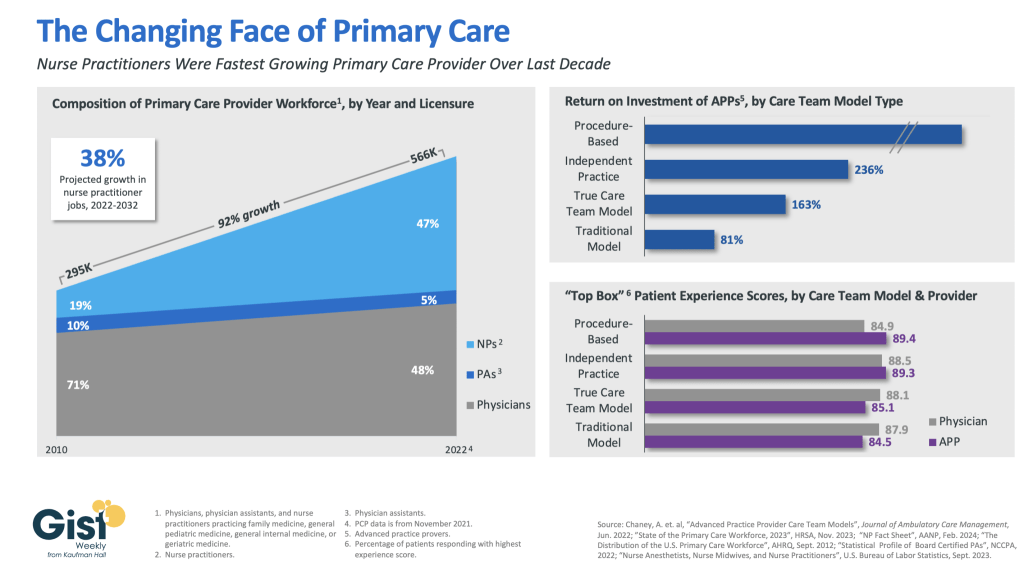
Prices for non-trauma inpatient admissions were 4.4 percent higher at trauma center hospitals than at hospitals without a trauma designation.
Hospitals designated as trauma centers charged higher prices for non-trauma inpatient admissions and emergency department visits compared to non-trauma center hospitals, a Health Affairs study found.
Hospital prices are the largest driver of rising healthcare spending in the commercial market and are often influenced by the structure of hospital markets. Trauma centers are a critical aspect of the hospital market as they are highly regulated and endowed by regulators with monopoly power over trauma patients in their service areas.
In most states, regulations are designed to encourage the entry of new trauma centers in areas that do not already have one and restrict new entry into areas that already have a trauma center. Additional regulations often require all trauma patients within an area to be transported or transferred to the designated hospital serving the area.
These restrictions create local monopolies for hospitals that are designated as trauma centers. Those in favor of the regulations argue that the monopolies are necessary to ensure each trauma center has sufficient volume to support high-quality and low-cost care. However, this structure could allow hospitals with market power over trauma services to raise prices for non-trauma services.
Researchers used claims data from 2011 to 2018 to assess whether hospitals designated as trauma centers use their market power for trauma services to receive above-market rates for non-trauma services. The sample included 2,000 hospitals with more than two million inpatient admissions and ten million emergency department visits over the study period.
The share of hospitals included in the sample serving as trauma centers increased from 21 percent in 2012 to 28 percent in 2018, resulting in a net addition of 138 trauma centers. The share of non-trauma inpatient admissions and emergency department visits at hospitals serving as trauma centers also increased between 2012 and 2018.
Hospitals serving as trauma centers every year from 2012 to 2018 were categorized as an always trauma center. Opened trauma centers were those not serving as a trauma center in 2012 but serving as one by 2018. Hospitals serving as a trauma center in 2012 but not in 2018 were closed trauma centers, and hospitals that did not serve as a trauma center at all during the study period were called “never trauma centers.”
The average price for non-trauma inpatient admissions among all hospitals was $21,112. Always trauma center hospitals had a higher average price of $22,568 per inpatient admission. The average price per admission was $22,097 at opened centers, $20,589 at closed centers, and $19,769 at never centers. Emergency department prices were similar, with always and opened center hospitals having higher prices than closed and never trauma center facilities.
Always trauma center hospitals were generally larger compared to the other hospital types and were more likely to be in more concentrated hospital markets. The average new injury severity score among emergency department visits in never trauma center hospitals was smaller compared to scores at other hospitals. The average MS-DRG weight for always trauma center hospitals was 1.61 compared to 1.54 for opened and never trauma center hospitals.
Holding these patient and hospital characteristics constant, prices for non-trauma inpatient admissions were 4.4 percent higher in hospitals with trauma center designation than at non-trauma center hospitals. Prices for non-trauma emergency department visits were 5.2 percent higher in trauma center hospitals.
“The results presented here provide an example of an important challenge: How to ensure access to specialized services and protect public health while also accounting for and possibly managing the effects of concomitant market failure,” researchers wrote.
“Our findings provide empirical support for the notion that provider market power in one area can be leveraged to affect prices in other areas.”
The No Surprises Act limits the amounts that hospitals can charge to out-of-network patients for emergency services, including trauma services. This may help limit trauma emergency cross-service leverage pricing, researchers said.