
Cartoon – Getting Resignation Papers Ready




A collection of provider and payer groups are imploring Congress to continue a moratorium on Medicare payment cuts instituted under the sequester.
The letter (PDF), sent Friday by more than 20 groups to congressional leaders, is concerned that the moratorium installed under the CARES Act expires on Jan. 1. The groups want the moratorium to extend through the COVID-19 public health emergency, which has been renewed by the federal government several times.
The groups said that the moratorium needs to be extended as healthcare facilities are under massive financial stress with new surges of COVID-19.
The surge has impacted the “financial health of medical professionals and facilities, including increased cost of labor to ensure adequate staffing, procurement of personal protective equipment, significant reductions in patient volume resulting from orders to cancel non-emergent procedures and the high cost of caring for COVID patients,” the letter said.
Some of the groups signing on to the letter include the American Medical Association, America’s Health Insurance Plans, Federation of American Hospitals and American College of Physicians.
The groups said that the moratorium on the sequester cuts installed as part of the CARES Act was an acknowledgment from Congress over the important role that Medicare reimbursement plays in “the financial well being of our healthcare system.”
The sequestration cut Medicare payments by 2% across the board to all Medicare providers back in 2013.
The letter comes as Congress is pondering another relief package for COVID-19 during the lame-duck period. Senate Majority Leader Mitch McConnell said after the presidential election that he was open to restarting talks on a new relief package and added that hospitals will need some additional relief.
But McConnell said earlier this week that the same issues that have held up a deal with House Speaker Nancy Pelosi are still there.
“I don’t think the current situation demands a multi-trillion dollar package,” McConnell told reporters. “I think it should be highly targeted.”
But Pelosi has endorsed a larger package. The House passed the HEROES Act, a $3 trillion relief bill, several months ago.

A federal appeals court upheld a ruling that would allow hospitals to calculate their disproportionate share hospital (DSH) payments using Medicaid patients as well as patients eligible for treatment under experimental Medicaid “demonstration projects” approved by the Department of Health and Human Services (HHS).
The opinion, issued Friday, upheld the decision of a lower court that sided with 10 Florida hospitals seeking to include days of care funded by Florida’s Low Income Pool, an approved Medicaid demonstration project. Through the pool, the state and federal governments jointly reimbursed hospitals for care provided to uninsured and underinsured patients.
HHS argued against allowing the hospitals to include those patients in their Medicaid fraction on the ground that the patients were treated out of charity rather than as designated beneficiaries of a demonstration project.
“The district court found the Secretary’s arguments to the contrary unpersuasive. The Secretary argued the text of the regulation allows hospitals to include days of care provided under a demonstration project only if the project entitles specific patients to specific benefit packages,” the judges said (PDF). “As the court noted, however, this is not what the regulation says. Rather, a patient must have been ‘eligible for inpatient services,’ meaning the demonstration project enabled the patient to receive inpatient services, regardless whether the project gave the patient a right to these services or allowed the patient to enroll in an insurance plan that provided the services.”
DSH payments have traditionally been calculated using the costs incurred to treat Medicaid and uninsured patients. However, the Centers for Medicare & Medicaid’s 2017 rule says costs incurred treating other patients are applicable. For example, a dually eligible patient who’s admitted to the hospital will likely have their stay paid for by Medicare, the agency said, as Medicaid is treated as the “payer of last resort.” As such, those costs would be eligible to be subtracted from DSH payouts.
In backing the hospitals on the DSH dispute, the judges pointed to a similar case considered by the Fifth Circuit last year in which the agency sought to exclude from the Medicaid fraction days of care funded through an “uncompensated care pool” created by a demonstration project. That pool reimbursed hospitals in Mississippi for services provided to uninsured patients affected by Hurricane Katrina but did not entitle specific patients to specific services.
In that case, the Fifth Circuit held “plain regulatory text demands that such days be included—period.”
“We see no flaw in Judge Collyer’s analysis and therefore embrace the district court’s opinion as the law of this circuit,” the judges said.

Providence health system reported a $214 loss for the first nine months of the year, as the system continues to recover patient volume that declined during the pandemic.
The 51-hospital not-for-profit system also gave an update on its patient volumes during a recent earnings release.
Providence posted operating revenues of $18.9 billion during the first nine months of 2020, but its operating expenses ballooned to $19.1 billion.
That was an increase of 4% compared to the same period in 2019.
“The increased expenses were largely driven by the higher cost of labor, supplies and pharmaceuticals needed to safely and effectively respond to COVID-19,” Providence said in a release.
But the system is also fighting a major decline in patient volumes.
Hospital systems across the country faced plummeting patient volumes in March and April as COVID-19 spread across the country and facilities were forced to cancel or postpone elective procedures.
But even as patients started to return to the hospital in the spring and summer, volumes continue to be below pre-pandemic levels.
“Year-to-date volumes as measured by case mix adjusted admissions were 10% lower than the same period last year,” Providence said.
But a bright spot for the system has been its pivot to virtual care.
“We’ve dramatically ramped up virtual care and are on track to log 1.4 million video visits by the end of the year,” said Providence President and CEO Rod Hochman, M.D.
The income loss also comes as Providence recognized $682 million in relief funding as part of a $175 billion fund passed by Congress as part of the CARES Act.
Providence also got help from a recovering stock market.
The system posted year-to-date, non-operating income of $263 million during the first nine months of the year, compared with $772 million during the same period in 2019.
“Non-operating income helps to recoup reimbursement shortfalls from Medicaid and Medicare coverage, allowing us to serve vulnerable populations while balancing our financial standing,” Providence said.

The Federal Trade Commission (FTC) filed a lawsuit to stop Memphis, Tennessee-based Methodist Le Bonheur Healthcare’s $250 million acquisition of two hospitals in the area owned by Tenet Healthcare.
The agency said in the federal lawsuit filed Friday that the acquisition of two Memphis-based hospitals known as Saint Francis would imperil competition in the area.
Competition would dampen for a “broad range of inpatient medical and surgical diagnostic and treatment services that require an overnight hospital stay,” the FTC said in a release Friday. “If the proposed acquisition is consummated, healthcare costs will rise.”
FTC said only four hospital systems provide general services to the area. If the deal goes through, the new health system would control approximately 60% of the Memphis market.
“It’s clear that patients in the Memphis area have benefited from the competitive pressure that Saint Francis brings to bear on Methodist, through lower rates, more options for insurers and patients, and quality improvements,” said Daniel Francis, deputy director of the FTC’s Bureau of Competition, in a statement.
FTC is seeking a preliminary injunction to halt the deal until completion of a trial next year.
This is the latest move by the FTC to combat hospital mergers. Last year, the FTC launched a probe into the effects of health system mergers on prices and healthcare quality.
Methodist and Tenet said in a joint statement they are reviewing the lawsuit and were bewildered by the move.
“We are surprised by the FTC action given the strong support for the transaction by local stakeholders, including leading local health plans, physicians, employers and community leaders,” the statement said.
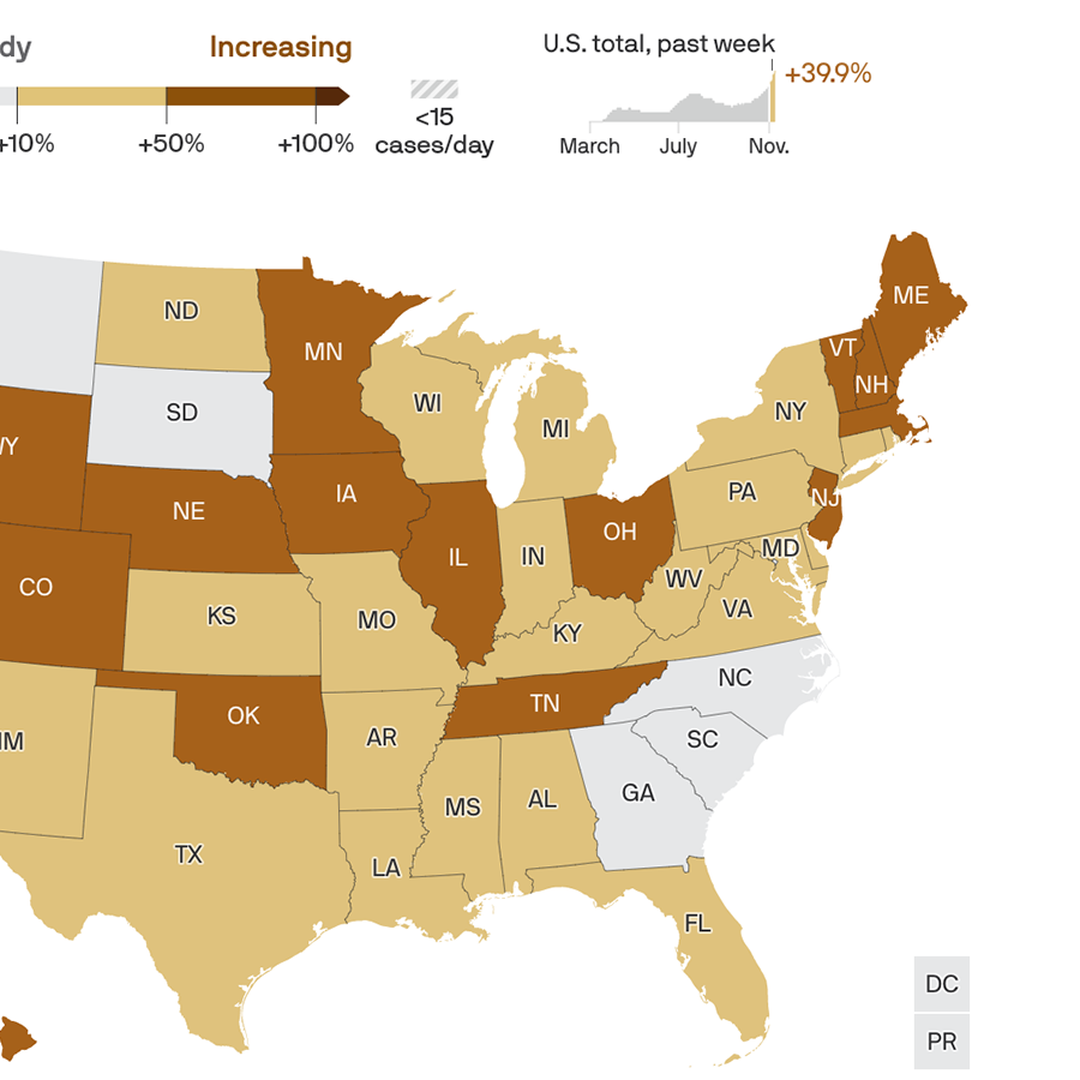
No state in America could clear the threshold right now to safely allow indoor gatherings, Axios’ Sam Baker and Andrew Witherspoon report.
The big picture: This is bad as the pandemic has ever been — the most cases, the most explosive growth and the greatest strain on hospitals.
By the numbers: Over the past week, the U.S. averaged more than 154,000 new cases per day, the highest rate of the entire pandemic.
Between the lines: Whatever metric you might use to decide whether it’s safe to have a large Thanksgiving get-together, or to sit inside a bar or restaurant, the answer is probably no.
The bottom line: Eating and drinking indoors with large groups of people, at a time when 150,000 people are contracting the virus every day, is about as risky as it gets.
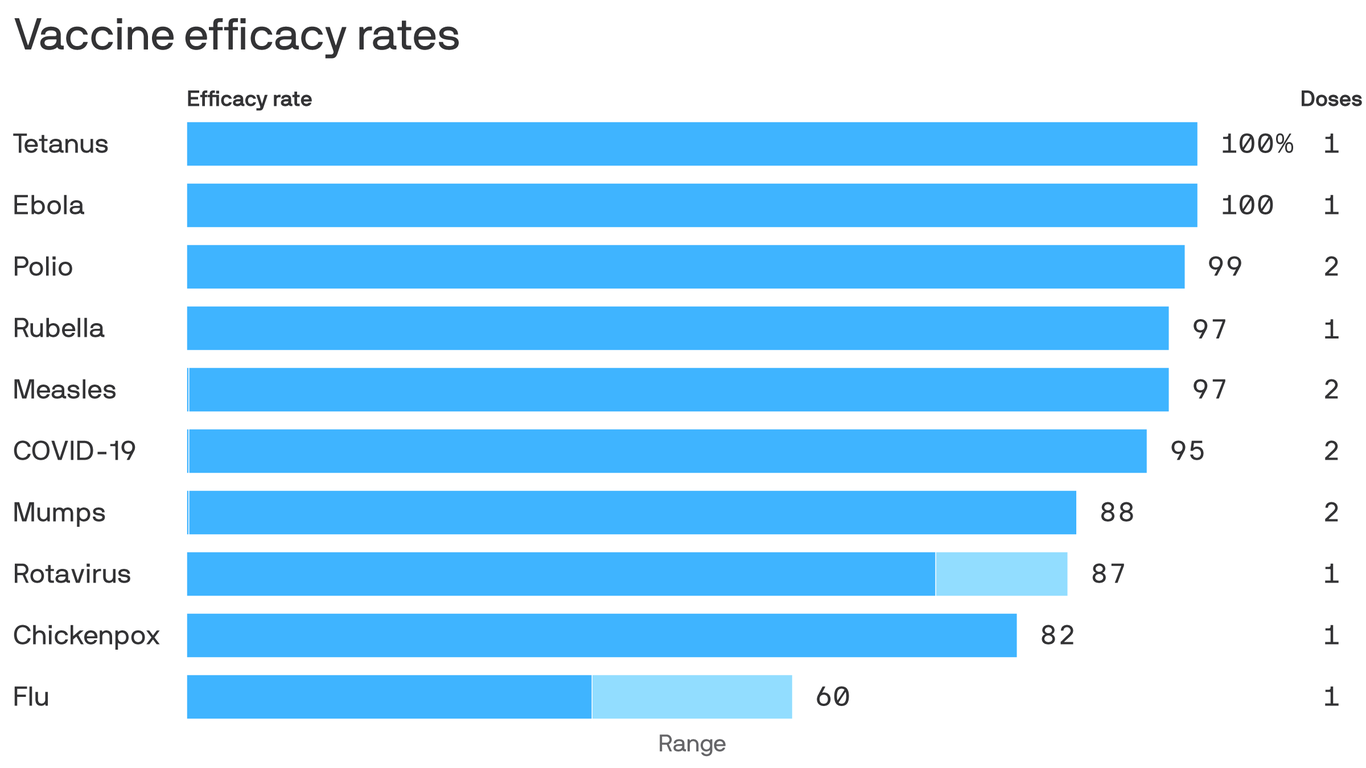
The leading coronavirus vaccines are shaping up to be on par with some of the most effective vaccines in medicine, Axios’ Marisa Fernandez reports.
Why it matters: Vaccines with efficacy rates of about 95% — which both Pfizer and Moderna say they’ve achieved — will be more powerful weapons against the coronavirus than many experts had anticipated.
Flashback: The Food and Drug Administration initially set the bar for a COVID-19 vaccine at 50% efficacy, roughly in line with the seasonal flu vaccine.
But coming in closer to 95% would put Pfizer and Moderna’s vaccines more in line with the highly effective inoculations against measles, mumps and rubella.
Yes, but: There’s still a lot we don’t know about these vaccines, including how well they’re likely to work among various demographic groups, and how long the immunity they confer will last.

