
Category Archives: Unvaccinated
US COVID-19 cases fall for 4th consecutive week: 9 CDC stats to know
COVID-19 cases have declined nationwide for the fourth consecutive week, according to the CDC’s COVID data tracker weekly review published Oct. 15.
Nine numbers to know:
Reported cases
1. The nation’s current seven-day case average is 84,555, a 12.5 percent decrease from the previous week’s average.
Hospitalizations
2. The current seven-day hospitalization average for Oct. 6-12 is 6,659, an 8.8 percent drop from the previous week’s average.
Vaccinations
3. About 218 million people — 65.6 percent of the total U.S. population — have received at least one dose of the COVID-19 vaccine, and more than 188.3 million people, or 56.7 percent of the population, have gotten both doses.
4. About 9.3 million booster doses in fully vaccinated people have been reported.
5. The seven-day average number of vaccines administered daily was 841,731 as of Oct. 14, a 11.3 percent decrease from the previous week.
Variants
6. Based on projections for the week ending Oct. 9, the CDC estimates the delta variant accounts for more than 99 percent of all U.S. COVID-19 cases.
Deaths
7. The current seven-day death average is 1,241, down 13.4 percent from the previous week’s average. Some historical deaths have been excluded from these counts, the CDC said.
Testing
8. The seven-day average for percent positivity from tests is 5.7 percent, down 4.1 percent from the previous week.
9. The nation’s seven-day average test volume for the week of Oct. 1-7 was about 1.49 million, down 5.4 percent from the prior week’s average.
Breakthrough infections might not be a big transmission risk. Here’s the evidence
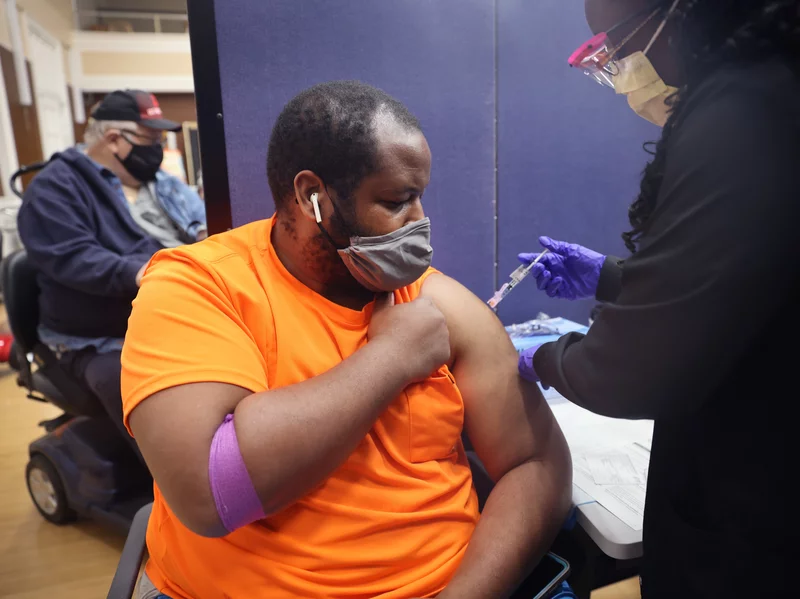
Conventional wisdom says that if you’re vaccinated and you get a breakthrough infection with the coronavirus, you can transmit that infection to someone else and make that person sick.
But new evidence suggests that even though that may happen on occasion, breakthrough infections might not represent the threat to others that scientists originally thought.
Ross Kedl, an immunologist at the University of Colorado School of Medicine, will point out to anyone who cares to listen that basic immunology suggests the virus of a vaccinated person who gets infected will be different from the virus of an infected unvaccinated person.
That’s because vaccinated people have already made antibodies to the coronavirus. Even if those antibodies don’t prevent infection, they still “should be coating that virus with antibody and therefore helping prevent excessive downstream transmission,” Kedl says. And a virus coated with antibodies won’t be as infectious as a virus not coated in antibodies.
Scant evidence for easy transmission of breakthrough infections
In Provincetown, Mass., this summer, a lot of vaccinated people got infected with the coronavirus, leading many to assume that this was an example of vaccinated people with breakthrough infections giving their infection to other vaccinated people.
Kedl isn’t convinced.
“In all these cases where you have these big breakthrough infections, there’s always unvaccinated people in the room,” he says.
In a recent study from Israel of breakthrough infections among health care workers, the researchers report that in “all 37 case patients for whom data were available regarding the source of infection, the suspected source was an unvaccinated person.”
It’s hard to prove that an infected vaccinated person actually was responsible for transmitting their infection to someone else.
“I have seen no one report actually trying to trace whether or not the people who were vaccinated who got infected are downstream — and certainly only could be downstream — of another vaccinated person,” Kedl says.
There’s new laboratory evidence supporting Kedl’s supposition. Initially, most vaccine experts predicted that mRNA vaccines like the ones made by Pfizer and Moderna that are injected into someone’s arm muscle would generate only the kinds of antibodies that circulate throughout the body.
But that might not be the whole story.
“I think what was the big surprise here is that the mRNA vaccines are going beyond that,” says Michal Caspi Tal, until recently an instructor at Stanford University’s Institute for Stem Cell Biology and Regenerative Medicine and now a visiting scientist at the Massachusetts Institute of Technology.
What Tal has found is that in addition to the circulating antibodies, there was a surprisingly large amount of antibodies in mucosal membranes in the nose and mouth, two of the primary entry points for the coronavirus.
The vaccinated aren’t “sitting ducks”
Immunologist Jennifer Gommerman of the University of Toronto found this as well.
“This is the first example where we can show that a local mucosal immune response is made, even though the person got the vaccine in an intramuscular delivery,” Gommerman says.
If there are antibodies in the mucosal membranes, they would likely be coating any virus that got into the nose or throat. So any virus that was exhaled by a sneeze or a cough would likely be less infectious.
Gommerman says that until now, it seemed likely that a vaccine that was delivered directly to the mucosal tissue was the only way to generate antibodies in the nose or throat.
“Obviously a mucosal vaccination would be great too. But at least we’re not sitting ducks,” Gommerman says. “Otherwise everyone would be getting breakthrough infection.”
Now, these studies by Gommerman and Tal have yet to undergo peer review, and some have already suggested that the antibodies they have described may not confer true mucosal immunity.
But there’s other evidence that a vaccinated person’s breakthrough infection may not transmit efficiently to others.
Marion Pepper, an immunologist at the University of Washington, says a recent study from the Netherlands looked at how well virus from vaccinated people could infect cells in the lab.
Pepper says the answer was not well.
“If you actually isolate virus from people who are getting a secondary infection after being vaccinated, that virus is less good at infecting cells,” Pepper says. “It’s not known why. Is it covered with an antibody? Maybe. Has it been hit by some other kind of immune mediators, cytokines, things like that? Maybe. Nobody really knows. But the virus does seem to be less viable coming from a vaccinated person.”
More studies are emerging that suggest there’s something different about the virus coming from a vaccinated person, something that may help prevent transmission.
Whatever it is, the University of Colorado’s Kedl says it’s one more reason that getting vaccinated is a good idea.
“Because you’re going to be even more protected yourself. And you’re going to be better off protecting other people.”
Kedl says that’s what you call a win-win situation.
‘A triple whammy’: Why hospitals are struggling financially amid the delta surge

n addition to treating an influx of Covid-19 patients, many hospitals are struggling with what one administrator calls a “triple whammy” of financial burdens—stemming from plummeting revenue, higher labor costs, and reduced relief funds, Christopher Rowland reports for the Washington Post.
Hospitals in less-vaccinated areas face spiking labor costs
In areas with low vaccination rates, particularly in southern and rural communities, hospitals have been overwhelmed with Covid-19 patients, exacerbating labor shortages as workers burn out or leave for more lucrative positions, Rowland reports.
“The workforce issue is just dire,” Stacey Hughes, EVP of government relations and policy for the American Hospital Association (AHA), said. “The delta variant has wreaked significant havoc on hospitals and health systems.”
In Louisiana, Mary Ellen Pratt, CEO of St. James Parish Hospital, said many nurses quit due to the grueling conditions as Covid-19 cases spiked. “I didn’t have any extra money to incentivize my staff to pick up additional shifts,” she said. “This is coming out of bottom-line money I don’t have.”
Separately, Lisa Smithgall, SVP and chief nursing executive at Ballad Health, said the health system—which has 21 hospitals in eastern Tennessee and southwestern Virginia—has faced similar problems retaining staff amid Covid-19 surges.
“We knew we were at risk in our region because of where we live and because of our vaccination rate being so poor,” Smithgall said. “At one point, we were seeing four or five nurse resignations per week. They couldn’t do it again; they emotionally didn’t have it. They were so upset with our community.”
To fill in these growing gaps in their workforce, many hospitals have had to turn to costly contract workers, Rowland reports—a significant financial burden that further strains hospitals’ resources.
For example, Ballad Health went from hiring fewer than 75 contract nurses before the pandemic to 150 in August 2020 and 450 in August 2021. Moreover, according to Smithgall, contract nurses previously made double or triple what permanent staff nurses made, but now Ballad sometimes has to pay up to seven times as much for contract nurses as hospitals compete for workers to fill shifts.
Delayed elective surgeries deepen hospitals’ financial struggles
Many hospitals, including those in areas with high vaccination rates, have delayed elective surgeries, a crucial source of revenue, amid nationwide surges in Covid-19 cases, Rowland reports—further compounding financial struggles for many organizations.
On Aug. 26, Ballad Health postponed a long list of elective surgeries—including hernia repair, cardiac and interventional radiology procedures, joint replacements, and nonessential spine surgery—to preserve space in its hospitals and conserve workers. Ballad is now allowing elective surgeries again, but only for a limited number of procedures that do not require overnight stays.
Similarly, St. Charles Health System in Oregon postponed elective surgeries in August “while we responded to a surge that was significantly greater and much more sudden than the surge in 2020,” Matt Swafford, the health system’s VP and CFO, said.
According to Swafford, the health system lost $5 million a week through August and September, around $1 million of which was repayment of emergency advances on Medicare reimbursements from last year.
“I don’t think anybody saw this level of surge coming in 2021 after what we saw in 2020,” he said. “We’re just not equipped to be able to simultaneously respond to the urgent needs of the community [for more typical surgeries and care] at the same time that a third of our beds are occupied by highly infective Covid patients.”
Many hospitals likely to end the year at a deficit
Further compounding the issue, according to Moody’s Investors Service, is that the provider relief funds that previously made up 43% of operating cash flow at nonprofit and government-run hospitals in the United States are now dwindling down.
In addition, the latest portion of provider relief funds to be distributed must be based on expenses incurred by hospitals before March 31, 2021, which don’t account for months of the delta surge, Rowland reports.
Premier, a group purchasing and technology company serving more than 4,000 hospitals and health systems, analyzed payroll data of 650 hospitals and found that U.S. hospitals have spent a total of $24 billion a year during the pandemic to cover excess labor costs, primarily for overtime and contract nurses. This was an increase of 63% from October 2019 to July 2021, Rowland reports, with hospitals in the Upper Midwest and across the South seeing the largest increases.
“It’s going to leave them huge deficits that they are going to have to work out of for years to come,” Michael Alkire, Premier’s CEO, said.
A $200 surcharge for unvaccinated spouses? It’s coming to one Louisiana health system.

As more companies consider implementing insurance surcharges for their unvaccinated employees, Ochsner Health plans to add a $200 monthly surcharge for employees with unvaccinated spouses and domestic partners covered by the organization’s health plan.
Unvaccinated employees face potential insurance surcharges
While many companies have relied on incentives to encourage employee Covid-19 vaccination, some have recently opted to implement penalties, such as premium surcharges, for those who remain unvaccinated instead.
Recent polling suggests that these surcharges could spur a significant portion of unvaccinated employees to get the Covid-19 vaccine. According to an Affordable Health Insurance poll of 1,000 unvaccinated individuals with employer-based health plans, nearly 75% said a health insurance surcharge could motivate them to get vaccinated, with 43% saying a surcharge would definitely motivate them to get vaccinated.
“As they say, the vaccine is not mandatory, but if people have extra charges with their insurance due to not being vaccinated, people will surely push themselves to be vaccinated,” Nick Schrader, insurance agent at Texas General Insurance, said.
So far, Delta Airlines is the largest employer to implement an insurance surcharge for unvaccinated employees, and it has already seen significant increases in employee vaccination.
In August, Delta announced unvaccinated employees would have to pay a $200 monthly health insurance surcharge to remain on the company’s health insurance plan beginning Nov. 1.
According to Delta, the surcharge will protect the company from lost revenue due to unvaccinated employees being hospitalized with Covid-19—which costs the company an average of $50,000 for each case.
Henry Ting, Delta’s chief health officer, said almost 20% of the company’s unvaccinated employees received the Covid-19 vaccine in the two weeks after the surcharge was announced. In addition, the company did not see any employee turnover or resignation due to the announcement, Ting said.
Ochsner Health’s ‘spousal Covid vaccine fee’
Ochsner Health, Louisiana’s largest health system with nearly 32,000 employees and more than 4,500 physicians, plans to implement a $200 monthly surcharge for employees with unvaccinated domestic partners and spouses on the organization’s health insurance plan, the Associated Press reports.
Ochsner is the first health system to apply insurance surcharges to unvaccinated family members, not just employees. Other Louisiana health care organizations, such as Our Lady of the Lake Regional Medical Center and LCMC Health, said they would ask families of employees to be vaccinated, but did not plan on implementing a surcharge for unvaccinated spouses or partners, the Times-Picayune/New Orleans Advocate reports.
According to a letter sent from Ochsner leaders to employees, the surcharge, called the “spousal Covid vaccine fee,” will begin in 2022 and could deduct up to $2,400 a year from an employee’s paycheck. The surcharge will only apply to domestic partners or spouses, not other dependents covered by an employee’s health plan like children.
Warner Thomas, Ochsner’s president and CEO, said the surcharge for unvaccinated spouses and partners is similar to a surcharge for tobacco users and will be used to help keep health premiums low for employees. As a self-insured organization, Ochsner is responsible for the cost of Covid-19 treatment for patients on its health insurance plan, the Associated Press reports.
“The reality is the cost of treating Covid-19, particularly for patients requiring intensive inpatient care, is expensive, and we spent more than $9 million on Covid care for those who are covered on our health plans over the last year,” Thomas said.
“We know that Covid-19 vaccination dramatically reduces transmission, severity of symptoms, hospitalizations, and death. Approximately 90% of those hospitalized with Covid in our facilities have been unvaccinated since vaccines were approved in December 2020,” he added. “Widespread vaccination is critical to stopping the spread of Covid-19, and we hope this change will encourage even more community members to get vaccinated.”
Thomas also clarified that unvaccinated spouses and partners are not required to be vaccinated because of the surcharge. “This is not a mandate as non-employed spouses and domestic partners can choose to select a health plan outside of Ochsner Health offerings,” he said.
Unvaccinated spouses and partners can also apply for medical or religious exemptions for the Covid-19 vaccine, Thomas said. Currently, around 300 Ochsner employees have applied for medical or religious exemptions, the Times-Picayune/New Orleans Advocate reports.
U.S. hits 700,000 COVID deaths
https://www.axios.com/covid-deaths-700000-us-6dd0223d-562a-41b9-a780-ef54e646b07e.html

The U.S. surpassed 700,000 deaths from the coronavirus on Friday, according to data from Johns Hopkins University.
Why it matters: A summer of division over vaccine and masking mandates only added to the surge in cases caused by the Delta variant. The U.S. went from 600,000 deaths to 700,000 in the span of three-and-a-half months.
- Public health experts have become increasingly frustrated as the “pandemic of the unvaccinated” spread across the country.
- Roughly 70 million eligible Americans remain unvaccinated, AP reports.
Coronavirus vaccine mandates are working — for now
Coronavirus vaccine mandates imposed by employers seem to be working so far, suggesting that most vaccine holdouts would rather get the shot than lose their job, Axios’ Caitlin Owens writes.
Why it matters: Every vaccine helps in our fight against the coronavirus, although the U.S. still has a long way to go.
Driving the news: States with vaccine mandates for health care workers that have taken effect, like California and New York, have seen a large uptick in vaccinations.
- These, of course, are blue states and have higher vaccination rates to begin with. But some health systems in red states, like Texas, have seen similar results when their mandates took effect.
- High-profile mandates outside of the health care sector have also been successful. For instance, United Airlines achieved nearly 100% vaccination among its employees, and Tyson Foods announced that more than 90% of its workers are now vaccinated.
- The Biden administration announced that it will require all employers with 100 or more employees to ensure their workers are vaccinated or tested weekly, but this hasn’t yet been implemented.
Yes, but: Hospitals and long-term care facilities are already stretched so thin that it won’t take a mass exodus for them to feel the effects of layoffs.
- In New York, Gov. Kathy Hochul signed an executive order last week to help provide relief to health systems struggling with staff shortages.
- The Biden administration announced nursing home workers will soon be required to be vaccinated, which could be a much tougher lift. Only about two-thirds of nursing home staff are vaccinated.
What they’re saying: “As we get down to the harder core unvaccinated who are more resistant, what we are seeing is that reality is a more powerful tool to change behavior than information and messaging,” said Drew Altman, president and CEO of KFF.
An unsettling start to the school year
https://mailchi.mp/a2cd96a48c9b/the-weekly-gist-october-1-2021?e=d1e747d2d8

As a long hoped-for sign of the “return to normal”, most children went back to in-person learning this fall. And with the patchwork of COVID safety protocols and masking policies across school districts, classrooms became a learning lab for scientists studying the efficacy of masking and other precautions.
Unsurprisingly, getting a bunch of unvaccinated kids back together caused a surge in pediatric COVID cases. But recent Centers for Disease Control and Prevention (CDC) data from 500 counties demonstrate just how effective mask mandates have been at mitigating outbreaks.
The graphic above shows that cases in counties without school mask mandates increased at nearly three times the rate of those with mask mandates. In the five-week period spanning the start of the school year, cases in counties without a mask mandate rose by 62.6 cases per 100K children, while cases in counties with a mask mandate rose by only 23.8 per 100K. COVID outbreaks are incredibly disruptive to learning; according to a recent KFF survey, nearly a quarter of parents report their child has already had to quarantine at home this school year following a possible COVID exposure.
Even once vaccines are approved for children under 12, recent data suggest that a majority of parents will be hesitant to vaccinate their child. Just over half of 12- to 17-year-olds have received at least one dose of the vaccine so far, and only a third of parents of 5- to 11-year-olds plan to vaccinate their child right away, once the shot is approved.
Many want more information, or are worried about side effects—concerns that will best be assuaged by their pediatricians and other trusted sources of unbiased information.
A new antiviral pill shows promise, as do vaccine mandates
https://mailchi.mp/a2cd96a48c9b/the-weekly-gist-october-1-2021?e=d1e747d2d8

Two pieces of hopeful news on the COVID front this week.
First, pharmaceutical manufacturer Merck announced this morning that molnupiravir, the oral antiviral drug it developed along with Ridgeback Biotherapeutics, reduced hospitalizations among newly diagnosed COVID patients by 50 percent. A five-day course of the drug was so successful in Merck’s clinical study that an independent monitoring group recommended halting the study and submitting the pill to the Food and Drug Administration (FDA) for emergency use authorization. Molnupiravir is activated by metabolism, and upon entering human cells, is converted into RNA-like building blocks, causing mutations in the COVID virus’s RNA genome and interfering with its replication. For that reason, the drug is unlikely to be prescribed during pregnancy, but otherwise the therapy seems to hold great promise in adding to the limited armamentarium available to fight the pandemic. One possible concern: the drug’s price tag. The federal government has agreed to purchase 1.7M courses of the drug at $700 per course, and with most insurance companies having returned to normal cost-sharing for COVID treatments, the drug may be out of reach for some patients. Still, a major clinical development to be celebrated, and more to come as Merck’s drug is vetted by the FDA.
At $20 to $40 per dose, with costs fully absorbed by the federal government, and remarkable effectiveness at preventing severe disease, hospitalizations, and deaths, vaccines remain far and away our best frontline weapon for fighting the COVID pandemic. Promising, then, that the much-debated vaccine mandates have begun to demonstrate success in increasing vaccination rates, even among those who have thus far resisted getting the shot.
Despite concerns about massive staffing shortages among hospitals resulting from the implementation of its mandate, the state of New York found that 92 percent of healthcare workers had been vaccinated by Monday, when the mandate went into effect. That was a 10-percentage-point increase from a week earlier, holding promise that the Biden administration’s planned federal mandate for healthcare workers could have the desired effect.
California’s mandate for healthcare workers went into effect yesterday, and was credited with boosting vaccination rates to 90 percent at many of the state’s health systems. Among private employers considering mandates, the experience of United Airlines may also be instructive: its employee mandate led to the vaccination of more than 99 percent of its workers, resulting in the termination of only 700 of its 67,000 employees. Of course, everyone prefers carrots to sticks, but sweepstakes and bonuses have only gotten so far in encouraging people to get vaccinated—now it appears mandates have a useful role to play as well.
With 56 percent of the population fully vaccinated, the US now ranks 43rd among nations, just ahead of Saudi Arabia and far behind most of Europe. In the next few days we’ll reach the grim milestone of 700,000 COVID deaths in this country—anything that helps stop that number from growing further should be welcome news.


