https://georgetown.app.box.com/s/65qfhbzz7fabx9oypsteg6d1aghz4fsj

INTRODUCTION
Few communities in the United States have been exempt from the recent wave of consolidation among health care providers, whether it is hospital-to-hospital mergers and acquisitions (horizontal consolidation) or hospital acquisitions of physician groups and other ambulatory service providers (vertical consolidation). Increased provider concentration has been demonstrated to lead to higher provider reimbursement rates and thus higher premiums for people with private insurance, although outcomes vary, market to market.
To examine the strategies that private insurance companies and employer-purchasers use to constrain health care cost growth and how they are affected by increased provider consolidation, we conducted six market level, qualitative case studies, focusing on mid-sized health care markets in which there had been recent consolidation activity
These are: Detroit, Michigan; Syracuse, New York; Northern Virginia; Indianapolis, Indiana; Asheville, North Carolina; and Colorado Springs, Colorado.
BACKGROUND
Hospital and hospital-physician consolidation has accelerated in recent years, creating dominant local and regional health care systems. In nine out of ten metropolitan areas, the provider market is considered highly concentrated. Although merging hospitals and health systems claim they can achieve greater efficiencies and better care coordination through their consolidation, the economic literature almost universally finds that hospitals that merge charge prices above those of surrounding hospitals. Indeed, hospital mergers have been found to increase the average price of hospital services by 6 to 40 percent. Another study found that hospital acquisition of physician practices increased outpatient prices by 14 percent. At the same time, increased market concentration is strongly associated with lower quality care. There is also evidence that the prices of independent, non-acquired hospitals also increase in the wake of a rival’s acquisition.
Increases in provider prices have been a key factor driving the growth of commercial health insurance costs over the past decade. Annual family premiums have now surpassed $20,000, and the average annual deductible has increased 100 percent over the last 10 years. While policymakers have focused attention on rising health insurance premiums and out-of-pocket costs (for employers and employees alike), provider consolidation—and its role as a major health care cost driver—has received less attention in the media and among policymakers.
APPROACH
In a series of six market-level, qualitative case studies, we assessed the impact of recent provider consolidations, the resulting provider concentration, the ability of market participants (and, where relevant, regulators) to respond to those consolidations, and strategies for constraining cost growth while maintaining high-quality care. Our case studies focus on the employer-sponsored group insurance market, though we recognize that providers and insurers are often operating across multiple sources of insurance, including Medicare Advantage, Medicaid managed care, and the Affordable Care Act (ACA) marketplaces. We do not attempt to quantify the effect of provider consolidation in these markets, such as through provider rate or premium changes.
For each case study, we conducted an environmental scan of local media and published literature about market conditions and structured interviews with insurer, provider, and employer representatives, as well as other experts on the health care market. We also interviewed 10 national experts on provider consolidation and payer-provider network negotiations. Over the six case studies, we conducted 77 interviews with local respondents. Each case study, as well as an interim cross-cutting report, can be found at https://chir georgetown edu/provider-consolidation-case-studies/ .
We focused on mid-sized markets that had experienced recent horizontal or vertical consolidation. We identified these through an environmental scan of local media and research literature and a review of trends in market concentration indices, primarily via the Herfindahl-Hirschman Index (HHI). The six study markets were chosen to reflect geographic diversity as well as a range of market dynamics (see Table).
In markets such as Asheville, for instance, hospital mergers and acquisitions over the last decade have left the Mission Health System virtually without competition.
Observers describe other markets, such as Colorado Springs and Detroit, as relatively competitive even with recent provider consolidation. Across all six markets, hospitals purchased or entered into clinical affiliations with physician group practices. In some markets, such as Northern Virginia and Colorado Springs, hospital systems faced competition for physician practices from outside private equity firms and practice management companies.
In four out of our six markets, the Blue Cross Blue Shield affiliate was the dominant insurer in the commercial group market, with well over half the market share. Their dominance extended to all types of employers, including for third-party administrator contracts with self-funded employer plans. In two of our markets, the local health care system or systems were the largest private employers. In the other four, the health systems were among the top three or four employers. The states in our case studies were evenly split in having Certificate of Need laws, the lack of which some stakeholders suggested contributed to significant health system construction and concomitant increases in utilization and, less intuitively, prices (explained further, below).
FINDINGS
1. Hospitals are in various phases of empire-building
Across the six markets, the hospitals’ motivations for consolidation are similar, with stakeholders reporting a pursuit of greater market share and a desire to increase their negotiating leverage with payers to demand higher reimbursement. These observations run counter to the justifications often cited by hospital systems that consolidation is needed to create efficiencies and improve care coordination. Following consolidation, the hospitals and hospital systems in our studied markets have engaged in various phases of empire building.
While approaches varied, providers had similar goals in expanding their empire: to increase their geographic footprint, acquire points of referral (such as free-standing emergency departments and physician practices), or build new facilities in areas with a higher proportion of commercially insured residents. In all study markets except Indianapolis, a larger multi-state health system acquired or merged with a local independent provider to gain new entry or additional market share in a particular region Hospital system expansion was also not limited only to study markets: many hospital systems were expanding their footprint across the state.
In addition to consolidation, hospitals have pursued other strategies to gain greater leverage in negotiations with payers. For example, the Syracuse hospital systems have developed clinical niches, so that they are perceived by local residents as the best facility for certain services, such as orthopedics or cancer care In Indianapolis, each of the four health systems carved out “mini-monopolies” within geographic boundaries that have historically been respected by the other systems. For many years, systems largely did not compete directly, although this de facto arrangement has broken down recently.
2. Providers are exercising their increased market clout
Consolidation appears to be having the providers’ desired effect in our study markets: hospital systems reportedly use their market clout to seek higher reimbursement from payers. For example, a payer representative in Colorado noted that when an independent hospital is acquired by one of the major health systems: “the next thing I know, I see a 100 percent increase [in prices] ”. Similarly, payers in Detroit noted a “toughened stance” from a local hospital system following a recent consolidation. They, along with payers in other markets, also noted that when independent local hospitals are acquired by large national systems, negotiations shift from the local provider to the central corporate office, where there are fewer long-standing relationships, less understanding of local needs, and often a demand to take all or none of the hospitals in the system.
Even non-dominant hospitals appear to benefit from the consolidation of their rivals. For example, a small hospital in Northern Virginia was able leverage its position as an alternative to the dominant Inova Health System, effectively telling insurers: “If you think it’s healthy to have independent health systems in this market, then give us [higher prices] ”. In other cases, hospitals appear to use their market power to build more market power. For example, Asheville’s Mission hospital reportedly used its dominance to pressure physician groups to join their accountable care organization (ACO).
At the same time, our case studies provide examples of constraints on market power. The local nature of health care delivery sometimes demands that providers “play nice” in the sandbox. In Syracuse, executives of the providers and payers have longstanding personal and professional relationships. “Everyone knows each other and we all go to the same meetings,” said one observer, who believed the tight-knit nature of the community contributed to less-than-hardball tactics in the negotiating room. In Northern Virginia, some thought Inova, based just outside of D C , had been relatively restrained in its demands for increased reimbursement in part to avoid raising red flags with federal regulators.
3. Payers have tools to constrain cost growth, but lack the incentive and ability to deploy them effectively
As third-party administrators for self-insured employer-sponsored group health plans, insurers are typically paid a percentage of the overall cost of the plan. As a result, these insurers have a perverse incentive to keep costs high and growing, limiting their motivation to pursue aggressive strategies to reduce provider prices, a phenomenon one respondent called “middleman economics.” This incentive for payers is compounded by the fact that some of the more obvious strategies to contain costs (cutting or threatening to cut a high-cost hospital from their plan networks, for example) are likely to result in negative publicity and resistance from employers and their employees. The result is a strong incentive for commercial insurers to agree to providers’ demands for price increases each year, which employers and their employees will feel more gradually over time than a provider termination. The result is that employers and employees become the proverbial “frogs in the pot of water.”
Payers identify several cost containment strategies, but all come with downsides. Payers in our study markets do negotiate to limit price increases and are pursuing some cost containment strategies, but none identified a “magic bullet” approach that would moderate price growth while minimizing negative feedback from employers and employees.
Network design
One obvious strategy for insurers in response to a provider’s demand for a price increase would be to decline to contract with that provider and terminate them from their network. However, most payers and purchasers described this as a non-viable “nuclear option.” In addition to concerns about bad publicity, unhappy employer customers, and lost competitive advantage over other payers, quite often the provider at issue is essential to an adequate network, either because it is the sole provider within a reasonable geographic distance or because of its dominance in a particular clinical specialty.
Payers in several markets also noted that, more often than not, employers “don’t have their back” during provider negotiations, taking away their ability to credibly threaten to drop the provider from the network. Many large employers were loath to limit their employees’ choice of providers. Without the ability to credibly cite demand for lower prices from employers, insurers have less leverage in their negotiations with providers.
There are exceptions to this rule, but they were quite rare in the study markets. The only exception we observed was when Blue Cross Blue Shield of North Carolina (BCBSNC) terminated Mission Health System, Asheville’s only hospital system, from its network for two months in 2018. When BCBSNC, the dominant insurer in North Carolina, did so, it reportedly faced little public backlash. Rather, the public largely took BCBSNC’s side in the dispute Mission was forced to rejoin the network without the hoped-for price increases.
Designing “narrow” network product is another option for payers. By offering to drive more patient volume to a limited set of providers, payers can, in theory, extract greater price concessions. But payers across our study markets have found little interest among employer customers in narrow network products. As with the “nuclear option,” employers were typically not willing to restrict their employees’ choice, with several noting that the savings rarely outweigh the perceived limits on employees’ choices. At the same time, several payers are successfully marketing narrow network products in the individual market, where consumers may be more price sensitive and appear more willing to accept a constraint on their choice of providers in exchange for a lower premium.
Provider tiering and centers of excellence
A few payers in our markets offer plans that tier providers based on cost and quality, so that enrollees who choose lower cost providers will pay lower cost-sharing. However, the strategy is limited to markets in which there is sufficient competition so that lower-cost options are available. Payers and purchasers also noted that they often lacked the necessary data to effectively tier providers, and that patients lacked access to real-time pricing tools to enable them to make cost-effective choices.
In Asheville, a tiering strategy is difficult because the Mission Health System is so dominant. However, at least one large, self-funded employer in Asheville has designated out-of-state “centers of excellence” hospital systems that can offer lower prices and high quality for certain elective procedures. Even after reimbursing enrollees’ travel costs, this employer said, it is still more cost effective than receiving the care at Mission. However, there is a small set of elective procedures that can be performed at these facilities, and the bulk of enrollees’ care must be delivered locally.
Risk-sharing arrangements
Payers in Detroit and Northern Virginia suggested they were pinning at least some cost-containment hopes on risk-sharing arrangements with providers. In this they are following the Medicare program, and several hospital systems in our study markets participate in Medicare risk-sharing programs. However, most payers acknowledged that risk-sharing arrangements they have implemented to date have had only a limited impact. Current arrangements have largely involved only upside risk for providers, with the aim of having the provider take on more downside financial risk at a future date. Payers reported deploying risk-sharing arrangements with physician group practices more than hospitals, likely because they have greater leverage with physicians in most of the studied markets. For example, while hospital executives in Northern Virginia told us they had been presented with possible risk-sharing payment models, they declined to participate due to their lack of “economic incentive.”
Provider-payer partnerships
In some cases, payers have taken a “if you can’t beat ‘em, join ‘em” tactic, by entering into partnerships or joint ventures with health systems. For example, in 2012 Aetna entered into a joint venture with Inova in Northern Virginia to create Innovation Health. More recently, the self-insured General Motors plan entered into an exclusive partnership with the Henry Ford Health System in Detroit. While it is too early to say what the impact of the GM-Henry Ford partnership will have, observers in Northern Virginia largely dismissed Innovation Health’s impact on the market, noting that Aetna had obtained no discernible competitive advantage from the venture.
4. Employers’ tools to help control costs are limited
Unable (or unwilling) to push back on high and rising provider prices, employers have historically looked elsewhere to contain costs. Across our six markets, the most widespread strategy among employers to constrain their health plan costs has been to shift them to employees, largely through higher deductibles Increasing deductibles and other enrollee cost-sharing has been an attractive strategy because it can be ratcheted up slowly over time, limiting employee pushback. At the same time, several employer respondents in our study markets observed that this cost-shifting strategy may have been tapped out, noting that many of their employees can no longer afford the deductibles. One also observed that, because of high provider prices, employees often exceed their deductible after just one imaging service or ER visit, limiting its utility as a cost-containment tactic.
Employers reported investing in employee wellness programs. However, they were unable to document whether these programs generated savings. This is not surprising given that the weight of the evidence to date suggests minimal, if any, return on investment. Employers also touted on-site primary care as a promising strategy in Indianapolis, in part because they offer a subscription-based (capitated) model for the delivery of primary care services. However, not all employers have the requisite size or centralized location to offer this service.
Another strategy, direct contracting, is similarly limited to employers with sufficient size and human resources capacity to bypass payers and negotiate with providers. But this trend may be catching on among some Large employers in both Detroit and Indianapolis are actively considering direct contracting, and as noted above, General Motors directly contracted with the Henry Ford system in 2018. In 2019, the Peak Health Alliance, a coalition of employers and citizens of Summit County, Colorado, successfully negotiated price discounts from local providers, lowering 2020 premiums an estimated 11 percent. It remains to be seen whether such efforts are replicable outside of Summit County and if employers will, over the long term, be able to strike better bargains than private payers.
Employers also differ dramatically in their level of engagement and willingness to push insurers to deliver lower prices. One significant impediment is the lack of access to claims data, which would enable them to identify and address cost drivers. Indeed, in Indiana, a coalition of large, self-funded employers was forced to take Anthem to court in order to obtain access to their claims data, even though they bear the financial risk of their plans. For many other employers, the expertise and knowledge needed to negotiate effectively with sophisticated provider systems are well outside their core competency; they have delegated that responsibility to their third-party administrators and will continue to do so.
5. Public policy strategies have had limited effectiveness
Across our six markets, anti-trust and other public policy strategies have been deployed to constrain the ill-effects of market concentration, but they have had limited effectiveness.
Anti-trust enforcement
Stakeholders in Northern Virginia suggested that the Federal Trade Commission’s (FTC’s) intervention in Inova’s attempted acquisition of a smaller independent hospital in Prince William County has had a dampening effect on what had been a region-wide buying spree. However, respondents suggested perhaps the FTC intervention was too little, too late, noting that it would be hard for the “super concentrated” region to become any more concentrated. Nationwide, a lack of resources, a narrow focus on horizontal consolidation within local markets, and some negative court decisions have limited the FTC’s ability to be more than a speed bump to the consolidation boom of the past 10 years.
State attorneys general (AGs) have also played a role in our markets. When the for-profit hospital chain HCA acquired Mission Health System in Asheville, the state AG demanded a 10-year commitment that HCA will not close rural hospitals or require major cuts to services. Similarly, in the wake of Optum’s acquisition of the DaVita Medical Group, which owned many of the largest primary care practices in Colorado Springs, that state’s AG imposed time-limited restrictions on Optum and its owner UnitedHealthCare to mitigate anti-trust concerns in the Colorado Springs market. Specifically, UnitedHealthCare had to lift its exclusive Medicare Advantage contract with one of the two major hospital systems for at least 3.5 years and honor DaVita’s prior agreement with Humana (the main Medicare Advantage competitor in Colorado Springs) through at least 2020.
The “Certificate of Public Advantage” or COPA, has been another tool used by states to limit anti-competitive behavior, post-merger. A COPA allows a state, rather than the FTC, to oversee antitrust issues after a consolidation among providers. In North Carolina, the state legislature granted a COPA to Mission after it merged with the competing hospital system in Asheville in 1998. However, COPAs can be subject to “regulatory capture,” where regulators become overly influenced by the industry they are meant to police At least in North Carolina, the COPA appeared to do little to limit Mission’s acquisition of other nearby hospitals or physician groups. In 2015, Mission lobbyists convinced the legislature to repeal the COPA, paving the way for its purchase by the for-profit HCA system.
Certificate of Need laws
Stakeholders offered competing views on the value of state certificate of need (CON) laws. These laws generally require the state’s review and approval of new hospital facilities. Some observers argued that lifting these laws would encourage competing hospitals to enter the market, potentially putting pressure on the dominant hospital system to lower prices However, while Indianapolis experienced a hospital building boom after it repealed its CON law, payers and purchasers alike report that the increase in capacity not only led to a spike in utilization, it also, somewhat counterintuitively, drove hospitals to hike their unit prices. With more competition, hospitals had fewer patients but the same (or higher) overhead costs, leading them to demand higher prices from commercial insurers.
Rate setting and purchasing alliances
Market and public policy failure to adequately counter rising costs has prompted policymakers in some states to consider using the power of the government to set provider payment rates or to encourage the formation of multi-purchaser alliances to demand price concessions from providers. For example, a bill promoted by the Colorado insurance department would have linked some hospital reimbursement to the amount reimbursed by Medicare, while the administrator of North Carolina’s state employee health plan has proposed setting rates via reference to the Medicare program. Although Maryland was not part of our market case study, stakeholders in Northern Virginia attributed that state’s lower hospital prices to its all-payer rate setting program.
As noted above, Colorado leaders have also encouraged the formation of locally based purchasing alliances—built on the Peak Health Alliance model—that could combine the purchasing power of multiple employers to directly negotiate with hospitals. Although a payer would be sought to administer the plan, their role in contracting with providers would be greatly diminished. The concept of employer purchasing pools is not new: past efforts, such as California’s PacAdvantage program, ultimately floundered But it is too soon to tell if these nascent efforts to harness government—or employers’—purchasing power will generate significant cost savings or the type of political support needed to initiate and sustain them.
LOOKING AHEAD
As the literature and our case studies show, consolidation leads to higher provider prices and ultimately higher premiums for consumers. Any policy discussion about improving health care affordability will need to confront the limits of the market to constrain provider monopolies and their resulting increased negotiation leverage.
Misaligned incentives among commercial payers and the “must have” status of many hospital systems mean that market-based tools to hold health care costs down have been largely ineffective or difficult to replicate. And, with 90 percent of markets in the country already highly consolidated, the prospect of greater anti-trust enforcement is “too little, too late.”
In addition to the public policies discussed above, states have implemented or are considering requiring providers to work within cost growth targets and leveraging the power of state agencies to demand price concessions from providers. For example, Delaware and Massachusetts have set targets for annual increases in health care spending, while Montana’s state employee plan recently began setting a Medicare-based “reference price” for covered hospitalizations. In California, state agencies are consolidating their pharmacy purchasing authorities to negotiate lower drug prices, pursuant to a 2019 executive order by Governor Newsom. Also, in litigation that has been closely watched because it could embolden more post-consolidation anti-trust lawsuits nationwide, the California AG and a coalition of roughly 1,500 self-funded employers reached a settlement agreement with one of that state’s largest health systems, Sutter Health, over allegations that Sutter used its market power to drive up prices.
Policymakers can also do more to activate or assist employers in demanding lower prices. The first step is to help inform employers about the true drivers of health care costs by banning clauses in payer-provider contracts that prohibit the sharing of data on reimbursement rates. Employers, particularly those that self-fund their plans, should not have to sue their third-party administrator (as they did in Indiana) to gain access to their own data. Being able to clearly see the data on hospital prices has sparked a number of Indiana employers to demand change. However, if incremental steps such as data sharing don’t ultimately reduce provider prices, it could increase the support for more dramatic steps, such as rate-setting, in response to provider consolidation. “The status quo isn’t an option anymore,” one large employer told us. Indeed, the status quo is no longer an option for most employers, and certainly not for their employees, who are bearing an ever greater burden of the cost of care.










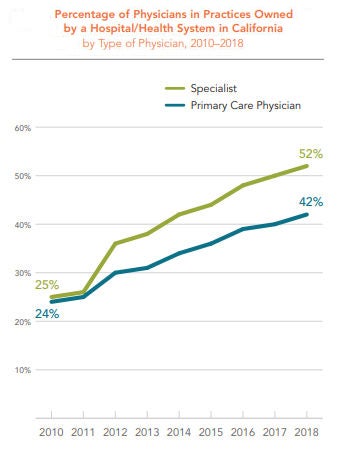
 The percentage of physicians in practices owned by a hospital or health system increased dramatically in California between 2010 and 2018 — from 24% in 2010 to 42% in 2018. The percentage of specialists in practices owned by a hospital or health system rose even faster, from 25% in 2010 to 52% in 2018.
The percentage of physicians in practices owned by a hospital or health system increased dramatically in California between 2010 and 2018 — from 24% in 2010 to 42% in 2018. The percentage of specialists in practices owned by a hospital or health system rose even faster, from 25% in 2010 to 52% in 2018.