Cartoon – State of the Union on Covid Denial



Riot at U.S. Capitol prompted review of campaign contributions.
The American Hospital Association (AHA) has suspended contributions to legislators who voted against accepting the results of the Electoral College, the organization said in a statement.
The group did not provide details on exactly which legislators would now be cut off from AHA funding. As of Jan. 18, the association had not returned a request for comment from MedPage Today.
A total of 147 GOP members of Congress voted to overturn the presidential election results: 139 in the House and eight in the Senate.
In the statement, AHA called the January 6 events at the Capitol an “assault on our democracy,” and said it immediately launched a review of its donation practices to “ensure they are guided by our Association’s vision and mission, as well as the democratic values we share as a nation.”
AHA’s board of trustees decides on its political contributions after consulting with the steering committee of its Political Action Committee, along with state hospital association partners and hospital and health system leaders from lawmakers’ states and districts, the organization said.
“Hospitals and health systems have a special role to play as community leaders, healers, and caregivers for our patients and the wider communities we serve,” AHA said in the statement.
In a Jan. 7 blog post, AHA President and CEO Rick Pollack wrote that “peaceful protest is a cherished right and hallmark of our democracy, but vandalism, violence and mob rule have always been out of bounds, and need to stay that way.”
“Throughout our nation’s history, Americans have taken pride in the peaceful transfer of power at the highest level,” Pollack wrote. “It’s part of our precious heritage and distinguishes us from so many other nations of the world. But that gap seems to have narrowed this week and should concern all of us.”
Pollack and AHA called on the country to come together and begin the healing process, particularly as the nation’s COVID-19 crisis worsens.
“With so many critical issues and challenges facing our country, including putting an end to the COVID-19 pandemic and improving our health care system, we must come together now,” Pollack stated.
Over the last year, COVID-19 has taught us painful lessons about the pitfalls of wishful thinking. Early in the pandemic, some people speculated that the virus would slow down over as the weather got warmer over the summer months; instead, the U.S. experienced a deadly wave of new cases. A few months ago, I hoped that here in Southern California, it would be easier for people to avoid spreading the virus than in colder parts of the country, because people can socially distance outdoors more easily year-round. Instead, our outbreak is now among the world’s deadliest—on Monday, California became the first state to report more than 3 million cases of the virus. Here in Los Angeles County, so many people are dying that officials temporarily lifted air quality regulations to permit more cremations, the Los Angeles Times reports.
California’s struggles to contain COVID-19 can at least partly be attributed to pandemic fatigue—after nearly a year of wearing masks and avoiding contact with others, people’s resolve is simply wearing thin. However, while we may feel done with the virus, it isn’t done with us—between 70 and nearly 120 people per 100,000 have died of COVID-19 in California every day in the last week, while more than 3,200 have died each day nationwide; the U.S. just today passed the grim milestone of 400,000 COVID-19 deaths.
If California can’t get its outbreak under control, more pain could lie ahead. Officials have discovered that new variants of the virus are spreading in the Golden State, including a more transmissible strain first identified in the U.K., where caseloads are skyrocketing and hospitals are overwhelmed. What’s happening here in California could be a bellwether for the rest of the country, as the virus continues its spread mostly unchecked across the country and world.
Regardless of which variant is spreading, experts say the defensive measures remain the same: we need to keep wearing our masks (new research shows just how effective they are), maintaining physical distance from others, and spend as much time as possible at home. It’s natural to want to give up—or even bend just a little—and spend time with friends and family we haven’t seen in ages, or do other risky things. That temptation is all the more real now that multiple highly effective vaccines are here, and the end of the pandemic seems within sight. But the vaccination process has gone frustratingly slowly so far, and not enough of us have the necessary protection to let our collective guard down, especially given the presence of at least one highly transmissible mutation.
With those alarming new variants spreading across the globe, it’s probably time to recalibrate our behavior in favor of safety—until more people are inoculated, it’s vital for us to reduce spread through other proven means. In the coming weeks, Californians and Americans elsewhere must buckle down, with their eyes on the final mission: ensuring that as many people as possible survive to see the end of the pandemic.
While 28.4 million doses of the COVID-19 vaccine have been shipped to various U.S. states as of this morning, only about 10.6 million doses have been administered thus far, according to TIME’s vaccine tracker—representing 3.2% of the overall U.S. population.

India launched its nationwide coronavirus vaccine rollout on Saturday, starting with healthcare workers, according to the New York Times. Prime Minister Narendra Modi has said that the 1.3 billion-person country aims to vaccinate 300 million healthcare and other front line workers by July. More than 10.5 million people have been infected in India, and more than 152,500 people have died.
Yesterday, New York Governor Andrew Cuomo asked Pfizer whether his state could purchase vaccines directly from the pharmaceutical company, thus bypassing the federal government. But Dr. Celine Gounder, who’s advising President-elect Joe Biden on the pandemic, said that such a strategy could create problems. “I think we’ve already had too much of a patchwork response across the states,” Grounder said in an interview with CNBC today; she also argued that Cuomo’s idea could create a bidding war among states for vaccines.

More than 95.5 million people around the world had been diagnosed with COVID-19 as of 3 p.m. E.T. today, and more than 2 million people have died. On Jan. 18, there were 514,013 new cases and 9,276 new deaths confirmed globally.
Here’s how the world as a whole is currently trending:

Here’s where daily cases have risen or fallen over the last 14 days, shown in confirmed cases per 100,000 residents:

And here is every country with over 1.5 million confirmed cases:

Hua Chunying, a spokeswoman for China’s foreign ministry, is pushing back on findings from an independent World Health Organization report that was critical of Beijing’s early response to the COVID-19 outbreak. China’s early lockdowns, Chunying said, helped reduce deaths and infections, Al Jazeera reports. Still, China has been criticized for failing to adequately disclose the scope and nature of the outbreak when it first began.
German leaders have agreed to extend a lockdown for businesses and schools until Feb. 14 and to require medical masks on public transportation, Reuters reports. While Germany is now reporting fewer than half as many new cases as it was a month ago, experts have raised concerns about new coronavirus variants that are thought to be more contagious, some of which have been detected in the country.
The U.S. had recorded more than 24 million coronavirus cases as of 3 p.m. E.T. today. More than 400,000 people have died. On Jan. 18, there were 141,999 new cases and 2,422 new deaths confirmed in the U.S.
Here’s how the country as a whole is currently trending:

And here’s where daily cases have risen or fallen over the last 14 days, shown in confirmed cases per 100,000 residents.

President-elect Joe Biden plans to continue a travel ban on non-U.S. citizens from European countries and Brazil, reversing outgoing President Donald Trump’s order to end the ban on Jan. 26, six days into Biden’s presidency. Jennifer Psaki, Biden’s incoming press secretary, tweeted that the Biden administration plans “to strengthen public health measures around international travel.” A week ago, the U.S. Centers for Disease Control and Prevention ordered that almost all airline passengers must have a negative coronavirus test or proof of recovery before entering the U.S.

Neighborhoods in cities like Chicago are rapidly becoming places where people can’t fill medical prescriptions locally because their drugstores have shuttered or don’t accept Medicaid.
Why it matters: The pandemic has accelerated the growth of “pharmacy deserts” as unprofitable and less-profitable stores have closed. It’s a worrisome trend for the urban poor, who are less likely to try online pharmacies and more likely to let their drug regimens lapse when they can’t get medication locally.
Driving the news: Effective Dec. 1, Medicaid patients in Illinois — of which there are 400,000, per the Chicago Tribune — could no longer get their prescriptions filled at Walgreens, a prevalent chain headquartered in a Chicago suburb.
The backstory: Researcher Dima Qato coined the term “pharmacy desert” in a 2014 article that found there were far fewer pharmacies in Chicago’s Black neighborhoods than in white and mixed neighborhoods.
Between the lines: Because pharmacies get the lowest reimbursements for filling Medicaid prescriptions, they’re more likely to close stores in low-income neighborhoods and open them in wealthy ones, notes Antonio Ciaccia, chief strategy officer of 3 Axis Advisors, a consultancy focused on the drug supply chain.
Of note: Studies draw a direct line between pharmacy closures and people stopping their vital medications — with terrible health outcomes.
What’s next: While “food deserts,” where inner-city residents lack access to fresh and healthy groceries, are a bigger problem in places like New York City, pharmacy access is a growing concern. The number of drugstores has declined 20% in NYC since 2016, according to Jonathan Bowles, executive director of the Center for an Urban Future.
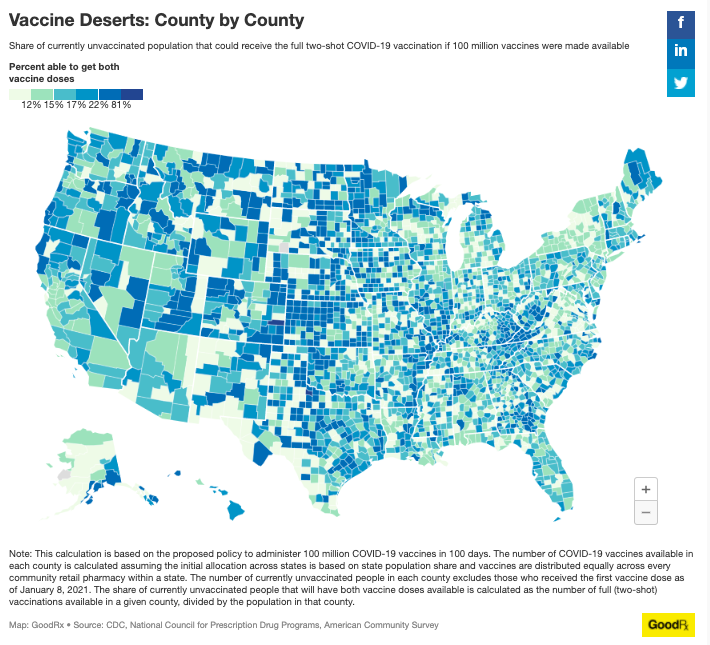
Millions of Americans who live in “pharmacy deserts” could have extra trouble accessing coronavirus vaccines quickly, according to a new analysis by GoodRx.
Why it matters: Places without nearby pharmacies, or with a large population-to-pharmacy ratio, may need to rely on mass vaccination sites or other measures to avoid falling behind.
The big picture: Pharmacies will play a huge role in the vaccine rollout, especially as shots become more available to the general population.
By the numbers: The incoming Biden administration has set a goal of vaccinating 100 million people in 100 days, or about 16% of the unvaccinated U.S. population, per GoodRx.
https://thehill.com/policy/healthcare/534765-us-passes-400000-coronavirus-deaths?rnd=1611069180

The United States on Tuesday passed 400,000 deaths from COVID-19, a stunning total that is only climbing as the crisis deepens.
The country is now averaging more than 3,000 coronavirus deaths every day, according to Johns Hopkins University data, more than the number of people killed in the Sept. 11, 2001, terror attacks, and the daily death toll has been rising. The effects of a surge in gatherings and travel over the holidays are now coming into focus.
The grim milestone of 400,000 deaths came on the last full day in office for President Trump, who has long rejected criticism of his handling of the pandemic.
The situation threatens to get even worse as a new, more contagious variant of the virus becomes more prevalent. The Centers for Disease Control and Prevention (CDC) warned last week that one of the new variants, first discovered in the United Kingdom, could be the predominant strain in the U.S. by March.
Vaccines offer hope, but it is crucial for the inoculation campaign to progress as quickly as possible to get as many people protected before the new variant takes greater hold.
The U.S. vaccination campaign has started slowly, though there are signs it is beginning to pick up some speed. President-elect Joe Biden has pledged a more aggressive federal role in the vaccination effort, including using the National Guard and the Federal Emergency Management Agency to set up more vaccination sites.
In the short term, however, the country is in for a bleak period.
Biden’s incoming CDC director, Rochelle Walensky, said Sunday on CBS’s “Face the Nation” that she expects 500,000 COVID-19 deaths by the middle of February.
“I think we still have some dark weeks ahead,” she said.
The country passed 300,000 deaths in mid-December.
At the end of March, as the crisis was beginning, Trump said that if deaths are limited to between 100,000 and 200,000 “we all, together, have done a very good job.” The country has long ago exceeded those numbers.
The U.S. has by far the most COVID-19 deaths of any country in the world. Brazil follows with around 210,000, and India and Mexico are around 150,000, according to Johns Hopkins University.
More than 124,000 people are in the hospital with coronavirus in the U.S., according to the COVID Tracking Project, though the number is starting to decline somewhat from a peak of over 130,000 about a week ago.
The spread of the more contagious variant, however, threatens to send that number spiking again.