
Cartoon – The Team needs Leadership
How the supply chain crisis is worsening the workforce crisis
https://mailchi.mp/7788648545f0/the-weekly-gist-february-25-2022?e=d1e747d2d8

In our recent conversations with executives, we’ve heard that the workforce crisis continues to be the most urgent issue confronting health systems.
It’s a many-sided problem: early retirements hitting the nursing staff, leading to an overall loss of experience; early and mid-career nurses choosing to work for temporary staffing agencies for much higher pay, resulting in increased labor costs and resentment among remaining nurses; and a rising vacancy rate made more challenging by difficulty competing for talent against others offering higher pay and less stressful work environments.
But one factor undermining frontline nurse engagement hadn’t occurred to us, until we heard a chief nursing officer describe it this week. The lingering supply chain crisis is forcing hospitals to change where they purchase basic items—think IV tubing and bags, surgery kits, some basic drugs—which in turn forces nurses to adapt to using unfamiliar supplies on the fly, making for a less predictable work environment. On a busy and staff-constrained nursing unit, even small changes to standard procedures can be incredibly frustrating for nurses, and even lead to patient safety issues. Just another way in which the current environment is creating unprecedented pressure on healthcare workers, with little prospect for improvement anytime soon.
What is an insurance company in 2022?
https://mailchi.mp/7788648545f0/the-weekly-gist-february-25-2022?e=d1e747d2d8
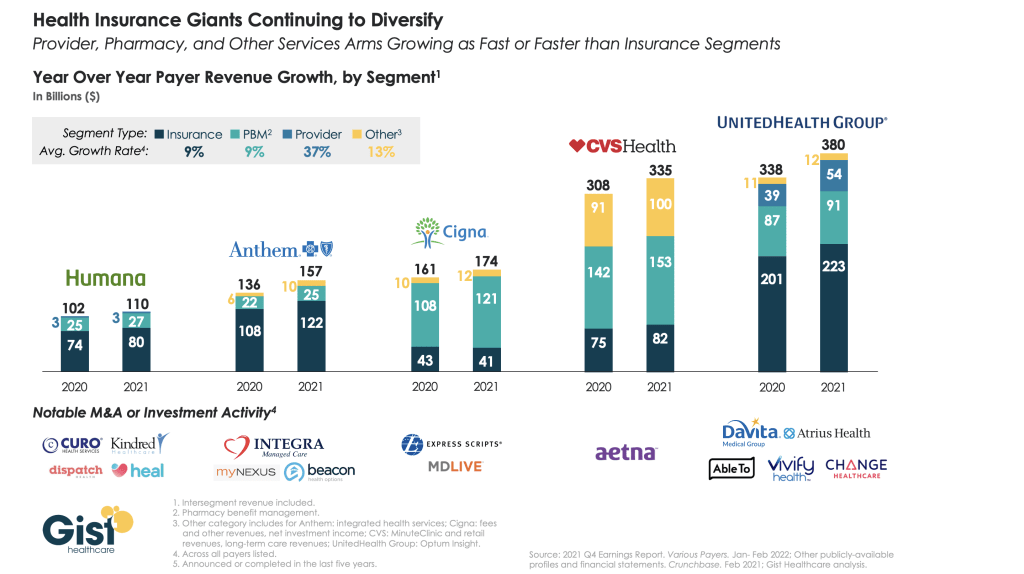
The largest health insurers are quickly becoming vertically integrated healthcare organizations that span the care and coverage continuum. While 2021 was a mixed year for these companies as healthcare volumes bounced back, their diversified portfolios helped cushion losses from higher claims.
The graphic above analyzes revenue growth by segment for the five largest insurers across the last two years. On average the insurance and pharmacy benefit management components of the companies grew at nine percent, while care delivery and integrated health services grew at much higher rates. UnitedHealth Group (UHG) and Anthem boasted the highest year-over-year revenue growth, driven by UHG’s Optum subsidiary and Anthem’s integrated health services.
Cigna and CVS Health each earned less than a quarter of their total revenue from their insurance arms last year. While Humana lags the others in topline revenue, it has assembled a robust portfolio of care delivery investments and partnerships, surpassed only by UHG.
As antitrust scrutiny on vertical integration increases (case in point: the DOJ is now challenging UHG’s acquisition of Change Healthcare), insurers will face the hard task of integrating their portfolio of service—and demonstrating that they deliver value to consumers and patients.
As America’s physician demographics shift, so do doctors’ priorities
https://mailchi.mp/7788648545f0/the-weekly-gist-february-25-2022?e=d1e747d2d8
A recent New Yorker article details the history of the American Medical Association’s (AMA) opposition to single-payer healthcare, and the grassroots movement that nearly changed its position in 2019.
Since its founding in the 1840s, the largest association of the nation’s doctors has wielded significant influence over healthcare policy, and has been the most effective opponent of several waves of progressive healthcare reform proposals across the last century. More recent changes in the demographic makeup of its physician constituents have begun to mirror the US population. A quarter of today’s practicing physicians graduated from foreign medical schools, and gender and racial gaps in medical schools have been reduced. Today, half of medical students are female, and half are people of color.
The Gist: The perspectives, needs, and politics of the physician community are changing. Younger physicians tend to be more left-leaning, and more are employees, rather than entrepreneurial business owners. While physician pocketbook issues historically dominated the AMA’s policy positions, today’s younger physicians are increasingly motivated by social justice concerns, leading to advocacy positions that would have been unimaginable a few decades ago.
Physician societies continue to move closer to endorsing more extensive healthcare reform policies, over trying to ensure economic protection for the profession—and in the long run, this shift in physician support could prove a key driver in increasing public approval of “Medicare for All” and other coverage reforms.
Hospitals avoid feared staff exodus after COVID vaccine mandate implementation
https://mailchi.mp/7788648545f0/the-weekly-gist-february-25-2022?e=d1e747d2d8

The February 14th deadline for healthcare workers to receive their first dose of the COVID vaccine does not appear to have significantly worsened the hospital staffing crisis, even in rural hospitals. But the mandate hasn’t necessarily meant that all healthcare workers are now vaccinated, as some hospitals reported approving a flurry of medical and religious exemptions to avoid staff departures.
The Gist: Just as when states and early-adopter health systems enforced healthcare worker vaccine mandates last year, COVID vaccine uptake jumped just ahead of the federal deadline.
After months of challenges, we may finally be moving beyond debates over healthcare worker vaccine requirements. And as hospitalizations from the Omicron wave continue to decline, most states and health systems are not planning to implement booster requirements.
Department of Justice (DOJ) files suit to block UnitedHealth Group (UHG)’s $13B acquisition of Change Healthcare
https://mailchi.mp/7788648545f0/the-weekly-gist-february-25-2022?e=d1e747d2d8

DOJ alleges that allowing UHG’s Optum subsidiary to acquire Change, a direct competitor used by most large commercial insurers for healthcare claims solutions, would give UHG 75 percent of the healthcare claims processing and management market. This would significantly reduce competition, the DOJ claims, while simultaneously giving UHG access to its competitors’ sensitive plan design and pricing information. UHG called the DOJ’s position ‘deeply flawed’ and promised to fight the case.
The Gist: This is the second big move by antitrust regulators in a week to put the brakes on consolidation in healthcare: shortly after the DOJ sued to block Rhode Island’s two largest health systems, Care New England and Lifespan, from merging, those systems abandoned plans to combine.
We are seeing the first real signs that the Biden administration is following through on plans to more closely scrutinize healthcare deals, including payer-led vertical integration. For both payers and providers, increased scrutiny will place a premium on the consumer value proposition of any combination—and force merging companies to deliver on the benefits of scale.
Centers for Medicare and Medicaid Services (CMS) overhauls the Direct Contracting payment model
https://mailchi.mp/7788648545f0/the-weekly-gist-february-25-2022?e=d1e747d2d8

On Thursday CMS announced it will replace all versions of its Global and Professional Direct Contracting (GPDC) model, which allowed primary care providers to take full or partial risk on managing cost of care for traditional Medicare beneficiaries, after progressive Democrats raised concerns about whether a growing presence of Medicare Advantage insurers and private equity-backed groups in the model might compromise patient care and access in the traditional Medicare program. GPDC will be replaced with a new three-year demonstration called Accountable Care Organization Realizing Equity, Access and Community Health (ACO REACH), to start enrollment in 2023. The 51 current participants in the GPDC model can move into ACO REACH as long as they meet new requirements, which include developing plans to identify and address health disparities, and ensuring providers control three quarters of governing boards (as compared to a quarter in the GPDC model). Private equity and insurer applicants can still apply, but must demonstrate a track record of direct patient care, delivering quality outcomes, and serving vulnerable populations.
The Gist: ACO REACH is largely a “re-skinning” of the Direct Contracting program, rather than a significant overhaul. Physician, health system, and ACO groups, who were concerned that the program would be canceled altogether, were pleased with the announced changes to the model, although debate continues on whether the new guardrails will effectively address concerns around for-profit insurer and investor participation.
Like Direct Contracting before it, ACO REACH will be an important vehicle for risk-ready providers to move more extensively into full-risk contracting, without launching a plan or partnering directly with a MA insurer.
Question of the Day: What is Salary?
Oklahoma Hospital Locks Down Its ICU Following Threats to Staff

Healthcare professionals in Oklahoma who have cared for COVID-19 patients throughout the pandemic are now facing a facility lockdown due to threats made against them.
Mercy Hospital Oklahoma City upped its security and locked down its intensive care unit following online threats against the facility and its staff, mostly revolving around COVID treatments and conspiracy theories, Becker’s Hospital Review reported.
Claims made during a recent protest outside the facility and online included that the hospital had a “Fauci protocol,” and that it received government vouchers for using certain medications or treatments for COVID patients, which Mercy Hospital denied, according to Becker’s.
Hospital officials released a statement to staff on Friday, which they shared with MedPage Today. “There is truly nothing more important to us than your safety. We have a team monitoring these online attacks in real time. Every level of our ministry is deeply concerned and committed to doing whatever it takes to protect our co-workers against these baseless attacks,” they said.
“We are proud to serve with you,” they added. “We know you are tired and weary, but please try your best to put these baseless claims out of your mind. Remember, you are called to serve our patients and each other. We are praying for peace and protection over each of you, as well as the protection of all our patients and visitors, while we take action on your behalf.”
Late last week, the hospital filed a restraining order against the founder and director of an Oklahoma church group that has been protesting outside the facility and making threats against its staff online, Oklahoma’s KFOR reported.
In a recent press release, the church group, known as Ekklesia Oklahoma, called Mercy Hospital an “evil Marxist controlled death camp.”
Court documents stated that the founder of the group called one of the hospital’s doctors a “murderer,” noting that members even posted the doctor’s home address online, according to KFOR.
Hospital officials told KFOR that they are thankful for local police departments that are providing extra security for staff and patients.
Other hospitals across the U.S. have also received threats to the safety of healthcare workers in recent days.
Last week, the Massachusetts Medical Society said it was “angered” over the recent neo-Nazi protest outside Brigham and Women’s Hospital in Boston that targeted two doctors whose work focuses on health equity.
Carole Allen, MD, MBA, president of the society, told MedPage Today that the protest outside Brigham and Women’s was a threat to healthcare workers who were just trying to do their jobs, as well as to patients, and was so disruptive that it “could endanger healthcare in general.”



