Category Archives: Hospital Bed Shortage
Cartoon – Sign of the Times (Hospital Bed Shortage)

Overwhelmed hospitals are sending Covid-19 patients 500+ miles away for care
As some states set Covid-19 hospitalization records, many overwhelmed hospitals are outsourcing patients on planes, helicopters, and ambulances to distant cities and states for treatment, Heather Hollingsworth and Jim Salter write for the Associated Press.
Transfers hundreds of miles away
As of last week, the number of Covid-19 patients in most hospitals remained below winter surge levels, Hollingsworth and Salter report. However, Florida, Arkansas, Oregon, Hawaii, Louisiana, and Mississippi recently set pandemic hospitalization records.
And unlike in the winter surge, many hospitals were already strained this summer due to patients catching up on previously deferred care, according to Hollingsworth and Salter.
“We are seeing Covid patients and we are seeing car accidents and we are seeing kids come in with normal seasonal viral infections. And we are seeing normal life come into the emergency department along with the extra surge of Covid patients, so it is causing that crisis,” said Mark Rosenberg, president of the American College of Emergency Physicians.
Amid the influx of patients, many of these overwhelmed hospitals are looking to neighboring cities and states for relief. For instance, in Arizona, a Covid-19 hotline is receiving calls from hospitals in Wyoming, Arkansas, Texas, and California in search of bed space, Hollingsworth and Salter report—although the hotline often cannot provide any help.
In Kansas, officials at the Wilson Medical Center in Kansas had to call 40 other facilities in several states seeking a bed for a Covid-19 patient before finally finding an available bed about 220 miles away. Across the state, according to Motient, a company contracting with Kansas to manage transfers, Covid-19 patients generally have to wait an average of 10 hours before being flown to another hospital location, which could be in Wisconsin, Illinois, Colorado, or Texas.
“That is just the worst day that you can have in the emergency room as a provider,” Richard Watson, Motient’s founder, said, “to be taking care of a patient that you are totally helpless to give them what you know they need.”
Similarly, in Washington state, the 25-bed Prosser Memorial Hospital, doesn’t have an intensive care unit, so critically ill patients are being sent as far as eastern Idaho—600 miles away.
Staffing shortages, low vaccination rates add to the problem
Finding a hospital to take in patients has become more difficult due to recent staffing shortages, according to Robin Allaman, CNO at the Kearny County Hospital in Kansas.
“Most [hospitals] are saying it isn’t that they don’t have an open bed, it is that they don’t have nursing staff to care for them,” he said. Officials at his hospital called health systems in Nebraska, Oklahoma, and New Mexico before one in Colorado Springs, Colo.—200 miles away—agreed to take a recent patient.
Watson said these delayed transfers can have dire consequences for patients, especially those who need to see specialists, who often are available only in larger hospitals. “Imagine being with your grandma in the ER who is having a heart attack in western Kansas and you are saying, ‘Why can’t we find a bed for her?’ We are watching this happen right in front of us. ‘This is America. Why don’t we have hospital bed for her?’ Well, here we are,” he said.
And while experts had hoped that the vaccines would prevent hospitals from becoming overwhelmed again, Justin Lessler, a professor of epidemiology at Johns Hopkins University, said there hasn’t been the reduction in hospitalizations that officials had hoped for. That’s in part because the delta variant seems to be more severe, particularly in younger people, whose vaccination rates are lower.
Steve Edwards—CEO of CoxHealth, whose hospital in Springfield, Mo., is treating patients from as far away as Alabama—added, “Just imagine not having the support of your family near, to have that kind of anxiety if you have someone grow acutely ill.”
Vaccination shortfall making it harder to fully staff hospitals
https://mailchi.mp/ef14a7cfd8ed/the-weekly-gist-august-6-2021?e=d1e747d2d8
With vaccine mandates on the rise among healthcare organizations, including many of the health systems we work with, we’ve begun to hear a new argument in favor of getting staff vaccinated—one that weighs against the worry that mandates will drive scarce clinical workers away.
With staffing already stretched, some systems have been concerned that implementing mandates could worsen shortages and force an increase in the use of costly agency labor. But, some executives are now telling us, so could not vaccinating staff. As the highly contagious Delta variant continues to sweep through unvaccinated populations, clinical workers who haven’t gotten their shots are especially susceptible to contracting the virus.
That’s driven a sharp increase in unvaccinated nurses and other workers calling out sick with COVID symptoms, which has made a difficult staffing situation even worse.
Some of the high-profile reports of hospitals running out of beds in the face of the Delta variant are actually driven by running out of staff to keep those beds in use—making it even more critical to ensure that frontline workers are protected against the virus.
As a growing number of hospitals and other care facilities mandate that their workers get vaccinated, we’d hope this unwelcome pressure on an already stretched workforce begins to wane.
States ranked by hospital beds per 1,000 population
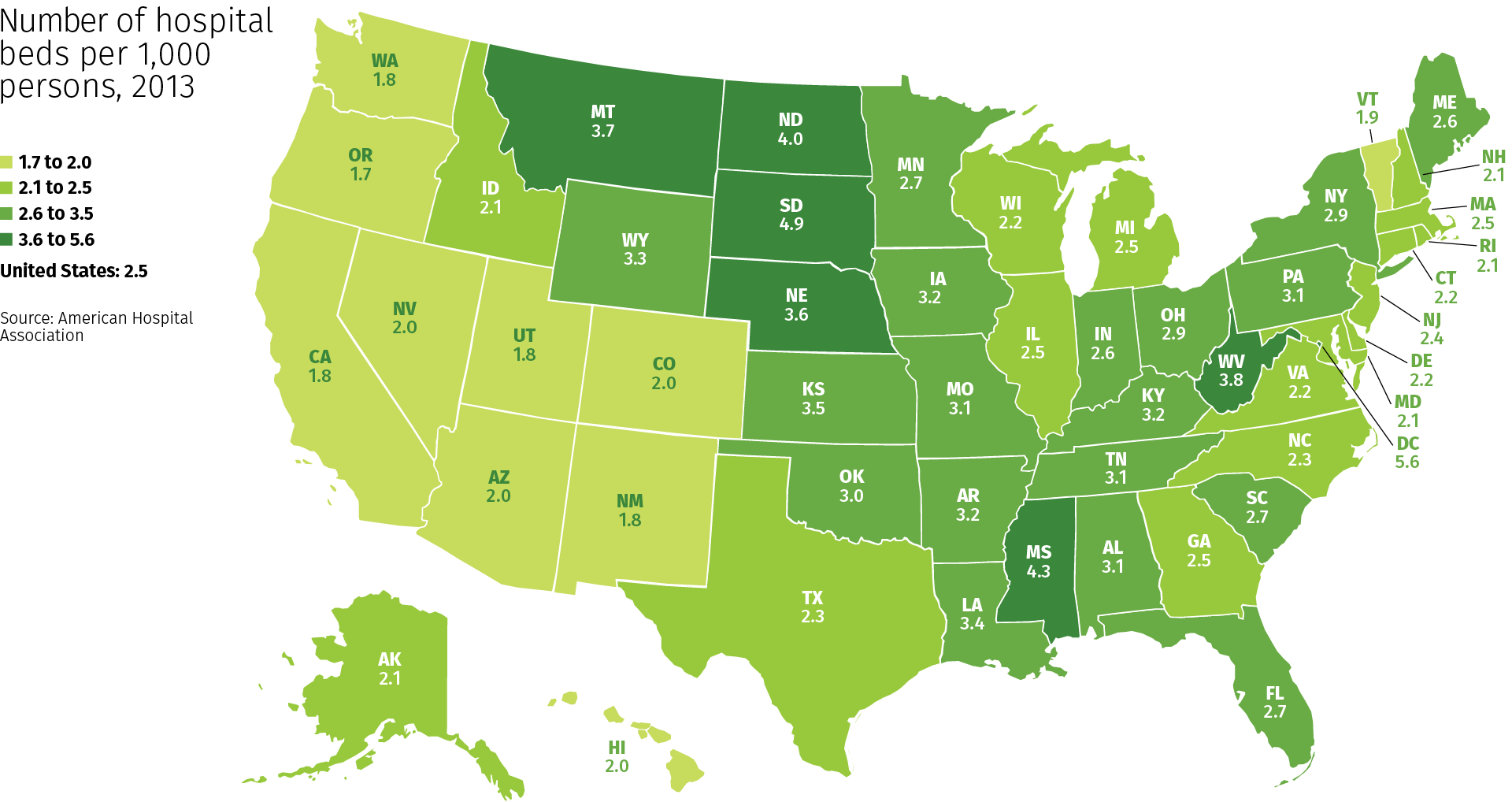
South Dakota has the highest number of hospital beds per 1,000 population in the U.S., while Oregon and Washington have the lowest, according to a ranking from the Kaiser Family Foundation.
The data is based on an analysis of the American Hospital Association’s annual survey from 2015 to 2019.
The national average per 1,000 U.S. residents was 2.4 hospital beds.
Here are the U.S. states ranked by number of staffed hospital beds per 1,000 population:
Note: The list includes ties and results in a numerical listing of 22.
1. South Dakota: 4.8 beds per 1,000 people
2. District of Columbia: 4.2
3. North Dakota: 4.4
4. Mississippi: 3.7
5. West Virginia: 3.6
6. Montana: 3.4
Wyoming: 3.4
7. Kansas: 3.3
Louisiana: 3.3
8. Kentucky: 3.2
9. Alabama: 3.1
Nebraska: 3.1
10. Arkansas: 3
Iowa: 3
Missouri: 3
11. Oklahoma: 2.9
12. Ohio: 2.8
Pennsylvania: 2.8
13. Indiana: 2.7
New York: 2.7
Tennessee: 2.7
14. Florida: 2.6
Maine: 2.6
Michigan: 2.6
15. Illinois: 2.5
Minnesota: 2.5
16. Georgia: 2.3
Massachusetts: 2.3
New Jersey: 2.3
South Carolina: 2.3
17. Alaska: 2.2
Delaware: 2.2
Texas: 2.2
18. New Hampshire: 2.1
North Carolina: 2.1
Rhode Island: 2.1
Virginia: 2.1
19. Connecticut: 2
Nevada: 2
Vermont: 2
Wisconsin: 2
20. Arizona: 1.9
California: 1.9
Colorado: 1.9
Hawaii: 1.9
Idaho: 1.9
21. Maryland: 1.8
New Mexico: 1.8
Utah: 1.8
22. Oregon: 1.7
Washington: 1.7
LA County Paramedics Told Not To Transport Some Patients With Low Chance Of Survival

Paramedics in Southern California are being told to conserve oxygen and not to bring patients to the hospital who have little chance of survival as Los Angeles County grapples with a new wave of COVID-19 patients that is expected to get worse in the coming days.
The Los Angeles County Emergency Medical Services Agency issued a directive Monday that ambulance crews should administer supplemental oxygen only to patients whose oxygen saturation levels fall below 90%.
In a separate memo from the county’s EMS Agency, paramedic crews have been told not to transfer patients who experience cardiac arrest unless spontaneous circulation can be restored on the scene.
Both measures announced Monday, which were issued by the agency’s medical director, Dr. Marianne Gausche-Hill, were taken in an attempt to get ahead of an expected surge to come following the winter holidays.
Many hospitals in the region “have reached a point of crisis and are having to make very tough decisions about patient care,” Dr. Christina Ghaly, the LA County director of health services, said at a briefing Monday.
“The volume being seen in our hospitals still represents the cases that resulted from the Thanksgiving holiday,” she said.
“We do not believe that we are yet seeing the cases that stemmed from the Christmas holiday,” Ghaly added. “This, sadly, and the cases from the recent New Year’s holiday, is still before us, and hospitals across the region are doing everything they can to prepare.”
Speaking to the CBS affiliate in Los Angeles, Gausche-Hill said personnel would continue to do everything possible to save the lives of patients, both at the scene and in the hospital.
“We are not abandoning resuscitation,” she said. “We are absolutely doing best practice resuscitation and that is do it in the field, do it right away.”
“[We] are emphasizing the fact that transporting these patients arrested leads to very poor outcomes. We knew that already and we just don’t want to impact our hospitals,” she added.
Meanwhile, the state is looking for ways to increase its supply of oxygen for use in treating COVID-19 patients, Gov. Gavin Newsom said, according to the Los Angeles Times.
“We’re just looking at the panoply of oxygen support … across the spectrum and looking how we can utilize more flexibility and broader distribution of these oxygen units all up and down the state, but particularly in these areas — San Joaquin Valley and Los Angeles, the larger Southern California region — that are in particular need and are under particular stress,” Newsom said.
Los Angeles County remains the worst-hit county in the U.S. for both confirmed COVID-19 cases and deaths from the disease. Johns Hopkins University listed more than 818,000 confirmed coronavirus cases and more than 10,700 deaths from complications from the virus in Los Angeles County by late Monday.
Last week, the new highly contagious coronavirus strain from the U.K. was discovered in Southern California. Experts have said it spreads faster than the common strain.
Banner Health halts elective surgeries
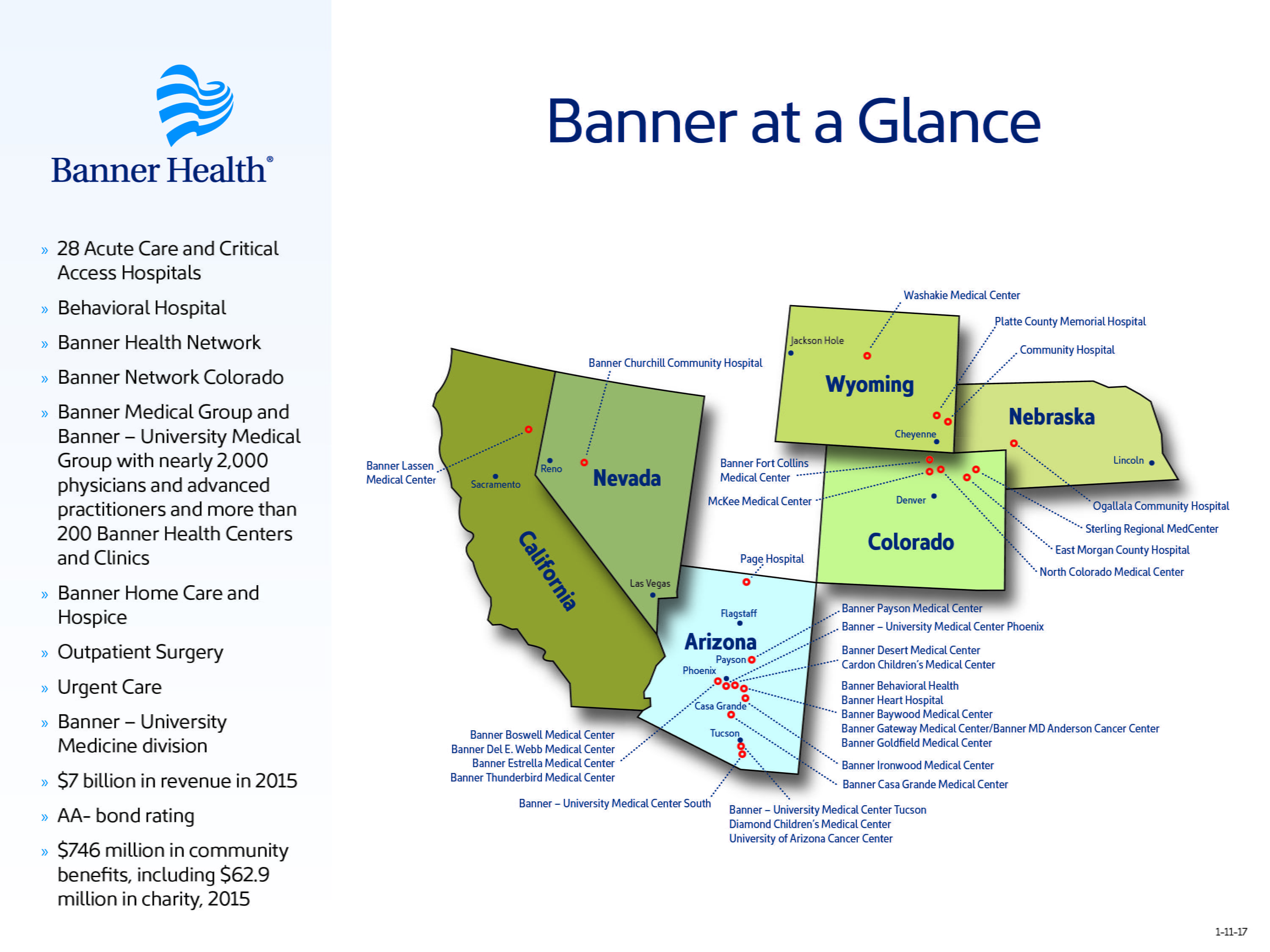
Banner Health will pause elective surgeries Jan. 1, the Phoenix-based system announced Dec. 30.
The health system is suspending nonurgent elective surgeries that can reasonably be postponed for 30 to 60 days without a negative impact on the patient’s health, according to TV station CBS 5.
Banner’s hospitals are facing a surge of COVID-19 patients. As of Dec. 29, the system was at 104 percent licensed bed capacity, Banner Chief Clinical Officer Marjorie Bessel, MD, said Dec. 30, according to TV station ABC 15. Some Banner hospitals have exceeded 120 percent licensed bed capacity.
Because of a backlog of patients, some Banner hospitals are diverting incoming ambulance transports.
“This diversion activity is an early indication that triage may soon be necessary if volumes continue to increase like they did this past week,” Dr. Bessel said, according to CBS 5. “What triage would look like, would be that we might, if we got to that point, be unable to care for everybody.”
Scripps CEO: Care rationing near if Californians ignore COVID-19 mitigation efforts

Hospitals in Southern California will need to start rationing care if more action isn’t taken by the community to mitigate the spread of COVID-19, Chris Van Gorder, president and CEO of Scripps Health, wrote in a Dec. 28 op-ed for The San Diego Union-Tribune.
As of Dec. 29, 20,642 California residents were hospitalized with COVID-19. The state’s hospital bed capacity is 72,511. In San Diego County, where Scripps is headquartered, 18 intensive care unit beds were available as of Dec. 28, “not even enough to handle a single mass casualty incident,” Mr. Van Gorder wrote. Out of Scripps’ 173 ICU beds, seven staffed beds were available as of Dec. 28.
“This past weekend, one of our community hospitals ran out of room in their morgue. We are nearing the point where we have to make the decision of who gets care and who does not,” Mr. Van Gorder wrote.
He pleaded with the San Diego and California community to adhere to mask-wearing and social distancing guidelines, especially as the New Year’s Day holiday approaches. He called on residents to stay home for New Year’s, wear a mask, wash their hands, and not eat or drink with people who aren’t in their immediate family household.
Mr. Van Gorder’s commentary comes as Kaiser Permanente hospitals in Northern California are suspending elective, non-urgent procedures through Jan. 4 as they continue to face a surge in COVID-19 hospitalizations. The Oakland, Calif.-based system announced the suspension Dec. 26, days after Chair and CEO Greg Adams said during a news conference, “We simply will not be able to keep up if the COVID surge continues to increase. We’re at or near capacity everywhere.”
Kaiser Permanente CEO: ‘We’re at or near capacity everywhere’

Hospital executives in California are sounding alarms on their inpatient capacity as COVID-19 hospitalizations surge in the state, according to ABC News.
As of Dec. 23, California is among the eight states where the virus is spreading quickest. On Dec. 22, the state saw one of its biggest jumps in one-day COVID-19 hospitalizations, with an additional 653 patients admitted to hospitals.
Officials from Oakland-based Kaiser Permanente, San Francisco-based Dignity Health and Sacramento-based Sutter Health said during a Dec. 22 news conference that they are facing capacity issues. In some cases, COVID-19 patients are being treated in hallways, gift shops and conference rooms.
Greg Adams, the chairman and CEO of Kaiser Permanente, said during the conference, “We simply will not be able to keep up if the COVID surge continues to increase. We’re at or near capacity everywhere.”
Many hospital officials said Thanksgiving gatherings contributed to the surge. The executives urged Californians to not gather for Christmas and New Year’s.
Cartoon – Healthcare System in Crisis


