Cartoon – Lateral Career Moves
Quote of the Day: On Culture
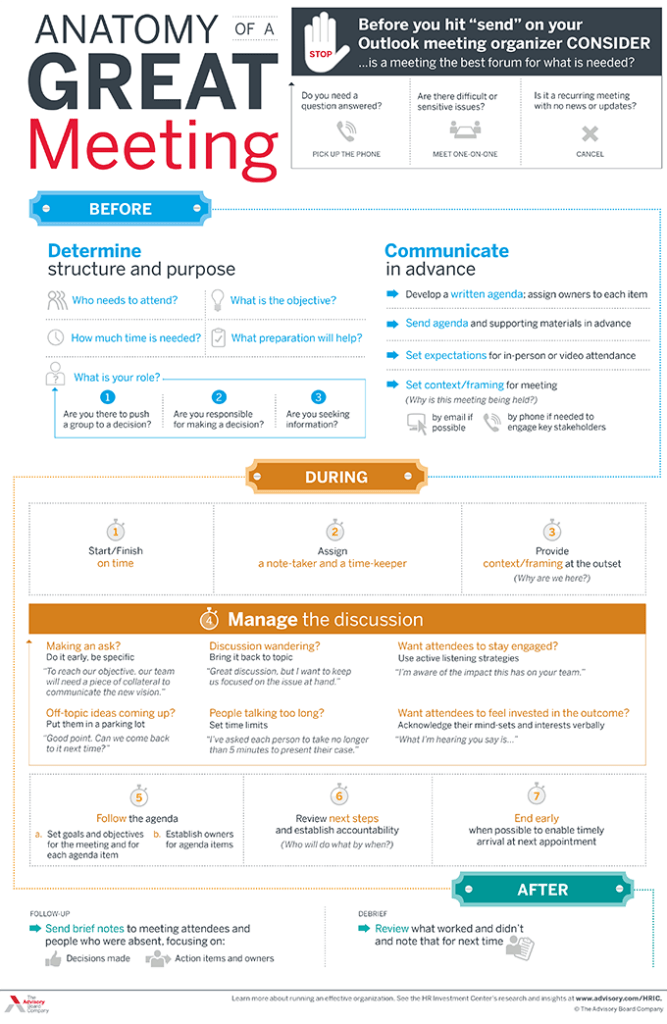
Anatomy of a Great Meeting
CVS Health is close to acquiring Oak Street Health for $10.5B

CVS Health is close to a deal to acquire primary care provider Oak Street Health for around $10.5 billion, including debt, marking the latest move among major healthcare stakeholders in acquiring primary care companies, the Wall Street Journal reports.
According to people with knowledge of the matter who spoke to the Journal, the two companies are discussing a deal in which CVS would acquire Oak Street for a price of around $39 a share. If the deal goes through, it could be announced as soon as this week.
According to the Journal, “the Oak Street acquisition would further the company’s long-term shift to broaden into businesses beyond retail pharmacy by adding doctors who can more fully manage patients’ care.”
Oak Street has more than 160 centers across 21 states and focuses mainly on caring for patients enrolled in Medicare. The company, which is based in Chicago, was founded in 2012 and specializes in caring for patients under value-based care arrangements.
Aetna, which is owned by CVS, has a growing Medicare Advantage business that would likely tie in with Oak Street’s clinics, which care for about 159,000 patients under value-based arrangements, the Journal reports.
The move is the latest among major healthcare stakeholders acquiring primary care companies. In September 2022, CVS announced an $8 billion deal to acquire home healthcare company Signify Health.
Meanwhile, Amazon in July 2022 announced a $3.9 billion deal to acquire primary care company One Medical, Humana in September 2022 announced its intention to spend up to $550 million to purchase 20 CenterWell Senior Primary Care clinics, and Walgreens Boots Alliance in November 2022 announced a roughly $9 billion deal to acquire Summit Health.
The 6 challenges facing health care in 2023—and how to handle them

With input from stakeholders across the industry, Modern Healthcare outlines six challenges health care is likely to face in 2023—and what leaders can do about them.
1. Financial difficulties
In 2023, health systems will likely continue to face financial difficulties due to ongoing staffing problems, reduced patient volumes, and rising inflation.
According to Tina Wheeler, U.S. health care leader at Deloitte, hospitals can expect wage growth to continue to increase even as they try to contain labor costs. They can also expect expenses, including for supplies and pharmaceuticals, to remain elevated.
Health systems are also no longer able to rely on federal Covid-19 relief funding to offset some of these rising costs. Cuts to Medicare reimbursement rates could also negatively impact revenue.
“You’re going to have all these forces that are counterproductive that you’re going to have to navigate,” Wheeler said.
In addition, Erik Swanson, SVP of data and analytics at Kaufman Hall, said the continued shift to outpatient care will likely affect hospitals’ profit margins.
“The reality is … those sites of care in many cases tend to be lower-cost ways of delivering care, so ultimately it could be beneficial to health systems as a whole, but only for those systems that are able to offer those services and have that footprint,” he said.
2. Health system mergers
Although hospital transactions have slowed in the last few years, market watchers say mergers are expected to rebound as health systems aim to spread their growing expenses over larger organizations and increase their bargaining leverage with insurers.
“There is going to be some organizational soul-searching for some health systems that might force them to affiliate, even though they prefer not to,” said Patrick Cross, a partner at Faegre Drinker Biddle & Reath. “Health systems are soliciting partners, not because they are on the verge of bankruptcy, but because they are looking at their crystal ball and not seeing an easy road ahead.”
Financial challenges may also lead more physician practices to join health systems, private-equity groups, larger practices, or insurance companies.
“Many independent physicians are really struggling with their ability to maintain their independence,” said Joshua Kaye, chair of U.S. health care practice at DLA Piper. “There will be a fair amount of deal activity. The question will be more about the size and specialty of the practices that will be part of the next consolidation wave.”
3. Recruiting and retaining staff
According to data from Fitch Ratings, health care job openings reached an all-time high of 9.2% in September 2022—more than double the average rate of 4.2% between 2010 and 2019. With this trend likely to continue, organizations will need to find effective ways to recruit and retain workers.
Currently, some organizations are upgrading their processes and technology to hire people more quickly. They are also creating service-level agreements between recruiting and hiring teams to ensure interviews are scheduled within 48 hours or decisions are made within 24 hours.
Eric Burch, executive principal of operations and workforce services at Vizient, also predicted that there will be a continued need for contract labors, so health systems will need to consider travel nurses in their staffing plans.
“It’s really important to approach contract labor vendors as a strategic partner,” Burch said. “So when you need the staff, it’s a partnership and they’re able to help you get to your goals, versus suddenly reaching out to them and they don’t know your needs when you’re in crisis.”
When it comes to retention, Tochi Iroku-Malize, president of the American Academy of Family Physicians (AAFP), said health systems are adequately compensated for their work and have enough staff to alleviate potential burnout.
AAFP also supports legislation to streamline prior authorization in the Medicare Advantage program and avoid additional cuts to Medicare payments, which will help physicians provide care to patients with less stress.
4. Payer-provider contract disputes
A potential recession, along with the ensuing job cuts that typically follow, would limit insurers’ commercial business, which is their most profitable product line. Instead, many people who lose their jobs will likely sign up for Medicaid plans, which is much less profitable.
Because of increased labor, supply, and infrastructure costs, Brad Ellis, senior director at Fitch Ratings, said providers could pressure insurers into increasing the amount they pay for services. This will lead insurers to passing these increased costs onto members’ premiums.
Currently, Ellis said insurers are keeping an eye on how legislators finalize rules to implement the No Surprise Act’s independent resolution process. Regulators will also begin issuing fines for payers who are not in compliance with the law’s price transparency requirement.
5. Investment in digital health
Much like 2022, investment in digital health is likely to remain strong but subdued in 2023.
“You’ll continue to see layoffs, and startup funding is going to be hard to come by,” said Russell Glass, CEO of Headspace Health.
However, investors and health care leaders say they expect a strong market for digital health technology, such as tools for revenue cycle management and hospital-at-home programs.
According to Julian Pham, founding and managing partner at Third Culture Capital, he expects corporations such as CVS Health to continue to invest in health tech companies and for there to be more digital health mergers and acquisitions overall.
In addition, he predicted that investors, pharmaceutical companies, and insurers will show more interest in digital therapeutics, which are software applications prescribed by clinicians.
“As a physician, I’ve always dreamed of a future where I could prescribe an app,” Pham said. “Is it the right time? Time will tell. A lot needs to happen in digital therapeutics and it’s going to be hard.”
6. Health equity efforts
This year, CMS will continue rolling out new health equity initiatives and quality measurements for providers and insurers who serve marketplace, Medicare, and Medicaid beneficiaries. Some new quality measures include maternal health, opioid related adverse events, and social need/risk factor screenings.
CMS, the Joint Commission, and the National Committee for Quality Assurance are also partnering together to establish standards for health equity and data collection.
In addition, HHS is slated to restore a rule under the Affordable Care Act that prohibits discrimination based on a person’s gender identity or sexual orientation. According to experts, this rule may conflict with recently passed state laws that ban gender-affirming care for minors.
“It’s something that’s going to bear out in the courts and will likely lack clarity. We’ll see differences in what different courts decide,” said Lindsey Dawson, associate director of HIV policy and director of LGBTQ health policy at the Kaiser Family Foundation. “The Supreme Court acknowledged that there was this tension. So it’s an important place to watch and understand better moving forward.”
So, Is the Pandemic Over Yet?

In his second State of the Union speech on Feb. 7, President Joe Biden made it clear that the Administration is moving into the next phase of the COVID-19 pandemic—one in which the threats of disease and death are considerably diminished, and therefore no longer require the resources and urgent allocation of funds that the previous two years have.
“While the virus is not gone…we have broken COVID’s grip on us,” Biden said. “And soon we’ll end the public health emergency.”
The President outlined his reasons for not renewing the COVID-19 national and public health emergencies when they expire on May 11, which have been extended every 90 days since they were established in 2020. The decision represents a de-escalation in the way the government is treating the pandemic.
But health experts say now is not the time to let down our collective guard on SARS-CoV-2. “I don’t believe the virus has gotten the memo that the pandemic is winding down,” says Dr. Jeffrey Glenn, director of the Stanford Biosecurity and Pandemic Preparedness Initiative.
“There is a disconnect between the broad perception that the pandemic is behind us, and focusing on getting back to life as it was pre-pandemic,” says Wafaa El-Sadr, founder and director of the International Center for AIDS Care and Treatment Programs (ICAP) at Columbia University’s Mailman School of Public Health. “But the reality is that we still continue to have substantial transmission and deaths due to COVID in the U.S., and we are in a situation where the virus will be with us for a long time.”
Even when the emergency states end, therefore, the pandemic will not be over, they and others say.
One reason is that the definition of a “pandemic” is primarily based on the breadth and speed of a virus’ spread, and the amount of the world affected by a pathogen. It’s only partially related to the severity of disease caused by a virus like SARS-CoV-2, or even the amount of immunity a population may have against it.
By that main criterion, COVID-19 is still very much with us, with around 200,000 new cases and 1,000 deaths a day globally. The latest Omicron variants quashed any hope of the pandemic ending any time soon. While they do not cause more serious infections than past variants, they have mastered the challenge of hopping more efficiently from one infected person to another.
Even though the pandemic is far from over, many health experts agree that ending the U.S. national emergencies is justified at this point. When these measures were first implemented in 2020, most people were immunological sitting ducks for the virus. The declarations were designed to devote financial resources and personnel to controlling the impact of infections on the population’s health as much as possible by shoring up the health care system and later by providing free vaccinations. U.S. officials decided to end the national and public health emergencies in May primarily because most people have either been vaccinated or have recovered from an infection (or both), so the population’s immunity stands at a higher level. COVID-19 cases—both overall and the severe kind—have declined considerably since those early days.
But the continuing stream of infections means that the virus is still reproducing and churning out mutations. So far, those variants haven’t caused more serious disease—but that’s purely by chance, which makes public health experts uncomfortable with declaring victory just yet. Even though COVID-19 cases are no longer inundating most hospitals, that means it’s time to rethink the COVID-19 response, not abandon it.
The best way forward at this point is to refine and target COVID-19 services to optimize the chances of controlling the virus where it may be causing the most health problems. “I think we need to move away from universal guidance on vaccines and boosters and mitigation measures where everybody gets the same guidance, to a more differentiated and tailored approach based on the different characteristics—both socioeconomic and clinical—of different groups of people,” says El-Sadr. “We are at a different moment in the pandemic, so the moment is now for a different message.”
That message isn’t to put COVID-19 completely behind us, but to move forward armed with the lessons we’ve learned from our experience—the most important of which is never to underestimate SARS-CoV-2.
5-hospital system exits bankruptcy with 5 new C-suite leaders

Segundo, Calif.-based Pipeline Health, now a five-hospital system, exited bankruptcy Feb. 7
Former CFO Robert Allen has replaced Andrei Soran as CEO. Mr. Allen previously served as group CEO for CHA Hollywood Presbyterian Medical Center in Los Angeles. He also held CFO positions at San Francisco-based Dignity Health and Keck Medical Center of USC, Valley Presbyterian Hospital and Sherman Oaks Hospital and Health Center, all in Los Angeles.
Four other leaders have also been appointed to executive positions:
- Steve Blake has been promoted to CFO
- Vince Green, MD, has returned to Pipeline as chief medical officer
- Patrick Rafferty assumed a new role as COO for Pipeline’s Los Angeles market while also serving as CEO for Coast Plaza Hospital in Norwalk, Calif.
- Elaine Stephenson has been promoted to vice president for human resources
Pipeline filed for Chapter 11 bankruptcy Oct. 2, and its plan to emerge was confirmed Jan. 13. Over the last few months, the system has worked through a restructuring process that included selling two Chicago hospitals, evaluating vendor contracts, creating a business plan with realistic financial goals and securing financial agreements with key stakeholders. It now owns four hospitals in the Los Anegeles area and one in Dallas.
In a memo sent Feb. 7 to employees and affiliated physicians, Mr. Allen wrote, “Hospitals across the country face similar financial challenges. You should take great pride in knowing that our company stands on solid footing now with a clear path forward. And I am proud — and grateful — that our employees and physicians have stayed with us, keeping their focus on delivering quality patient care throughout this period of uncertainty.”
Pipeline’s path forward includes a renewed commitment to quality care and an improved workforce strategy, according to Mr. Allen.
“That means providing the right care in the right place at the right time to every patient who comes to us and ensuring timely patient discharges,” he said in a Feb. 7 news release. “We also will focus on enhanced workforce management to care for the patients we serve and to enhance our critical relationships with our employees.”
11 Characteristics of Truly Inspiring Leaders
White House announces COVID public health emergency will end in May
https://mailchi.mp/a44243cd0759/the-weekly-gist-february-3-2023?e=d1e747d2d8

On the eve of a scheduled House vote on a bill that would immediately end the federal public health emergency (PHE), the Biden administration announced Monday that both the PHE and the COVID national emergency will end on May 11. With the Omnibus legislation passed at the end of December, Congress already decoupled several key provisions once tied to the PHE, including setting April 1st as the date on which states can resume Medicaid redeterminations, and extending key Medicare telehealth flexibilities.
However, once the PHE ends, various other provider flexibilities will expire: hospitals will no longer receive boosted Medicare payments for COVID admissions, and the cost of COVID tests, vaccines, and treatments will shift from the government to insurers and consumers.
The Gist: While previous Congressional action addressed some pressing provider concerns, the end of the PHE will still bring big changes.
The healthcare system will soon be responsible for covering, testing, and treating COVID like any other illness, even as the virus continues to take the lives of hundreds of Americans each day.
Many patients may soon find it difficult to access affordable COVID care, and many health systems will see an increase in uncompensated care, exacerbating current margin challenges. COVID remains an urgent public health concern in need of a coordinated strategy.