
Part one of our six-part series on vaccinations, supported by the National Institute for Health Care Management Foundation, dives into the history of variolation, exploring the beginning of the long road that led to vaccines as we know them today.

Part one of our six-part series on vaccinations, supported by the National Institute for Health Care Management Foundation, dives into the history of variolation, exploring the beginning of the long road that led to vaccines as we know them today.

President Biden promised on the campaign trail to expand the Affordable Care Act to cover more of the roughly 29 million nonelderly Americans (about 11 percent of that population) who remain uninsured. He also said he’d strengthen the law by, for instance, providing an accessible and affordable public option and increasing tax credits to make it easier for people who buy insurance on their own to afford monthly premiums. Once in office, Biden immediately moved to reopen the period when people could enroll in the ACA marketplaces.
Unfortunately, the administration is paying little heed to a problem that is in many ways just as insidious as lack of insurance: underinsurance. That’s when people get too little from the insurance plans that they do have.
After passage of the ACA, the number of Americans lacking any insurance fell by 20 million, dropping to 26.7 million in 2016 — a historic low as a percentage of population. The figure began to creep up again during the Trump administration, reaching 28.9 million in 2019. That’s the problem that the current administration wants to address, and it certainly needs attention.
But according to research by the Commonwealth Fund, a foundation focused on health care, 21.3 percent of Americans have insurance so skimpy that they count as underinsured: Their out-of-pocket health-care expenses, excluding premiums, amount to at least 5 to 10 percent of household income. The limits in coverage mean their plans might provide little financial protection in a health-care crisis.
High-deductible plans offered by employers are one part of the problem. Among people covered by the companies they work for, enrollment in high-deductible health plans rose from 4 percent in 2006 to 30 percent in 2019, according to a report from the Kaiser Family Foundation. The average annual deductibles in such plans are $2,583 for an individual and $5,335 for families.
In theory, high-deductible plans, which make people spend lots of their own money before insurance kicks in, turn people into careful consumers. But research finds that people covered by such plans skip care, both unnecessary (elective cosmetic surgery, for instance) and necessary (cancer screenings and treatment, and prescriptions). Black Americans in these plans disproportionately avoid treatment, widening racial health inequities.
Health savings accounts are designed to blunt the harmful effects of high-deductible plans: Contributions by employers, and pretax contributions by individuals, help to cover costs until the deductible is reached. But not all high-deductible health plans offer such accounts, and many people in lower-wage jobs don’t have them. In the rare cases that they do, they often don’t have extra money to deposit in them.
In a November 2020 article in the journal Health Affairs, scholars affiliated with Brown University and Boston University found that enrollment in high-deductible plans had increased across all racial, ethnic and income groups from 2007 to 2018; they also found that low-income, Black and Hispanic enrollees were significantly less likely than other groups to have a health savings account — and the disparities had grown over time.
The short-term health-care plans — a.k.a. “junk” plans — that the Trump administration expanded also contribute to the problem of underinsurance. They often have low premiums but do not cover preexisting conditions or basic services like emergency health care.
Fortunately, proposals like Biden’s that make health care more accessible also tend to address the problem of underinsurance, at least in part. For example, to make individual-market insurance more affordable, Biden proposes expanding the tax credits established under the ACA. His plan calls for removing the cap on financial assistance, now set at 400 percent of the federal poverty level, in the insurance marketplaces and lowering the statutory limit on premiums to 8.5 percent of income (from nearly 10 percent).
The president also proposes to peg the size of the tax credits that subsidize premiums to the best plans on the marketplaces, the “gold” plans, rather than “silver” plans. This would increase the size of these credits, thereby making it easier for Americans to afford more-generous plans with lower deductibles.
The most ambitious Biden proposal is a public option, which would create a Medicare-like offering on marketplaces, available to anyone. Pairing this with allowing any American to opt out of their employer plan if they found a better deal on HealthCare.gov or their state marketplace — which they can’t now — would help some people escape high-deductible plans. The public option would also eliminate premiums and involve minimal to no cost-sharing for low-income enrollees — especially helpful for uninsured (and underinsured) people in states yet to expand Medicaid.
Given political realities, however, this policy may not see the light of day. So it would be best to target underinsurance directly. Most people with high-deductible plans get them through an employer. Yet unlike in the marketplace plans, the degree of cost sharing in these employer plans is the same for low-income as well as high-income employees. To deal with that problem, the government could offer incentives for employers to expand the scope of health services they cover — even in high-deductible plans. Already, many such plans exempt from the deductible some primary-care visits and generic-drug prescriptions. The list could grow to include follow-up visits and certain specialist care.
Instead of encouraging health savings accounts, the government could offer greater pretax incentives that encourage employers to absorb some of the costs that they have shifted onto their lower-income employees; that would help to prevent the insurance equity gap from widening further. The government could compensate employers that cover co-pays or other costs for their low-income employees. It could also subsidize employers that move away from high-deductible plans, at least for lower-income people.
Health insurance is complicated: More-affordable premiums are good only if they don’t bring stingy coverage. Greater investment in well-trained (and racially diverse) “navigators” — the people who help Americans enroll in plans on the federal marketplace, for example — would make it less likely that consumers would choose high-deductible plans without grasping their downsides. But it’s also important that people have options beyond risky high-deductible coverage.
The ACA expanded coverage dramatically — but the government needs to make sure that coverage amounts to more than an unused insurance card.

Part five of our six-part series on vaccinations, supported by the National Institute for Health Care Management Foundation, continues to explore the history of societal backlash against vaccination, with particular attention to vaccine-adjacent incidents and misinformation.

Part four of our six-part series on vaccinations, supported by the National Institute for Health Care Management Foundation. It turns out, people have been resistant to the idea of vaccines pretty much since vaccines were invented. This video explores the history of anti-vaccine sentiments, vaccine legislation, and societal backlash.

APR 14MORE ON REIMBURSEMENT

Susan Morse, Managing Editor

In a vote of 384-38, the House on Tuesday passed a bill that eliminates the 2% cut to Medicare payments until the end of 2021. However, the bill proposes to offset the change by increasing the sequester cuts in 2030.
WHY THIS MATTERS
The cuts were triggered by a federal budget sequestration.
Hospitals, physicians and other providers protested the 2% cuts as coming at a time when they were struggling financially and clinically to handle the COVID-19 pandemic.
The bill also makes several technical changes to the rural health clinic provisions that were included in the Consolidated Appropriations Act. Specifically, the CAA required that the payment rate for RHCs, including provider-based RHCs certified after Dec. 31, 2019, to be capped at $100 per visit, starting from April 1, 2021.
This rate will increase over time based on the Medicare Economic Index, but will remain well below typical provider-based RHC rates. The bill would correct the Dec. 31, 2019, date to Dec. 31, 2020, and include both Medicare-enrolled RHCs located in a hospital with less than 50 beds and RHCs that have submitted an application for Medicare enrollment as of this date, according to the AHA.
THE LARGER TREND
Last year, Congress paused the 2% Medicare cuts, but they were to resume on April 1.
The Centers for Medicare and Medicaid Services instructed Medicare administrative contractors to hold all claims with dates of service on or after April 1 for a short period until potential legislation was enacted.
In March, the House passed the bill to delay the cuts, and the Senate approved it later that month, but with an amendment to delay through December 31 and ensure that the cost of the delay is paid for.
PROVIDER REACTION
Providers have reacted positively to the news.
American Hospital Association president and CEO Rick Pollack said, “Even though our country is making great progress by vaccinating millions of people a day, it is clear that this pandemic is far from over and that there is an urgent need to keep hospitals, health systems and our heroic caregivers strong.”
American Medical Association president Dr. Susan R. Bailey said, “The Senate and House, Democrats and Republicans, have overwhelmingly acknowledged that cutting Medicare payments during a pandemic is ill-conceived policy. Physician practices are already distressed, and arbitrary 2% across-the-board Medicare cuts would have been devastating.”
America’s Essential Hospitals SVP of policy and advocacy Beth Feldpush said, “Extending the moratorium through the end of this year provides much-needed relief for essential hospitals, which continue to face heavy financial pressure from their frontline response to COVID-19. The sequester would weaken the ability of our hospitals to care for the communities of color that have suffered disproportionately from the pandemic.”

The Biden administration has proposed giving rehabilitation facilities a 2.2% payment increase for the 2022 federal fiscal year that starts in October.
The payment rate outlined in a proposed rule released late Thursday is slightly below the 2.4% that CMS gave rehab facilities for the 2021 federal fiscal year. CMS proposed in a separate rule a 2.3% increase for payments to inpatient psychiatric facilities as well.
Both payment rules also give updates on outlier payments, which help facilities deal with the costs of treating extremely costly beneficiaries.
For rehab facilities, CMS proposes to maintain outlier payments to 3% of the total facility payments for fiscal 2022, which begins on Oct. 1.
CMS also aims to keep the outlier payments for psychiatric facilities at 2% for 2022.
A major change for both rules is a new addition aimed to track coverage of COVID-19 vaccinations among healthcare personnel.
CMS also wants to add vaccination coverage among healthcare personnel as a measure to the quality reporting program for psychiatric facilities. The program outlines quality metrics that facilities need to meet.
“This measure would be reported using the COVID-19 modules on the [Centers for Disease Control and Prevention’s] National Healthcare Safety Network web portal,” a fact sheet on the psychiatric payment rule said.
The agency also is proposing a similar measure for rehab facilities to report any vaccinations of healthcare personnel for COVID-19.
“This proposed measure is designed to assess whether [IRFs] are taking steps to limit the spread of COVID-19 among their [healthcare personnel], reduce the risk of transmission within their facilities and help sustain the ability of [rehabilitation facilities] to continue serving their communities through the public health emergency and beyond,” a fact sheet on the rehab rule said.
In the rehab facility rule, CMS also asked for comments on how to improve health equity for all patients.
CMS is seeking comments on whether to add more measures that address patient equity in standardized patient assessment data elements, which must be collected by facilities after post-acute care.
The agency also wants comments on ways to attain health equity for psychiatric facilities as well.
“CMS is committed to addressing the significant and persistent inequities in health outcomes in the United States through improving data collection to better measure and analyze disparities across programs and policies,” the agency said in a fact sheet.
Comments for both rules are due by June 7.

President Joe Biden proposed an ambitious budget for the next federal fiscal year that includes more money for fighting the opioid epidemic, bolstering public health and several other healthcare items.
The budget request to Congress, released Friday, acts as essentially a wish list of priorities for the administration for the next year.
It is doubtful how much would get approved by Congress but sends a message of what the administration prioritizes.
Here are three healthcare priorities outlined in the request:

A new report out later today concludes that basic scientific research plays an essential role in creating companies that later produce thousands of jobs and billions in economic value.
Why it matters: The report uses the pandemic — and especially the rapid development of new mRNA vaccines — to show how basic research funding from the government lays the necessary groundwork for economically valuable companies down the road.
By the numbers: The Science Coalition — a nonprofit group that represents 50 of the nation’s top private and public research universities — identified 53 companies that have spun off from federally funded university research.
What they’re saying: “The COVID-19 pandemic has shown that the need for the federal government to continue investing in fundamental research is far from theoretical,” says John Latini, president of the Science Coalition. “Consistent, sustained, robust federal funding is how science evolves.”
Details: Latini praised the Biden administration’s first budget proposal to Congress, released last week, which includes what would be a $9 billion funding boost for the National Institutes of Health (NIH) — the country’s single biggest science research funding agency.
The catch: The Biden budget proposal is just that, and it will ultimately be up to Congress to decide how much to allocate to research agencies.
Context: Government research funding is vital because private money tends to go to applied research. But without basic research — the lifeblood of science — the U.S. risks missing out on potentially world-changing innovations in the future.
The bottom line: Because its ultimate payoff might lay years in the future, it’s easy to see basic research funding as a waste — until the day comes when we need it.

There’s widespread agreement that it’s important to help older adults and people with disabilities remain independent as long as possible. But are we prepared to do what’s necessary, as a nation, to make this possible?
That’s the challenge President Joe Biden has put forward with his bold proposal to spend $400 billion over eight years on home and community-based services, a major part of his $2 trillion infrastructure plan.
It’s a “historic and profound” opportunity to build a stronger framework of services surrounding vulnerable people who need considerable ongoing assistance, said Ai-jen Poo, director of Caring Across Generations, a national group advocating for older adults, individuals with disabilities, families and caregivers.
It comes as the coronavirus pandemic has wreaked havoc in nursing homes, assisted living facilities and group homes, killing more than 174,000 people and triggering awareness of the need for more long-term care options.
“There’s a much greater understanding now that it is not a good thing to be stuck in long-term care institutions” and that community-based care is an “essential alternative, which the vast majority of people would prefer,” said Ari Ne’eman, senior research associate at Harvard Law School’s Project on Disability.
“The systems we do have are crumbling” due to underfunding and understaffing, and “there has never been a greater opportunity for change than now,” said Katie Smith Sloan, president of LeadingAge, at a recent press conference where the president’s proposal was discussed. LeadingAge is a national association of more than 5,000 nonprofit nursing homes, assisted living centers, senior living communities and home care providers.
But prospects for the president’s proposal are uncertain. Republicans decry its cost and argue that much of what the proposed American Jobs Plan contains, including the emphasis on home-based care, doesn’t count as real infrastructure.
“Though this [proposal] is a necessary step to strengthen our long-term care system, politically it will be a challenge,” suggested Joseph Gaugler, a professor at the University of Minnesota’s School of Public Health, who studies long-term care.
Even advocates acknowledge the proposal doesn’t address the full extent of care needed by the nation’s rapidly growing older population. In particular, middle-income seniors won’t qualify directly for programs that would be expanded. They would, however, benefit from a larger, better paid, better trained workforce of aides that help people in their homes — one of the plan’s objectives.
“This [plan] isn’t everything that’s needed, not by any step of the imagination,” Poo said. “What we really want to get to is universal access to long-term care. But that will be a multistep process.”
Understanding what’s at stake is essential as communities across the country and Congress begin discussing Biden’s proposal.
The services in question. Home and community-based services help people who need significant assistance live at home as opposed to nursing homes or group homes.
Services can include home visits from nurses or occupational therapists; assistance with personal care such as eating or bathing; help from case managers; attendance at adult day centers; help with cooking, cleaning and other chores; transportation; and home repairs and modifications. It can also help pay for durable medical equipment such as wheelchairs or oxygen tanks.
The need. At some point, 70% of older adults will require help with dressing, hygiene, moving around, managing finances, taking medications, cooking, housekeeping and other daily needs, usually for two to four years. As the nation’s aging population expands to 74 million in 2030 (the year all baby boomers will have entered older age), that need will expand exponentially.
Younger adults and children with conditions such as cerebral palsy, blindness or intellectual disabilities can similarly require significant assistance.
The burden on families. Currently, 53 million family members provide most of the care that vulnerable seniors and people with disabilities require — without being paid and often at significant financial and emotional cost. According to AARP, family caregivers on average devote about 24 hours a week, to helping loved ones and spend around $7,000 out-of-pocket.
This reflects a sobering reality: Long-term care services are simply too expensive for most individuals and families. According to a survey last year by Genworth, a financial services firm, the hourly cost for a home health aide averages $24. Annually, assisted living centers charge an average $51,600, while a semiprivate room in a nursing home goes for $93,075.
Medicare limitations. Many people assume that Medicare — the nation’s health program for 61 million older adults and people with severe disabilities — will pay for long-term care, including home-based services. But Medicare coverage is extremely limited.
In the community, Medicare covers home health only for older adults and people with severe disabilities who are homebound and need skilled services from nurses and therapists. It does not pay for 24-hour care or care for personal aides or homemakers. In 2018, about 3.4 million Medicare members received home health services.
In nursing homes, Medicare pays only for rehabilitation services for a maximum of 100 days. It does not provide support for long-term stays in nursing homes or assisted living facilities.
Medicaid options. Medicaid — the federal-state health program for 72 million children and adults in low-income households — can be an alternative, but financial eligibility standards are strict and only people with meager incomes and assets qualify.
Medicaid supports two types of long-term care: home and community-based services and those provided in institutions such as nursing homes. But only care in institutions is mandated by the federal government. Home and community-based services are provided at the discretion of the states.
Although all states offer home and community-based services of some kind, there’s enormous variation in the types of services offered, who is served (states can set caps on enrollment) and state spending. Generally, people need to be frail enough to need nursing home care to qualify.
Nationally, 57% of Medicaid’s long-term care budget goes to home and community-based services — $92 billion in the 2018 federal budget year. But half of states still spend twice as much on institutional care as they do on community-based care. And 41 states have waiting lists, totaling nearly 820,000 people, with an average wait of 39 months.
Based on the best information available, between 4 million and 5 million people receive Medicaid-funded home and community-based services — a fraction of those who need care.
Workforce issues. Biden’s proposal doesn’t specify how $400 billion in additional funding would be spent, beyond stating that access to home and community-based care would be expanded and caregivers would receive “a long-overdue raise, stronger benefits, and an opportunity to organize or join a union.”
Caregivers, including nursing assistants and home health and personal care aides, earn $12 an hour, on average. Most are women of color; about one-third of those working for agencies don’t receive health insurance from their employers.
By the end of this decade, an extra 1 million workers will be needed for home-based care — a number of experts believe will be difficult, if not impossible, to reach given poor pay and working conditions.
“We have a choice to keep these poverty-wage jobs or make them good jobs that allow people to take pride in their work while taking care of their families,” said Poo of Caring Across Generations.
Next steps. Biden’s plan leaves out many details. For example: What portion of funding should go to strengthening the workforce? What portion should be devoted to eliminating waiting lists? What amount should be spent on expanding services?
How will inequities of the current system — for instance, the lack of accessible services in rural counties or for people with dementia — be addressed? “We want to see funding to states tied to addressing those inequities,” said Amber Christ, directing attorney of the health team at Justice in Aging, an advocacy organization.
Meanwhile, supporters of the plan suggest it could be just the opening of a major effort to shore up other parts of the safety net. “There are huge gaps in the system for middle-income families that need to be addressed,” said David Certner, AARP’s legislative counsel.
Reforms that should be considered include tax credits for caregivers, expanding Medicare’s home health benefit and removing the requirement that people receiving Medicare home health be homebound, said Christ of Justice in Aging.
”We should be looking more broadly at potential solutions that reach people who have some resources but not enough to pay for these services as well,” she said.
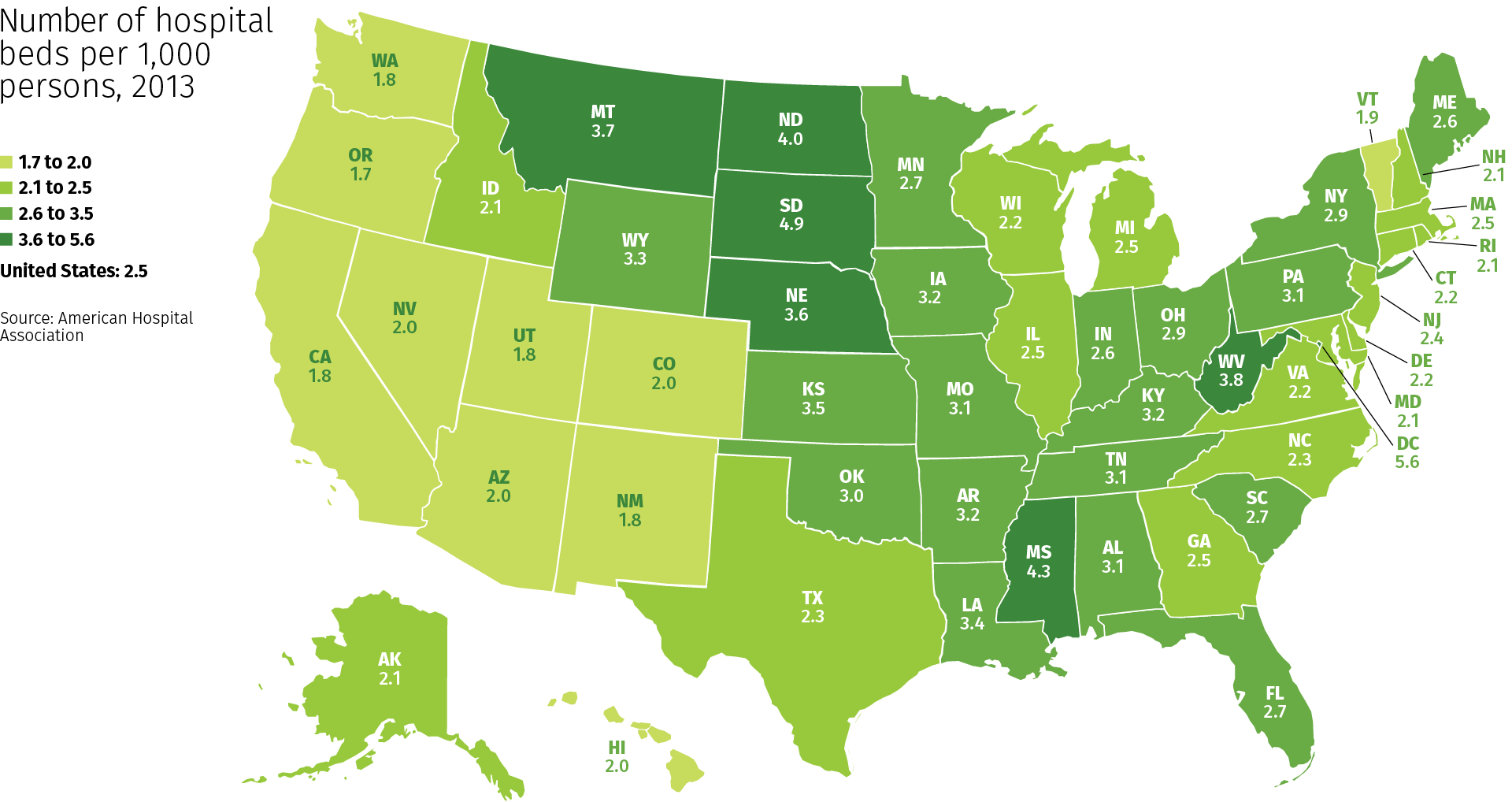
South Dakota has the highest number of hospital beds per 1,000 population in the U.S., while Oregon and Washington have the lowest, according to a ranking from the Kaiser Family Foundation.
The data is based on an analysis of the American Hospital Association’s annual survey from 2015 to 2019.
The national average per 1,000 U.S. residents was 2.4 hospital beds.
Here are the U.S. states ranked by number of staffed hospital beds per 1,000 population:
Note: The list includes ties and results in a numerical listing of 22.
1. South Dakota: 4.8 beds per 1,000 people
2. District of Columbia: 4.2
3. North Dakota: 4.4
4. Mississippi: 3.7
5. West Virginia: 3.6
6. Montana: 3.4
Wyoming: 3.4
7. Kansas: 3.3
Louisiana: 3.3
8. Kentucky: 3.2
9. Alabama: 3.1
Nebraska: 3.1
10. Arkansas: 3
Iowa: 3
Missouri: 3
11. Oklahoma: 2.9
12. Ohio: 2.8
Pennsylvania: 2.8
13. Indiana: 2.7
New York: 2.7
Tennessee: 2.7
14. Florida: 2.6
Maine: 2.6
Michigan: 2.6
15. Illinois: 2.5
Minnesota: 2.5
16. Georgia: 2.3
Massachusetts: 2.3
New Jersey: 2.3
South Carolina: 2.3
17. Alaska: 2.2
Delaware: 2.2
Texas: 2.2
18. New Hampshire: 2.1
North Carolina: 2.1
Rhode Island: 2.1
Virginia: 2.1
19. Connecticut: 2
Nevada: 2
Vermont: 2
Wisconsin: 2
20. Arizona: 1.9
California: 1.9
Colorado: 1.9
Hawaii: 1.9
Idaho: 1.9
21. Maryland: 1.8
New Mexico: 1.8
Utah: 1.8
22. Oregon: 1.7
Washington: 1.7