
Cartoon – Retail Healthcare


Click to access CBC_59_032719.pdf

Funded by Private Equity, the ongoing consolidation of solo and small-group physician practices into Physician Practice Management organizations reflects a maturing healthcare marketplace that is repositioning to deliver single specialty care services in retail settings.
Time is running out for solo and small group practices. To position themselves for successful consolidation transactions now and in the future, operators and buyers need to understand the fundamental market dynamics shaping valuations.

Health system operating income is deteriorating as hospital expenses continue to grow, according to a recent Navigant analysis.
In the three-year analysis of the financial disclosures for 104 prominent health systems that operate almost one-half of US hospitals, the healthcare consulting firm found that two-thirds of the organization saw operating income fall from FY 2015 to FY 2017. Twenty-two of these health systems had three-year operating income reductions of over $100 million each.
Furthermore, 27 percent of the health systems analyzes lost revenue on operations in at least one of the three years analyzed and 11 percent reported negative margins all three years.
In total, health systems facing operating earnings reductions lost $6.8 billion during the period, representing a 44 percent reduction.
Rapidly growing hospital expenses as the primary driver of declining operating margins, Navigant reported. Hospital expenses increased three percentage points faster hospital revenue from 2015 to 2017. Top-line operating revenue growth decreased from seven percent in 2015 to 5.5 percent by 2017.
Hospital revenue growth slowed during the period because demand went down for key hospital services, like surgery and inpatient admissions, Navigant explained.
Many of the revenue-generating services hospitals rely on are under the microscope. Policymakers and healthcare leaders are particularly looking to decrease the number of hospital admissions and safely shift inpatient surgeries to less expensive outpatient settings.
In exchange, Medicare and other leading payers are reimbursing hospitals for decreasing admissions or readmissions and their performance on other value-based metrics.
The shift to value-based reimbursement, however, is slow and steady, with just over one-third of healthcare payments currently linked to an alternative payment model. Hospitals and health systems are still learning to navigate the new payment landscape while keeping their revenue growing.
Value-based contracts also failed to deliver sufficient patient volume to counteract the discounts given to payers, Navigant added.
According to the firm, other factors contributing to a slowdown in hospital revenue growth included a decline in collection rates for private accounts and reductions in Medicare reimbursement updates because of the Affordable Care Act and the 2012 federal budget sequester.
“Because of reductions in Medicare updates from ACA and the sequester, hospital losses in treating Medicare patients rose from $20.1 billion in 2010 to $48.8 billion in 2016, according to American Hospital Association analyses,” the report stated. “The sharp $7.2 billion deterioration in Medicare margins that occurred from 2015 to 2016 surely contributed to the reduction in hospital operating margins in the same year of this analysis.”
While hospital revenue growth slowed, hospital expenses sharply rose as healthcare organizations invested in new technologies. Value-based reimbursement, federal requirements, and other components of the Affordable Care Act prompted hospitals to make strategic investments in EHRs, physicians, and population health management, causing expenses to increase, Navigant stated.
Key strategic investments made by hospitals and health systems included:
- Compliance with the 2009 Health Information Technology for Economic and Clinical Health (HITECH) Act, which requires certified EHR implementation in hospitals and affiliated physician practices
- Compliance with Medicare payment reform initiatives, such as accountable care organizations (ACOs) or pay-for-performance programs
- Participation in new value-based contracts with payers
- Establishment of employed physician groups or clinically integrated networks to develop the capabilities needed for compliance with performance- or value-based initiatives
“In addition to these strategic investments, other factors drove up routine patient care expenses, including a nursing shortage that increased nursing wages and agency expenses; specialty drug costs, particularly for chemotherapeutic agents; and, for some systems, recalibration of retirement fund costs,” the report stated.
The shift to value-based reimbursement and all of its accompanying policies will be the “new normal,” and hospitals should expect the low rate of revenue growth to persist, Navigant stated.
But hospitals and health systems can withstand the economic downturn by achieving strategic discipline and operational excellence, the firm advised.
“Systems must be disciplined to invest their growth capital in areas of actual reachable demand; that is, matched to the growth potential in the specific local markets the system serves,” the report stated. For example, creating a Kaiser-like closed panel capitated health offering in markets where there is no employer or health plan interest in buying such a product is a waste of scarce capital and management bandwidth.”
In line with strategic discipline, organizations will need to “prune” their owned assets portfolio by improving the utilization of their clinical capacity and growing patient throughput. Health systems can achieve this by focusing on scheduling and staffing, ensuring adherence to clinical pathways, streamlining discharges and care transitions, and adjusting physical capacity to actual demand.
The tools used to succeed in value-based contracts should also be applied to Medicare lines of business to reduce Medicare operating losses.
Additionally, vertical alignment will be key to weathering falling operating earnings, Navigant explained.
“Revenue growth is more likely to occur around the edges of the hospital’s core services — inpatient care, surgery, and imaging — rather than from those services themselves,” the report stated. “Creatively repackaging services like care management that is presently imbedded in every aspect of clinical operations, and finding retail demand for services presently bundled as part of the hospital’s traditional service offerings, represent such edge opportunities.”
Reducing patient leakage in multi-specialty groups and systems through improved referral patterns, scheduling, or care coordination will help to grow revenue and keep it within the system.
“To achieve better performance, health system management and boards must take a fresh look at their strategy considering local market realities. They need to look closely at the markets they serve, and size and target their offerings to actual market demand,” the report concluded. “They must re-examine and rationalize their portfolio of assets and demand marked improvements in efficiency and effectiveness, and measurable value creation for those who pay for care, particularly their patients. Since much of this should have been done five years ago, time is of the essence.”

Healthcare’s confluence of unknowns and erratic overtures coming out of Washington has stalled many healthcare biggest stakeholders—payer, provider, and pharma. Success in transformative, threatened markets requires companies to continually reassess strategic direction: anticipate and absorb change, generate situational-driven strategic insights, and act with deliberate speed. Healthcare leaders need to step back, ask tough questions, and manage through a new set of obstacles to capture opportunity.
For healthcare marketers it’s a time to rethink basic assumptions, challenge institutional bias, breakdown silos, and force debate around longstanding approaches to marketing. Tomorrow’s marketers will be healthcare orchestra leaders. They will help set strategic pillars, sequence strategic execution, and lead go-to-market implementation that is results-driven and measurable.
Following are six healthcare impact trends that will challenge marketers in the upcoming year.
For healthcare marketers social media is a critical tool to extend reach and enhance engagement. More than 65% of chief marketing officers say they use social media to drive business and build their digital brand. Done well it boosts awareness, generates new business leads, and builds more intimate, connected customer relationships. Purpose-driven healthcare social media comes down to a brand’s respect for the importance of content. Today’s perpetually connected consumers are impatient. Their most valued brands engage with them in an evocative, relevant dialogue. They look for social media content that is shareable, fresh, unique, and above all, worth reading. Its compelling healthcare content that attracts their interest and holds their attention around a personalized, interactive value exchange.
For healthcare marketers the challenge is bringing key stakeholders along for the ride. Moving from traditional fee-for-service to value-based payment means answering the question “what’s in it for me?” Not only for patients, but equally as important are the providers of care responsible for living within the guardrails of high-performance, consumer-centric healthcare built on new models of financing, care delivery, and patient engagement, and measured on cost and quality of clinical outcomes. Marketers must use successes to demonstrate the value in value-based care, and use any failures as lessons learned.
For healthcare marketers, innovation isn’t just a substitute for brand narrative or value proposition, it’s a means to an end. Simply stating ’we are an innovative company’ won’t cut it. The storyline has to read…we are an innovative company that delivers value to our customers, improves health outcomes and does it in a way that changes healthcare delivery. Entrepreneurs and risk-takers are making stunning advances in cancer, Alzheimer’s, population health, and wellness. And, they’re the agile innovators breaking down barriers with wearables, blockchain, artificial intelligence/AI, Internet of Things, and precision medicine. If storytelling is the new marketing, marketers will have a treasure trove of material to draw from in this era of digital health technology.
Healthcare marketers have seen sweeping changes over the last few years. Gone are days where ‘product, price, place, and promotion’ is the ultimate marketing framework. As healthcare marketers face full-blown marketplace transformation, there’s a new priority: the need for marketing to have a power seat at the c-suite business strategy table. Why? 72% of CEOs believe the next three years will be more critical to their industry than the last 50 years—and the question is how many are ready, according to KPMG. Marketing can no longer take a functional or tactical focus, it has to expand its influence and integrate with leadership’s vision-driven corporate business strategy.
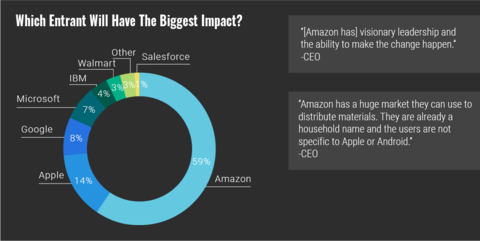
Out of all the technology giants with ambitions in healthcare, hospital executives have overwhelmingly put their faith in Amazon, according to a new survey.
A full 59% of executives say Amazon will have the biggest impact, according to the survey by Reaction Data. Respondents cited resources available to the retail and technology behemoth, the company’s current influence and name recognition.
Comparatively, 14% said Apple, with its foray into EHRs, would be the most influential, followed by Google at 8% and Microsoft at 7%
Among healthcare CEOs—which accounted for 26 of the survey’s 97 respondents—75% said Amazon would make the biggest impact.
About 80% of survey respondents were from the C-suite, including chief nursing officers, chief financial officers and chief information officers.
While Amazon alone may be generating significant excitement in boardrooms, a previous survey by HealthEdge shows consumers are largely skeptical about Amazon’s partnership with JPMorgan and Berkshire Hathaway.
Amazon’s push into healthcare “has been a shot across the bow for the entire industry,” Rita Numerof, Ph.D., president of Numerof & Associates told FierceHealthcare. The company’s consistent and deliberate investments indicate they are serious about making substantial changes within the industry.
“Amazon is known for its relentless focus on the consumer and its ability to use data systematically to identify and meet unmet needs in an accessible manner,” she said. “Unfortunately, access, consumer engagement, and segmentation haven’t been the hallmark of healthcare delivery.”
Executives were also bullish on telemedicine, with 29% saying the technology would have the biggest impact on healthcare, followed by artificial intelligence at 20%. That’s less surprising given that nearly 75% of respondents were already using telehealth in some way.However, 51% of respondents said telemedicine is revenue neutral, and key focus areas were split equally around rural patients, follow-up care and managing specific populations.
