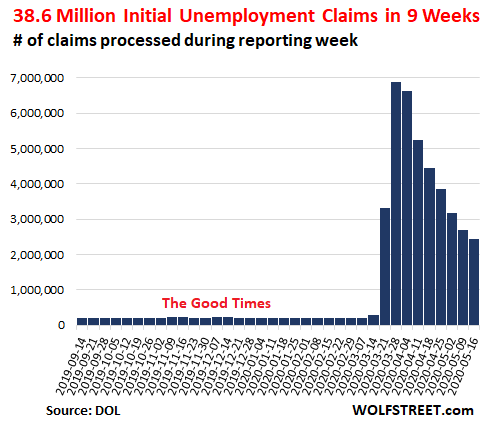
Our ability to access nutritious food is a critical factor to our health and well-being, which is why it has been alarming to see images in recent weeks of cars lining up by the thousands at food banks across the country. Indeed, a university survey taken since the onset of the crises found nearly 4 in 10 Americans reported having moderate to high levels of food insecurity, compared to 11 percent of households who were food insecure in 2018, according to the USDA Economic Research Service.
In response, the federal government has given states administrative relief and funding through various Covid-19 response packages. USDA also has authorized temporary waivers that grant states greater flexibility to address the increased demands and to align with shelter-in-place and social-distancing orders.
USDA also created two new programs: the Pandemic EBT (P-EBT) and the Coronavirus Food Assistance Program (CFAP). P-EBT allows states to issue eligible households an EBT card, a type of debit card used to purchase food, with the value of the free school breakfast and lunch reimbursement rates for the number of weekdays that schools are closed due to Covid-19 (estimated to be around $5.70 per day).
As of the first week of May, 18 states have been approved to provide benefits through P-EBT and 20 additional states have submitted plans for approval. CFAP aims not only to assist families in accessing food but also ranchers and farmers who have an excess supply. Through CFAP, the USDA will procure an estimated $100 million per month of fresh fruits and vegetables and $300 million per month in dairy and meat products for food banks and other nonprofits providing food to Americans in need.
Are these measures enough? Let’s examine the changes, particularly the USDA waivers for the federal food assistance programs.
The Supplemental Nutrition Assistance Program (SNAP), formerly known as food stamps, provides financial support to supplement the food budget of needy families. USDA waivers that increased flexibility in the administration of SNAP include:
- waived the requirements for in-person interviews during the SNAP enrollment process,
- provided emergency supplementary benefits up to the maximum benefit a household can receive for up to two months,
- removed the requirement for SNAP recipients to re-certify midway through their participation,
- provided flexibility for jobless workers to remain eligible, and
- expanded the SNAP online grocery purchase pilot from the original eight states adding an additional 12 states and the District of Columbia.
These efforts are a step in the right direction to ease family burdens, but the supplemental benefits and program flexibilities are time-limited by the federal public health emergency declaration for Covid-19. Also, the 40 percent of SNAP households who already receive the maximum benefit are excluded from the supplemental benefits. Especially as we are experience the sharpest increase in food costs in decades, we need to provide additional support to the lowest income SNAP recipients. To assist families during the longer economic recovery, advocates and policy experts are calling for the following expansions to ensure these benefits cover a larger share of the people who need them:
- boost the benefit for households by 15 percent (an additional $25 per person per month),
- increase the minimum benefit per month from $16 to $30, and
- suspend implementation of all administrative rules that restrict access for millions of Americans.
The Supplemental Nutrition Program for Women Infants and Children (WIC), a public health nutrition program that provides nutrition education, breastfeeding support and nutritious foods to low-income pregnant women and mothers of small children, has been providing services remotely. USDA waivers that increased flexibility in the administration of WIC include:
- waived requirements for the physical presence for certification,
- waiver for deferment of measurements and blood tests,
- ability to issue benefits remotely, and
- food package substitutions.
That’s a good start and more can be done. The Center on Budget and Policy Priorities recommends temporarily extending WIC certification periods for infants to two years as well as extending WIC eligibility from age five to age six. The National WIC Association is also advocating for an increase in the Cash Value Benefit to enhance fruit and vegetable purchases by WIC families.
The National School Lunch Program (NSLP) and Breakfast Programs, Summer Food Service Program, and the Child and Adult Care Food Program (CACFP), which serve low-income school children, quickly revamped and developed innovative ways to distribute meals to families, often expanding their regular productions. USDA waivers that increased flexibility to help better serve families during the pandemic include:
- ability to serve non-congregate meals,
- allowing for pick-up and delivery of meals,
- allowing modification in the meals components requirements,
- waiving time elements and meal spacing requirements,
- allowing virtual desk enrollment of new CACFP providers, and
- waive requirement that afterschool meals and snacks be accompanied by educational activities.
CACFP provides meals to preschool-aged children in Child Care Centers and licensed child care family homes. During the pandemic, most centers have been closed, while a majority of family homes remained open and provided services for essential workers.
According to Paula James, director of child health and nutrition at CocoKids in northern California, about 68 percent of the Contra Costa county’s family homes participating in CACFP remained open in April, and these waivers were helpful. Moving forward, she believes CACFP should continue the allowance of virtual enrollment and expand the use of that technology to regular monitoring site visits, specifically in rural areas or locations where safety could be a concern. While the pandemic has provided the opportunity to test technological advances that could streamline program operations in the future, it also revealed some systemic weaknesses, including that CACFP has no centralized database system, which is needed at the state level and requires federal guidance. Lack of technology throughout the program was a hinderance to providing additional services to families during COVID-19. “Continued use of technology into the future will be very important,” said James.
What more can be done? The federal government should extend COVID-19 related waivers for all nutrition programs until September 30, the date provided by congressional authority. While the public health restrictions may be lifting across the states, the economic fallout will likely be felt by families for many months to come.
In addition, states should leverage communication, technology, all federal supports, and evaluation to ensure they are successfully reaching as many in need as possible. This includes:
- conducting a public information campaign to alert newly unemployed families in need about available food assistance programs and how to apply and access benefits;
- utilizing technology solutions to provide remote program services and enrollment including mobile uploading of required documents;
- taking advantage and apply for all available waiver options from the federal government; and
- evaluating the revised work systems and if appropriate, take actions to allow for permanent program changes.
This week House Democrats passed the Health and Economic Recovery Omnibus Emergency Solutions (HEROES) Act, the fifth Covid-related legislative package, which includes a boost in funding for SNAP, WIC, and Child Nutrition Programs. The bill also provides support to local food banks and emergency food providers. Any bill that goes to the president should include these food access supports.
It is critical to strengthen federal food assistance programs and the social safety net while working to address the root causes of poverty to reduce health and social disparities. To learn how Altarum can assist your state in program assessment, planning, evaluation, training and analytic support for quality services, contact Tara Fowler, PhD, director of the Center for Healthy Women and Children, at tara.fowler@altarum.org.