The health of a community is measured by the health of its individual members, and the health of its members depends on their access to local, high-quality medical care. Health coverage is a key indicator of the health and wellness of an individual. When people have health insurance, they have greater access to care, reduced mortality, and better health outcomes, according to a report from the American Hospital Association.
However, the current approach taken by some of the nation’s largest health insurers, or payers, is putting this at jeopardy as payers focus on profits and quarterly earnings, strip rates and put the long-term viability of health systems at risk. With hospitals in the middle of the worst economic performance in decades, it is time for payers to own up to how their actions negatively impact the communities and those they claim to serve.
As a physician and the chief of population health at a large metro-area health system, Northeast Georgia Health System, my patients’ ability to readily access medical care at our facilities — and have that care be covered by insurance — matters greatly. Any disruption in a patient’s experience, such as restricting access to care by their health plan or going out of network with an insurance company, can wreak havoc on population health. It’s no secret that many health systems across the country have felt the weight of increased administrative and contractual burdens from health insurers as denial rates continue to creep upwards.
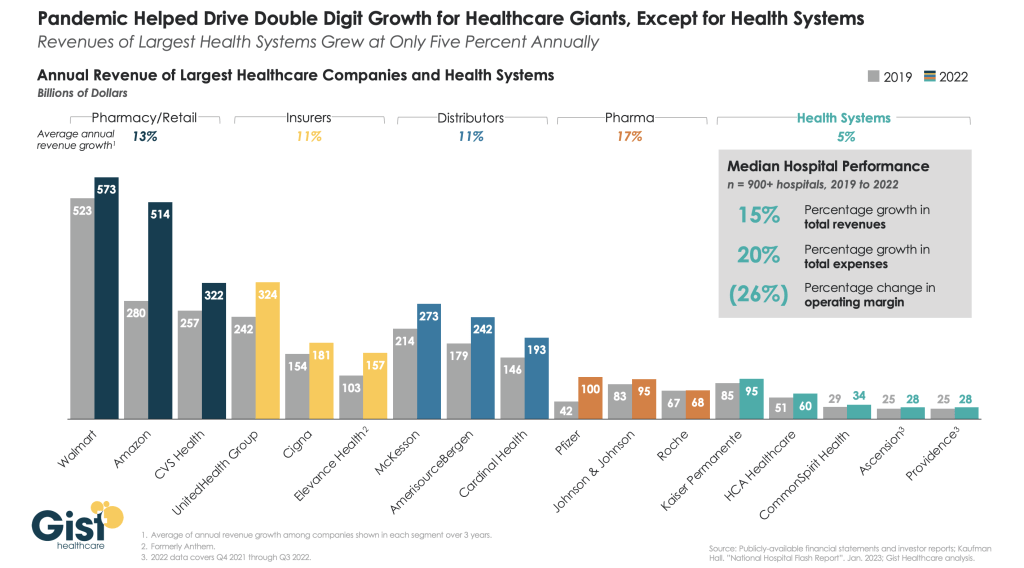
Health insurance companies, like the nation’s largest, UnitedHealthcare, have seen profits soar in recent years. UnitedHeatlhcare’s profits were up 28 percent during the third quarter of 2022 – achieving a profit of $5.3 billion in just those three months – before closing the year at $28.4 billion in net earnings in 2023. Elevance (formerly Anthem), Cigna, and Aetna have also posted record profits recently.
We have seen the impact of the pressure payers are putting on hospitals across the country. Nearly 200 hospitals have closed since 2005, according to the Sheps Center for Health Services Research at the University of North Carolina. Many of these hospitals have closed because they failed to receive fair contracted rates from large payers and thus were insolvent.
Community benefits like charity care, health education and economic impact are provided by hundreds of hospitals nationally, but that impact is at risk if they are not fairly compensated for the services they provide.