According to a new report from the American Hospital Association (AHA), hospitals and health systems are facing significant financial pressures from rising expenses, including for labor, drugs, medical supplies and more. And without increased government support, the organization warns that patients’ access to care could be at risk.
Hospitals continue to see expenses grow, negative margins
In the report, AHA writes that several factors, including historic inflation and critical workforce shortages leading to a reliance on contract labor, led to “2022 being the most financially challenging year for hospitals since the pandemic began.”
According to data from Syntellis Performance Solutions, overall hospital expenses increased by 17.5% between 2019 and 2022 — more than double the increases in Medicare reimbursements during the same time. Between 2019 and 2022, Medicare reimbursement only grew by 7.5%.
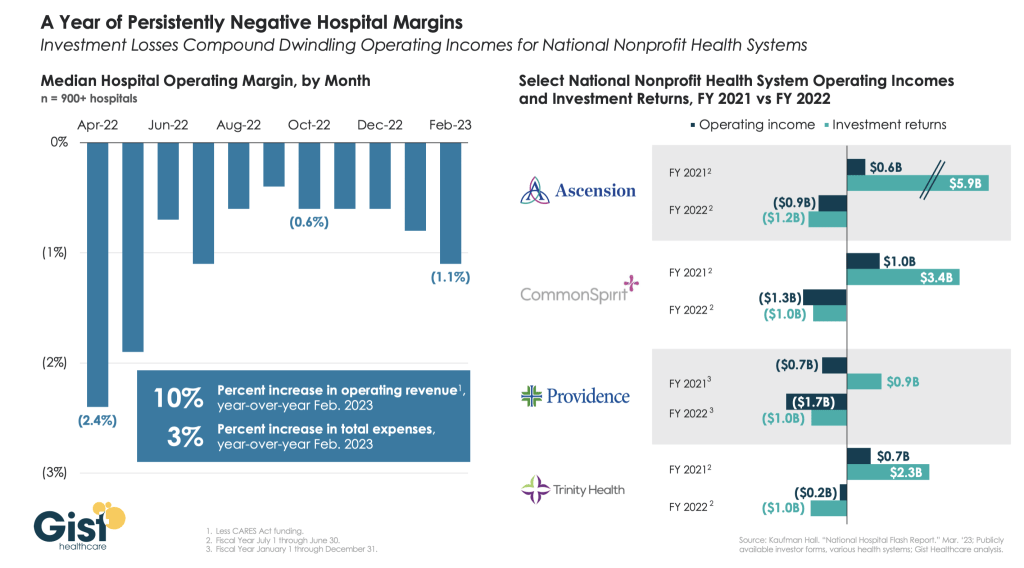
With expenses significantly outpacing reimbursement, hospital margins have been consistently negative over the last year. In fact, AHA noted that “over half of hospitals ended 2022 operating at a financial loss — an unsustainable situation for any organization in any sector, let alone hospitals.”
So far, this trend has continued into 2023, with hospitals reporting negative median operating margins in both January and February.
A recent analysis also found that the first quarter of 2023 had the largest number of bond defaults among hospitals in over 10 years.
Where are hospital expenses increasing?
Between 2019, and 2022 hospital labor expenses increased by 20.8%, a rise that was largely driven by a growing reliance on contract labor to fill in workforce gaps during the pandemic. Even after accounting for an increase in patient acuity, labor expenses per patient increased by 24.7%.
Compared to pre-pandemic levels, hospitals saw a 56.8% increase in the rates they were charged for contract employees in 2022. Overall, hospitals’ contract labor expenses increased by a “staggering” 257.9% in 2022 compared to 2019 levels.
A sharp rise in inflation in recent months has also led to a significant increase in hospitals’ non-labor expenses, particularly for drugs and medical expenses. According to a report by Kaufman Hall, just non-labor expenses would lead to a $49 billion one-year expense increase for hospitals and health systems.
Since 2019, non-labor expenses have grown 16.6% per patient. Hospitals’ expenses for drugs and medical supplies/equipment have seen similar increases per patient at 19.7% and 18.5%, respectively. Costs of laboratory services (27.1%), emergency services (31.9%), and purchased services, including IT and food and nutrition services, (18%) have also increased significantly per patient.
Outside of labor and non-labor expenses, AHA writes that policies from health insurers have also contributed to significant burden among hospital staff and increased administrative costs. Currently, administrative costs account for up to 31% of total healthcare spending — of which, billing and insurance makes up 82%.
What Congress can do to support hospitals
With the COVID-19 public health emergency ending on May 11, several important hospital waivers and flexibilities will soon end, and “[t]he downstream effects of this will be wide-ranging as hospitals will be faced with a set of additional challenges,” AHA writes.
“Rising costs for drugs, supplies, and labor coupled with sicker patients, longer hospital stays, and government reimbursement rates that do not come close to covering the costs of caring for patients have created a dire situation for hospitals and health systems,” said AHA president and CEO Rick Pollack.
“This is not just a financial problem; it is an access problem.
When healthcare providers cannot afford the tools and teams they need to care for patients, they will be forced to make hard choices and the people who will be impacted the most are patients. We can’t let that happen. Congress and others must act to preserve the care our nation needs and depend on.”
To address these financial challenges and ensure that hospitals are able to continue caring for patients, AHA has suggested several actions Congress could take to support hospitals going forward, including:
- Enacting policies to support efforts to boost the healthcare workforce and ensure of future pipeline of professionals to combat longstanding labor shortages
- Rejecting attempts to cut Medicare or Medicaid payments to hospitals, which could further reduce patients’ access to care
- Encouraging CMS to use its “special exceptions and adjustments” to make retrospective adjustments to account for differences between what was implemented for fiscal year 2022 and what is currently projected
- Creating a special statutory designation and providing additional support to hospitals that serve historically marginalized communities
“As the hospital field maintains its commitment to care in the face of significant challenges, policymakers must step up and help protect the health and well-being of our nation by ensuring America has strong hospitals and health systems,” AHA writes.