The Democratic argument over health care is beginning to get heated, which unfortunately means that things are becoming more problematic. In fact, the candidates making what is arguably the most sensible policy choice are justifying it with some absolutely abominable arguments — arguments that should warm the heart of the Republican Party.
Right now there’s a divide within the party, with some of the presidential candidates including Bernie Sanders and Elizabeth Warren supporting single payer (though Warren hasn’t been specific), and most of the others including Joe Biden, Amy Klobuchar and Pete Buttigieg suggesting some form of public option that would be voluntary, not Medicare For All but Medicare For All Who Want It.
I’ve come to believe that for all the benefits of a single payer system, trying to move immediately to one is a task with such overwhelming political obstacles and policy complications that it’s probably a better idea to achieve universal coverage through a dramatic expansion of public insurance while, for the moment, leaving substantial portions of the private system intact, even if that’s in many ways distasteful. I realize many readers will disagree with that, which is fine; we should continue to debate it.
But let’s at least grant that it’s a reasonable position to take. The problem with what’s happening now is that some advocates of the public option approach are sounding a lot like, well, Republicans.
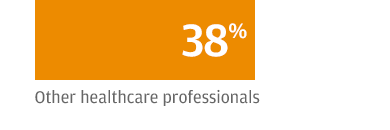
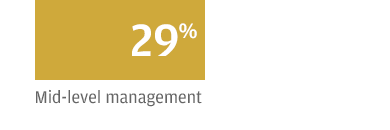
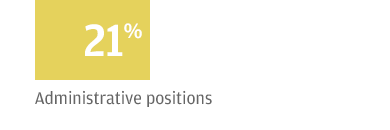
Their most common talking point when defending their plan is some variation of “We can’t kick 150 million people off their insurance,” referring to the number of people who are covered by employer plans:
- “We should have universal health care, but it shouldn’t be the kind of health care that kicks 150 million Americans off their health care,” says John Delaney.
- Beto O’Rourke says Medicare-for-all “would force 180 million Americans off their insurance.”
- “I am simply concerned about kicking half of America off their health insurance within four years, which is what [Medicare-for-all] would do,” says Amy Klobuchar.
The generous interpretation of this line is that it’s warning about widespread disruption; the other interpretation is that it’s meant to stoke the fear that if you now have coverage and single payer passes, you could be left with no insurance at all, which is just false. If we passed single payer, you’d move from your current plan to a different plan, one that depending on how it’s constructed would probably offer as good or better coverage at a lower cost.
The further danger is that that kind of talk inevitably leads one toward the promise that got Barack Obama into such trouble, “If you like your plan, you can keep it.” In fact, here’s O’Rourke saying that under his plan, “For those who have private, employer-sponsored insurance or members of unions who have fought for health care plans … they’ll be able to keep that.” And here’s Biden saying much the same thing: “If you like your health care plan, your employer-based plan, you can keep it. If in fact you have private insurance, you can keep it.”
Haven’t they learned anything?
While there may be political value in communicating to people that a public option would be voluntary, we have to tell them the truth, which is that if you’re going to open it to employers and not just individuals, some people will be moved to the public plan whether they want to or not, since their employers will make that choice for them. That’s how employer coverage works: What plan you’re on is seldom up to you, it’s a decision made by your employer.
And the broader truth is that no one, I repeat, no one gets to keep their plan if they like it even under the status quo. “If you like your plan, you can keep it” is a fantasy. If you have insurance through your employer, you’ve probably had the experience of your employer changing insurers or changing plans; many do it every year. Sometimes the new plan is better; often it’s not. But if you liked your plan, you didn’t get to keep it.
That’s even true of people on public insurance plans, though to a far lesser degree. Medicare and Medicaid go through changes, and benefits are added or taken away. It’s not up to you.
The trouble is that we have a situation where change is constant yet everyone is afraid of change, which makes it awfully tempting to encourage that fear. But the more we propagate the fiction that Americans, especially those with private insurance, aren’t vulnerable under the current system, the easier it will be to crush any reform effort.
Apart from the praise of the Affordable Care Act, this video could almost have been scripted by the Republican National Committee, with its paeans to private health insurance. Of particular note is the woman’s explanation of how she and her husband “earned” health coverage through decades of work, which implies that health care is not a right, as most Democrats believe, but a privilege one has to earn.
To top it off, Biden’s caption to the video says that “Because a union fought for their private health insurance plan, Marcy and her husband were able to retire with dignity and respect,” which is why Biden wants to let them stay on their existing insurance.
Let me suggest a crazy idea: What if retiring with dignity and respect wasn’t something you only got if you were lucky enough to be represented by a union (as a mere 1 in 10 American workers is, and 1 in 16 private sector workers), and only if that union happened to be successful in its fight to get you health benefits? What if everybody got dignity and respect? Isn’t that the world Joe Biden is trying to create?
You can make a strong case for both a single payer plan and one built around a public option. But please, Democrats, when you’re arguing for your preferred solution, don’t undermine the entire philosophical approach your party takes to health care. That only makes the job of reform more difficult.