with air and ground ambulances across 46 states and the District of Columbia, KKR said in a statement.
Envision’s President of Ambulatory Services Randall Owen will step in as President and CEO of the new company, and when the deal is done, a new company name will be designated.
That deal is scheduled to close in the fourth quarter of 2017.
Envision Healthcare owns and operates 263 surgery centers and one surgical hospital in 35 states and the District of Columbia, with medical specialties ranging from gastroenterology to ophthalmology and orthopedics.
“The Envision leadership team conducted a robust process to review strategic alternatives for AMR. The agreement delivers on our commitment to continue the proud tradition of AMR and enables Envision to focus on its physician-centric strategy and ongoing services, including facility-based provider services, post-acute care and ambulatory surgery,” said Christopher A. Holden, Envision’s President and Chief Executive Officer.
A little more than a week ago, KKR also revealed their deal for their company Internet Brands to buy WebMD in a transaction valued at approximately $2.8 billion. This acquisition is also expected to close in the fourth quarter of 2017.

In what advocates say is a continued downward death spiral for their state, two more Texas rural hospitals closed for good earlier this week, bringing the total count of rural hospital closures in the Lonestar State to 18 in the last four and a half years alone, according to the Texas Organization of Rural and Community Hospitals or TORCH.
A hospital in Trinity, Texas closed on August 1, and another in Crockett, Texas on July 1. The closures leave those communities without immediate access to emergency and other hospital care services.
“This closure crisis, which has left many rural communities without emergency and other care, has clearly reached epidemic proportions and unless the Texas Legislature and Congress take immediate steps, it will only worsen,” said Dave Pearson, CEO of TORCH.
TORCH represents the 163 rural hospitals in the state of Texas. Of the 18 closures, they noted that four were temporary closures and three were replaced with free-standing ERs. Still, the organization said the care is those towns is now very limited, and 11 communities have no hospital or emergency care.
Many more are teetering on the edge of closure, Pearson said, with a third of the remaining rurals operating on “shoestring budgets” and struggling to keep their doors open. The worst part is these situations could be avoided he said, and are largely due to Medicare cuts in recent years totaling more than $50 million and Medicaid underpayments to rurals that total close to $60 million each year.
Torch Director of Government Relations Don McBeath said these closures and the resulting lack of access to emergency care has resulted in “documented deaths” because the local hospital was not there to service those patients.
Additionally, the closures have a devastating impact on both the local and state economies. Rural hospitals cover 85% of the state’s geography and serve 15% of the population. That population, kept healthy by the presence of their rural hospitals, drives the state economy, from food production to fuel. David Byrom, CEO of Coryell Hospital in Gatesville, said each Texas rural hospital employs an average 173 people and has $23 million in yearly payroll. That equals more than 22,000 jobs and expenditures of $3.7 billion a year, for a combined economic impact of more than $18 billion a year.
“The citizens of our rural communities fortunate enough to still have a rural hospital need to know this is happening around them and call their elected state and federal representatives and tell them to take action now to stem the tide of Texas’ rural hospital closures. The two closures in the last month, bringing the total to eighteen in the last four and a half years, could be the tip of the iceberg.”
Pearson said the closures have the potential to crush their local community economically and send residents moving out of town looking for jobs. Local businesses and schools will suffer as well, and the chances of bringing future economic development are hurt.
The Texas state legislature has recently instructed the state Department of Health and Human Services to look into the ongoing situation but that could move too slowly to stem more closures. “With a two-year study window, followed by who knows how much time to react to the findings, we could see dozens more of Texas’ rural hospitals vanish.”
An Early Look at 2018 Premium Changes and Insurer Participation on ACA Exchanges

Each year insurers submit filings to state regulators detailing their plans to participate on the Affordable Care Act marketplaces (also called exchanges). These filings include information on the premiums insurers plan to charge in the coming year and which areas they plan to serve. Each state or the federal government reviews premiums to ensure they are accurate and justifiable before the rate goes into effect, though regulators have varying types of authority and states make varying amounts of information public.
In this analysis, we look at preliminary premiums and insurer participation in the 20 states and the District of Columbia where publicly available rate filings include enough detail to be able to show the premium for a specific enrollee. As in previous years, we focus on the second-lowest cost silver plan in the major city in each state. This plan serves as the benchmark for premium tax credits. Enrollees must also enroll in a silver plan to obtain reduced cost sharing tied to their incomes. About 71% of marketplace enrollees are in silver plans this year.
States are still reviewing premiums and participation, so the data in this report are preliminary and could very well change. Rates and participation are not locked in until late summer or early fall (insurers must sign an annual contract by September 27 in states using Healthcare.gov).
Insurers in this market face new uncertainty in the current political environment and in some cases have factored this into their premium increases for the coming year. Specifically, insurers have been unsure whether the individual mandate (which brings down premiums by compelling healthy people to buy coverage) will be repealed by Congress or to what degree it will be enforced by the Trump Administration. Additionally, insurers in this market do not know whether the Trump Administration will continue to make payments to compensate insurers for cost-sharing reductions (CSRs), which are the subject of a lawsuit, or whether Congress will appropriate these funds. (More on these subsidies can be found here).
The vast majority of insurers included in this analysis cite uncertainty surrounding the individual mandate and/or cost sharing subsidies as a factor in their 2018 rates filings. Some insurers explicitly factor this uncertainty into their initial premium requests, while other companies say if they do not receive more clarity or if cost-sharing payments stop, they plan to either refile with higher premiums or withdraw from the market. We include a table in this analysis highlighting examples of companies that have factored this uncertainty into their initial premium increases and specified the amount by which the uncertainty is increasing rates.
A number of insurers have requested double-digit premium increases for 2018. Based on initial filings, the change in benchmark silver premiums will likely range from -5% to 49% across these 21 major cities. These rates are still being reviewed by regulators and may change.
In the past, requested premiums have been similar, if not equal to, the rates insurers ultimately charge. This year, because of the uncertainty insurers face over whether the individual mandate will be enforced or cost-sharing subsidy payments will be made, some companies have included an additional rate increase in their initial rate requests, while other companies have said they may revise their premiums late in the process. It is therefore quite possible that the requested rates in this analysis will change between now and open enrollment.
Insurers attempting to price their plans and determine which states and counties they will service next year face a great deal of uncertainty. They must soon sign contracts locking in their premiums for the entire year of 2018, yet Congress or the Administration could make significant changes in the coming months to the law – or its implementation – that could lead to significant losses if companies have not appropriately priced for these changes. Insurers vary in the assumptions they make regarding the individual mandate and cost-sharing subsidies and the degree to which they are factoring this uncertainty into their rate requests.
Because most enrollees on the exchange receive subsidies, they will generally be protected from premium increases. Ultimately, most of the burden of higher premiums on exchanges falls on taxpayers. Middle and upper-middle income people purchasing their own coverage off-exchange, however, are not protected by subsidies and will pay the full premium increase, switch to a lower level plan, or drop their coverage. Although the individual market on average has been stabilizing, the concern remains that another year of steep premium increases could cause healthy people (particularly those buying off-exchange) to drop their coverage, potentially leading to further rate hikes or insurer exits.

It’s hard to say exactly what transpired at that January meeting between then-Vice President Joe Biden and Epic CEO Judy Faulkner.
What we do know is that it triggered a visceral online reaction over the importance of interoperability and access to health data—and even some Twitter threads on the nuances of HIPAA. But that might be more telling about where the industry currently stands and the direction it’s quickly heading.
It began last week when Politico recounted the exchange between Biden and Faulkner as told by the vice president’s aide Greg Simon, who now serves as president of the Biden Cancer Initiative. The short version: Faulkner reportedly asked Biden why he wanted 1,000 pages of medical records to which Biden retorted, “None of your business.”
“It went downhill from there,” Simon said.
The story developed more on Monday, when former White House Chief Technology Officer Aneesh Chopra told CNBC the meeting was cordial and there “was a motivation and desire to work together to improve data access.” An Epic spokesperson told Health IT News that the company “supports patients’ rights to access their entire record,” adding that Biden was “consistently polite and positive” during the meeting.
By then, Twitter had worked itself into a full lather. Many were particularly incensed at Faulkner’s insinuation that that length and complexity of a medical record somehow rendered it useless to patients.
The reactions to Biden’s exchange with Faulkner may say more about the state of health IT than the interaction itself that was either contentious or cordial, depending on who you ask. There’s still a lot of frustration over the amount of money invested in EHR adoption and the fact that interoperability is still a challenging task.
At the same time, the vast majority of the industry is embracing the concept of replacing medical paternalism with patient-centered care, and more healthcare consumers are recognizing the benefits of having all of your health information at your fingertips.
In other words, demand is growing, but healthcare is still short on supply. That might explain the visceral reactions.
This week, Chilmark Research analyst Brian Eastwood argued that the debate over patient access to data revolves more around culture than software, and that’s probably true. Embracing the idea that patients should be able to access their medical record is a basic hurdle before anyone can tackle the technology that can make that happen.
But the heated debate that followed shows how much people across the healthcare industry see this as a core priority. It may not have infiltrated every corner of the ecosystem, but it touched a nerve that was far more basic than the technical minutia of interoperability or data standardization. It’s clear that the broader notion that patient records aren’t just the property of the health system—or even the software vendor—is carving out a substantial role in healthcare’s ongoing transformation. Any insinuation to the contrary is seen as shortsighted.
Clearly, it’s not ubiquitous yet, but there’s a strong undercurrent pushing the industry beyond the question of why patients might want their data and into the how. Perhaps that’s a small measure of progress. – Evan | @DB_Sweeney, @FierceHealthIT
http://www.cnn.com/2017/08/09/politics/kfile-ron-johnson-john-mccain/index.html

Sen. Ron Johnson on Thursday walked back controversial remarks he made about Sen. John McCain earlier in the week when he suggested the Arizona Republican’s dissenting vote on health care might have been influenced by his recent brain cancer surgery.

Seven states currently are implementing the Affordable Care Act’s (ACA) Medicaid expansion to low income adults up to 138% of the federal poverty level (FPL, $16,643 per year for an individual in 2017) in ways that extend beyond the flexibility provided by the law through Section 1115 demonstration waivers. While the future of federal legislation affecting the Medicaid expansion is unclear at this time, Section 1115 Medicaid expansion waiver activity continues as states submit amendments, extensions, and new waivers. While no decisions on expansion waivers have been issued under the new Administration to date, the Administration’s March, 2017 letter to state governors signaled some potential policy changes beyond what has been approved in the past. This issue brief focuses on approved (Arizona, Arkansas, Indiana, Iowa, Michigan, Montana, and New Hampshire) and pending (Arkansas, Kentucky, and Indiana) Section 1115 waivers that implement the ACA’s Medicaid expansion. Table 1 below summarizes approved and pending provisions in Medicaid expansion waivers across these states. (See the Appendix Tables for additional detail about each state’s waiver.)
The ACA’s Medicaid expansion changes the role of Section 1115 waivers for coverage expansions, eliminating the need for a state to obtain a waiver to cover childless adults and providing significant federal funding (100% from 2014 through 2016, gradually decreasing to 95% in 2017, and 90% by 2020) for states to expand coverage. Prior to the ACA, a number of states used Section 1115 waivers to expand coverage to childless adults who then could not otherwise be covered under federal rules. Because Section 1115 waivers must be budget neutral for federal spending, according to long-standing federal policy, states could not receive additional federal funds to expand coverage to these adults and, as such, needed to redirect existing federal funds or find offsetting program savings to finance this coverage. The ACA eliminates the historic exclusion of adults without dependent children from Medicaid, enabling states to expand coverage without a waiver and with enhanced federal matching funds. As of August, 2017, 32 states including DC have adopted the expansion, with most implementing traditional expansions as set forth by the law, and seven states using Section 1115 waivers to implement in ways not otherwise permitted under federal law. In March 2017, the Trump Administration sent a letter to state governors signaling support for waiver provisions including provisions not previously approved like those related to work requirements.Introduction
As of August, 2017, seven states (Arizona, Arkansas, Indiana, Iowa, Michigan, Montana, and New Hampshire) have approved Section 1115 waivers to implement the ACA’s Medicaid expansion in ways that extend beyond the flexibility provided by the law. Some states sought waiver authority as a politically viable way to expand coverage and receive enhanced federal matching funds. Nearly all of these waivers are limited to provisions related to the Medicaid expansion; these waivers were the mechanisms by which these states first implemented their expansions. The exception is Arizona, which has a long-standing Section 1115 waiver that governs its entire Medicaid program, and which initially implemented a traditional expansion but subsequently obtained waiver authority to alter the terms of that expansion in ways not otherwise permitted under existing law.
While each expansion waiver is unique, they include some common provisions, such as implementing the Medicaid expansion through a premium assistance model; charging premiums beyond what is authorized in federal law; eliminating non-emergency medical transportation, an otherwise required benefit; and using healthy behavior incentives to reduce premiums and/or co-payments (Table 2). Indiana’s waiver includes provisions that had not been approved in other states, such as making coverage effective on the date of the first premium payment instead of the date of application; barring certain expansion adults from re-enrolling in coverage for six months if they are dis-enrolled for unpaid premiums (a three-month lock-out was later approved in Montana); and eliminating retroactive eligibility (later approved in New Hampshire and Arkansas). The retroactive eligibility waivers were conditional, requiring states to implement safeguards to protect beneficiaries from unpaid medical costs incurred just prior to Medicaid eligibility. For example, Indiana expanded its presumptive eligibility program and implemented a prior claims payment program to cover retroactive costs for the mandatory (non-expansion) parents and 19 and 20 year olds covered under its waiver. Arkansas and New Hampshire were required to ensure that eligibility determinations are timely and without gaps in coverage.
The previous Administration denied some specific provisions included in states’ Medicaid expansion waiver proposals, including premiums for beneficiaries with incomes under 100% FPL as a condition of eligibility; elimination of Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefits and beneficiaries’ free choice of family planning provider; and work requirements as a condition of eligibility. The previous Administration also denied Ohio’s waiver application, noting that Ohio had implemented a successful traditional ACA expansion and estimated that its proposed policy changes “would lead to over 125,000 people losing coverage each year” compared to the current expansion. CMS also issued policy guidance, consistent with its legal interpretation of the ACA, indicating that states cannot receive enhanced federal ACA expansion funding unless they cover all newly eligible adults through 138% FPL.DENIED ACA EXPANSION WAIVERS OR WAIVER PROVISIONS
Three states (Indiana, Kentucky and Arkansas) currently have Medicaid expansion waivers pending before the Centers for Medicare and Medicaid Services (CMS). Indiana proposes to extend its current Medicaid expansion waiver from 2018 through 2021, with some changes, such as a three-month coverage lock-out for beneficiaries who do not timely renew eligibility, a 1% premium surcharge for tobacco users beginning in the second year of enrollment, and outcome-based healthy behavior incentives related to tobacco cessation, substance use disorder treatment, chronic disease management, and employment. Indiana also submitted an amendment to its extension application, which includes conditioning eligibility on work for most adults, changing to a tiered premium structure instead of a flat 2% of income, and ending the premium assistance program for people with access to employer-sponsored insurance, among other changes (see Appendix Table 3). Kentucky has a waiver pending that seeks changes to its traditional expansion including: implementing sliding scale premiums, requiring premium payment before coverage is effective, locking those above 100% FPL out of coverage for six months for premium non-payment, requiring work as a condition of eligibility for most adults, locking beneficiaries out of coverage for six months for failure to timely renew eligibility, adding a high deductible health savings account, offering a healthy behavior incentive account, and waiving NEMT (see Appendix Table 5). Kentucky also submitted an amendment to its pending application, which includes changing the work requirement from a graduated requirement (beginning at 5 hours/week and increasing to a maximum 20 hours/week) to a flat 20 hour/week requirement; adding disenrollment and lock-out provisions for failing to timely report changes to income or employment, or for making false statements involving work verification; and removing a proposed expansion of presumptive eligibility sites included in the original waiver application (see Appendix Table 5). Additionally, Arkansas submitted a proposed waiver amendment that would reduce Medicaid eligibility for expansion adults from 138% to 100% FPL while continuing to receive enhanced federal matching funds, establish a work requirement, end its premium assistance program for those with access to employer-sponsored insurance, and remove the conditions on its waiver of retroactive eligibility (establishing a hospital presumptive eligibility program, offering coverage during a reasonable opportunity period for verification of immigration status, and completing an eligibility determination mitigation plan).
One other state is preparing a waiver submission to CMS. Arizona completed a state public comment period for a waiver amendment that proposes changes to coverage for all “able-bodied” Medicaid adults, not only those who newly gained coverage under the ACA’s expansion, including a work requirement as a condition of eligibility, a 5-year lifetime limit on benefits, monthly income and work verifications and eligibility renewals, and a one-year lock-out for those who knowingly fail to report a change in income or make a false statement about work compliance. Arizona previously sought similar changes, which were denied by the Obama Administration in September, 2016, but state law requires Arizona to request these components annually. Table 3 summarizes states’ pending waiver requests that have not been approved by CMS to date.
Certain requirements apply to all Section 1115 waivers, not just those that authorize Medicaid expansions. While not required by statute or regulation, CMS has a longstanding policy that waiver financing must be budget neutral for the federal government, meaning that federal costs under a waiver must not exceed what federal costs would have been for that state without the waiver. The ACA also established new rules about transparency and evaluations for all waivers. Recognizing that waivers can authorize changes that impact beneficiaries, providers, health plans, and other stakeholders in important ways, the waiver transparency rules require state and federal public comment periods before all new waiver applications and extensions of existing waivers are approved by CMS. Although the final regulations involving public notice do not require a state-level public comment period for amendments to existing/ongoing demonstrations, CMS has historically applied these regulations to amendments.1 However, recently, Indiana submitted an amendment to its pending extension application and Kentucky submitted an amendment to its pending waiver application without completing/holding a state-level public comment period before submission.2 3 In keeping with statutory requirement that Section 1115 waivers test new program approaches, the evaluation rules require states to have a publicly available, approved evaluation strategy and to submit an annual report to HHS that describes the changes occurring under the waiver and their impact on access, quality, and outcomes.OTHER WAIVER PARAMETERS
State interest in Medicaid waivers (for expansion and for traditional Medicaid populations as well) as a way to gain flexibility to adapt their programs continues under the Trump Administration. While no decisions on new or amended expansion waivers have been issued to date, the Administration’s March, 2017 letter to state governors signaled some potential policy changes beyond what has been approved in the past. In terms of the waiver approval process, the letter reaffirms support for HHS’s long-standing budget neutrality policy, acknowledges reasonable public input processes and transparency guidelines, offers an expedited process for waiver renewals, and suggests greater consistency in evaluating and incorporating waiver requests that already have been approved in another state. The future of federal legislation affecting the Medicaid expansion is unclear at this time, so Medicaid policy changes authorized through Section 1115 waivers could happen on a faster timeline than federal legislative changes to the program and thus will be a key area to watch.

With the failure of several bills in the Senate to repeal or replace the Affordable Care Act (ACA), the effort to significantly remake the 2010 health law is apparently on hold, if not dead. This is a dramatic turn of events that few anticipated when Republicans took control of the White House and Congress after 7 years of vowing to repeal the ACA.
So, now what?
For the foreseeable future, all the ACA’s benefits and requirements stand—expanded Medicaid coverage for 11 million people, low-income adults; premium tax credits for about 9 million low- or middle-income people buying their own insurance; guaranteed insurance for people with preexisting conditions, and requirement that people buy insurance or pay a penalty.
The biggest question at this point is whether the Trump administration will pivot towards trying to make the law work, after the president said he might just “let Obamacare fail” to gain negotiating leverage in the repeal and replace debate.
This is without a doubt an awkward situation for President Trump and Secretary of Health and Human Services Tom Price. They have bitterly criticized the ACA, and that was at some level understandable during the high-stakes Congressional debate. But now that the debate is over for the time being, the Trump administration is left running a government responsible for implementing the law.
What would it look like for the administration to run the ACA effectively?
Most immediately, open enrollment for the ACA’s marketplaces begins November 1, and insurers have to decide by late September whether they will participate. There are a host of actions the administration could take to make it successful.
Provide Clarity Around the Rules: There is still uncertainty as to whether the administration will enforce the individual mandate and continue to make $7 billion in cost-sharing subsidy payments to insurers—which have been in limbo because of threats from the administration to cut them off and a lawsuit brought by the House of Representatives challenging the authority to make them. This uncertainty is leading insurers to propose bigger premium increases than necessary to cover the anticipated growth in medical care expenses or, in some cases, to pull out of the market entirely. If the cost-sharing payments are stopped, the Kaiser Family Foundation (KFF) estimates that insurers would have to raise premiums by an additional 19% to offset the losses.
Maintaining Outreach and Consumer Assistance: There is enormous churn in the individual insurance market as people get or lose jobs with health benefits and see their incomes rise or fall. Millions of new people need to sign up for insurance each year just to maintain steady enrollment. Importantly, any decrease in enrollment is likely to be disproportionately among healthy people. So far, the administration has mostly taken steps to pare back outreach activities, cancelling ads at the conclusion of open enrollment for this year, and recently ending contracts for consumer assistance activities. It seems unlikely that President Trump will promote ACA enrollment on an online video show like “Between Two Ferns,” as President Obama did. However, a basic level of outreach is key to making the market function.
Encouraging Insurers to Participate: The ACA represents a market-based approach to health coverage, and insurers need to participate to make it work. The number of insurers selling in the marketplaces has dropped somewhat, as some carriers found they couldn’t compete and others were concerned that not enough healthy people were signing up to maintain a balanced risk pool. However, a recent KFF analysis suggests that insurers are doing much better financially this year in the individual market, following substantial premium increases. Still, there are currently 17 counties at risk of having no insurers participating in the marketplace for 2018 (out of a total of 3143), and that number could grow if uncertainty about cost-sharing payments and individual mandate enforcement persists. If there are no marketplace insurers in a county, there is no way for enrollees to access premium tax credits, and many would likely end up uninsured. The Trump administration has generally characterized insurer exits as a sign that the ACA is failing, rather than encouraging carriers to expand their service areas to fill in bare counties.
There are also ways the Trump administration can tweak the ACA through its executive powers, while still making a good faith effort to implement the law effectively.
In particular, the administration can give states flexibility to experiment through Medicaid waivers and ACA waivers under section 1332 of the law. These waivers have certain restrictions. For example, section 1332 waivers must be budget neutral for the federal government and provide coverage that is at least as comprehensive and affordable. And, certain provisions cannot be changed through waivers, such as guaranteed insurance for people with preexisting conditions and community rating (offering insurance at the same price regardless of a person’s health status). However, these waivers provide an opportunity to create a more state-based approach, which was a key goal for Republicans in the recent health care debate.
Congress could be pivotal, as well. Appropriation of funding for the cost-sharing payments to insurers could remove any ambiguity that they will be paid. Also, even if uncertainty about the cost-sharing payments and individual mandate is resolved, there are still pockets of the country, particularly in rural areas, where the individual insurance market is fragile. An infusion of federal funding to help cover the medical expenses of high-cost patients could lower premiums and bring stability to those markets. Sen Lamar Alexander (R, Tennessee), chair of the Senate Health, Education, Labor, and Pensions Committee, has announced plans to hold bipartisan hearings in early September with a goal to quickly pass legislation.
There are also potential political consequences to just allowing—or, in fact, pushing—the ACA to fail at this point. According to KFF polling, 59% of the public believes that the president and Republicans in Congress are now responsible for any ACA-related problems moving forward. So in much of the public’s view, particularly now that the Congressional debate has stalled, Obamacare may have become Trumpcare.