https://www.axios.com/2025/06/18/hospital-purchasing-tariffs-trump-ppe
Tariffs and supply chain uncertainty are playing havoc with hospitals’ purchasing plans, especially for lower-margin products like gloves, gowns and syringes.
Why it matters:
The uncertainty is in some cases delaying spending decisions, including capital improvements, as health system administrators wait to see the effect of increased duties and whether manufacturers win exemptions from the Trump administration.
What they’re saying:
“Hospitals are definitely feeling a pinch,” Mark Hendrickson, director of Premier’s supply chain policy, told Axios. “We’ve never seen tariffs for this long a period of time for this broad a portfolio of products in basically all of our lifetimes.”
- “It’s really an uncertain enough environment that we’re cautioning members from panic buying and buying ahead,” he added. “We don’t want to drive artificial shortages of products that could be avoided.”
The big picture:
The health care supply chain is already hard enough to navigate, with certain sterile injectable drugs and other essentials regularly going into shortage.
- But President Trump’s existing and threatened tariffs are scrambling the calculus for health systems and the group purchasing organizations they contract with, as they seek a steady supply of what they need and identify possible new sources.
- “Everyone in the supply chain, from hospitals to suppliers to manufacturers, is grappling with how to plan thoughtfully and proceed in a way that doesn’t either under- or over-correct for the potential impacts of these tariffs,” Akin Demehin, the American Hospital Association’s vice president of quality and patient safety policy, told Axios.
Between the lines:
So far, there haven’t been clear price hikes or shortages.
- But certain types of products are being watched more closely, starting with low-cost, high-volume items often imported from China such as PPE and disposable medical devices.
- “Are there going to be instances where those low margin products are just not worth manufacturing anymore?,” Hendrickson said.
U.S. manufacturing of protective gear picked up during the pandemic, to alleviate foreign supply chain disruptions. But some of those sources dried up with the end of mask mandates and other public health measures, when hospitals went back to buying from overseas.
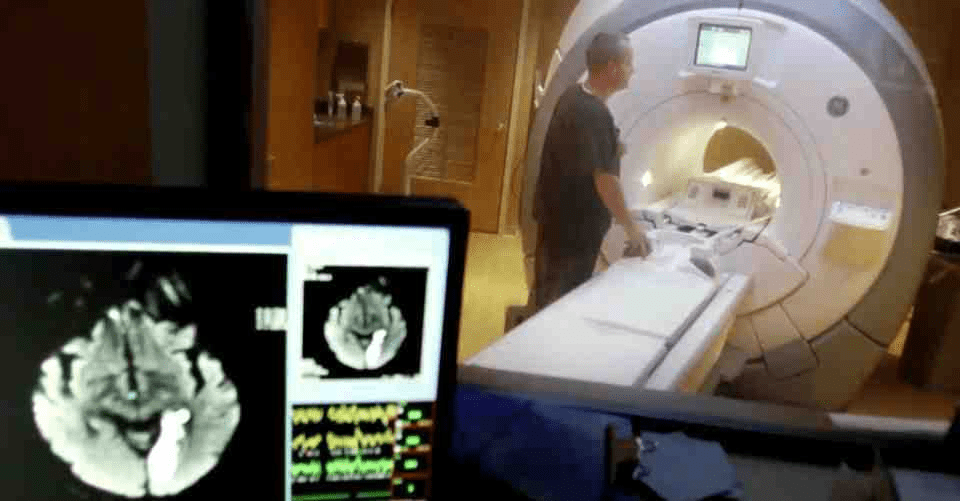
- The hospital association is particularly concerned about critical minerals and derivatives used in medical imaging, radioactive drugs and other applications, which could be subject to sectoral levies imposed in the interests of national security.
- Last month, the AHA sent a letter to the Trump administration calling for medical exemptions.
The bottom line:
“We haven’t seen the bottom fall out,” Hendrickson said. “I’m hoping we don’t.”