
Joe Garagiola: “Yogi, we’re lost.”
Yogi Berra: “Yeah, I know it. But we’re making good time, ain’t we?”

Economists anticipated lackluster economic growth last quarter. Instead, growth surged, a sign of the still-resilient economy.
Why it matters:
The soft landing was very much intact this spring: Price pressures eased, but not at the expense of the strong economy and labor market.
What they’re saying:
“While these estimates will be revised a few times, they do point to the continued strength of the U.S. economy despite the high interest rate environment we’ve been in for over a year,” NerdWallet senior economist Elizabeth Renter wrote this morning.
The big picture:
The economy grew at an annualized 2.8% in the second quarter, up from the modest gain of 1.4% at the start of 2024.
Capital spending rose at a 5.2% annualized rate, reflecting a surge in spending on equipment (+11.6%) and continued investment in intellectual property (+4.5%).
Between the lines:
A narrower measure of growth affirms the economy’s resiliency in the second quarter.
The intrigue:
The second quarter saw strong growth alongside lower inflation — a reversal of dynamics observed in the January to March period, when inflation resurged and headline GDP moderated.
What to watch:
The Federal Reserve holds a policy meeting next week. No rate changes are expected, though officials look likely to lay the groundwork for a rate cut in the fall.
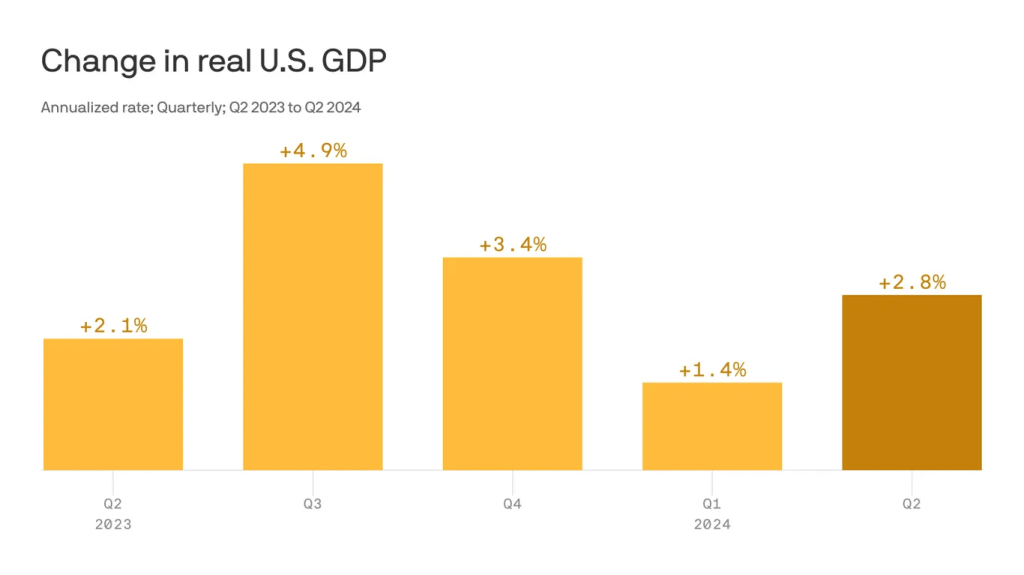
The U.S. economy grew at a 2.8% annualized rate in the second quarter—a faster rate than economists expected as consumer spending increased and businesses built up inventories, the Commerce Department said on Thursday.
Why it matters:
The new data raises confidence the economy has achieved a “soft landing” — healthy economic growth alongside cooling inflation.
Driving the news:
The accelerated growth stemmed from a jump in inventory investment and consumer spending.
The big picture:
Gloomy forecasts of a recession over the past year have not come to pass.
The bottom line:
The economy continues to defy expectations of a slowdown.
https://www.kaufmanhall.com/insights/blog/gist-weekly-july-12-2024

On Wednesday, the Centers for Medicare & Medicaid Services (CMS) issued its proposed annual changes to physician payments in its 2025 Medicare Physician Fee Schedule Proposed Rule. Required by statute to maintain budget neutrality, CMS is proposing to reduce the conversion factor—which translates the cost of providing medical services into physician payments—by 2.8%.
This is expected to lower physician payments by 2.93% on average. The proposed rule also includes new telehealth flexibilities, changes allowing eligible accountable care organizations access to a quarterly advance on their earned savings, and new payments for providers that help patients at high risk of overdose or suicide.
The Gist: With CMS proposing to reduce physician payments for the fifth straight year, the American Medical Association and other physician groups are once again calling on Congress to avert these cuts.
Congress has previously responded with “Band-Aid” solutions to temporarily reduce or eliminate reductions for the next calendar year, but physician groups are demanding a more comprehensive fix that ties Medicare payment updates to the Medicare Economic Index, a measure of practice cost inflation.
Medicare physician pay has declined 20% relative to practice costs from 2000 to 2021, and post-COVID inflation has only worsened the issue. Although lawmakers on Capitol Hill have explored various means of doing so, structural changes to Medicare budgetary policy face an uphill legislative battle in a presidential election year.
https://www.kaufmanhall.com/insights/blog/gist-weekly-july-12-2024

Using the latest data forecast from Sg2, a Vizient company, the graphic above illustrates how the outpatient shift will continue to accelerate through 2034.
Home-based care and outpatient services, including ambulatory surgery centers, are projected to be the fastest growing care sites over the next decade, with volumes increasing 22% and 14% respectively.
Sg2 forecasts that physician offices, emergency departments, and inpatient settings will experience more modest volumes increases, whereas skilled nursing facilities and retail care volumes are predicted to decline.
Additionally, although the initial outpatient procedural shift was largely focused on orthopedics, the next wave of outpatient volume growth will come from other service lines.
Driven by regulatory changes, as well as patient demand, outpatient cardiovascular volumes are expected to increase by 25% over the next decade, closely followed by neurosciences at 23%.
Continued health system investment into higher-acuity outpatient care remains crucial.

Over the weekend, President Biden called it quits and Democrats seemingly coalesced around Vice President Harris as the Party’s candidate for the White House. While speculation about her running mate swirls, the stakes for healthcare just got higher. Here’s why:
A GOP View of U.S. Healthcare
Republicans were mute on their plans for healthcare during last week’s nominating convention in Milwaukee. The RNC healthcare platform boils down to two aims: ‘protecting Medicare’ and ‘granting states oversight of abortion services. Promises to repeal and replace the Affordable Care Act, once the staple of GOP health policy, are long-gone as polls show the majority (even in Red states (like Texas and Florida) favor keeping it. The addition of Ohio Senator JD Vance to the ticket reinforces the party’s pro-capitalism, pro-competition, pro-states’ rights pitch.
To core Trump voters and right leaning Republicans, the healthcare industry is a juggernaut that’s over-regulated, wasteful and in need of discipline. Excesses in spending for illegal immigrant medical services ($8 billion in 2023), high priced drugs, lack of price transparency, increased out-of-pocket costs and insurer red tape stoke voter resentment. Healthcare, after all, is an industry that benefits from capitalism and market forces: its abuses and weaknesses should be corrected through private-sector innovation and pro-competition, pro-consumer policies.
A Dem View of Healthcare
By contrast, healthcare is more prominent in the Democrat’s platform as the party convenes for its convention in Chicago August 19. Women’s health and access to abortion, excess profitability by “corporate” drug manufacturers, hospitals and insurers, inadequate price transparency, uneven access and household affordability will be core themes in speeches and ads, with a promise to reverse the Dobb’s ruling by the Supreme Court punctuating every voter outreach.
Healthcare, to the Democratic-leaning voters is a right, not a privilege.
Its majority think it should be universally accessible, affordable, and comprehensive akin to Medicare. They believe the status quo isn’t working: the federal government should steward something better.
Here’s what we know for sure:
My take:
Regardless of the election outcome November 5, the U.S. healthcare industry will be under intense scrutiny in 2025 and beyond. It’s unavoidable.
Discontent is palpable. No sector in U.S. healthcare can afford complacency. And every stakeholder in the system faces threats that require new solutions and fresh voices.
Stay tuned.

UnitedHealth Group, the largest health insurance conglomerate by far, continues to show how rewarding it is for shareholders when corporate lawyers find loopholes in well-intentioned legislation – and game the Medicare Advantage program in ways most lawmakers and regulators didn’t anticipate and certainly didn’t intend – to boost profits.
UnitedHealth announced this morning that it made $15.8 billion in operating profits between the first of January and the end of June this year. That compares to $4.6 billion it made during the same period in 2014. One way the company is able to reward its shareholders so richly these days is by steering millions of people enrolled in its health plans to the tens of thousands of doctors it now employs and to the clinics and pharmacy operations it now owns.
This is the result of the hundreds of acquisitions UnitedHealth has made over the past 10 years in health care delivery as part of its aggressive “vertical integration” strategy.
The other big way the company has become so profitable is by rigging the Medicare Advantage program in a way that enables it to get more money from the federal government in a scheme – detailed in a big investigative report by the Wall Street Journal a few days ago – in which it claims its Medicare Advantage enrollees are sicker than they really are. The WSJ calculated that Medicare Advantage insurers bilked the government out of more than $50 billion in the three years ending in 2021 by engaging in this scheme, and it said UnitedHealth has grabbed the lion’s share of those billions. In many if not most instances, those enrollees were not treated for the conditions and illnesses UnitedHealth and other insurers claimed they had. As the newspaper reported:
Insurer-driven diagnoses by UnitedHealth for diseases that no doctor treated generated $8.7 billion in 2021 payments to the company, the Journal’s analysis showed. UnitedHealth’s net income that year was about $17 billion.
By far, most of UnitedHealth’s health plan enrollment growth over the past 10 years has come from the Medicare Advantage program, and it now takes in nearly twice as much revenue from the 7.8 million people enrolled in that program as it does from the 29.6 million enrolled in its commercial insurance plans in the United States.
Since the second quarter of 2014, UnitedHealth’s commercial health plan enrollment has increased by 720,000 people. During that same time, enrollment in its Medicare Advantage plans has increased by 4.8 million.
UnitedHealth and other insurers that participate in the Medicare Advantage program know a cash cow when they see one.
As the Kaiser Family Foundation noted in a recent report, the highest gross margins among insurers come from Medicare Advantage, which, as Health Finance News reported, boasted gross margins per enrollee of $1,982 on average by the end of 2023, compared to $1,048 in the individual (commercial) market and $753 in the Medicaid managed care market.
UnitedHealth has significant enrollment in all of those areas. Enrollment in the Medicaid plans it administers in several states increased from 4.7 million at the end of the second quarter of 2014 to 7.4 million this past quarter.
In its disclosure today, UnitedHealth did not break out its health plan revenue as it has in past quarters, but you can see how public programs like Medicare Advantage and Medicaid have become so lucrative by comparing revenue reported by the company at the end of the second quarter of 2013 to the second quarter of 2023. Over that time, total revenues for commercial plans (employer and individual) increased by slightly more than $5.6 billion, from $11.1 billion in 2Q 2013 to $16.8 billion in 2Q 2023. Total revenues from Medicaid increased by $14.2 billion, from $4.5 billion to $18.7 billion, and total revenues from Medicare increased by $21.4 billion, from $11.1 billion to $32.4 billion.
Here’s another way of looking at this: At the end of 2Q 2013, UnitedHealth took in almost exactly the same revenue from its commercial business and its Medicare business ($11.053 from Medicare and $11.134 from its commercial plans.
At the end of 2Q 2023, the company took in nearly twice as much from its Medicare business ($32.4 billion from Medicare compared to $16.8 billion from its commercial plans.)
The change is even more stark when you add in Medicaid. At the end 2Q 2023, UnitedHealth’s Medicare and Medicaid (community and state) revenues totaled $51.1 billion; It’s commercial revenues, as noted, totaled $16.8 billion). It’s now getting three times as much revenue from taxpayer-supported programs as from its commercial business.
As impressive for shareholders as all of that is, growth in the company’s other big division, Optum, which encompasses its pharmacy benefit manager (Optum Rx) and the physician practices and clinics it owns) has been even more eye-popping. At the end of 2Q 2014, Optum contributed $11.7 billion to the company’s total revenues. At the end of 2Q 2024, it contributed $62.9 billion, an increase of $51.2 billion. At that rate of growth, it’s only a matter of a few quarters before Optum is both the biggest and most profitable division of the company.
And here’s the way the company benefits from that loophole in federal law I mentioned above. The Affordable Care Act requires insurers to spend 80%-85% of health plan revenue on patient care. UnitedHealth is consistently able to meet that threshold by paying itself, as HEALTH CARE un-covered explained in December. The billions UnitedHealthcare (the health plan division) pays Optum every quarter are categorized as “eliminations” in its quarterly reports. In 2Q 2024, 27.7% of the company’s revenues fell into that category.
The more it is able to steer its health plan enrollees into businesses it owns on the Optum side, the more it can defy Congressional intent – and profit greatly by it.
Wall Street loves how UnitedHealth has pulled all this off. It’s stock price jumped $33.50 to $548.87 a share during today’s trading at the New York Stock Exchange, an increase of 6.5% – in one day.
Embattled Steward Health Care has canceled auctions for its hospitals in Ohio and Pennsylvania after it did not receive qualified bids for those facilities, according to a court filing.
The health system said in a document filed Sunday with a bankruptcy court in Texas that it is working to determine alternatives for those facilities, and expects to make an announcement at a later date. It had initially set a bid deadline for June 24 for these assets, which was later pushed back to July 15.
Steward filed for chapter 11 bankruptcy in the Southern District of Texas in May.
The system did reveal that it found potential buyers for one facility in Arkansas and another in Louisiana. Pafford Health Systems bid on the Arkansas-based Wadley Regional Medical Center for $200,000, while AHS South LLC is seeking to buy Louisiana hospital Glenwood Regional Medical Center for $500,000.
The buyers would have to take on the facilities’ liabilities, but would not be held to a rental agreement with Medical Properties Trust, Steward Health Care’s landlord.
The bid deadlines have been pushed back as high-profile potential sales have fallen through. Optum, for instance, had signed on to buy Steward’s physician group before walking away from the deal amid mounting criticism from lawmakers and others.
A hearing over these potential sales will be held on July 31, according to the court filing.
Meanwhile, the Senate Health, Education, Labor and Pensions (HELP) committee will hold a bipartisan vote on Thursday to determine whether to subpoena Steward CEO Ralph de la Torre to compel him to speak at a hearing on the health system’s struggles in September.
The HELP Committee previously invited de la Torre to testify but he declined, according to a statement from Chair Bernie Sanders, I-Vt., and Ranking Member Bill Cassidy, R-La.

UC Davis Medical Center in Sacramento, Calif., has broken ground on a $3.74 billion expansion that includes a 14-story hospital tower and a five-story medical pavilion.
The new tower will add nearly 1 million square feet of space to the existing medical center. It will include new operating rooms, an imaging center, facilities for pharmacy and burn care units, and about 334 private patient rooms.
More than 250 of the rooms are being designed for greater flexibility in the event of a patient surge such as a pandemic, wildfire or other disaster. These will easily convert into intensive-care-unit rooms with air isolation to treat patients of any level of hospitalization.
“We are building into this new tower some of the lessons we learned from the recent pandemic. As an example, three out of four of the rooms in this new tower can be easily converted to fully functional ICUs if needed, tripling our ICU capacity,” UC Davis Health CEO David Lubarsky said in a July 22 news release.
The current, 646-bed hospital will have between 675 and 700 inpatient beds when the project is completed in 2030.
“This project further harnesses the advantages of UC Davis Medical Center being Sacramento’s No. 1 hospital and delivering nationally ranked care,” Mr. Lubarsky said. “UC Davis Health is Sacramento County’s second-largest employer, and we’re making sure we are bringing not only healthcare, but jobs and community wealth-building to our surrounding neighborhoods.”