https://www.beckershospitalreview.com/strategy/hospitals-and-health-systems-6-trends-and-issues.html

This article discusses the current state and issues of hospitals and health systems for several different areas. First, this discusses types of hospitals and health systems. Second, it addresses what’s working and what’s not for health systems. Third, this discusses the mix of access, quality and cost as well as the shortages of different kinds of providers fourth. Fifth, this discusses policy issues and political issues. Sixth, we address threats and challenges.
1. 5,200+ acute-care hospitals. Currently, there are approximately 5,200 acute-care hospitals in the country. This number changes a little each year, with more closures than openings.
We view the landscape as one with seven core types of health systems.
First, there’s what we think of as the very elite health systems, which are often academic medical centers. This usually includes the top 20 to 30 systems as ranked by U.S. News & World Report. These are typically great research institutions that provide great care in some of the most critical, life-threatening areas. This category may include hospitals like NewYork-Presbyterian, UChicago Medicine, Cleveland Clinic, Mayo Clinic, Northwestern Medicine and a number of other institutions that typically comprise the top 20 to 30 in the U.S. News & World Report’s Best Hospitals.
Second are regionally dominant systems. These systems are so important to a given area that they are often the focus point of care in said area. There are also situations where it’s very hard for payers and patients to go around these institutions — even if they wanted to. This might be an institution like Carilion Clinic or Sentara Healthcare in Virginia, Northwell in New York, Ochsner in Louisiana or NorthShore University Health System in the north suburbs of Chicago. It may be Advocate Aurora Health in the Chicagoland area and Eastern Wisconsin, Hartford HealthCare in Connecticut, Intermountain Healthcare in Utah and Idaho, and a number of institutions regionally strong in their areas.
A third type of system is the community hospital, typically the single- or two-hospital system. This could be rural, urban or suburban. Here, this may be a health system that has served as the core of primary care — and at one time tertiary care — for a community, but more and more has to have a certain reason for being, something that its really great at to remain relevant and open.
A fourth type of hospital is what we think of as a specialty hospital, usually built around a certain specialty like pediatrics, behavioral health, oncology or some other area. It is a hospital that has a specific focus and is just great at what it does, much like Hospital for Special Surgery in New York, which U.S. News & World Report has ranked as the No. 1 hospital in the country for orthopedics for the past 10 years.
National chains of hospitals and health systems make up the fifth type of system. This can be for-profit or nonprofit, and they come in a couple different varieties. First, they can pursue a strategy of being in lots of different markets, but regionally dominant in the markets they’re in. This has typically been the strategy for success. Second, they can pursue the strategy of having the most hospitals possible. This has typically not been a strategy for success. Market strength or market dominance and excellence in certain areas is far more important than having lots of different hospitals.
The sixth type of hospital that we think of as Kaiser Permanente. Here, we put Oakland, Calif.-based Kaiser Permanente in its own category. It is a regionally dominant system in certain parts, but more importantly it is vertically integrated with its own insurance plan. This has allowed Kaiser to do things in the cost savings areas and the efficiency area that many other systems have not been able to do. We have also found over the last decade that it is much harder for other systems to replicate what Kaiser has done, in terms of fully integrating insurance, than expected.
The seventh category of hospital we think of as the safety-net hospital. The safety-net hospital can really be in any of the above categories. We largely think of safety-net hospitals as those that are serving a huge percentage of Medicare and Medicaid patients. The safety-net hospital is a very important part of the fabric of American healthcare and the delivery system, and at the same time they often struggle to ensure they have the finances to make the system go.
2. What has worked the last 10 years? The three types of categories that have really worked the past 10 years are as follows.
First, one prescription for success has been to be regionally dominant. Whether a Novant Health or an Atrium Health, both based in North Carolina, or a system like Advocate Aurora in Wisconsin or ProMedica in Ohio, being regionally strong has been a prescription for success. It allows one to stack resources, invest in talent, invest in systems and get better and better.
The second prescription for success the last decade and for a long time is being an elite health system. As much as the world changes, these elite systems — whether Stanford Medicine, Mayo Clinic, Cleveland Clinic or UCLA Health — continue to be sought out for care and continue to recruit great physicians, researchers and providers. This may also include being elite in certain areas like Rush University Medical Center in Chicago in orthopedics, MD Anderson in oncology or a number of other actors that are elite.
The third type of category that has worked is clearly the Kaiser Permanente category. This is a situation where Kaiser is almost its own vehicle, led famously by the late Bernard J. Tyson. Over the years, Kaiser grew into being a great integrated system and was able to do things on the value-based side and make major investments to address social determinants of health that really no one else was able to do.
3. Access, quality and cost. There is constant discussion of access, quality and cost. As we look as things evolve, we see things as follows.
On the quality side, the American healthcare system seems to do a pretty good job of delivering pretty good care to a huge percentage of people. In essence, compared to other countries, the U.S. is providing care to more than 325 million people. While imperfect, it is pretty good. There are pockets of care in other countries that are certainly better and more advanced than it is here, but often in pockets versus an entire system.
In terms of access, the American healthcare system seems to be challenged in numerous ways. As shortages evolve, particularly among specialties and subspecialties, it is harder and harder to find access to the right type of provider when one needs that provider. Access can also be a challenge in many different ways for poor communities in our country and, of course, there is no quality without access.
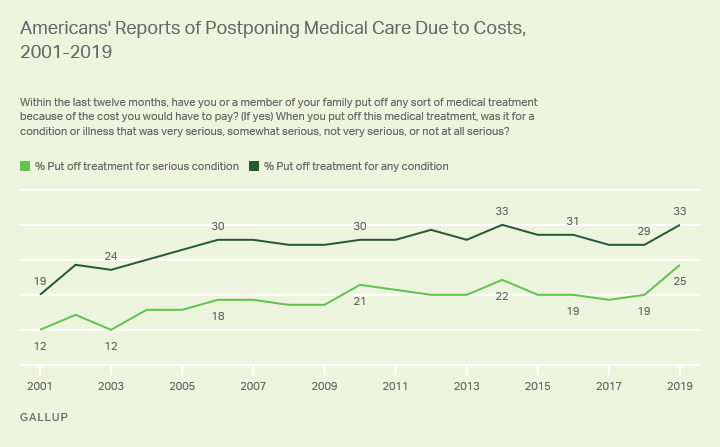
A third issue in terms of the American healthcare system is cost. As costs continue to grow at a percentage higher than inflation, particular pockets of costs remain very challenging, specifically on the pharmaceutical side, technology side and labor side.
4. Shortages of doctors and allied health professionals. As we look at access challenges in the country, there is a perspective that it is very hard to solve without the minting of a great deal more of physicians and allied health professionals. Even as the ways care is delivered evolve, the physician shortage remains. We will see a shortage of up to nearly 122,000 physicians by 2032 as the population grows and ages and demand continues to grow faster than supply, the Association of American Medical Colleges.
There are different structural elements in place that make it hard to add on providers at a fast clip. For example, medical school, residency and fellowship take many years. In efforts to modernize medical education, there is a question as to whether that much education is needed. The American Medical Association is one body that is working with major institutions for accelerated programs, like a six-year model at University of California, Davis School of Medicine. The school offers a six-year path to practice — three years each of medical school and residency — in partnership with Kaiser Permanente Northern California.
As we look at our society, we probably need more incentive for people to go to medical school and graduate with medical degrees than are currently in place. The more one tries to attack some of benefits of being a physician, the harder it is to encourage the next generation to become physicians. In response, we do see a growing number of medical schools being opened, including those at Kaiser Permanente and Hackensack Meridian. We think this is absolutely critical. It is also critical that we develop more and more allied health professionals and those allied health professionals are largely able to practice at the top of their license.
Finally, there is this concept in medical school and in premed of “weed out” classes. We believe this is somewhat overdone and overemphasized, and many bright, talented people are weeded out that would be perfectly great physicians. As one resident at Stanford University School of Medicine put it, “Today we ‘weed out’ potentially wonderful doctors through a demoralizing maze of basic sciences that more often resembles the Hunger Games than a sensible recruitment process.”
5. Political polarization. In healthcare, and the hospital sector specifically, we see a great deal of political polarization. There are largely three different types of systems that people think about in terms of reform.
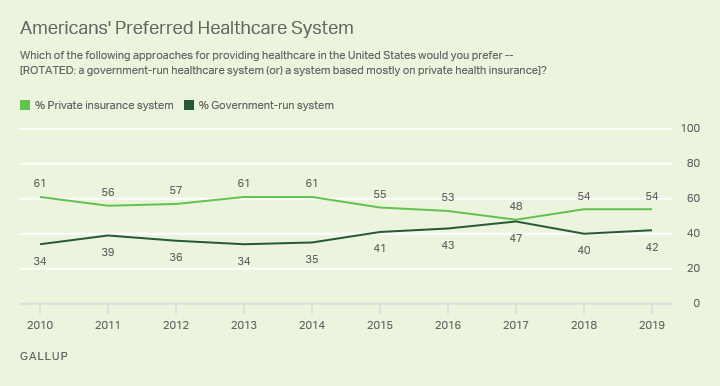
First, there is the “Medicare for All” perspective. While this would provide adequate “access” at a certain level for everybody in terms of health insurance coverage, there is concern from providers that reimbursement would be so low it would not encourage people to pursue medicine, thus flattening or denting the supply of physicians needed to provide the care that is needed.
Second, there is the concept of the “free market.” Here, the concept of a total free market and free market alternatives is somewhat illusory. In reality nearly 30 to 50 percent of most providers’ revenue comes from Medicare and Medicaid. Thus, you are never really dealing with a free market in healthcare. There are free market incentives — like health savings plans and transparency — that can help, but one is not in total dealing with a free market.
Third, is the concept of a public option. One way to think about a public option is to think about it as akin to the post office. One can either go to the post office to mail something via the United States Postal Service, or one could use UPS or Federal Express. The idea of a public option is that you would not have to buy insurance from an insurance company. Rather, you could buy into the Medicare program through a public option. Washington signed a public option into law this past summer and will launch it in 2021, becoming the first state to test the policy.
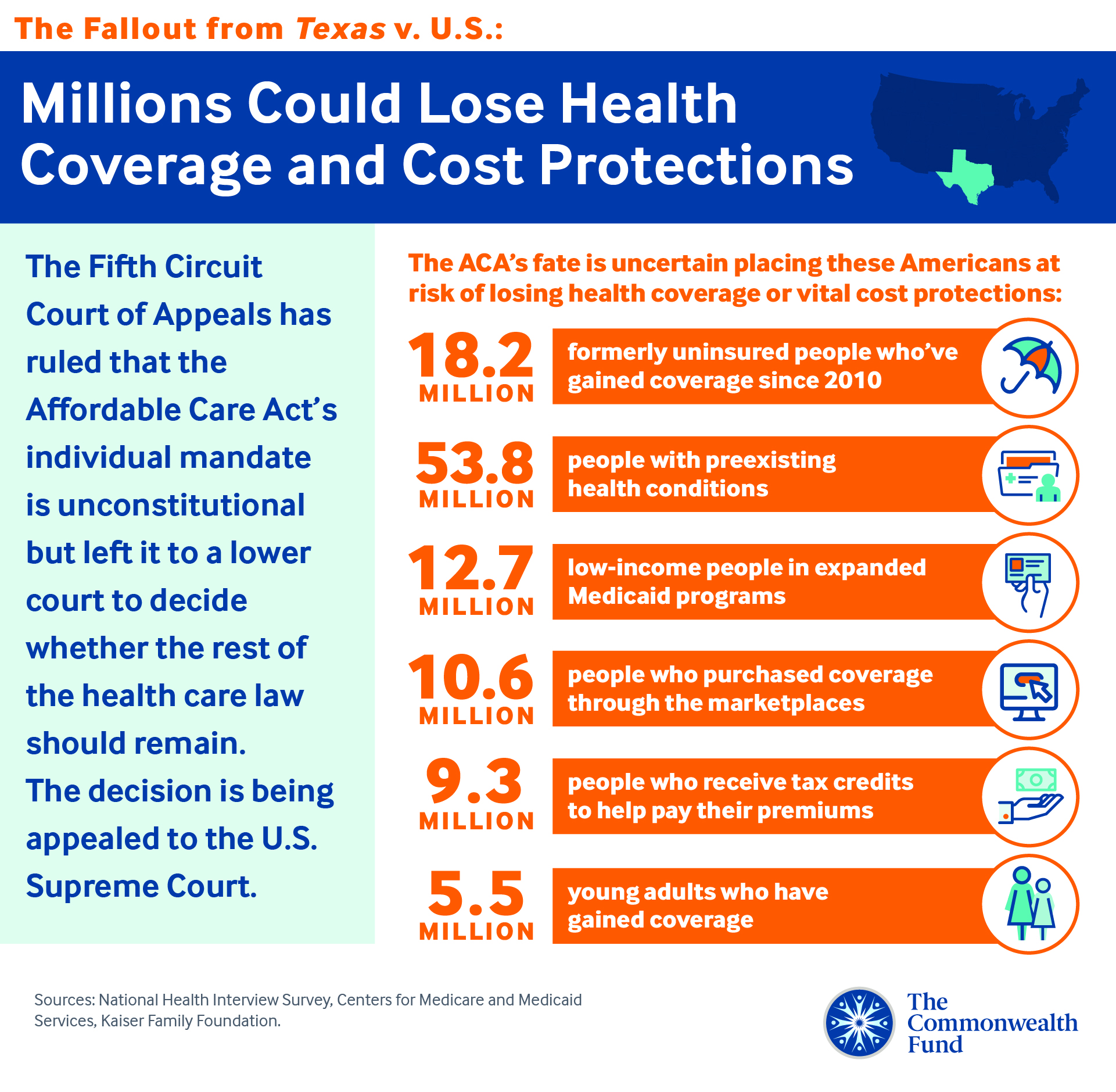
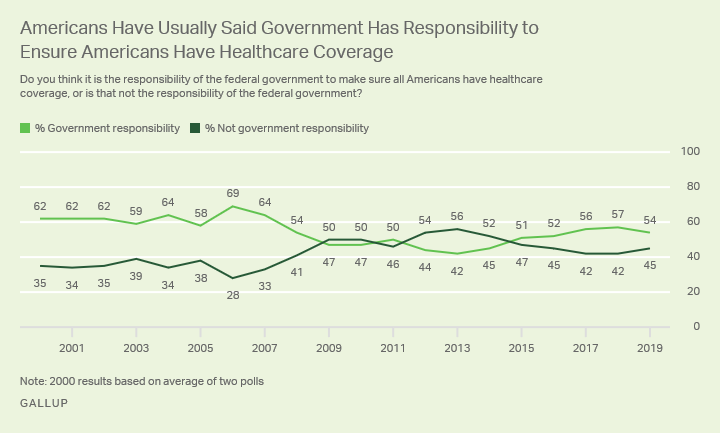
Whatever the answer is for healthcare reform, it is clear that the general public prefers two things. First, they like the concept that you should be able to buy insurance regardless of whether or not you have a pre-existing condition. Second, a large percentage of the public seems to prefer that there be some sort of public option to access care.
6. Threats and challenges. Some the challenges healthcare systems face today are as follows.
First, the strength of payers and the power they hold, especially as they diversify and broaden their scope of business. Under the UnitedHealth Group umbrella, for instance, is Optum, the Advisory Board and Equian, among other arms. In 2018, Cigna acquired Express Scripts, CVS Health combined with Aetna, and Humana and private equity firms acquired Kindred Healthcare. Highmark, one of the largest insurers in the country, acquired the West Penn Allegheny Health System years ago. Each of these forays into technology, consulting, payment, pharmacy benefit management, post-acute care and provider spaces make health insurers more prevalent in the industry.
A second great concern is the growing number of access points that are providing threats to health systems and their margins and revenues. This may be things like the CVS’, Walgreens and Walmarts of the world, which are expanding the medical services and health hubs in their stores to provide consumers with an alternative access point for chronic conditions and routine care. This fall, Walmart even revealed plans to build its own healthcare workforce.
Third, powerful payers are developing provider networks and providing alternatives to health systems and their delivery systems. Blue Cross Blue Shield Association, for instance, will launch a national provider network in 2021 that spans across 55 markets to help large employers better control medical costs.
Fourth is the total costs of bricks and mortar and labor that hospitals and health systems carry.
Fifth is the development of new types of insurance programs by companies like Haven, which is JPMorgan, Berkshire Hathaway and Amazon’s effort to serve their combined 1.2 million employees. Currently, commercial insurance and payments from employed people ultimately subsidize what hospitals and health systems receive from Medicare and Medicaid. Thus, if these efforts like Haven are successful at peeling off good-paying patients, this will have a big negative impact on hospitals and health systems.