
Cartoon – Nauseously Optimistic



At least 250,000 people in the United States have died of covid-19, the disease caused by the coronavirus, since February, and many public health officials warn the pandemic is just entering its deadliest phase. Yet, as the country confronts this horrifying death toll, there is little understanding of what a loss of this size represents.
Here is some historical perspective about losing a quarter of a million people, looking at major events in our past that have cost American lives.
More than 58,000 Americans were killed during the decade-plus of involvement in the Vietnam War. So the pandemic’s fatalities represent four Vietnam Wars since February.
During the Korean War, nearly 37,000 Americans were lost; covid-19 has claimed nearly seven times more.
During World War II, the country mourned 405,000 members of the “Greatest Generation.” The pandemic has taken nearly two-thirds as many people, a lot of them old enough to remember the fight against the Nazis and the Japanese.
And World War I? 116,000 U.S. dead in two years of fighting. The pandemic has more than doubled that number in a fraction of the time.
What about our deadliest conflict, the Civil War? Death toll estimates range from 600,000 to 850,000. Even at the high end of that range, the pandemic has permanently taken nearly 30 percent as many family members from Thanksgiving tables.
On Sept. 11, 2001, almost 3,000 people were killed in terrorist attacks in New York, Washington and Shanksville, Pa.
The deadliest day of the pandemic so far — Sept. 18 — surpassed that, at 3,660 deaths. Wednesday, as the virus surged across the country, the daily death toll had risen again to 1,894. Public health officials fear that by the end of this month, the United States could lose more people per day from the pandemic than the 2,403 Americans killed in the Japanese attack on Pearl Harbor on Dec. 7, 1941.
And how does this pandemic compare to others in U.S. history?
The Centers for Disease Control and Prevention keeps records on four of them. The 2009 H1N1 pandemic killed 12,469 Americans. The 1968 Influenza A pandemic killed about 100,000 people. And the 1957-1958 Influenza A pandemic took 116,000 U.S. lives.
The deadliest event in U.S. history was the 1918 flu pandemic, which is estimated to have killed 675,000 Americans.
One of the more conservative disease models currently projects the United States could reach 438,000 deaths, more than during World War II, by March 1, 2021.

https://covidtracking.com/data/charts/us-all-key-metrics
https://covidtracking.com/data/charts/us-currently-hospitalized
https://covidtracking.com/data/charts/us-daily-deaths
https://covidtracking.com/data/charts/us-daily-positive
https://covidtracking.com/data/charts/cases-per-million-by-state
https://covidtracking.com/data/charts/hospitalized-per-million-by-state

Providence health system reported a $214 loss for the first nine months of the year, as the system continues to recover patient volume that declined during the pandemic.
The 51-hospital not-for-profit system also gave an update on its patient volumes during a recent earnings release.
Providence posted operating revenues of $18.9 billion during the first nine months of 2020, but its operating expenses ballooned to $19.1 billion.
That was an increase of 4% compared to the same period in 2019.
“The increased expenses were largely driven by the higher cost of labor, supplies and pharmaceuticals needed to safely and effectively respond to COVID-19,” Providence said in a release.
But the system is also fighting a major decline in patient volumes.
Hospital systems across the country faced plummeting patient volumes in March and April as COVID-19 spread across the country and facilities were forced to cancel or postpone elective procedures.
But even as patients started to return to the hospital in the spring and summer, volumes continue to be below pre-pandemic levels.
“Year-to-date volumes as measured by case mix adjusted admissions were 10% lower than the same period last year,” Providence said.
But a bright spot for the system has been its pivot to virtual care.
“We’ve dramatically ramped up virtual care and are on track to log 1.4 million video visits by the end of the year,” said Providence President and CEO Rod Hochman, M.D.
The income loss also comes as Providence recognized $682 million in relief funding as part of a $175 billion fund passed by Congress as part of the CARES Act.
Providence also got help from a recovering stock market.
The system posted year-to-date, non-operating income of $263 million during the first nine months of the year, compared with $772 million during the same period in 2019.
“Non-operating income helps to recoup reimbursement shortfalls from Medicaid and Medicare coverage, allowing us to serve vulnerable populations while balancing our financial standing,” Providence said.
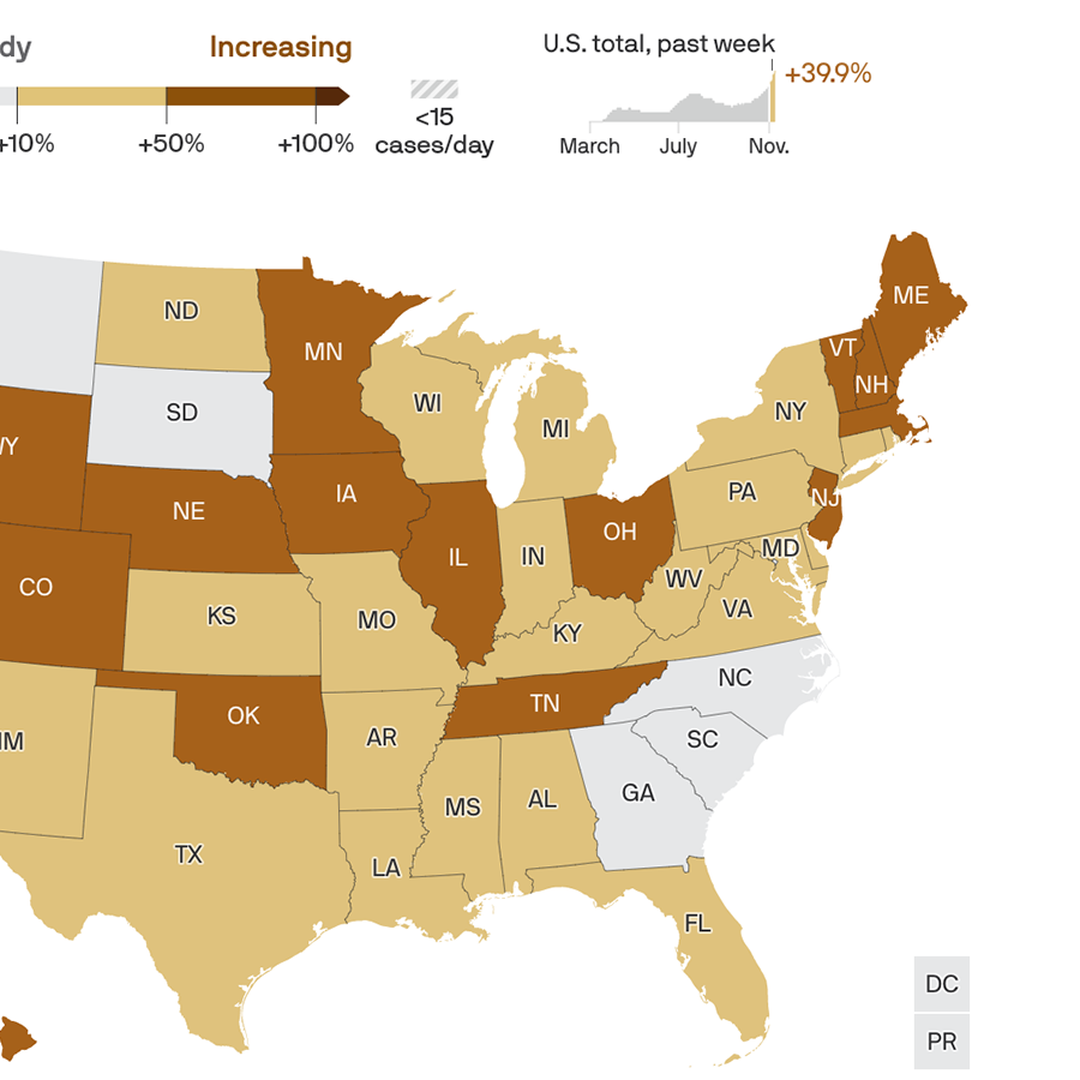
No state in America could clear the threshold right now to safely allow indoor gatherings, Axios’ Sam Baker and Andrew Witherspoon report.
The big picture: This is bad as the pandemic has ever been — the most cases, the most explosive growth and the greatest strain on hospitals.
By the numbers: Over the past week, the U.S. averaged more than 154,000 new cases per day, the highest rate of the entire pandemic.
Between the lines: Whatever metric you might use to decide whether it’s safe to have a large Thanksgiving get-together, or to sit inside a bar or restaurant, the answer is probably no.
The bottom line: Eating and drinking indoors with large groups of people, at a time when 150,000 people are contracting the virus every day, is about as risky as it gets.
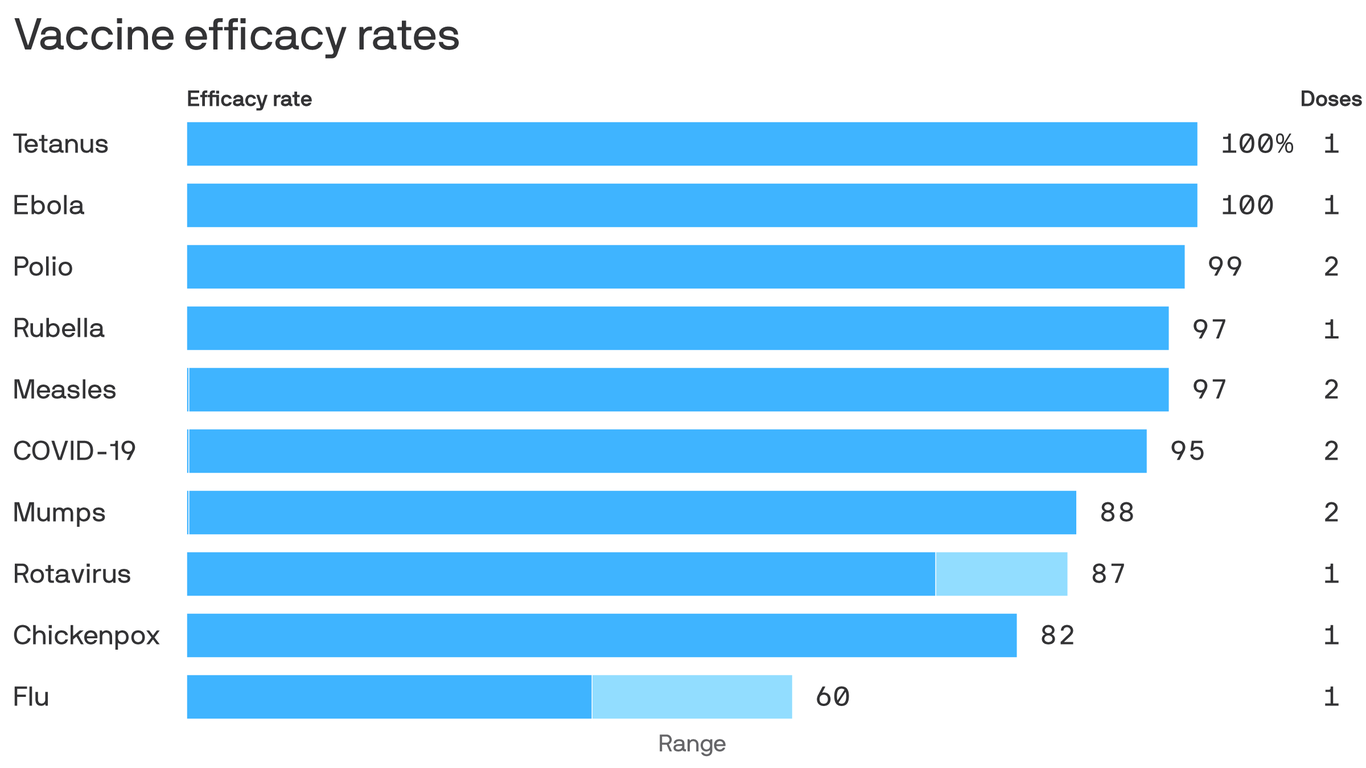
The leading coronavirus vaccines are shaping up to be on par with some of the most effective vaccines in medicine, Axios’ Marisa Fernandez reports.
Why it matters: Vaccines with efficacy rates of about 95% — which both Pfizer and Moderna say they’ve achieved — will be more powerful weapons against the coronavirus than many experts had anticipated.
Flashback: The Food and Drug Administration initially set the bar for a COVID-19 vaccine at 50% efficacy, roughly in line with the seasonal flu vaccine.
But coming in closer to 95% would put Pfizer and Moderna’s vaccines more in line with the highly effective inoculations against measles, mumps and rubella.
Yes, but: There’s still a lot we don’t know about these vaccines, including how well they’re likely to work among various demographic groups, and how long the immunity they confer will last.
At least 11,357,000 cases have been reported.
The disease caused by the novel coronavirus has killed at least 247,000 people in the United States since February and has enveloped nearly every part of the country.
As health officials long predicted, autumn brought soaring case counts, strained hospital capacity and increased deaths nationwide, as the virus is not only popping up in new places but also circling back to areas that once appeared to have it contained. Nearly all metrics in most of the country are trending in the wrong direction.
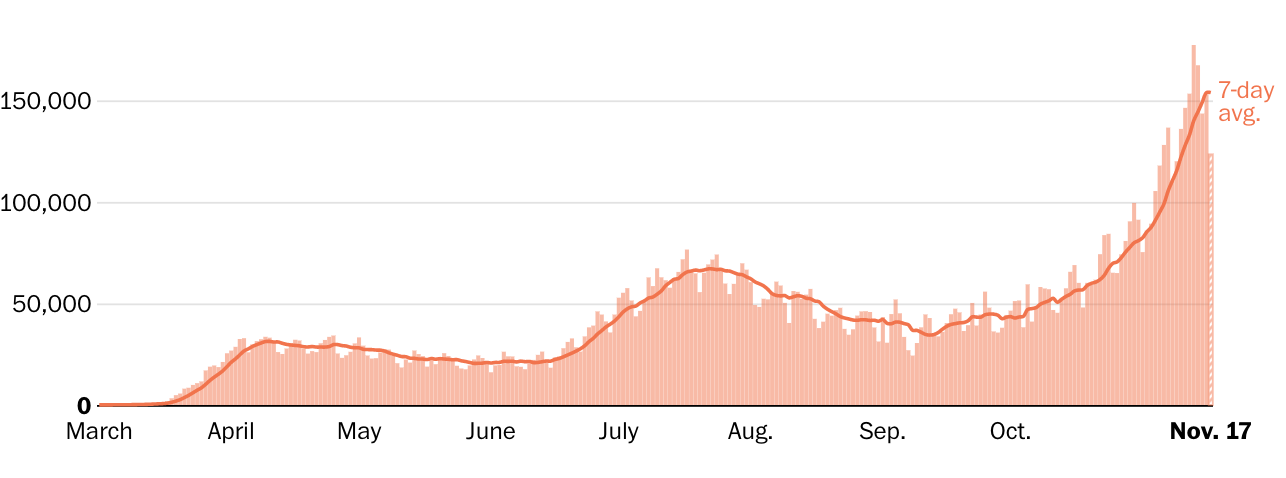
During an April peak, the seven-day-average U.S. death toll hit more than 2,000 per day, but cases were concentrated largely in the Northeast. During a July lull, average deaths sank to a low of 463 per day, although cases surged in the Sun Belt.
By early November, however, the country was recording more new cases than ever — well over 100,000 per day — and many states reported record-high caseloads and hospitalizations. The average U.S. deaths per day again shot past 1,000, despite improvements in treatment that make survival more likely.
In the past week in the U.S….New daily reported cases rose 26% New daily reported deaths rose 13.5% Covid related hospitalizations rose 23.9%.
Among reported tests, the positivity rate was 10%.
The number of tests reported rose 9.6% from the previous week.
Numbers in this article have fluctuated as testing and reporting criteria have evolved, particularly in areas that were hit early. Three spikes in the deaths chart above reflect large, one-time adjustments: In mid-April, New York City added more than 3,700 deaths. New Jersey added more than 1,800 on June 25. And in September, The Post changed its methodology for reporting deaths in New York and added a one-day increase of more than 2,700 on Sept. 18.
Health officials, including the country’s top infectious disease expert, Anthony S. Fauci, have said the virus has killed more people than official death tolls indicate.
No longer concentrated solely in a few urban areas or in nursing homes, prisons and factories, the virus seems to flourish wherever people let down their guard.
New York, which was slammed with the new disease in spring and where at least 33,000 have died, is one of several states experiencing a second or even third wave.
Sun Belt states had serious outbreaks after Memorial Day when people flocked to beaches. By late summer, parts of the Midwest were inundated. In August and September, clusters appeared in newly reopened college campuses, particularly in the Northeast and Midwest. By October, Upper Midwest, Great Plains and Western states that had previously been mostly spared were reporting major outbreaks, including Minnesota, Wisconsin, Arkansas, the Dakotas and Alaska.
In November, most states reported record-high case counts and greater demand for hospital beds. Several set records for single-day fatalities.
In the absence of a federal plan, containment strategies vary by state and locality and have often reflected political polarization. The mounting crush of cases this fall, however, has prompted officials of both parties to tighten mask mandates, reimpose restrictions on gatherings and discourage holiday travel and gatherings to try to squelch the spread.
A majority of states and many retail chains required masks in public places by late July, and public health officials touted them as one of the easiest ways to stop the pandemic. Still, some people in even the hardest-hit areas refuse to wear them, despite evidence that they protect wearers and those around them.
People older than 65 and those with obesity and underlying health problems are the mostly likely to die from covid-19, but a large percentage of infections occur in younger, more mobile people. People younger than 40 tend to become less sick but also unknowingly may pass the disease to others around them.
The virus rarely kills children, although researchers have linked it to a mysterious and deadly inflammatory syndrome.
Outbreaks of covid-19 have hit Black, Hispanic and Native American communities particularly hard.
Sparsely populated areas don’t have the huge raw numbers that cities have reported, but some rank among the highest in deaths and cases per capita.
By late October, covid-19 had been documented in all but three U.S. counties and areas in Montana, the Dakotas and Idaho had some of the highest per capita caseloads.
People in very rural areas may be more vulnerable to covid-19 than urbanites, according to a Post analysis of CDC data.
Testing was slow to begin in the United States, and a system has yet to be standardized.
Demand has often overwhelmed testing infrastructure, muddying the ability of officials to get a true picture of the virus’s reach. In June, CDC Director Robert Redfield estimated that, based on antibody tests, the actual number of U.S. residents who had been infected by the virus was likely to be 10 times as high as the number of confirmed cases. More recently, conflicting CDC guidelines about whether people without symptoms should be tested caused confusion and inhibited contact tracing.
A sharp increase in hospitalizations in late October and November demonstrates that the virus is spreading, not just that more testing is finding more asymptomatic cases. A group of Illinois health-care workers predicted in a Nov. 10 open letter to state and Chicago officials that “Illinois will surpass its ICU bed capacity by Thanksgiving.”
Some hospitals, straining to find beds and health-care workers to handle the crush of patients, are considering unusual measures.
In North Dakota, health-care workers who test positive but have no symptoms can continue working in covid-19 wards, according to Gov. Doug Burgum (R). Some facilities in Oklahoma, Kansas and Ohio are limiting routine care and deferring non-emergency surgeries.
Not all news is bleak, however.
On Nov. 9, Pfizer announced that its promising vaccine — one of many in the works — appeared more than 90 percent effective in an ongoing trial. The same day, regulators granted emergency authorization to an antibody treatment that may keep mild illness from becoming severe.
And the next day, Fauci told CNN that the average American may have access to a vaccine by April.

State-level reports are the best publicly available data on child COVID-19 cases in the United States. The American Academy of Pediatrics and the Children’s Hospital Association are collaborating to collect and share all publicly available data from states on child COVID-19 cases (definition of “child” case is based on varying age ranges reported across states; see report Appendix for details and links to all data sources).
As of November 12th, over 1 million children have tested positive for COVID-19 since the onset of the pandemic. The age distribution of reported COVID-19 cases was provided on the health department websites of 49 states, New York City, the District of Columbia, Puerto Rico, and Guam. Children represented 11.5% of all cases in states reporting cases by age.
A smaller subset of states reported on hospitalizations and mortality by age; the available data indicated that COVID-19-associated hospitalization and death is uncommon in children.
The number of new child COVID-19 cases reported this week, nearly 112,000, is by far the highest weekly increase since the pandemic began. At this time, it appears that severe illness due to COVID-19 is rare among children. However, there is an urgent need to collect more data on longer-term impacts on children, including ways the virus may harm the long-term physical health of infected children, as well as its emotional and mental health effects.
(Note: Data represent cumulative counts since states began reporting)
* Note: Data represent cumulative counts since states began reporting; All data reported by state/local health departments are preliminary and subject to change
Download Full Report (11/12/2020)
Download Full Report (11/5/2020)
Download Full Report (10/29/2020)

Like a lot of people, I have really gotten into listening to podcasts over the last year. They’re such an immersive way to learn about the world, and I like how the format lets you dive as deep on a topic as you want. So, I was inspired to start one of my own—but I knew I couldn’t do it on my own.
I couldn’t ask for a better partner on this project than Rashida Jones. A mutual friend suggested that the two of us might have a lot to talk about, and it turned out he was right. I already knew she was a talented actor, but I was impressed by her thoughtful perspective on the world. So, we decided to start a podcast that lets us think through some of today’s most pressing problems together. In our first episode, Rashida and I explore a big question that is top of mind for many people: what will the world look like after COVID-19?
I know it’s hard to imagine right now while new cases are surging around the world, but there will come a time when the COVID-19 pandemic is behind us. I think it’s safe to assume that society will be changed forever, given how disruptive the virus has been to virtually every part of our lives.
Unfortunately, we still have a long way to go before life truly gets back to “normal.” Rashida and I were joined by Dr. Anthony Fauci, the director of the National Institute of Allergy and Infectious Diseases, to discuss what to expect in the months to come. I’ve had the opportunity to work with Dr. Fauci on a number of global health issues over the years, including the quest for an HIV vaccine and cure. He’s such a quiet and unassuming guy normally, so it’s been wild to watch him become a huge celebrity.
Dr. Fauci and I are both optimistic that a vaccine will bring an end to the pandemic at some point in the near future. But what the world looks like after that is a lot less clear. I suspect that some of the digitization trends we’ve seen—especially in the areas of online learning, telemedicine, and remote work—will become a regular part of our lives. I hope this episode leaves you hopeful about the future and curious about what comes next.
