https://www.healthleadersmedia.com/finance/insurance-consolidation-may-soon-include-hospitals-create-powerhouses
Recent moves to consolidate insurance customers under one corporate structure could lead next to carriers acquiring hospital networks.
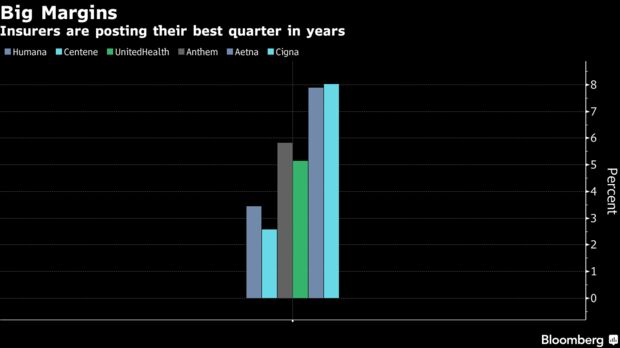
The continued market consolidation and efforts to create an “all-in-one” approach to healthcare insurance customers may lead to carriers acquiring large hospital networks, particularly if the CVS-Aetna transaction proves to be successful and profitable, one analyst says.
The mergers and acquisitions in the insurance industry over the last year is the preamble for what will happen over the next two years, says CEO of Tom Borzilleri of InteliSys Health, a company aimed at bringing greater transparency to prescription drug prices, and the former founder and CEO of a pharmacy benefit manager (PBM).
The effort will ramp up to include hospitals if health plans start seeing financial rewards from the recent moves, he says.
“We are seeing carriers acquiring PBMs, as with Cigna/Express Scripts, and pharmacy chains/PBMs acquiring carriers, like CVS/Aetna, in search of cost efficiencies to increase earnings,” he says. “One may view these mergers and acquisitions as a favorable strategy to delivering both cost savings and patient convenience, but this strategy also has the potential to produce a serious negative effect on other critical stakeholders like doctors, hospitals, clinics, and others.”
In the past, many carriers managed their pharmacy benefits internally and found that it would be more cost-efficient to outsource that function to third-party PBMs, Borzilleri notes.
“As the PBM industry grew significantly over the last decade, allowing PBMs to gain market share and buying power for the millions of lives they managed, it opened the door for PBMs to methodically profiteer at the expense of both the carriers and their insured through the vague and complicated contracts for services the carriers were forced to sign,” he says.
Borzilleri continues, “In essence, the carriers really didn’t know what they were paying for at the end of the day for these services. As the market began to change with the onset of a movement and demand within the industry for more price transparency, carriers began to realize that they would be better served to bring the PBM function back in-house to reduce costs and increase earnings.”
CREATING A CLOSED LOOP
Borzilleri explains that a merger like the CVS-Aetna acquisition provides the insurer the ability to:
- Control drug costs by eliminating the profits that the PBM formerly enjoyed
- Realize cost efficiencies to dispense medications at the pharmacy level
- Directly employ the providers that can treat their members at a cost much lower than the reimbursement rates they currently pay their network doctors
- Create a brand-new revenue stream from the retail products sold in these stores
That brings a ton of reward to CVS-Aetna, but not to anyone else, Borzilleri says.
“This type of closed-loop network will limit patient options to everything from who will be treating them, where they will be treated, and how much they will be forced to pay for services and their prescriptions,” he says.
“Based on the millions of patient lives that both CVS-Caremark and Aetna manage, patients will be herded into their own locations to be treated by their own doctors/providers and the independent physician or practice will be significantly impacted. So in essence, both the patients and doctors who treat them will lose,” Borzilleri says.
RETURNING TO CLASSIC DESIGN
Hospital acquisition also could be driven by consumers, says Bill Shea, vice president of Cognizant, a company providing digital, consulting, and other services to healthcare providers. As consumers select health services on demand, they will create their own systems of care instead of relying on a third party to do so, he says.
“The impact of these changes likely means integrated delivery systems must focus on providing on-demand healthcare and do so on a large scale. These systems can point to the proven value of offering a vetted and curated set of cost-effective providers and coordinating care to deliver better cost and quality outcomes,” Shea says.
Health plans also may consider returning to their pre-managed care origins to purse a classic insurance model of benefit design, risk management, and underwriting, he says. Some organizations could become a one-stop shop for every insurance need.
“These diversified insurance players will have the economies of scale to better manage profit and loss across multiple lines of business and to take creative approaches to health-related insurance, such as offering personalized policies targeted to specific market segments,” Shea says.
MORE STATE, REGIONAL MOVES
Consolidation is likely to increase at the state and regional level, says Suzanne Delbanco, PhD, executive director of Catalyst for Payment Reform.
“As providers with market dominance command higher prices, insurers will need to amass greater market power to push back. This means fewer choices of insurers for employers, other healthcare purchasers and consumers,” Delbanco says.
She says, “Fewer choices means less competition and less pressure to innovate. It’s possible we’ll see more of the integrated delivery systems and accountable care organizations beginning to offer insurance products where state laws and regulations allow them to as new entrants into the market.”
Those changes will make it more and more difficult to thrive as a small insurer or a small provider, she says.
Also, while rising prices and a continuation of uneven quality will motivate employers and other healthcare purchasers to demand greater transparency into provider performance and prices, larger players may more easily resist that call, she says.
“Increasingly it will be a seller’s game, not a buyer’s,” Delbanco says. “While quality measurement, provider payment reforms, and healthcare delivery reforms increasingly move toward putting the patient at the center, this may be more lip service than reality. Even if consumers end up with more information to make smarter decisions, their options may have dwindled to ones that are largely unaffordable.”