https://www.healthcaredive.com/news/ma-debt-dampen-us-healthcare-risk-profile-report-finds/540922/

Dive Brief:
- Demand for healthcare products and services has helped to keep wind in the sales of U.S. healthcare companies, but continuing deal activity and increasing issuance of high-grade bonds to fund large strategic acquisitions and capital projects is causing credit ratings to trend south, Fitch Ratings reports.
- Regulatory changes, pricing pressures, pushes from activist investors and low interest rates will likely spark more horizontal mergers and acquisitions, as well as vertically integrated deals, according to the ratings agency.
- “We view M&A and investor appetite for high quality paper, particularly during the late stages of the economic cycle, as major contributors to the risk in investment-grade bond issuance,” Fitch says. “However, prospects of enhanced cash flow generation and greater efficiencies of scale are not fully offsetting increased leverage and this is altering the long-term credit risk profile of the sector.”
Dive Insight:
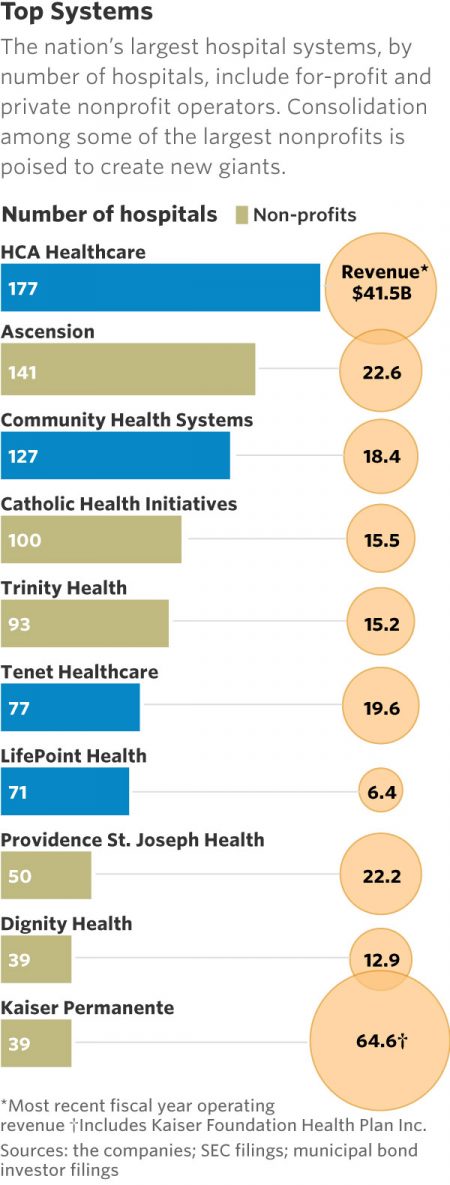
Other pressures fueling healthcare M&A include technological innovation and consumer-centricity, according to a recent PwC report. The largest deal in the third quarter of 2018 was RCCH Healthcare Partner’s $5.6 billion purchase of LifePoint Health. The quarter also saw HCA Healthcare pick up Mission Health for $1.5 billion.
Overall, though, the quarter marked the fewest number of deals since the first quarter of 2017. Value of deals also declined compared to the same period the previous year.
The slowdown in M&A includes deals among hospitals and health systems. The third period saw just 18 deals, 38% fewer than the 29 in Q3 2017, according to Kaufman Hall. The turndown suggests providers are looking at options other than mergers and acquisitions to achieve strategic aims.
Over the past 10 years, the number of investment grade bonds in healthcare has been growing at an 18% compound annual growth rate, nearly tripling in size to $609 billion by the end of September, according to Fitch. Currently, 58% of those outstanding bonds in the sector have ratings in the BBB category, compared with 1% at the end of 2009.
Roughly half of all outstanding IG bonds in healthcare are held by 10 companies, including CVS Health and Cigna. CVS took out $40 billion in loans to help fund its $67.5 billion purchase of Aetna, resulting in an A/rating watch negative. Cigna issued $20 billion worth of bonds to help cover its $67 billion acquisition of Express Scripts. Cigna’s current credit rating is BBB/RWN.
Fewer than 10% of BBB-rated companies have a BBB/negative rating. Among those are two medtech companies, Becton Dickinson and Bio-Rad Laboratories.
Fitch recently lowered Cardinal Health’s rating BBB+/negative to BBB/stable over concerns of higher than usual leverage following recent deal activity.
Moody’s Investor Services this year revised its outlook for the nonprofit and public hospitals sector from stable to negative. Moody’s warned facilities are “on an unsustainable path” due to high spending and low growth of revenues.