Martin Luther King Jr.’s Healthcare Justice Advocacy Makes America’s Hospitals Better Today

Every January, the United States celebrates the lasting legacy of Dr. Martin Luther King Jr. Not widely known is how his civil rights advocacy made a lasting impact on modern-day hospitals, including children’s hospitals.
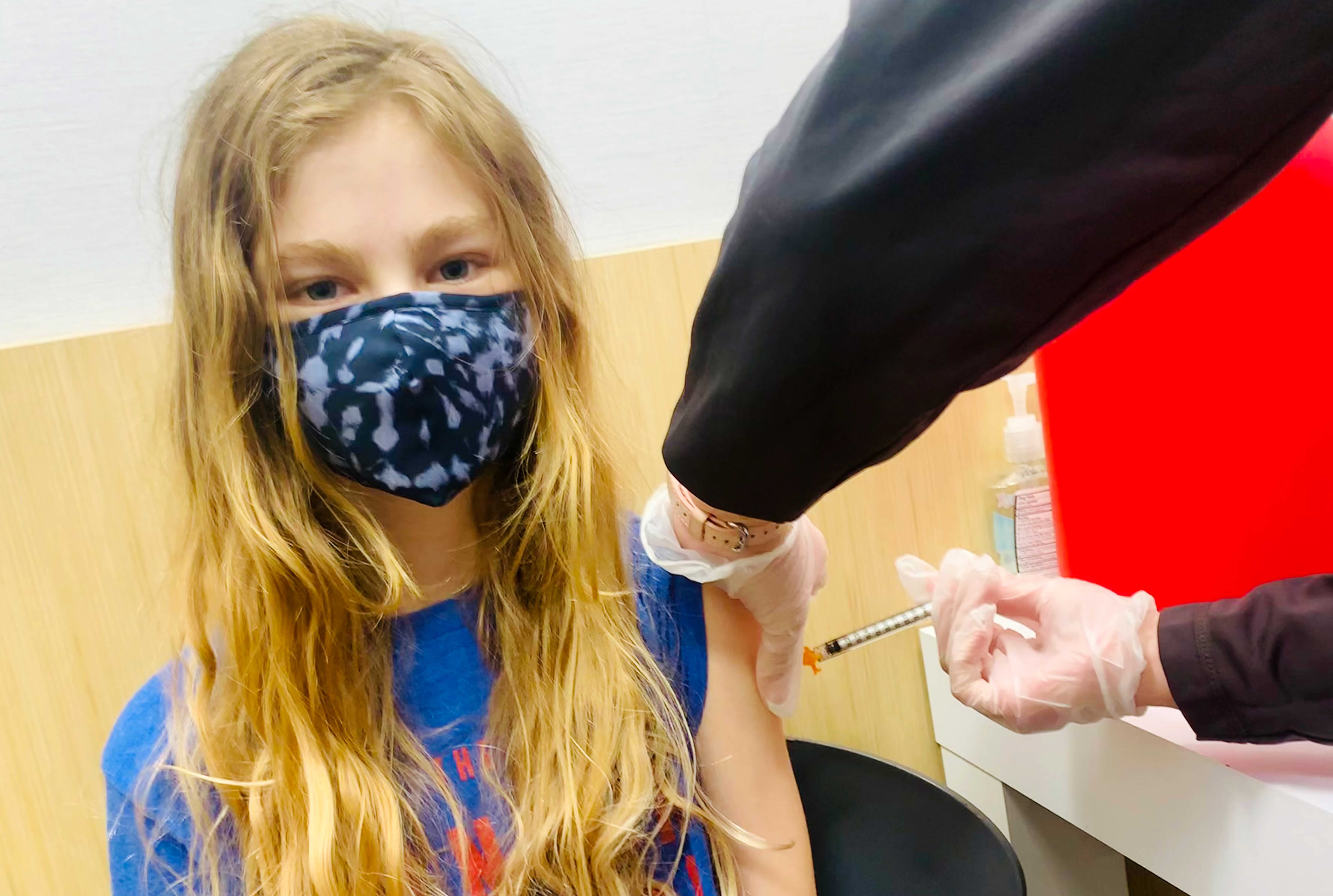
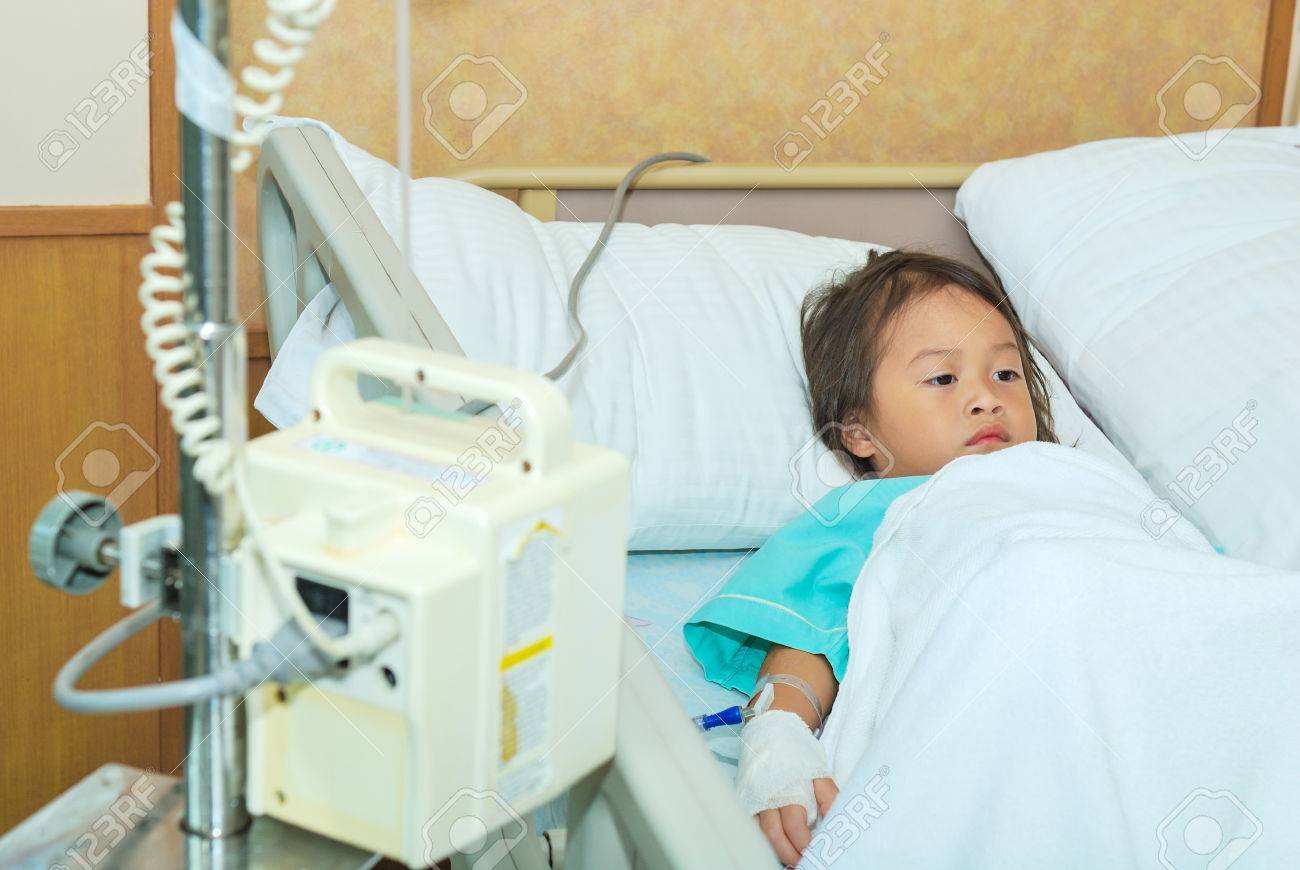
Today in 170 Children’s Miracle Network Hospitals, every young patient is treated regardless of their race or background. CMN Hospitals are deeply committed to offering world-renowned treatment to all kids in need and that’s why donations to your local hospital can make such a difference for families facing health crises.
Unfortunately, certain hospitals in America were still segregated in the not too recent past. When Brown vs. Board of Education passed in 1954, schools began to desegregate, and this paved the way for institutions like hospitals to follow suite. King’s healthcare justice advocacy advanced health care access in particular for the African American community.
A History of Unequal Healthcare
When patients enter a hospital, they expect to receive a standard of care that will improve their lives regardless of who they might be. That expectation, unfortunately, has not always been backed up by medical institutions across the United States. African Americans, in particular, experienced a history of receiving substandard care and outright abuse within the framework of medical science.
Notable examples of this include:
While the details of those specific examples weren’t publicly known in the 1960s, African Americans were certainly aware that they received care that was inferior to white patients. Doctors and hospitals continued perpetuating this double standard even after the passage of the Civil Rights Act in 1964. The disparity in treatment quality was so egregious that Dr. Martin Luther King Jr. spoke out against it, calling for an awakening in the conscience of the United States.
Desegregating Hospitals
King uttered his famous words on healthcare while addressing the press before attending the annual meeting of the Medical Committee for Human Rights, an organization formed because the American Medical Association was segregated at the time. “Of all the forms of inequality, injustice in health is the most shocking and the most inhuman because it often results in physical death,” said King.
The Civil Rights Act of 1964 isn’t typically associated with healthcare. However, at that point in history, it was well known that some hospitals and medical institutions were resisting the push for desegregation, a practice which hospitals used to provide less than adequate care to African American patients. Hospitals would continue to hold onto such discriminatory practices unless something was done.
Legal Gains for Equality in Hospitals
The reason King spoke out so vehemently in 1966 was due to the passage of Medicare and Medicaid in 1965, something that was only possible due to the efforts of the Medical Committee for Human Rights and its head, W. Montague Cobb. The organization made use of the non-violent protest strategies of King and the Civil Rights Movement. The passage of the Social Security Act, which created Medicare and Medicaid brought federal funding into every hospital and medical institution in the United States, forever binding each facility to the Civil Rights Act, a stipulation of which was that any organization receiving federal funding could not discriminate on the basis of race.
From that point onward, hospitals that clung to the old ways of discrimination were subject to lawsuits from mistreated African Americans and pressure from activists like King and the Medical Committee for Human Rights. This gave King the legal ground to stand on when calling on hospitals to abandon the evil practice of systemic discrimination in 1966 with those now famous words from that 1966 conference.
While we know there’s more work to be done to promote equal healthcare access to every child in need across North America, we’re proud that our non-profit children’s hospitals can be a part of the solution.
Thank you, King.