

https://www.commonwealthfund.org/blog/2019/rhode-island-most-improved-state-health-performance

States use the Commonwealth Fund’s 2019 Scorecard on State Health System Performance to identify places where their health care policies are on track and areas that need improvement. Using the Scorecard, states can compare their improvement to others, and see how they stack up. In the most recent edition, released in June, Rhode Island improved on the most health system performance indicators tracked over time, followed by Missouri, Washington, West Virginia, and Arkansas.
Rhode Island particularly made strides in the areas of coverage and behavioral health. The state uninsured rate among adults dropped from 17 percent in 2013 to 7 percent in 2015 and 6 percent in 2017. In addition, the percentage of adults with any mental illness reporting an unmet need dropped from 27 percent in 2010–11 to 18 percent in 2014–16. The state also saw significant reductions in the percentage of children with unmet mental health needs.
These improvements did not happen by chance. What actions did policymakers take to drive progress and what work lies ahead?
In 2014, Governor Gina Raimondo came into office fully committed to the Affordable Care Act, including Rhode Island’s state-based health insurance marketplace and expanded Medicaid eligibility.
Another early administration priority was making sure behavioral health care was as available and affordable as medical care. The opioid epidemic was hitting Rhode Island hard, making access to treatment for mental health and substance use disorder a top concern.
Coverage expansion. The decision to create a state-based marketplace, HealthSource Rhode Island (HSRI), was instrumental in helping the state make gains in coverage and affordability. The state has its own funding for marketing and navigators who help people understand and choose health plans. This has helped shield residents from federal outreach cuts. The state’s commitment also helped when the Trump administration decided to end marketplace cost-sharing-reduction subsidies. The state’s Office of the Health Insurance Commissioner (OHIC) worked with the state marketplace HSRI to protect consumers by building price increases to cover the loss of subsidies into silver-level health plans and keeping premiums lower in the other plans. HSRI plans offered among the lowest state-based marketplace premiums in the country. During last year’s open-enrollment period, HSRI saw a 5 percent increase in new and overall customers.
Access to behavioral health. In 2015, Governor Raimondo issued an executive order to establish the Overdose Prevention and Intervention Task Force, which has guided state reforms. The opioid crisis also has led to more open conversations about mental health and to improved relationships between first responders and communities. To facilitate these relationships, Rhode Island now requires police officers receive training to recognize behavioral health issues and help connect individuals with the care they need.
Rhode Island experienced a decline in overall overdose deaths, from 336 in 2016 to 314 in 2018. Community programs and pharmacies have worked hard to get naloxone, used to counter the effects of opioid overdose, into the hands of people who need it. Rhode Island was also the first state to offer medication-assisted opioid treatment in prison. Community health workers follow up on inmates after release to ensure treatment is continued. Fatal overdoses declined by 60 percent among people leaving detention from 2016 to 2017, and continued to drop in 2018.
OHIC also has prioritized integrating behavioral health into the primary care setting as a cost-effective way of increasing access to such services. Studies have shown that integrated care improves depression and anxiety outcomes, along with quality of life, while reducing the total cost of care.
Additionally, OHIC has been working on encouraging parity between medical and behavioral health in the insurance market by reviewing insurers’ coverage documents. It is focusing on limiting mental health benefit exclusions and ensuring the states’ major carriers are in compliance with the laws related to coverage for mental health and substance use disorder treatment. As a result, the four major insurers have agreed to discontinue prior authorization requirements for certain medication-assisted treatments.
In 2018 an HSRI/OHIC workgroup was formed to develop policy options to mitigate the potential impact of federal changes on health coverage costs, consumer choice, and access. The group recommended pursuing a Section 1332 waiver to establish a reinsurance program to reduce premium increases in the individual market; implementing a state-level requirement that individuals have health insurance to offset the impact of the federal health insurance mandate penalty repeal; and establishing OHIC’s regulatory authority over short-term limited duration plans. All three recommendations were signed into law on July 5.
In addition, recent state legislation has expanded OHIC’s authority related to establishing behavioral health parity, such as a law giving it authority over health plans and third-party organizations that conduct benefit reviews.
Addressing population health challenges demands a concerted effort. Rhode Island is fortunate to have a culture of collaboration among health care leaders, coupled with strong political commitment to health system improvement.

New numbers from the U.S. Census Bureau show an uptick in Americans who are uninsured but modest progress on poverty and income — handing Democrats and Republicans data for talking points.
Overall, the percentage of Americans lacking health coverage at any point in the year rose from 7.9% in 2017 to 8.5% in 2018. That’s according to annual numbers released Sept. 10.
The rise in the uninsured spanned demographic groups. Uninsured rates rose between 2017 and 2018 for whites, African-Americans, Hispanic Americans, Asian Americans, native-born Americans, foreign-born Americans, people with disabilities, people without high school degrees, and those under 18.
The 2017 and 2018 figures are not directly comparable with previous years due to changes in how the data is calculated. But a different data set showed that the small rises in the uninsured rate for 2017 and 2018 marked a change for a number that had improved every year since its peak in 2010, when the Affordable Care Act was passed. The law created a national marketplace for individual insurance and allowed states to expand Medicaid to more people.
Democrats pounced on the data release, with House Speaker Nancy Pelosi, D-Calif., blaming “President Trump’s cruel health care sabotage,” including his efforts to pare back the Affordable Care Act through regulations and in court.
But the Trump administration could point to modest gains in other statistics reported by the Census Bureau.
“Americans of all backgrounds are experiencing economic success in the Trump economy,” the White House said in a statement that cited media coverage of the new numbers on income and poverty.
The U.S. poverty rate fell for the fourth consecutive year, from 12.3% in 2017 to 11.8% in 2018. The national poverty rate is currently lower than it has been in any year since 2000, as this chart indicates.
Meanwhile, median household income rose for the fourth consecutive year after adjusting for inflation. It was a small rise, however, from $62,626 in 2017 to $63,179 in 2018, or an increase of less than 1%. And the pace of growth has slowed somewhat since the middle of this decade.
A leading measure of income inequality known as the GINI coefficient dipped slightly between 2017 and 2018. But its decades-long rise toward greater inequality was not greatly slowed.
Under this measurement, a score of 0.0 represents total income equality, while a score of 1.0 represents total inequality.
The overall statistics for poverty and income also mask significant differences by race and ethnicity.
In 2018, for instance, the poverty rate for whites was 8.1%. But it was much higher for African-Americans (20.8%) and Hispanic-Americans (17.6%) and modestly higher for Asian-Americans (10.1%).
The poverty rate fell slightly in 2018 for whites, African-Americans and Hispanic-Americans, while rising slightly for Asian-Americans.
|
||
|

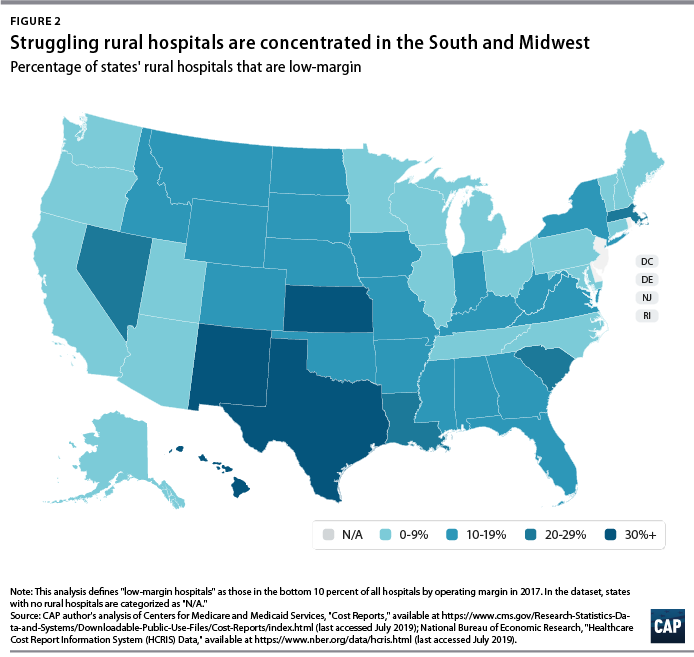
The number of rural hospital closures in the United States has increased over the past decade.1 Since 2010, 113 rural hospitals,2 predominantly in Southern states, have closed. This is a concerning trend, since hospital closures reduce rural communities’ access to inpatient services and emergency care.3 In addition, hospitals that are at risk financially are more likely to serve rural communities with higher proportions of vulnerable populations.4
Understanding the financial pressures facing rural hospitals is imperative to ensuring that America’s 60 million rural residents have access to emergency care.5 Rural hospitals are generally less profitable than urban ones, and those with the lowest operating margins maintain fewer beds and have lower occupancy rates. Low-margin rural hospitals are also more likely to be in states that have not expanded Medicaid under the Affordable Care Act (ACA). According to new analysis by the Center for American Progress, future hospital closures would reduce rural Americans’ proximity to emergency treatment. Among low-margin, rural hospitals—those most likely to close—the majority of those with emergency departments are at least 20 miles away from the next-closest emergency department.
This report first discusses the role that hospitals and emergency care play in rural health care as well as trends in hospital closures. It then uses federal data to examine differences in the financial viability of rural and urban hospitals and the availability of hospital-based emergency care in rural areas. The final section of this report offers policy recommendations to improve health care access and emergency care for rural residents.
From 2013 to 2017, rural hospitals closed at a rate nearly double that of the previous five years.6 (See Figure 1) According to the Government Accountability Office (GAO), recent rural hospital closures have disproportionately occurred among for-profit and Southern hospitals. Southern states accounted for 77 percent of rural hospital closures over that time period but only 38 percent of all rural hospitals in 20137

Hospital closures may deepen existing disparities in access to emergency care. Closures are more likely to affect communities that are rural, low income, and home to more racial/ethnic minority residents.8 Although about half of acute care hospitals are located in rural communities and the other half are located in urban areas,9 rural residents live 10.5 miles from the nearest acute care hospital on average, compared with 4.4 miles for those in urban areas.10 According to a poll by the Pew Research Center, about one-quarter (23 percent) of rural residents said that “access to good doctors and hospitals” is a problem in their community, while only 18 percent of urban residents and 9 percent of suburban residents said it was a problem.11
A variety of factors influence hospitals’ sustainability. Thanks to medical and technological advances, conditions that once required hospitalization can now be treated in an ambulatory care center or a physician’s office. University of Pennsylvania professor and CAP nonresident senior fellow Ezekiel Emanuel has argued that one reason hospitals are closing is that “more complex care can safely and effectively be provided elsewhere, and that’s good news.”12 As a whole, the hospital industry remains highly profitable, and hospital margins are at their highest in decades.13
Evidence on the relationship between hospital closures and health outcomes is mixed. A 2015 study of nearly 200 hospital closures in Health Affairs found no significant changes in hospitalization rates or mortality in the affected communities, whether rural or urban.14 More recent studies have found an association between rural hospital closures and increased mortality. Harvard researcher Caitlin Carroll showed that rural hospital closures led to an overall increase in mortality rates for time-sensitive health conditions,15 and Kritee Gujral and Anirban Basu of the University of Washington found that rural hospital closures in California were followed by increases in mortality for inpatient stays.16
In rural areas, hospitals face additional challenges to their viability, including lower patient volumes; higher rates of uncompensated care; and physician shortages.17 In addition, rural patients tend to be older and lower income.18 Rural hospitals tend to be smaller, serve a higher share of Medicare patients, and have lower occupancy rates than urban hospitals.19 Rural hospitals commonly offer obstetrics, imaging and diagnostic services, emergency departments, as well as hospice and home care,20 but patients needing more complicated treatment are often referred to tertiary or specialized hospitals. In fact, rural patients are more likely to be transferred to another hospital than patients at urban hospitals.21
Most urban hospitals are reimbursed under the prospective payment systems (PPS) for Parts A and B of Medicare. Through both the inpatient and outpatient PPS, the Centers for Medicare and Medicaid Services (CMS) reimburse hospitals at a predetermined amount based on diagnoses, with adjustments—including those for local input costs and patient characteristics.22 However, rural hospitals often face higher costs due to lower occupancy rates and provide care to a higher percentage of patients covered by Medicare, Medicaid, and the Children’s Health Insurance Program (CHIP). Such hospitals may be eligible to receive higher payments from Medicare if they qualify as a Sole Community Hospital (SCH) or Medicare-Dependent Hospital (MDH).23
Another form of financial relief for rural hospitals is obtaining designation as a Critical Access Hospital (CAH), which Medicare reimburses based on cost rather than on the PPS.24 To qualify as a CAH, a hospital must provide 24/7 emergency services; maintain no more than 25 beds; and serve a rural area that is 35 miles from another hospital.25 Medicare reimburses CAHs at 101 percent of reasonable costs, rather than through the inpatient and outpatient PPS structures.26 As of 2018, there were 1,380 CAHs nationwide,27 accounting for about two-thirds of all rural hospitals.28
Even with cost-based reimbursement, however, some CAHs are unable to sustain the costs required to maintain inpatient beds.29 The 25-bed limit for CAHs prevent participating hospitals from eliminating inpatient services and restrict their ability to expand in response to fluctuations in community populations or care volumes. Other challenges facing rural hospitals include lacking sufficient patient volume to maintain high-quality performance for certain procedures and pressure to drop high-value but poorly reimbursed services such as obstetrics while maintaining low-volume, high profit services such as joint replacement procedures. 30
A key way that states can support struggling rural hospitals is by expanding Medicaid under the ACA. Expanding Medicaid increases coverage among low-income adults, 31 which in turn reduces uncompensated care costs for hospitals32 and allows financially vulnerable hospitals to improve their viability.33 Consistent with other recent studies,34 the GAO concluded in a 2018 report on rural hospitals that those “located in states that increased Medicaid eligibility and enrollment experienced fewer closures.”35
Rural hospitals in different states have responded to financial pressures in a variety of ways, trying to balance community needs with financial viability. For many hospitals this has meant cutting inpatient obstetric services, leaving more than half of rural counties without hospital obstetric services.36 For instance, in Wisconsin, falling birth rates led to 12 hospitals in the state closing their obstetric services in the past decade.37 In Grantsburg, Wisconsin, lower birth rates and an older community population led Burnett Medical Center to shut down its obstetrics services.38 In order to offer these services, Burnett Medical Center would have needed to keep a general surgeon on call to perform caesarean sections, and with just 40 deliveries in 2017, the hospital could not justify the expense.39 While the hospital will continue providing prenatal and postnatal care, it will refer patients to a facility in Minnesota for deliveries—a facility is almost 40 minutes away.40
In other communities, hospitals have been replaced by other types of health care facilities. For example, Appalachian Regional Healthcare System closed Blowing Rock Hospital in North Carolina in 2013. Three years later, it opened a 112-bed post-acute care center in Blowing Rock in response to demand for rehabilitation services and the aging population in the surrounding area.41
To compare the financial situations of rural and urban hospitals and examine how future rural hospital closures could affect the availability of emergency care, CAP analyzed data from the CMS Healthcare Cost Report Information System (HCRIS). The CMS requires all Medicare-certified hospitals to report their financial information annually. CAP used the HCRIS to examine the financial margins and other characteristics of 4,147 acute care hospitals for fiscal year 2017. Of these, 1,954 hospitals (47 percent) were in rural areas, while the remaining were in urban areas. Hospitals self-report their status in the HCRIS as either urban or rural, which the CMS defines as either inside or outside of a metropolitan statistical area, respectively.42 Further information about CAP’s hospital sample can be found in the Methodological appendix.
Hospital operating margins, which measure excess patient-related revenues relative to patient-related expenses, are often used as an indicator of financial health.43 A 2011 study by Harvard researchers Dan Ly, Ashish Jha, and Arnold Epstein found that the lowest 10 percent of hospitals by operating margin were 9.5 times more likely to close within two years compared to all others. 44 The same study concluded that hospitals with low operating margins were also more likely to be acquired or merge.45
In CAP’s hospital sample, the median operating margin was negative 2.6 percent among all hospitals, negative 0.1 percent for urban hospitals, and negative 4.9 percent for rural hospitals.46 Public hospitals and MDHs in the sample were more likely to have negative operating margins, consistent with what other studies have found.47 To analyze hospitals’ relative financial health across geographic areas, CAP ranked hospitals in the HCRIS sample based on operating margin, splitting them into three groups: the lowest 10 percent, the middle 80 percent, and the highest 10 percent. The range of operating margins for each group is shown in Table 1.

Rural hospitals are less likely to be financially healthy than urban hospitals. In 2017, rural hospitals comprised only 27.9 percent of the hospitals with operating margins in the highest decile but comprised 59.7 percent of the hospitals in the lowest decile. Southern and Midwestern states had the greatest proportion of rural hospitals with low operating margins, mimicking the geographic patterns in hospital closures that the GAO report identified. CAP finds that from 2015 through 2017, rural hospitals were consistently more likely than urban hospitals to fall in the bottom 10 percent of operating margins. CAP’s analysis also confirms that rural hospitals in states that expanded Medicaid had a higher median operating margin (negative 3.4 percent) than those in states that have not expanded Medicaid (negative 5.7 percent).
To examine commonalities among the hospitals most vulnerable to closure, CAP analyzed characteristics of the hospitals with low margins, defined as having an operating margin in the lowest 10 percent among all hospitals. Smaller, low-occupancy rural hospitals were most likely to struggle financially: nearly 1 in 6 (15 percent) of hospitals with 25 or fewer beds had low margins, and nearly one-fifth (17 percent) of hospitals with low-occupancy rates had low margins. (See Figure 3)

In some emergency situations, hospital closures can be life-threatening, increasing the time and distance patients travel to receive care. Studies show that the probability of dying from a heart attack increases with distance from emergency care,48 and traumatic injuries are more likely to be fatal for rural residents than for urban ones.49
Rural residents are more likely than urban residents to visit the emergency department.50 A shortage of primary care providers; lack of public transportation infrastructure; shortages in preventive care; higher rates of smoking and obesity; and greater prevalence of chronic disease in rural areas all contribute to the greater utilization of emergency room care.51 As a result, emergency departments often stand in as the main source of care for vulnerable and low-income populations, especially for communities that face a shortage of primary care. 52 Among the dozens of rural hospitals that have closed in recent years, some served as the only emergency department in a community, according to MedPAC53
While freestanding emergency departments have proliferated,54 they are not filling the gap for rural emergency care. MedPAC found that, as of 2016, nearly all the country’s 566 stand-alone emergency departments were in urban areas and tended to be located in more affluent communities.55 Researchers at the North Carolina Rural Health Research Program found that the freestanding emergency department model was generally not viable in rural areas of the state due to low patient volumes, high rates of uninsured patients, and provider shortages.56 One limit on the growth of independent freestanding emergency centers is that they are not recognized in Medicare law and are therefore unable to bill the program, unlike hospital-affiliated off-campus emergency departments. 57
To better understand how future rural hospital closures could affect access to emergency care, CAP calculated hospitals’ distance to the next-closest hospital-based emergency department. CAP restricted its 2017 HCRIS data sample to the 3,616 acute care hospitals that provide 24-hour emergency services.58 Using addresses or coordinates provided in the HCRIS, CAP mapped each low-margin rural hospital to the next-closest hospital emergency department. Mapping strategies are detailed in the Methodological appendix.
Among the 222 low-margin rural hospitals, more than half (55 percent) were more than 20 miles away from the next-closest hospital-based emergency department, and one-tenth were more than 35 miles away. (See Figure 4). The average distance to the next-closest emergency department was 22 miles.
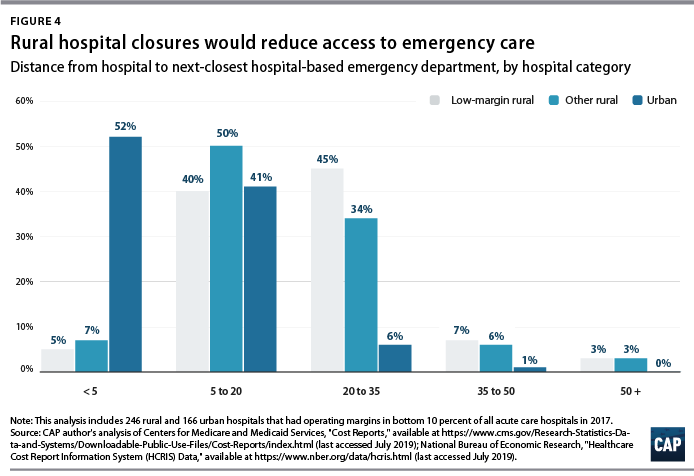
The disappearance of rural, low-margin hospitals would greatly increase patients’ travel distances for emergency care. Without other resources to fill the gap, some patients might forgo care they need and others would be forced to undertake an even longer journey to receive medical attention.
As rural hospitals continue to close, it is crucial to preserve access to emergency care for rural Americans. The following section details a series of policy recommendations to support adequate emergency care and address care shortages in rural communities.
Experience to date suggests that rural hospitals in those states that have not yet expanded their Medicaid programs under the ACA would benefit from Medicaid expansion through lower levels of uncompensated care and increased financial sustainability. Medicaid expansion is associated with improvements in health and a wide variety of other outcomes, including lower mortality, less uncompensated care, and lower rates of medical debt.59 According to the Kaiser Family Foundation, about 4.4 million adults would gain Medicaid eligibility if the remaining 14 nonexpansion states expanded their programs.60
Policymakers can also support rural communities and their hospitals by opposing efforts to repeal the ACA. If the Trump administration-backed lawsuit against the ACA were to succeed, 20 million Americans would lose health insurance coverage, and uncompensated care would rise by $50 billion, according to the Urban Institute.61
To preserve access to emergency care, Congress could allow rural hospitals like CAHs to downsize to an emergency department and eliminate inpatient beds without giving up special Medicare reimbursement arrangements. Qualifying hospitals could transfer patients requiring inpatient admission to other hospitals, while continuing to offer some diagnostic imaging and other outpatient services.
One such proposal is the Rural Emergency Acute Care Hospital Act (REACH Act), bipartisan legislation proposed by Sen. Amy Klobuchar (D-MN) and Sen. Chuck Grassley (R-IA) that would create rural emergency centers.62 This designation would allow hospitals to provide only emergency care in rural communities and receive Medicare reimbursement at 110 percent of operating costs. Separately, MedPAC has recommended that rural hospitals located more than 35 miles from the nearest emergency department be allowed to convert to freestanding emergency departments while still being reimbursed at hospital rates.63
Under global budgeting, hospitals are paid a fixed amount rather than having their reimbursements based on the volume and types of services they provide.64 Global budgeting can reduce small, rural hospitals’ financial risk by providing them with a more predictable stream of revenue. In addition, payment reforms that include both hospital and nonhospital care can encourage communities to invest in services that are typically less generously reimbursed, such as preventive care.65
For example, in 2014, Maryland transitioned its acute hospitals from fee-for-service payments to a global budget.66 An evaluation of the global budget program showed that it reduced hospital expenditures relative to trend without transferring costs to other parts of the health care system.67 Future global budgets should emphasize improvements in population health and primary care,68 including ensuring that patients receive care in appropriate settings and reducing the number of avoidable hospital visits.
The Pennsylvania Rural Health Model is the first Medicare demonstration project to test the financial viability and community effects of a global budget for strictly rural hospitals.69 This six-year program aims to smooth out cash flow for 30 rural Pennsylvania hospitals on a monthly basis with the goal of enabling hospitals to meet community needs, especially for substance-use disorder and mental health services.70 With global budgets based on the previous year’s revenues, participating hospitals will have a more predicable stream of revenue. Importantly, the program allows hospitals to share in the savings that result from avoidable utilization.71
The lack of transportation infrastructure can lead rural residents to rely on ambulances and emergency rooms for nonemergency care. In nonemergency situations, patients often cite the lack of affordable transportation as a major barrier to care access.72 In order to fill the gap, payers and policymakers should consider efforts to utilize existing community transit resources for medical transportation or reimburse patients who use ride-sharing services in areas that lack public transit or taxi services. 73 Another option would be to formalize volunteer services for medical transit. Oregon offers a tax credit for volunteer rural emergency medical services (EMS) providers, who provide medical and transportation services analogous to those of volunteer firefighter programs.74 The CMS should also consider policies to better reimburse and expand the use of telehealth in remote areas to reduce patients’ burden of transportation.75 Finally, the CMS should stop approving states’ requests to waive coverage of nonemergency medical transportation (NEMT) requirements under Medicaid.76 NEMT is vital to eligible beneficiaries’ access to care, including appointments for preventive care, chronic disease management, and substance-use disorder treatment.
Rural health care provider shortages contribute to poorer access to care and poorer quality of care in rural communities. While 20 percent of the U.S. population lives in rural areas, only 9 percent of primary care physicians practice in rural areas.77 Greater access to primary care providers in rural areas would improve quality of care and health outcomes while also reducing unnecessary emergency department visits.78
One way to assist rural areas would be to encourage health professionals to train and work in underserved communities. Federal funding for physician training should include reimbursements for community-based sites so that medical residents can rotate through nonhospital settings.79 Expanding the National Health Service Corps—which provides scholarships and student loan repayment for professionals who work in federally designated health professional shortage areas—could also help bolster the rural workforce. In addition, changes to immigration policy—such as expanding the Conrad 30 program that funnels immigrant doctors into rural and underserved communities, reforming H-1B visas to benefit high-need communities—could help alleviate rural areas’ shortage of medical professionals.80
Mounting closures of rural hospitals across the country are exacerbating the disparity in health care access between rural and urban areas. The financial vulnerability of the remaining rural hospitals suggests that the trend may continue, leaving shortages in emergency care and other hospital services.
Policymakers should support initiatives that allow remaining rural hospitals the flexibility to tailor their services to meet community needs and improve access to care for rural Americans.

The U.S. trade war with China threatens to hit hospitals and health systems as well as consumers in the form of higher prices and product shortages, the president of medical supply distributor DealMed told Yahoo Finance.
On Sept. 1, President Donald Trump imposed a 10 percent tariff on $300 billion in Chinese imports, tacking more medical supplies on the list. And the administration is threatening to hike the current 25 percent tariff on $250 billion in Chinese imports to a 30 percent tariff on Oct. 1.
The products affected by the tariffs are used daily in physician offices, hospitals, pharmacies and by consumers at home, according to DealMed President Michael Einhorn.
“Think of products like gauze that are in Band-Aids. Think of other products like medical gloves,” Mr. Einhorn told Yahoo Finance. “Those products will be somewhat affected, somewhere between 10 percent and 25 percent.
“When you throw tariffs into the mix, we’re talking about potential shortages, we’re talking about potential price increases — not only to hospitals and big healthcare systems, but also to the consumer at home,” Mr. Einhorn said.
Read the full report here.

In the last presidential election, the idea of abolishing private health insurance was confined to the far left of American politics. Now it’s the central argument of the Democratic primary race.
On June 17, 2016, 15 prominent Democratic Party activists and elected officials gathered in a hotel conference room in downtown Phoenix. Their job was to formulate language for the party platform, which would be adopted at the following month’s national convention in Philadelphia. But the platform-drafting committee also had an unspoken mission: to defuse the lingering intraparty tension in the wake of Bernie Sanders’s spirited but unsuccessful primary battle against Hillary Clinton.
The Democrats hadn’t faced convention infighting since 1980, when Senator Edward M. Kennedy challenged the incumbent president, Jimmy Carter, and party leaders hoped to use the process of drafting the platform — the compendium of official positions on policies and issues that the party faithful formally approve at the convention — to head off a similar situation. Sanders, the Vermont senator, had been awarded five of the committee’s 15 seats in order to come up with platform language that would be as unifying and unoffensive as possible.
The fifth session was devoted to health care, and it began innocently enough. “The Democratic Party believes accessible, affordable and high-quality health care is part of the American promise,” the committee’s chairman, the Maryland congressman Elijah Cummings, intoned. Several minutes’ worth of earnest self-congratulation about the Affordable Care Act, the legislative centerpiece of Obama’s presidency, followed. The Republican presidential nominee, Donald Trump, had vowed to eliminate “the disaster known as Obamacare,” which mandated that private insurers offer health-insurance plans to those who otherwise didn’t have access to insurance, and mandated that most uncovered Americans enroll in them. The Democrats in the Phoenix conference room were unanimous in their desire to preserve the A.C.A. and to draft platform language assuring the American public that their nominee, Hillary Clinton, would do just that.
A half-hour into the session, Cummings directed the attendees’ attention to a guest on their computer screen. It was RoseAnn DeMoro, the executive director of National Nurses United, the labor group that for years had been the dominant advocate for a government-run national health care system, also known as “single payer” or “Medicare for All.” DeMoro was Skyping in from Chicago, where she was due to speak that evening at the People’s Summit, a gathering of thousands of Sanders supporters. Sanders had requested that DeMoro be given one of his five seats on the platform-drafting committee but had been overruled by Clinton’s loyalists, most likely because DeMoro’s union had loudly supported Sanders over Clinton.
DeMoro, now 70, tends to wear an intent expression that alternates between amusement and withering skepticism. She dispensed with the pleasantries. Obama’s health care program in many ways, she told the attendees, “has fallen short.” Costs were continuing to go up. Sick people continued to be denied coverage. The legislation’s biggest winners were the insurance and pharmaceutical industries. “We’re urging the Democratic Party to put patients before profits,” DeMoro said, “and to make health care for everyone basically a right.”
The Sanders delegates in the conference room applauded enthusiastically. Later the Clinton adviser Neera Tanden reminded DeMoro that the convention intended to feature stories of people whose lives had been saved by Obamacare. Representative Barbara Lee of California insisted that she and other House Democrats had “fought very hard” for single payer. Their goal now should be to “build upon the Affordable Care Act,” Lee argued.
DeMoro was not having it. Building upon a for-profit plan would only serve to entrench the profiteers, she insisted. For every Obamacare success story Tanden might wish to promote, she told the committee, the nurses could recite a multitude of tragedies. “You are not ever going to corner the nurses into saying it’s adequate,” DeMoro said. “I see the dynamic that’s happening here,” she added, her eyes narrowing. “You think that I’m criticizing the Democratic Party for not fighting hard enough for a single-payer health care system. And I think that’s probably accurate.”
Onstage that evening at the People’s Summit, DeMoro gleefully recounted the rancorous exchange. “They wanted me to say that the Democratic Party fought hard enough,” she told the audience. “But in reality, they didn’t.” Then, to thunderous applause, DeMoro said, “When I appeared by Skype before the committee, I could feel the Bernie movement’s power. I could feel the 58 percent of the American people who support single-payer health care.”
That power was not enough to sway the platform committee, which by a margin of one vote elected not to include any mention of a single-payer system in its 45-page official document. A little more than a month later at the Democratic convention, DeMoro remembers running into Lee. Lee, a liberal from DeMoro’s state, was still stung by her criticism. “Man, you went after me hard!” DeMoro recalls Lee saying. As a state senator in 1998, Lee reminded her, she had co-written a single-payer bill that died in committee. And Lee had, in fact, joined Sanders’s five drafting-committee members in voting to include single-payer language in the party platform.
DeMoro regarded Lee’s efforts as insufficient. The Sanders campaign’s success in making Medicare for All a defining progressive issue, she told me recently, “was a time in history when you knew change had come and the movement was moving past the standard-bearers of the left. It was one of those lead-or-get-out-of-the-way moments. And Barbara was playing an insider game and wasn’t willing to fight.”
Like many progressive activists, DeMoro — who retired from National Nurses United last year but remains an influential voice on the left — views her movement’s proximate adversary as the Democratic establishment rather than Trump’s Republicans. Of late, she has devoted much of her social-media energy to deriding Senator Kamala Harris, whom she has called “Chameleon Harris” on Twitter. A longtime resident of the Bay Area, DeMoro viewed Harris more or less favorably when she was California’s attorney general. But as Sanders’s presidential opponent, she had, to DeMoro’s thinking, revealed herself to be a transparently calculating triangulator: “There’s no there there.”
The day before the second round of Democratic presidential debates in Detroit, Harris’s campaign announced her new health care plan, which would guarantee universal coverage but also keep private insurers. Even though the plan was not a single-payer system, Harris had nonetheless felt compelled to call it Medicare for All. Three weeks later, however, she would tell her donors, “I’ve not been comfortable with Bernie’s plan, the Medicare for All plan.”
The contortions suggested how much the politics of health care among Democrats had changed — and how much Sanders and DeMoro had changed them. In a party that three short years ago kept single-payer advocates at Skyping distance, Medicare for All now sits at the head of the table, pulling the Democrats decisively leftward. Sanders’s Medicare for All bill in the Senate has 16 co-sponsors. In the House of Representatives, Pramila Jayapal, who is the co-chairwoman of the Progressive Caucus, has introduced a health care bill with 117 Democratic co-sponsors that is even more lavish in its benefits (and thus probably costlier) than the plan Sanders has put forward in the Senate; it, too, is called Medicare for All. In addition to Harris, two other presidential candidates have offered health care plans that pilfer from Sanders in name if not in substance: Pete Buttigieg, with Medicare for All Who Want It; and Beto O’Rourke, with Medicare for America — the latter borrowing from a proposal developed by Neera Tanden’s Center for American Progress, itself called Medicare Extra for All. The idea’s original advocates, like DeMoro and Sanders, after years of struggling to get into the mainstream Democratic policy debate, suddenly have an embarrassment of allies — or at least people who claim as much. “Medicare for All shouldn’t mean all things to all people,” Warren Gunnels, Sanders’s senior campaign adviser, told me. “It’s single payer. Everybody else’s program is Medicare for Some.”
Medicare for All, as envisioned by Sanders in a 2017 Senate bill, would expand coverage in phases over a four-year period. Drug co-payments would not exceed $200 a year. The overall cost of the plan would be roughly $30 trillion over a decade. According to an analysis by the University of Massachusetts Amherst’s Political Economy Research Institute, that amount would be largely offset through savings in areas such as administrative overhead, pharmaceutical costs and physician salaries. A combination of payroll, sales, capital gains and income taxes could pay for the remainder. The result would be a government-run health care system in which Americans of all ages are covered, are able to select whichever doctor they choose and incur almost no out-of-pocket expenses.
Not since the Great Society era has so ambitious a social program been so actively promoted by influential Democrats. Whether this is a good thing, both as a matter of policy and for a party longing to defeat Trump next year, is currently at issue. On the one hand, the predominance of health care as a voting concern typically favors Democrats; as Sanders’s pollster Ben Tulchin put it to me, “When the conversation is about health care, we’re already winning.”
Single-payer advocates achieved a victory of a sort in the July 30 Democratic presidential debate in Detroit, when the CNN moderator Jake Tapper said, “Let’s start the debate with the No. 1 issue for Democratic voters, health care — and Senator Sanders, let’s start with you.” The 10 candidates onstage discussed Medicare for All for the next 20 minutes — longer than any other issue.
It was an establishing shot that lingered even when the night’s camera frame panned over to immigration and climate change. A couple days after the debate, an ABC News/Ipsos poll showed that when Democratic voters watched both a video of Sanders explaining the virtues of Medicare for All and a video of the front-runner Joe Biden arguing for simply improving Obamacare, 31 percent found the Sanders plan “very convincing,” while only 18 percent said the same of Biden’s position.
A few days later, however, a Monmouth University poll of likely Democratic caucusgoers in Iowa found that 56 percent preferred the option to receive Medicare, as opposed to a mere 21 percent favoring a government-run plan that abolished private insurance. It underscored the fears of Democrats on the center-left that the issue will boomerang on them in 2020 — that campaigning on an entirely government-run health care system, the creation of which would remove about 156 million Americans from their employer-based plans, according to a Kaiser Family Foundation analysis, will invite an electoral backlash. “It’s been the case of health care policy for decades,” Tanden told me. “If a health care plan is perceived to be about protecting something, it’s usually good. If it’s about losing something, it’s usually toxic.”
Eighteen percent of the United States economy, or $3.5 trillion, is tied to health care, up from 5 percent in 1960. The United States spends at least double per capita what other industrialized nations spend on health care. The health sector is among America’s most profitable industries. And despite the vast profits and expenditures, the United States has comparatively worse health outcomes than other advanced nations that spend far less on health care: higher overall mortality rates, higher premature deaths and higher preventable deaths — all on top of the fact that two-thirds of all bankruptcies and nearly half of all foreclosures in America today are related to medical costs.
In spite of these dismal returns, the health care system has proved extraordinarily resistant to disruption — no doubt in part because of the uniquely palpable stakes. “Health care is unlike any other issue,” Tanden says. “People feel an expertise about it, because they’ve lived it. It’s very personal to them: They think of the care of their child, of their aging parents, of their own vulnerability.”
Though highly attuned to the health care system’s deficiencies, the public has also been fretful that their political leaders will only succeed in making a flawed system worse. For a quarter century, Gallup polls have found that almost without exception, 65 to 73 percent of Americans believe the health care system to be in a state of crisis or having major problems. The same polls observed Republicans feeling especially dire starting in 2010, while conservatives were condemning Obamacare; and Democratic fears spiked in 2018, after Obamacare narrowly escaped repeal by congressional Republicans.
Those sentiments might suggest that Americans would prefer the government to leave well enough alone. But at a moment when a reconsideration of the party’s staid politics is already brewing, they might just as easily be interpreted as a call to arms: a rationale for burning down the system and starting anew.
“I’m not an incrementalist,” DeMoro told me one afternoon at a pizza restaurant in Napa, where she now lives in retirement. “I firmly believe that change happens through rupturing. Trump’s a prime example of that. And the Democrats have used Trump as an excuse not to have a platform of their own. Well, Bernie’s running for systemic change.”
DeMoro became the executive director of the California Nurses Association in 1993. The daughter of the owners of a pizza parlor and a beauty salon in St. Louis, she had never worked in the medical profession. She was fluent in political theory as well as in blue-collar issues and had become close with two of the most tenacious grass-roots activists in postwar American history: the labor organizer Tony Mazzocchi, who successfully agitated for passage of the Occupational Safety and Health Act of 1970; and Ralph Nader, who prodded Congress to pass the Consumer Product Safety Act into law in 1972. “She was steeped in the history of the labor movement, had a critical mind and locked horns with everybody,” Nader recalls. “She would trash the A.F.L.-C.I.O. for lacking substance and courage. But she also really understood the issues. I thought she was the greatest labor leader out there.”
DeMoro took her post shortly after Bill Clinton was elected president, at a moment when rupture seemed imminent in the American health care system. The number of uninsured Americans under 65 had risen steadily from 33.4 million in 1989 to 37.1 million in 1992. (It would be 41.6 million in 2004.) This troubled a Washington State congressman and former child psychiatrist named Jim McDermott. As a medical-school student in the early 1960s, McDermott watched with interest as Canada built its single-payer system while, he recalled, “the American Medical Association leadership predicted that this was the end of the profession, socialized medicine, blah blah blah. Then they said the same about Medicare, until it became a goddamned cash cow for doctors.”
By 1993, McDermott was single payer’s leading champion in Congress. That same year, he put forward a single-payer bill in the House. (Among its 90 co-sponsors was an obscure Vermont freshman named Bernie Sanders.) “Then Clinton came into office,” McDermott told me recently. “Mrs. Clinton needed my 90 votes for their health care plan. She didn’t want to have anything that looked like socialism. She said, ‘Jim, you want to take out the insurance industry, but it’s deeply embedded in our society.’ ”
McDermott gamely offered his support. But Hillary Clinton’s determination to preserve the private insurance system was not enough to assuage Republicans or health care industry lobbyists. The 1,342-page Clinton plan known as “Hillarycare,” which required employers to either provide insurance or pay a penalty that would finance insurance exchanges, was demonized by the health-insurance industry’s “Harry and Louise” TV ads as a wallet-busting bureaucracy that would eliminate Americans’ right to choose their doctors.
The Democrats abandoned their efforts six weeks before the 1994 midterm elections so as to minimize the political damage. In the years that followed, health care costs rose and coverage rates fell. In 1999, medical expenses consumed 14 percent, on average, of American’s take-home pay. By 2017, that figure would more than double, to 31 percent.
These costs ballooned despite the health care industry’s efforts to maximize efficiency through a “managed care” approach, restructuring hospitals and clinics as health maintenance organizations, or H.M.O.s. Under the H.M.O. model, nurses found themselves losing status, leverage and in some cases their jobs. Those who remained employed often found their jobs transformed. “We as nurses were expected to get ’em out fast and move on,” Elizabeth Pataki, a former nurse and labor activist (and cousin of New York’s former governor George Pataki), recalls. “It was heartbreaking to see how little care they were getting and how so many of them couldn’t pay their deductibles, how their premiums were becoming ruinous, how they would ration their medicine by breaking it in half.”
That was the landscape DeMoro encountered as she led the undersize 17,000-member California Nurses Association into the fight against what she would term “the commodification of health.” She spent hours on picket lines with the nurses and absorbed their eyewitness grievances. In the male-dominated world of union leadership, the C.N.A. president stood out. “Nurses of a certain age like me didn’t have role models back then, except perhaps nuns and teachers,” Pataki says. “But RoseAnn, for many of us, showed what it meant to be a woman of commitment, to be warm and funny but also dedicated and direct. I could see where we could go with her.”
They did not go very far at first. In 1994, DeMoro’s California-based union pushed the State Legislature to adopt a single-payer bill, to no avail. Two years later, DeMoro’s union promoted Proposition 216, which aimed to curb the ability of hospitals and H.M.O.s to restrict coverage, only to be bombarded by TV ads (paid for by a coalition of H.M.O.s and business affiliates) conceived by the same political consultants whose “Harry and Louise” ads were used to defeat Clinton’s health care initiative.
The 2008 presidential campaign offered fleeting hopes for single-payer advocates. As a state senator in 2003, Barack Obama proclaimed himself to be “a proponent of a single-payer universal health care program.” Late in the summer of 2007, DeMoro remembers receiving a call from an Obama campaign staff member. The candidate was coming to the Bay Area, the staff member said. Would she like to spend the day driving around with him and discussing health care?
DeMoro agreed. But in typical fashion, she commissioned radio advertisements on the eve of Obama’s arrival, urging the candidate to openly advocate for a single-payer system. “I got a call from one of his people, asking, ‘Did you guys do this ad?’ ” she recalled. “And when I said it was us, they canceled the visit.”
Her union, which by 2008 had grown to around 100,000 members, nonetheless held events around the country for Obama. But in office, DeMoro told me, Obama “proved that he had learned exactly the wrong lesson from Hillarycare.” Insurance and pharmaceutical companies who viewed single payer as an apocalyptic proposition were awarded seats at the table, as were Republican senators.
“Barack said, ‘I don’t want to just message this issue, I want to get something done,’ ” Tom Daschle, Obama’s early pick for Health and Human Services secretary, told me. “The view was that if we started more moderately and reached out to Republicans with something they supported in the past, we’d have something we could accomplish. There were some who believed that Medicare was a good brand that we could expand on. But he didn’t believe Republicans were likely to join that effort.”
The question was whether Republicans were likely to join any effort. The party had been staunchly opposed to government health care expansions, including Medicare, for half a century, arguing instead for market-driven solutions, tax credits and restricting malpractice claims. (An exception to this was when President George W. Bush successfully pushed to extend Medicare coverage to include prescription drugs in 2003 — an industry-friendly initiative that was interpreted by some as a means of shoring up the president’s support among senior citizens in advance of the 2004 election.)
In practice, however, Republican lawmakers have struggled to reconcile what Ronald Reagan termed “the magic of the marketplace” with tens of millions of Americans’ inability to pay for adequate health care. Obama forced the issue by proposing a health care reform built on the bones of a 20-year-old market-based proposal from the conservative Heritage Foundation. “My line at the time,” Charlie Dent, a moderate Republican congressman from Pennsylvania who retired last year, told me, “was that every American had a right to have access to affordable health care insurance.”
The more expedient option was for Dent’s party to weaponize the issue. Obama and congressional Democrats spent a year and a half trying to engage Republicans on health care, along the way discarding one preferred policy option after the next in hopes of forging a bipartisan agreement.
Max Baucus, the Montana Democrat who was chairman of the Senate Finance Committee at the time and led the negotiating effort, had visited a Canadian hospital and was an admirer of that country’s health care system. Still, when he began committee meetings on health care in late 2008, “I told them, ‘Let’s find a uniquely American solution,’ ” he recalled. “ ‘And nothing’s off the table.’ The only exception to that I made was single payer. I thought our country was just not ready for it. I assumed that if we worked together in good faith that over time, we’d naturally evolve toward that kind of system.”
A few of the Republican senators on the committee, like Chuck Grassley of Iowa and Olympia Snowe of Maine, were active participants in Baucus’s meetings. Eventually, however, the Senate minority leader Mitch McConnell made clear his desire not to hand the new president any legislative victories.
“The Republicans started calling it Obamacare,” Baucus said, “and it tapped into a significant portion of the electorate’s opposition to the president. It was political in the end: ‘Hey, we can run against this thing.’ Grassley was under immense pressure from McConnell, who threatened to primary him if he stayed with this. He told me that, flat out.” (Spokespeople for Grassley and McConnell adamantly deny that McConnell applied any pressure on Grassley.) The Affordable Care Act passed in March 2010 without a single Republican vote.
In March 2015, Sanders paid a visit to DeMoro. Their relationship began in 1981 when DeMoro, then a graduate student at the University of California, Santa Barbara, contributed $20 to Sanders’s first campaign for mayor of Burlington, Vt. (Sanders won by 10 votes.) As mayor, Sanders became convinced, through conversations with physicians in Canada, that a single-payer system was the only sustainable means of delivering universal health care. Like DeMoro, he condemned any system that preserved a profit-dominated model, including what would later be known as the public option, as one that would inevitably shortchange patient care.
Now he told DeMoro that he was thinking seriously of running for president as a Democrat. Knowing that he would be heavily outspent by Hillary Clinton and her allies, he wanted DeMoro’s opinion as to whether he could count on grass-roots support. By that point, the California Nurses Association had joined together with other nursing unions in an umbrella organization, the more than 150,000-member National Nurses United, with DeMoro at its helm. Although DeMoro doubted that Sanders had much of a chance, she saw his candidacy as an opportunity to elevate the single-payer issue. In August, her organization became the first major union to endorse Sanders.
Sanders, as a presidential candidate, was an outlier’s outlier, and single payer had been deemed political kryptonite by the Democratic establishment. But DeMoro’s union bankrolled a series of surveys and focus groups by Sanders’s pollster Ben Tulchin. Tulchin was a rueful admirer of the conservative movement’s ability to frame policies in memorable ways: rebranding the estate tax as a “death tax,” for example, or slashing government programs for the poor in the name of promoting “freedom.” Democrats were too equivocal in how they framed their ideology, in Tulchin’s view. He sought to change that by devising a crisper way to sell a government-run health care system to the public.
The rebranding efforts by Tulchin happened to coincide with a gathering of progressive discontent. Throughout the 1990s, the left had more or less abided the Clinton administration’s apologetic view of big government as the cost of staying in power. In 2008, after eight years of Bush’s promoting tax cuts for the wealthy, threatening to constitutionally forbid gay marriage and waging two costly wars, progressives believed their moment had arrived and saw in Obama a new champion. But his legislative efforts proved to fall well short of revolutionary. While admonishing the left to play along and accept one moldy half-loaf after another — on the economic stimulus, on climate change, on gun control, on immigration and on several judicial appointments — the Obama White House’s varied attempts to attract Republican support met only scorn.
To many progressives, Obamacare represented the apotheosis of this strategic folly. The president’s health care initiative played by the private sector’s rules, to the pharmaceutical industry’s conspicuous benefit. And then free-market Republicans rewarded this gesture of conciliation by bashing Democrats as socialists while methodically eviscerating the program on both the state and federal levels. When in 2012 it appeared that the conservative-dominated Supreme Court might declare the A.C.A. to be unconstitutional, DeMoro led the nurses’ union on a bus tour to make the case that the time had arrived for a robust, lawsuit-proof single-payer system. The campaign was premature, however: Chief Justice John Roberts cast the tiebreaking vote in favor of Obamacare, and again progressives were compelled to leave the fight. They watched red-faced in the 2014 midterms as some of the Democratic Party’s most cautious-minded legislators were labeled big-government liberals, enabling the G.O.P. to retake the Senate. By the time the party machinery began clearing the way for Hillary Clinton’s nomination, the left had grown tired of shutting up and was now looking to a dyspeptic 74-year-old Vermont socialist as their avatar.
As Tulchin conducted his public-opinion research to address the question of how Sanders might frame his health care initiative, he hit on an answer that was hiding in plain sight. It came from the legacy of Lyndon B. Johnson, who as president had pushed Medicare and Medicaid through Congress. As Tulchin told me: “The reality is, people know what Medicare is, and it’s very popular and seen as very effective. It’s a true success story for the left. Whereas no one knows what single payer is.”
Tulchin’s findings convinced the Sanders campaign to recast single payer as “Medicare for All” — a name that had previously appeared on a 2006 health care bill written by Senator Edward M. Kennedy that included a role for private insurers. (Kennedy had been an early proponent of single payer but had come to believe that opposition from the insurance industry would doom its chances.) Sanders and DeMoro knew that the word “Medicare” would register favorably among older Americans. They had not anticipated the issue’s overwhelming popularity — close to 70 percent, according to recent polling — among millennial voters. “This had been a gray-haired movement for decades,” DeMoro told me. “It surprised all of us how resonant the issue was with young people.”
Sanders’s early campaign events were packed, in no small measure because of the mobilizing efforts of the ubiquitous union members dressed in National Nurses United’s trademark red hospital scrubs. The union’s political-action committee purchased more than several million dollars’ worth of print and TV ads. Sanders, meanwhile, occasionally called DeMoro from the campaign trail to enlist her help in demystifying the arcane mechanics of the health care industry. “When a single-payer system is finally enacted in the U.S.,” he told an aide, “RoseAnn DeMoro and the nurses are going to be the heroes of this fight.”
Although the Democratic platform committee shunted aside Medicare for All in favor of preserving the Affordable Care Act, Trump’s shocking victory in November shifted the ground again. The longstanding efforts by G.O.P. state officeholders and the Republican-controlled Congress to chip away at the A.C.A. now had an eager partner in the White House.
Shortly after the election, Sanders persuaded the Senate minority leader, Chuck Schumer, to borrow a page from Sanders’s 2016 campaign and stage pro-Obamacare rallies across the country. Those health care events — the first of them on Jan. 15, 2017, with Sanders, Schumer and other Democrats speaking before 6,000 people in Warren, Mich. — began a counteroffensive that ultimately thwarted the G.O.P.’s ambitions of repealing Obamacare.
The rallies, and the crowds they drew, suggested how the politics of health care were changing, and how quickly. Trump and congressional Republicans spent most of his first year in office working relentlessly to repeal Obamacare, an effort that barely fell short in the Senate in August. Republican governors picked up the gauntlet: by December 2018, 20 states had joined a lawsuit seeking to weaken Obamacare.
The imperiling of the Affordable Care Act had unintended consequences. One was that, after years of unpopularity, the law began polling favorably. In the 2018 midterms, it was the Republicans who were on the defensive and stammering that, well, sure, there were a few good things about Obamacare and they could be counted on to protect those things. “I’m taking on both parties and fighting for those with pre-existing conditions,” the California Republican congressman Dana Rohrabacher claimed in a TV ad, despite having voted repeatedly to gut or repeal Obamacare. Voters did not seem to buy the G.O.P.’s protestations. Exit polls following the November 2018 midterm elections, in which Republicans lost 38 seats — including Rohrabacher’s — and control of the House, showed that health care was the top concern.
But the vulnerability of Obamacare also served to underscore the case for a more resilient and comprehensive health care system of the sort that Sanders had been calling for. Medicare for All had become not merely a pet cause among the party’s progressive base but a defining one. It had also become a succinct representation to voters of what Democrats aspired to do for them that Trump’s Republicans would not.
That it had fallen to Sanders to rally Democrats to save what he found an inferior health care policy was a peculiarity not lost on Sanders, who growled to me: “I don’t think anyone will tell you that in any way single payer was seriously considered. In fact, until this year there’s never even been a goddamned hearing on single payer!” The first such hearing took place on April 30, but under the auspices of the House Rules Committee, which has no legislative jurisdiction on health care. A more meaningful second hearing was convened before the powerful House Ways and Means Committee two months later.
‘It surprised all of us how resonant the issue was with young people.’
The hearings were in a sense a validation of Medicare for All’s newfound legitimacy within the mainstream of the party, but they also demonstrated the party leaders’ wariness of the idea. The Democratic Ways and Means chairman, Richard Neal — who received nearly $550,000 in the 2018 election cycle from the health insurance and pharmaceutical industries — had already stated his preference for “a little more incremental” expansion of health care. According to The Intercept, Neal urged his fellow Democratic committee members beforehand to consider using phrases like “universal health coverage” rather than “Medicare for All.”
On one level, these are academic debates. Unless Democrats can break the Republican lock on the Senate in 2020 — a longer-odds proposition than winning the presidential election — they will have no chance of passing any laws, let alone an overhaul of health care far more sweeping than the A.C.A., which Democrats barely managed to enact with a majority in the Senate.
But on another level, the debate isn’t academic at all. It is in fact at the core of the liberal-versus-pragmatic argument among the Democratic presidential candidates, with the former vice president Biden on one end, flashing his battle scars from the Obamacare fight, and Sanders and Warren on the other, arguing that a populist movement now demands more than minor tweaks to a fundamentally flawed health care system. And indeed, on Aug. 21 Sanders tacitly acknowledged the challenge in passing so drastic a change in policy: His campaign announced that his Medicare for All plan had been modified to ensure that union workers who had already negotiated satisfactory health-insurance plans would be compensated for whatever wage increases they had sacrificed in the process.
Several health care experts with whom I spoke consider the Sanders plan, strictly as a matter of policy, to be an entirely reasonable health care solution for America. “The U.S. is an outlier in the rest of the developed world in not having universal coverage and for having such high-cost health care,” Larry Levitt, the nonpartisan Kaiser Family Foundation’s executive vice president for health policy, told me.
Sanders’s proposal “would be an enormous shift in how we pay for health care, and you have to make a lot of assumptions about how that would work, with a lot of uncertainty,” Levitt continued. “For example, how far down could prices for hospitals, physicians and drugs be pushed? How much more health care would people use if we had universal coverage with no deductibles and co-pays? And how well could the supply of hospitals and doctors adjust to an increase in use of health care? There’s a lot of uncertainty to how all of this would play out. But there’s a fair amount of consensus among economists who’ve looked at it that we could provide universal coverage through a Medicare-for-All-type plan and not pay much more for than we’re currently paying.”
Still, the change would be monumental. “The Sanders proposal would leapfrog every country in the world in creating a more liberal health care system,” Levitt said. “Every other system with universal coverage has at least some out-of-pocket costs for patients. And almost every other country still allows for private insurance.” And insurance companies in Europe, for instance, are often nonprofit, highly regulated and with little to no political power. American insurance companies are a different story, and it seems fair to conjecture that they will not forsake their billions in net earnings without a fight.
Though polling does not reflect an outpouring of love for private insurance, it is the devil Americans know. “There’s fear of change and comfort with what’s known, a bias toward the status quo, and it’s hard to quantify that,” says Topher Spiro, the Center for American Progress’s vice president for health policy. “There’s a real psychological issue that’s appropriate for policymakers to consider. I don’t think the people like us who are putting forth multipayer universal systems are doing so because we think insurers have some sort of superior efficiency or can improve the quality of care. It’s really a concern about how we get there the quickest in terms of political viability and with a minimum of disruption.”
Single-payer advocates play down the difficulty of transitioning into a government-run health care system. As Sanders puts it: “You have Medicare, a popular system that millions of people are already in. It seems to me the easiest way forward to get to universal care is to expand what’s already a popular system. I find it really amazing that people think this isn’t doable when back in 1965 they did Medicare without the technology we have today, and they were able to sign up 19 million people. So of course we can do it.”
But while the Republican efforts to gut Obamacare have bolstered support for a more ambitious health care policy, they have also clearly illustrated one potential downside of such a policy. “Medicare cuts are in Trump’s budget,” Tanden says. “If you’re worried about a Trump administration now, just imagine if the government has control of everyone’s health care. And I say that as a big-government liberal.”
The day before Sanders took to the debate stage in Detroit to defend Medicare for All, I met with him in a conference room at the Doubletree Suites hotel where he was staying. He was seated alone, wearing his customary off-the-rack navy suit and tieless white shirt, flanked by a Starbucks breakfast of coffee, granola and yogurt.
“We’ve got a health care crisis in this country,” he told me as he struggled with the plastic granola container, finally gouging it open with his car keys. Sanders has a reputation for being as beatific as a snapping turtle, but today he was happy(ish) to be discussing the topic that he and DeMoro had succeeded in crowbarring into the national debate. “You’ve heard me talk about F.D.R. in 1944 talking about economic rights as a human right,” he said. “That’s what we’re doing here, and I think with some success: changing consciousness in this country. Now everybody agrees health care is a human right. How you get there is subject to discussion. But that’s where we are.”
Recently Sanders had been campaigning in Las Vegas. While driving through the city, he marveled at the billboards advertising marijuana for sale. “Five years ago, corporations marketing marijuana would have been out of the question,” he said to the aides in his car. “Now they’re not only doing it, but it’s not even remarkable that they’re doing it. Politics change very quickly.”
A not-so-minor refinement to that thought would be: Politics change quickly as long as nothing is standing in the way. Nearly three decades have passed since Sanders and DeMoro began doing battle with the health industry and the political system. “What they do have is, they lie and they have an enormous amount of money — I get that,” Sanders conceded. “But I do think we’re at a moment in history where the American people are sick and tired of the insurance companies and drug companies. And I do believe we can beat them.”
For any movement, the answer to the question of how is not really legislative. The Rev. Martin Luther King Jr. had his dream. RoseAnn DeMoro told me hers recently. “I think it’s time now,” she said, smirking a bit as she studied her glass of white wine. “I think America needs to say to these C.E.O.s: ‘You’ve had your day. You’ve bought your 50 frigging yachts. But it’s over. Now let’s have health care in this country.’ ”

Are hospital mergers a good thing or a bad thing?
Much of the answer to that question depends on what happens after the merger—does the combined organization provide better, more efficient care, or does it use its increased leverage to raise prices? Yet another round of back and forth on this issue took place this week, as the American Hospital Association (AHA) released the results of a study it commissioned from economic analysis firm Charles River Associates (CRA), while a group of academic antitrust specialists countered with their own briefing in response.
The AHA study, based on interviews with select health system leaders and econometric analysis by CRA, shows (surprise, surprise) that consolidation decreases hospital expenses by 2.3 percent, reduces mortality and readmissions, and reduces revenue per admission by 3.5 percent—indicating that the “savings” from consolidation are being passed along to purchasers. The economists, including Martin Gaynor at Carnegie Mellon, Zack Cooper at Yale, and Leemore Dafny at Harvard, countered in their briefing (surprise, surprise) that CRA’s research was biased in favor of hospitals, and cited numerous academic studies that indicate that hospital consolidation drives overall healthcare costs higher.
Beyond the predictable debate, our view is that consolidation can and should lead to better quality and lower prices—but that it largely hasn’t delivered on that promise. The prospect of “integrated care” that’s often touted by consolidation advocates hasn’t materialized in most places, both because hospital executives haven’t pushed hard enough on strategies to produce it, and because the market lacks sufficient incentives to encourage it.

The American Hospital Association released a report stating that hospital acquisitions allow providers to provide better care at a lower cost to patients.
The report, which revisited an analysis concluding similar results three years ago, found acquisitions decrease cost due to the increased size of a combined system as well as clinical standardization.
Specifically, the AHA said hospital acquisitions lead to a 2.3 percent reduction in annual operating expenses at acquired hospitals. The study also said readmission and mortality rates decline at merging hospitals, and acquired hospitals see revenues per admission decline 3.5 percent, suggesting “savings that accrue to merging hospitals are passed on to patients and their health plans.”
However, the AHA’s findings — which were largely based on interviews with leaders of 10 health systems who weren’t randomly surveyed — contradict a wealth of economic data published that argues the opposite.
Last year, researchers found hospitals in monopoly markets, compared to hospitals in markets with four or more competitors, have prices that are 12 percent higher. In markets with four or more competitors, hospitals have lower prices and take on more financial risk, researchers said. Another independent analysis found hospital prices rise after hospitals combine. Researchers have also questioned whether consolidation really leads to better quality.