
Cartoon – Major Breakthrough


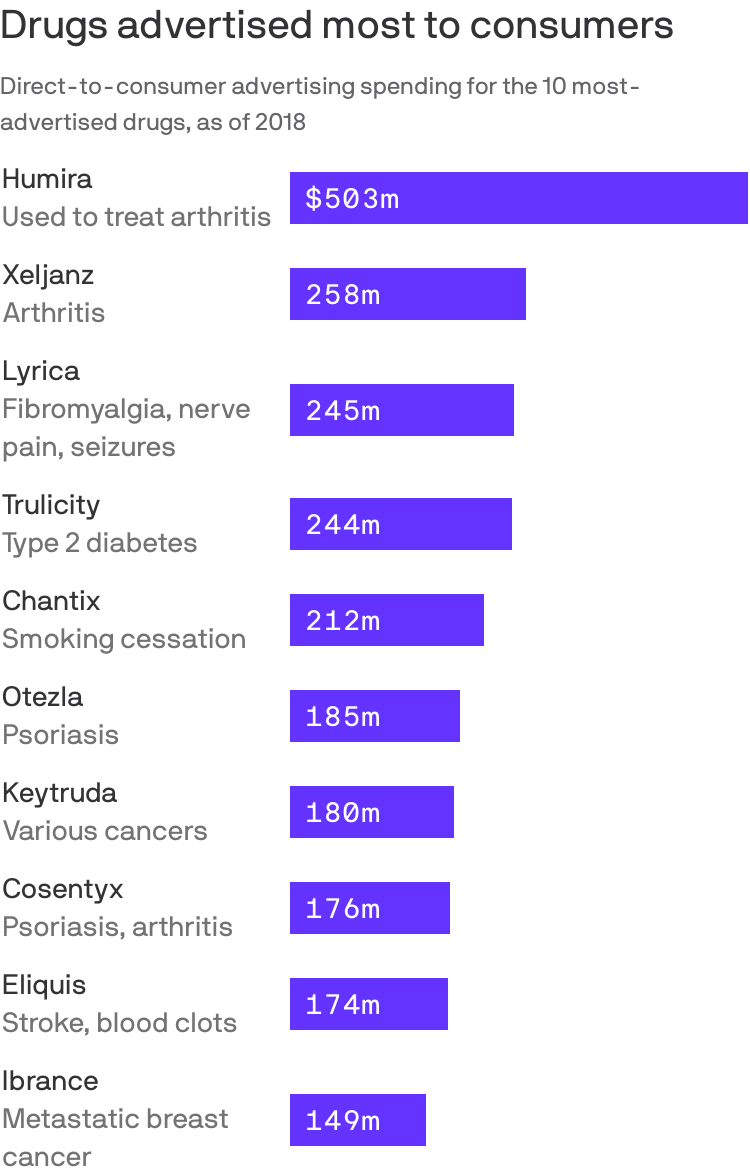
Prescription drugs with some of the highest Medicare spending also had the highest level of direct-to-consumer advertising, a recently-released GAO report found.
By the numbers: The GAO found the Medicare program and its beneficiaries spent nearly $324 billion on prescription drugs advertised to beneficiaries and other consumers between 2016 and 2018.
This amount is more than half (58%) of total Medicare Parts B and D spending on drugs during that time, the most recent data available.
With a $56,000-a-year price tag, Biogen’s newly approved Alzheimer’s drug Aduhelm is dovetailing into the debate on Capitol Hill over how to lower prescription drug prices.
Why it matters: Democrats may be positioning themselves to push policy measures that assign value to drugs and then price them accordingly — a huge potential blow to the pharmaceutical industry.
To truly address its launch price, policymakers have to grapple with big questions the U.S. system currently avoids: How should we determine the value of a drug, and who gets to make that decision?
The bottom line: “Any kind of process for valuing new drugs like Aduhelm take you immediately into the controversial quagmire of how to quantify improvements in quality of life for people,” said KFF’s Larry Levitt.

UPDATE: May 21, 2021: Late Thursday, drug manufacturing giant Eli Lilly filed a motion in an Indiana district court to halt 340B-related monetary penalties, scant days after the Biden administration set a June 1 deadline for biopharmaceutical companies to comply with new conditions in the drug discount program and allow hospital contract pharmacies access to discounted drugs.
The suit alleges a Monday letter from Diana Espinosa, acting head of the Health Resources and Services Administration, gives “no legal explanation or justification for the arbitrary June 1 deadline.”
Lilly previously filed an almost identical lawsuit January 2020. The Indianapolis-based biopharma said it expected the government to follow the briefing schedule outlined in that suit before mandating compliance with 340B and forcing it to pay “substantial and irretrievable sums of money.”
“If the Court ultimately decides Lilly was required to extend 340B pricing to contract pharmacies, Lilly will comply with that decision. Conversely, if the Court ultimately decides manufacturers are not required to extend 340B pricing to contract pharmacies, then we surely expect the government will comply with that decision. But there is no explanation or justification for the government’s attempt to make Lilly pay now, other than to evade this Court’s review and leave Lilly without recourse for such payments,” the motion reads.
In the petition, Lilly, which brought in $6.2 billion in profit last year, alleges the shifting terms of the program are due to HHS director Xavier Becerra bending to political pressure to “take action” against drug manufacturers, as pharmaceutical prices continue to climb.
Lilly asked the district court to temporarily block HHS from moving against Lilly until the drugmaker’s request for a preliminary injunction is resolved; and for an accelerated legal schedule to settle its claims before the looming June deadline.
An HRSA spokesperson declined to comment on the suit.
Providers and drugmakers have sparred for years over the 340B drug discount program that requires pharmaceutical companies to give discounts on outpatient drugs for providers serving low-income communities.
AHA along with five other provider groups in December filed a federal lawsuit against HHS, alleging the department failed to enforce 340B program requirements and allowed actions from drug companies that undermined the program. That lawsuit was later dismissed.
But with the change in administrations, providers now seem to have an ally in the fight.
Previously, as California’s Attorney General, newly minted HHS chief Xavier Becerra led a group of states pushing the agency to force drugmakers to comply with the law late last year.
Provider groups cheered the move after raising the alarm last year that an increasing number of drug companies were refusing to offer discounts to such eligible hospitals.
“The denial of these discounts has damaged providers and patients and must stop. It is vital that these companies immediately begin to repay the millions of dollars owed to these providers,” 340B Health CEO Maureen Testoni said in a statement.
In separate letters to drugmakers, HRSA outlines complaints against them and their actions, ultimately saying their policies violated the statute and resulted in overcharges that need to be refunded. The companies must work to ensure all impacted entities are contacted and efforts are made to pursue mutually agreed upon refund arrangements, according to the letters.
Any additional violations will be subject to a $5,000 penalty for each instance of overcharging under the program’s Ceiling Price and Civil Monetary Penalties final rule.
The American Hospital Association also praised the agency in a release for “taking the decisive action we’ve called for against drug companies that skirt the law by limiting the distribution of certain 340B drugs through community pharmacies.”
Hospitals in the 340B program provide 60% of all uncompensated care in the U.S. and 75% of all hospital care to Medicaid patients, according to 340B Health.

Some countries have stockpiles. Others have nothing. Getting a vaccine means living in the right place — or knowing the right people.
A 16-year-old in Israel can get a vaccine.
So can a 16-year-old in Mississippi.
And an 18-year-old in Shanghai.
But a 70-year-old in Shanghai can’t get one. Older people are at high risk for severe illness from Covid-19. But Chinese officials have been reluctant to vaccinate seniors, citing a lack of clinical trial data. Neither can an 80-year-old in Kenya. Low vaccine supply in many countries means only health care employees and other frontline workers are eligible, not the elderly.
Nor a 90-year-old in South Korea. Koreans 75 and older are not eligible until April 1. Only health care workers and nursing-home residents and staff are currently being vaccinated. The government initially said it was awaiting assurances that the AstraZeneca vaccine was safe and effective for older groups.
Anyone in Haiti.
Anyone in Papua New Guinea.
Anyone in these 67 countries. These countries have not reported any vaccinations, according to Our World in Data. Official figures can be incomplete, but many countries are still awaiting their first doses.
It wasn’t supposed to be like this: Covax, the global vaccine-sharing initiative, was meant to prevent unequal access by negotiating vaccine deals on behalf of all participating nations. Richer nations would purchase doses through Covax, and poorer nations would receive them for free.
But rich nations quickly undermined the program by securing their own deals directly with pharmaceutical companies. In many countries, they have reserved enough doses to immunize their own multiple times over.
Anyone who can afford a smartphone or an internet connection in India and is over 60 can get one. Mostly wealthy Indians are being inoculated in New Delhi and Mumbai, hospitals have reported, since vaccine appointments typically require registering online. Less than half of India’s population has access to the internet, and even fewer own smartphones.
And anyone who can pay $13,000 and travel to the U.A.E. for three weeks and is 65 or older or can prove they have a health condition.
A British travel service catering to the rich offered vaccination packages abroad, and wealthy travelers to the U.A.E. have acknowledged they were vaccinated there.
A member of Congress in the United States. Friends of the mayor of Manaus, Brazil. Lawmakers in Lebanon. A top-ranking military leader in Spain. The extended family of the deputy health minister in Peru. The security detail to the president of the Philippines. Government allies with access to a so-called “V.I.P. Immunization Clinic” in Argentina. Around the world, those with power and connections have often been first in line to receive the vaccine — or have cut the line altogether.
A smoker in Illinois can get one. But not a smoker in Georgia.
A diabetic in the United Kingdom can. A diabetic in Connecticut can’t.
Countries have prioritized different underlying health conditions, with the majority focusing on illnesses that may increase the risk of severe Covid-19. In the U.S., health issues granted higher priority differ from state to state, prompting some people to travel across state borders.
A pregnant woman in New York. Not a pregnant woman in Germany. Up to two close contacts of a pregnant woman in Germany. Pregnant women were barred from participating in clinical trials, prompting many countries to exclude them from vaccine priority groups. But some experts say the risks to pregnant women from Covid-19 are greater than any theoretical harm from the vaccines.
A grocery worker in Texas, no. A grocery worker in Oklahoma, yes.
Many areas aim to stop the virus by vaccinating those working in frontline jobs, like public transit and grocery stores. But who counts as essential depends on where you live.
A police officer in the U.K. A police officer in Kenya. A postal worker in California. A postal worker in North Carolina. A teacher in Belgium. A teacher in Campeche, Mexico. Other jobs have been prioritized because of politics: Mexico’s president made all teachers in the southern state of Campeche eligible in a possible bid to gain favor with the teacher’s union.
Medical staff at jails and prisons in Colombia. A correctional officer in Tennessee. A prisoner in Tennessee. A prisoner in Florida. The virus spread rapidly through prisons and jails, which often have crowded conditions and little protective equipment. But few places have prioritized inoculating inmates.
An undocumented farm worker in Southern California. A refugee living in a shelter in Germany. An undocumented immigrant in the United Kingdom. Britain has said that everyone in the country is eligible for the vaccine, regardless of their legal status.
A Palestinian in the West Bank without a work permit. Despite leading the world in per-capita vaccinations, Israel has so far not vaccinated most Palestinians, unless they have permits to work in Israel or settlements in the occupied West Bank.
An adult in Bogotá, Colombia. An adult in the Amazonian regions of Colombia that border Brazil. In most of Colombia, the vaccine is only available to health care workers and those over 80.
But the government made all adults in Leticia, Puerto Nariño, Mitú and Inírida eligible, hoping to prevent the variant first detected in Brazil from arriving in other areas. A police officer in Mexico City. A teacher in rural Mexico.The government of populist president Andrés Manuel López Obrador has prioritized vaccinating the poor and those in rural communities, despite the country’s worst outbreaks occurring in major cities.
Native populations not federally recognized in the United States. The pandemic has been particularly deadly for Native Americans. But only tribes covered by the Indian Health Service have received vaccine doses directly, leaving about 245 tribes without a direct federal source of vaccines. Some states, including Montana, have prioritized all Native populations.
Indigenous people living on official indigenous land in Brazil.
These 43 countries, mostly high income, are on pace to be done in a year. These 148 countries, mostly low income, are on pace to take until next year or even longer. Countries like the U.S. continue to stockpile tens of millions of vaccine doses, while others await their first shipments.
“The vaccine rollout has been inequitable, unfair, and dangerous in leaving so many countries without any vaccine doses at all,” said Gavin Yamey, director of Duke University’s Center for Policy Impact in Global Health.
“It’s a situation in which I, a 52-year-old white man who can work from home and has no pre-existing medical conditions, will be vaccinated far ahead of health workers or a high-risk person in a middle- or low-income country.”

COVID-19 accelerated a number of trends already brewing in the healthcare industry, and that’s not likely to change this year, according to a new report from CVS Health.
The healthcare giant released its annual Health Trends Report on Tuesday, and the analysis projects several industry trends that are likely to define 2021 in healthcare, ranging from technology to behavioral health to affordability.
“We are facing a challenging time, but also one of great hope and promise,” CVS CEO Karen Lynch said in the report. “As the pandemic eventually passes, its lessons will serve to make our health system more agile and more responsive to the needs of consumers.”
Here’s a look at four of CVS’ predictions:
Behavioral health needs were a significant challenge in healthcare prior to COVID-19, but the number of people reporting declining mental health jumped under the pandemic.
Cara McNulty, president of Aetna Behavioral Health, said in a video attached to the report that it will be critical to “continue the conversation around mental health and well-being” as we emerge from the pandemic and to reduce stigma so people who need help seek it out.
“We’re normalizing that it’s important to take care of our mental well-being,” she said.
Data released in December by GoodRx found that prescription fills for depression and anxiety medications hit an all-time high in 2020. GoodRx researchers polled 1,000 people with behavioral health conditions on how they were navigating the pandemic, and 63% said their depression and/or anxiety symptoms worsened.
McNulty said symptoms to look for when assessing whether someone is struggling with declining mental health include whether they’re withdrawn or agitated or if there’s a notable difference in their self-care routine.
CVS dubbed 2021 “the year of the pharmacist” in its report.
The company expects pharmacists to be a key player in a number of areas, especially in vaccine distribution as that process inches toward broader access. They also offer a key touchpoint to counsel patients about their care and direct them to appropriate services, CVS said.
CVS executives said in the report that they see a significant opportunity for pharmacists to have a positive impact on the social determinants of health.
“We’ve found people are not only open and willing to share social needs with their pharmacists but in many cases, they listen to and act on the advice and recommendations of pharmacists,” Peter Simmons, vice president of transformation, pharmacy delivery and innovation at CVS Health, said in the report.
Revolutionary drugs and therapies are coming to market with eye-popping price tags; it’s not uncommon to see new pharmaceuticals priced at $1 million or more. For pharmacy benefit managers, this poses a major cost challenge.
To address those prices, CVS expects value-based contracting to take off in a big way. And drugmakers are comfortable with the idea, according to the report. Novartis, for example, is offering insurers a five-year payment plan for its $2 million gene therapy Zolgensma, with refunds available if the drug doesn’t achieve desired results.
CVS said the potential for these therapies is clear, but many payers want to see some type of results before they fork over hundreds of thousands.
“Though the drug may promise to cure these patients for life, these are early days in their use,” said Joanne Armstrong, M.D., enterprise head of women’s health and genomics at CVS Health, in the report. “What we’re saying is, show us the clinical value proposition first.”
CVS said it’s also offering a stop-loss program for gene therapy to self-funded employers contracted with Aetna and/or Caremark to assist them in capping the expenses associated with these drugs.
Diabetes risk is higher among vulnerable populations, such as Black patients, and addressing it will require local and community-based solutions, CVS executives said in the report. Groups at the highest risk for the disease are less likely to live in areas with easy access to a supermarket, for example, which boosts their risk of unhealthy eating, according to the report.
The two key hurdles to addressing this issue are access and affordability. The rise in retail clinics and ambulatory care centers can get at the access issue, as they can offer a way to better meet patients where they are.
At CVS’ MinuteClinics, patients can walk in and receive a number of services to assist them in managing diabetes, including screenings, consultations with providers and connections to diabetes educators who can assist with lifestyle changes.
Retail locations can also assist with medication costs, creating a one-stop-shop experience that’s easier for many diabetes patients to slot into their daily lives, CVS said.
“Diabetes is a case study in how a more connected experience can translate to simpler, affordable and more accessible care for underserved communities,” said Dan Finke, executive vice president of CVS Health and president of its healthcare benefits division.

The COVID-19 pandemic has accelerated the pace of artificial intelligence adoption, and healthcare leaders are confident AI can help solve some of today’s toughest challenges, including COVID-19 tracking and vaccines.
The majority of healthcare and life sciences executives (82%) want to see their organizations more aggressively adopt AI technology, according to a new survey from KPMG, an audit, tax and advisory services firm.
Healthcare and life sciences (56%) business leaders report that AI initiatives have delivered more value than expected for their organizations. However, life sciences companies seem to be struggling to select the best AI technologies, according to 73% of executives.
As the U.S. continues to navigate the pandemic, life sciences business leaders are overwhelmingly confident in AI’s ability to monitor the spread of COVID-19 cases (94%), help with vaccine development (90%) and aid vaccine distribution (90%).
KPMG’s AI survey is based on feedback from 950 business or IT decision-makers across seven industries, with 100 respondents each from healthcare and life sciences companies.
Despite the optimism about the potential for AI, executives across industries believe more controls are needed and overwhelmingly believe the government has a role to play in regulating AI technology. The majority of life sciences (86%) and healthcare (84%) executives say the government should be involved in regulating AI technology.
And executives across industries are optimistic about the new administration in Washington, D.C., with the majority believing the Biden administration will do more to help advance the adoption of AI in the enterprise.
“We are seeing very high levels of support this year across all industries for more AI regulation. One reason for this may be that, as the technology advances very quickly, insiders want to avoid AI becoming the ‘Wild Wild West.’ Additionally, a more robust regulatory environment may help facilitate commerce. It can help remove unintended barriers that may be the result of other laws or regulations, or due to lack of maturity of legal and technical standards,” said Rob Dwyer, principal, advisory at KPMG, specializing in technology in government.
Healthcare and pharma companies seem to be more bullish on AI than other industries are.
The survey found half of business leaders in industrial manufacturing, retail and tech say AI is moving faster than it should in their industry. Concerns about the speed of AI adoption are particularly pronounced among small companies (63%), business leaders with high AI knowledge (51%) and Gen Z and millennial business leaders (51%).
“Leaders are experiencing COVID-19 whiplash, with AI adoption skyrocketing as a result of the pandemic. But many say it’s moving too fast. That’s probably because of current debate surrounding the ethics, governance and regulation of AI. Many business leaders do not have a view into what their organizations are doing to control and govern AI and may fear risks are developing,” Traci Gusher, principal of artificial intelligence at KPMG, said in a statement.
Healthcare organizations are ramping up their investments in AI in response to the COVID-19 pandemic. In a Deloitte survey, nearly 3 in 4 healthcare organizations said they expect to increase their AI funding, with executives citing making processes more efficient as the top outcome they are trying to achieve with AI.
Healthcare executives say current AI investments at their organizations have focused on electronic health record (EHR) management and diagnosis.
To date, the technology has proved its value in reducing errors and improving medical outcomes for patients, according to executives. Around 40% of healthcare executives said AI technology has helped with patient engagement and also to improve clinical quality. About a third of executives said AI has improved administrative efficiency. Only 18% said the technology helped uncover new revenue opportunities.
But AI investments will shift over the next two years to prioritize telemedicine (38%), robotic tasks such as process automation (37%) and delivery of patient care (36%), the survey found. Clinical trials and diagnosis rounded out the top five investment areas.
At life sciences companies, AI is primarily deployed during the drug development process to improve record-keeping and the application process, the survey found. Companies also have leveraged AI to help with clinical trial site selection.
Moving forward, pharmaceutical companies will likely focus their AI investments on discovering new revenue opportunities in the next two years, a pivot from their current strategy focusing on increasing profitability of existing products, according to the survey. About half of life sciences executives say their organizations plan to leverage AI to reduce administrative costs, analyze patient data and accelerate clinical trials.
Industry stakeholders are taking steps to advance the use of AI and machine learning in healthcare.
The Consumer Technology Association (CTA) created a working group two years ago to develop some standardization on definitions and characteristics of healthcare AI. Last year, the CTA working group developed a standard that creates a common language so industry stakeholders can better understand AI technologies. A group also recently developed a new standard to advance trust in AI solutions.
On the regulatory front, the U.S. Food and Drug Administration (FDA) last month released its first AI and machine learning action plan, a multistep approach designed to advance the agency’s management of advanced medical software. The action plan aims to force manufacturers to be more rigorous in their evaluations, according to the FDA.

COVID-19 vaccine makers are under intense pressure to rev up production, but the scale of the challenge is unprecedented — and the speed of production is limited.
Why it matters: Even with help from the federal government and outside companies, vaccine-making is a complex, time-consuming biological process. That limits how quickly companies like Pfizer and Moderna can accelerate their output even during a crisis.
The big picture: With new, more transmissible variants emerging, we’re in a race to get shots into more people’s arms. What would normally take years to set up is being compressed into less than a year, leaving engineers to adapt manufacturing processes on the fly.
Between the lines: Making vaccines is complex, and the process can be hindered at different steps.
How it works: Axios got a deep dive into the making of Pfizer’s vaccine, a three-phase process that takes weeks from start to finish and involves three different facilities.
1) DNA manufacturing: At a plant near St. Louis, Mo., Pfizer produces DNA that encodes messenger RNA — instructions for cells to make part of the spike protein on the surface of the coronavirus. That primes the immune system to defend against future encounters with the virus.
2) Making the mRNA: In Andover, the template DNA is incubated with messenger RNA building blocks in a reactor to make the mRNA. Pfizer has been making two, 40-liter batches per week — up to 10 million doses worth —but expects to double that to four batches per week.
3) Formulating the vaccine: In Kalamazoo, the mRNA and lipid nanoparticles (oily envelopes that deliver mRNA to cells in the body) are combined and go through a series of filtrations.
Where it stands: Both Pfizer and Moderna say they’re on track to meet their commitments to deliver 200 million doses each to the U.S. over the first half of the year.
The latest: The Biden administration said last week that it will use its wartime powers under the Defense Production Act to give Pfizer priority access to critical components such as filling pumps and filtration units to try to help address bottlenecks.
Ordering other drug manufacturers to stand up manufacturing lines to whip up extra batches of Pfizer’s or Moderna’s vaccines is not an efficient or practical way for the federal government to quickly increase supplies, some experts say.
What to watch: Johnson & Johnson has requested emergency use authorization from the FDA for its single-dose vaccine, but is reportedly lagging in production, the NYT first reported last month.
https://www.washingtonpost.com/business/2021/02/12/opioid-settlement-tax-refund/?arc404=true

Four companies that agreed to pay a combined $26 billion to settle claims about their roles in the opioid crisis plan to deduct some of those costs from their taxes and recoup around $1 billion apiece.
In recent months, as details of the blockbuster settlement were still being worked out, pharmaceutical giant Johnson & Johnson and the “big three” drug distributors — McKesson, AmerisourceBergen and Cardinal Health —all updated their financial projections to include large tax benefits stemming from the expected deal, a Washington Post analysis of regulatory filings found.
In one example, Dublin, Ohio-based drug distributor Cardinal Health said earlier this month it planned to collect a $974 million cash refund because it claimed its opioid-related legal costs as a “net operating loss carryback” — a tax provision Congress included in last year’s coronavirus bailout package as a way of helping companies struggling during the pandemic.
The deductions may deepen public anger toward companies prosecutors say played key roles in a destructive public health crisis that kills tens of thousands of Americans every year. In lawsuits filed by dozens of states and local jurisdictions, public officials have argued that the companies, among other corporate defendants, flooded the country with billions of highly addictive pills and ignored signs they were being steered to people who abused them.
Under the terms of the proposed settlement — which is being finalized and will ultimately be subject to federal court approval — the four companies would pay between $5 billion and $8 billion each to reimburse communities for the costs of the health crisis. Plaintiffs who support the proposal say it will resolve a highly complex litigation process and make funds available to communities and individuals still struggling with addiction.
Others including Greg McNeil, whose son became addicted to opioids and died from an overdose, have said $26 billion is only a small fraction of the epidemic’s financial toll and argue the proposal doesn’t include what many family members of opioid victims want the most: an admission of guilt.
All four firms disavow any wrongdoing or legal responsibility. The companies have said they produced government-approved prescription pills, distributed them to registered pharmacies and took steps to try to prevent their misuse.
U.S. tax laws generally restrict companies from deducting the cost of legal settlements from their taxes, with one major exception: Damages paid to victims as restitution for the misdeeds can usually be deducted. Still, Congress has placed stricter limits on such deductions in recent years, and some tax experts say the Internal Revenue Service could challenge the companies’ attempts to deduct opioid settlement costs.
Harry Cullen, a Brooklyn-based activist who has worked to hold drug companies accountable for the epidemic, said it is “incredibly insulting” that companies would try deduct the settlement payments. “As if they are donating it to these people who they harmed in the first place.”
Erich Timmerman, a spokesman for Cardinal Health, said in a statement that the company’s tax deductions are permissible under federal law. He also pointed to a statement chief executive Mike Kaufmann made in November, when he said Cardinal takes its role in the pharmaceutical supply chain seriously and remains “committed to being part of the solution to this epidemic.”
AmerisourceBergen declined to comment on its taxes but said in a statement the company takes steps to mitigate the diversion of prescription drugs, including by refusing service to customers it sees as a risk and by making daily reports to federal drug officials.
Johnson & Johnson declined to comment on the opioid settlement and tax deductions beyond its regulatory filings.A spokeswoman for McKesson did not respond to multiple requests for comment.
Cardinal Health’s use of the “carryback” tax break draws attention to what some see as a shortcoming of the $2 trillion U.S. coronavirus bailout known as the Cares Act. In their haste to funnel cash benefits to businesses facing economic peril, lawmakers made billions of dollars in tax breaks broadly available to any company, regardless of whether it suffered during the pandemic.
Cardinal, a company with a $15 billion market capitalization and $4 billion in available cash, surpassed Wall Street expectations for its most recent earnings period. Last week, CEO Kaufmann told investors a rebound in medical treatments and procedures had revived demand for Cardinal’s health devices and drugs. He said the company was boosting its investment in sophisticated supply-chain technology.
On the same day, Cardinal said it was filing for a tax break using the Cares Act provision and expected a nearly $1 billion cash refund from the IRS within the next 12 months. The company plans to pay $6.6 billion in the settlement.
Francine J. Lipman, a tax professor at the University of Nevada at Las Vegas, said Cardinal Health appears to be “getting a bit of a windfall from laws that Congress intended to help companies that are suffering due to a pandemic.”
The “carryback” tax break permits any company that lost money in 2018, 2019 or 2020 to apply those losses to previous, more profitable years. Some form of this provision has been permitted by the U.S. tax code for over a century to help businesses that face ups and downs to even out their taxes.
The Cares Act raised the limit on the amount of losses companies can use to offset taxes and permitted them to apply those losses to earlier periods. Because the corporate tax rate was higher before 2018, companies with recent losses can increase tax refunds they received before that year by up to 67 percent.
Cardinal estimated in August it expected to deduct $488 million from the expected opioid legal settlement. But in its Feb. 5 filing, the company said the amount probably would be higher in part because the Cares Act permitted it to carry back losses related to the opioid litigation to previous years when the tax rate was higher.
UNLV’s Lipman said Cardinal’s decision to apply for a tax refund before any legal settlement has been finalized could face scrutiny from the IRS. Deductions must be made against business expenses that are shown to have “economic effect,” she said, which may preclude deductions against future, unpaid legal settlements.
Timmerman, Cardinal’s spokesman, said the company has already recorded a loss related to the opioid litigation because Cardinal insures itself through a wholly-owned insurance subsidiary. The opioid litigation caused a loss to the insurance company’s reserve, and that is the loss that Cardinal is deducting, he said.
“Tax and accounting rules applicable to insurance companies, including self-insurance companies, require recognition of loss when an insurance reserve is set, thus establishing economic effect, even if the underlying settlement is not final,” Timmerman said.
The three other companies involved in the $26 billion settlement have estimated the tax benefits of the deal but have not filed for tax refunds. They all said the tax benefits could be lower if courts or regulators determined some or all of the payments are not tax-deductible.
McKesson, which expects to pay $8.1 billion in the settlement, said in a Feb. 2 filing that the actual cost of the deal would be $6.7 billion after taxes, implying a $1.4 billion tax benefit. The company also said $497 million in tax benefits were “uncertain” because of the “uncertainty in connection with the deductibility of opioid related litigation and claims.”
AmerisourceBergen, which anticipates a $6.6 billion settlement payment, said in November it expects a $1.1 billion tax benefit. The company said an additional $371.5 million tax benefit was possible but “uncertain.”
“A settlement has not been reached, and, therefore, we applied significant judgment in estimating the ultimate amount of the opioid litigation settlement that would be deductible,” the company said.
Matthew Gardner, a senior fellow at the nonprofit Institute on Taxation and Economic Policy, said these disclaimers suggest the companies are making conservative estimates. “That’s one way of saying they are likely going to claim even bigger tax benefits in their tax returns than they are showing on their financial statements,” he said.
Whether the payments will be deductible may hinge on specific word choices in the final terms of the settlement. Though recent changes to the tax code have attempted to close loopholes that permit companies to deduct taxes when they have committed wrongdoing, many companies now push to make sure their settlements include a “restitution” payment for victims — the “magic word” that often qualifies them for deductions, Gardner said.
In previous opioid-related settlements local governments reached with McKesson, Purdue Pharma and Teva Pharmaceuticals, the companies admitted no fault and agreed to restitution payments that appeared to qualify them for tax deductions, USA Today reported in 2019.
Johnson & Johnson has said it expects it could deduct as much as 21.4 percent of its $5 billion share of the settlement, which would mean a roughly $1.1 billion tax benefit. However, the company said last summer that the deductible amount may be lower if a regulation proposed by the IRS last year came into effect.
The rule, which did take effect Jan. 20, requires companies to meet a long list of specific criteria to qualify government settlements for tax deductions.

In 2019, The Post analyzed a database maintained by the Drug Enforcement Administration that tracks the path of every pain pill sold in the United States. The database shows that America’s largest drug companies distributed 76 billion oxycodone and hydrocodone pain pills across the country between 2006 and 2012 as the nation’s deadliest drug epidemic spun out of control.
McKesson, Cardinal Health and AmerisourceBergen distributed 44 percent of the nation’s oxycodone and hydrocodone pills — the two most abused prescription opioid drugs — during that time.
An investigation by The Post last year found that near the peak of U.S. opioid production, a Johnson & Johnson subsidiary was manufacturing enough oxycodone and hydrocodone to capture half or more of the U.S. market. The company also lobbied for years to help persuade regulators to loosen a narcotics import rule, allowing Johnson & Johnson’s U.S. subsidiary to produce rising amounts of opioids out of potent poppies harvested by its Tasmanian subsidiary, The Post found.
Attorneys for Johnson & Johnson have said its opioid-producing subsidiaries did not cause the United States’ addiction crisis, that the companies were heavily regulated, and that such companies play only a “peripheral role in the multibillion-dollar market for prescription opioids.”

As happened with cars in the 1960s, price competition among brand-name drugs is hard to find.
Before 1973, when the Arab oil embargo upended the U.S. auto industry, Americans witnessed an annual ritual by carmakers. In the late summer, the Big Three — Ford, Chrysler, and General Motors — would release sticker prices for their products, always showing increases, of course.
Almost always, the increases from each company for similar models were nearly identical. If one company’s was out of line — substantially bigger or smaller than its erstwhile competitors’ — it quickly made an adjustment. Explicit collusion to fix prices was never proven, but the effect for consumers was the same.
Now, researchers report that something very similar seems to be occurring for big-market brand-name drugs, including anti-diabetic medications and blood thinners.
Average wholesale prices for products in five classes — direct-acting oral anticoagulants (DOACs), P2Y12 inhibitors, glucagon-like peptide-1 (GLP-1) agonists, dipeptidyl dipeptidase-4 (DPP-4) inhibitors, and sodium-glucose transport protein-2 (SGLT-2) inhibitors — increased in “lock-step” each year from 2015 to 2020, according to Joseph Ross, MD, of Yale University in New Haven, Connecticut, and colleagues writing in JAMA Network Open.
These increases ranged from annual averages of 6.6% for DDP4 inhibitors to 13.5% for P2Y12 inhibitors — far outpacing not only inflation in general, but even the 2.1% average for all prescription drugs.
Within each class, Kendall τb correlation coefficients for average wholesale prices were as follows:
“These results suggest there was little price competition among the sponsors of these products,” Ross and colleagues wrote.
Although the analysis came with significant limitations — it didn’t account for rebates or other discounts, for example — the researchers said some patients must suffer from these increases.
“Rebates, list prices, and net prices have been growing for brand-name medications, and rebate growth has been shown to positively correlate with list price growth, thereby impacting costs faced by patients paying a percentage of (or the full) list price,“ the group noted. “Therefore, the lock-step price increases of brand-name medications, without evidence of price competition, raise concerns and would be expected to adversely affect patient adherence to medications and thus clinical outcomes.”
For the car buyers, the solution to lock-step price increases was imposed from outside: soaring gas prices in the mid-1970s prompted demand for vehicles with better fuel economy than domestic makers were prepared to sell. That opened the market to Japanese cars that not only got better mileage, but were also more reliable and (in many cases) cheaper than Big Three products. Thus ended Detroit’s ability to set prices.
How to rein in Big Pharma is less clear. For their part, Ross and colleagues suggested policies to limit such lock-step price hikes, shortened patent exclusivity periods, and faster introduction of generic equivalents.