The White House is reportedly embracing a herd-immunity approach focused on “protecting the elderly and the vulnerable” but experts are calling the plan dangerous, “unethical”, and equivalent to “mass murder”.
The news comes following a petition titled The Great Barrington Declaration, which argued against lockdowns and school and business closures and got almost 500,000 signatures – although some of them were fake.
“Current lockdown policies are producing devastating effects on short and long-term public health,” the declaration states, adding, “The most compassionate approach that balances the risks and benefits of reaching herd immunity, is to allow those who are at minimal risk of death to live their lives normally to build up immunity to the virus through natural infection, while better protecting those who are at highest risk. We call this Focused Protection.”
Essentially, herd immunity is when enough people are immune to a disease, like Covid-19, that the disease can’t be transmitted as easily and thus provides indirect protection.
It’s been rumoured that the government has been leaning towards this plan of action for some time now, although this is the first real admission.
In response to today’s news, experts around the world have been voicing their concerns.
And this isn’t the first time we’ve heard experts say herd immunity is not a good idea.
For example, the head of the World Health Organization said Monday that allowing the novel coronavirus to spread in an attempt to reach herd immunity was “simply unethical.”
Similarly, the National Institutes of Health (NIH) director Francis Collins also denounced herd immunity as a viable plan.
“What I worry about with this is it’s being presented as if it’s a major alternative view that’s held by large numbers of experts in the scientific community. That is not true. This is a fringe component of epidemiology. This is not mainstream science. It fits into the political views of certain parts of our confused political establishment,” he said in an interview.
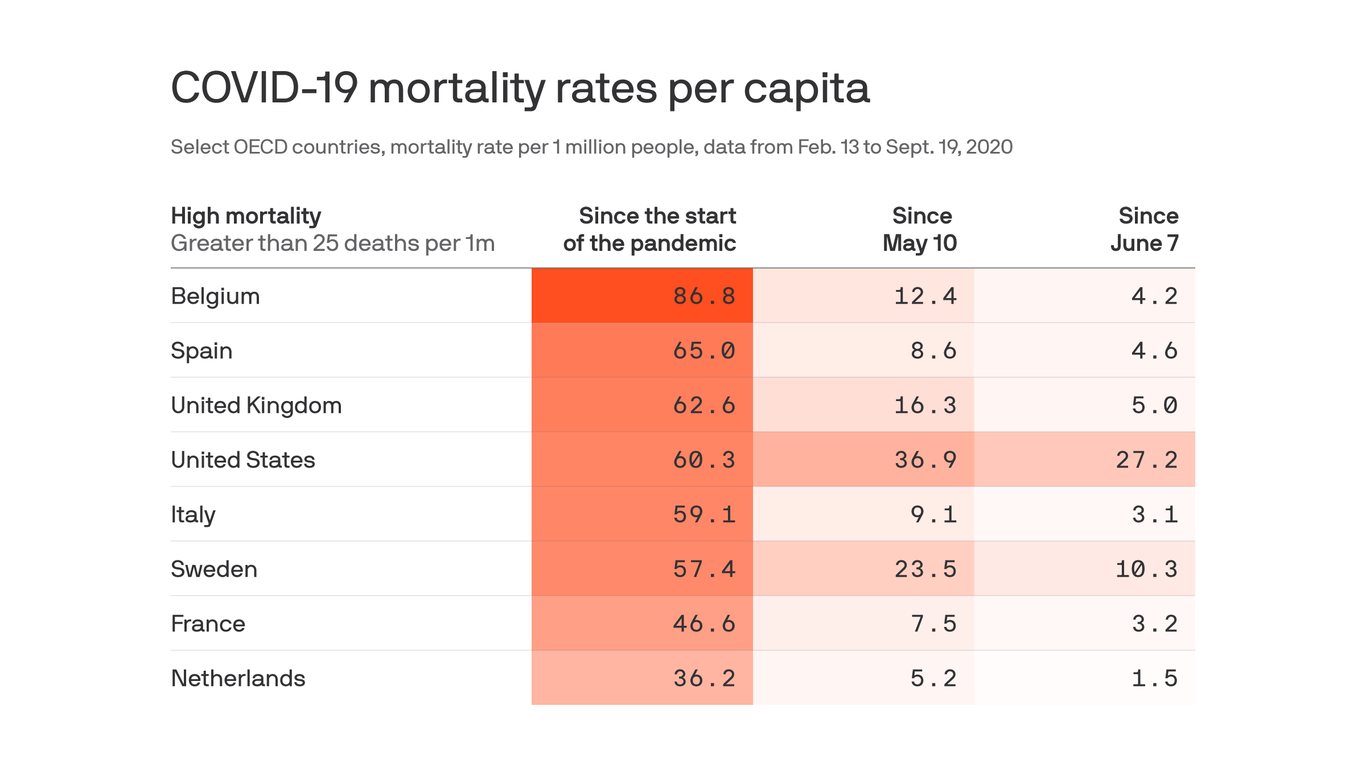
Not to mention studies continue to show that Sweden’s attempts at herd immunity have failed and have resulted in a higher Covid-19 death toll than expected.
As more research comes out, scientists are starting to learn that Covid-19 immunity, even in those who were severely infected, can fade after a few weeks.
This is why we’ve seen cases of reinfection and why many experts are advising against a herd immunity plan.
Currently less than 10% of the population in the U.S. are immune to Covid-19 but for herd immunity to be achieved most experts estimate between 40% to 80% of the population would need to be infected.
To put that into context, that means around 197 million people would need to be infected in America. And assuming that the Covid-19 fatality rate is somewhere between 0.5% and 1%, based on numbers from the World Health Organization (WHO), more than 1 million people would die – at minimum.
William Haseltine, Chair and President of ACCESS Health International, told CNN “herd immunity is another word for mass murder. We are looking at two to six million Americans dead – not just this year but every year.”
“This is an unmitigated disaster for our country – to have people at the highest levels of our government countermanding our best public health officials. We know this epidemic can be put under control. Other countries have done it. We are doing the opposite.”