
Cartoon – Honest Leadership Assessment
Cartoon – Natural Leadership
Cartoon – Lonely at the Top
Cartoon – An Insincere Gesture
Cartoon – Betting on Management
Hospital margins ‘well below sustainable levels’: Kaufman Hall

Hospitals across the U.S. saw their operating margins remain negative for the second consecutive month in February as they continued to feel the repercussions of the winter omicron surge, according to Kaufman Hall’s “National Hospital Flash Report: March 2022” posted March 28.
The median operating margin in February was -3.45 percent, up from -4.52 percent in January, but “still well below sustainable levels,” Kaufman Hall said.
Kaufman Hall said the improvement in hospital margin was driven by disproportionate increases among several hospitals that saw margin gains, but most hospitals reported margin declines in February. Specifically, the median operating margin was down 11.8 percent month over month.
“The second month of 2022 brought further challenges for the nation’s hospitals and health systems,” Kaufman Hall said. “Overall, the year is off to a difficult start.”
Kaufman Hall noted that patient days were down 13.3 percent month over month, and fewer severely ill COVID-19 patients also contributed to shorter hospital stays as the average length of stay dropped 5.3 percent month over month.
Hospitals’ gross operating revenue also decreased 7.4 percent compared to January 2022, with outpatient revenue falling 5 percent and inpatient revenue declining 19.3 percent.
Kaufman Hall noted that hospitals saw some improvement month over month in terms of expenses. Total expenses per adjusted discharge fell 4.5 percent compared to January, labor expense per adjusted discharge fell 6.1 percent and non-labor expenses per adjusted discharge was down 3.6 percent. However, Kaufman Hall noted that year over year, expenses are still up significantly, with total adjusted expense per adjusted discharge rising 10.4 percent compared to February 2021.
Is it the beginning of the end of CON?
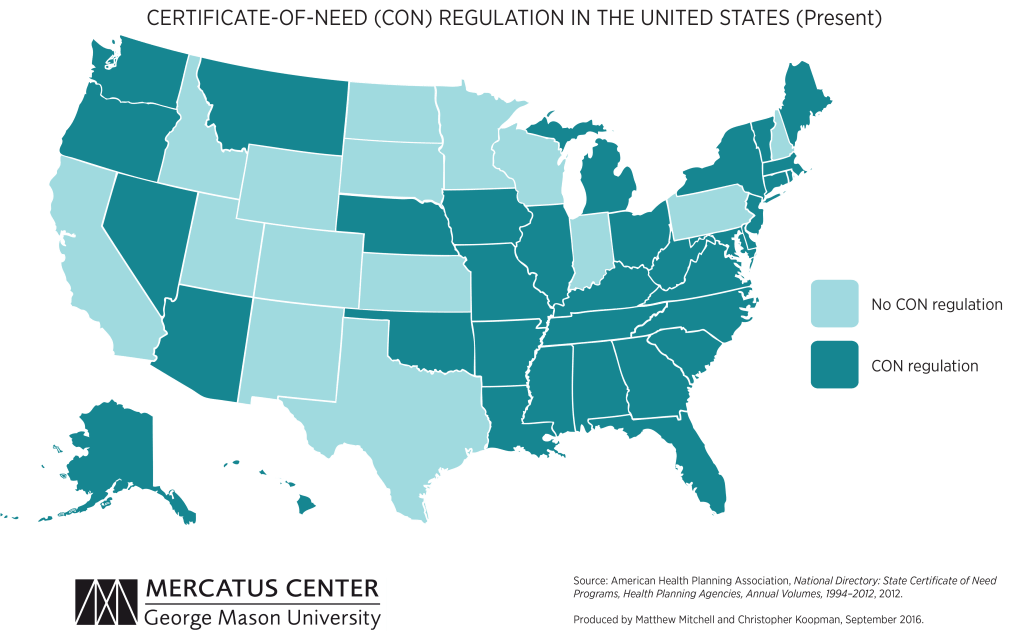
We’re picking up on a growing concern among health system leaders that many states with “certificate of need” (CON) laws in effect are on the cusp of repealing them. CON laws, currently in place in 35 states and the District of Columbia, require organizations that want to construct new or expand existing healthcare facilities to demonstrate community need for the additional capacity, and to obtain approval from state regulatory agencies. While the intent of these laws is to prevent duplicative capacity, reduce unnecessary utilization, and control cost growth, critics claim that CON requirements reduce competition—and free market-minded state legislators, particularly in the South and Midwest, have made them a target.
One of our member systems located in a state where repeal is being debated asked us to facilitate a scenario planning session around CON repeal with system and physician leaders. Executives predicted that key specialty physician groups would quickly move to build their own ambulatory surgery centers, accelerating shift of surgical volume away from the hospital.
The opportunity to expand outpatient procedure and long-term care capacity would also fuel investment from private equity, which have already been picking up in the market. An out-of-market health system might look to build microhospitals, or even a full-service inpatient facility, which would be even more disruptive.
CON repeal wasn’t all downside, however; the team identified adjacent markets they would look to enter as well. The takeaway from our exercise: in addition to the traditional response of flexing lobbying influence to shape legislative change, the system must begin to deliver solutions to consumers that are comprehensive, convenient, and competitively priced—the kind of offerings that might flood the market if CON laws were lifted.
Payer contracts, physician pay still anchored in fee-for-service
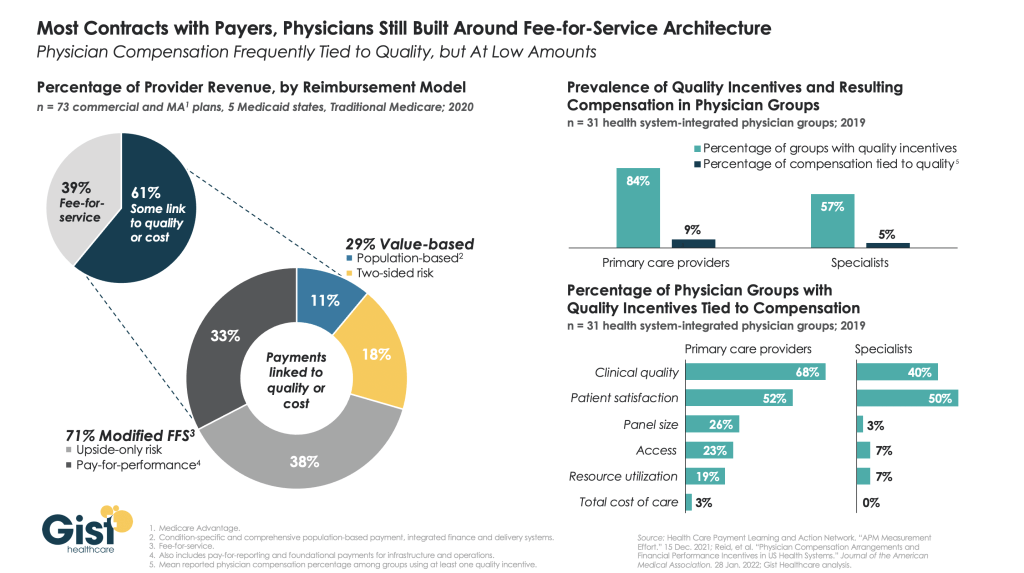
The healthcare industry has made some strides in the “journey to value” across the last decade, but in reality, most health systems and physician groups are still very much entrenched in fee-for-service incentives.
While many health plans report that significant portions of their contract dollars are tied to cost and quality performance, what plans refer to as “value” isn’t necessarily “risk-based.”
The left-hand side of the graphic below shows that, although a majority of payer contracts now include some link to quality or cost, over two-thirds of those lack any real downside risk for providers.
Data on the right show a similar parallel in physician compensation. While the majority of physician groups have some quality incentives in their compensation models, less than a tenth of individual physician compensation is actually tied to quality performance.
Though myriad stakeholders, from the federal government to individual health systems and physician groups, have collectively invested billions of dollars in migrating to value-based payment over the last decade, we are still far from seeing true, performance-based incentives translate into transformation up and down the healthcare value chain.
Three companies combine in kidney care merger
Dialysis giant Fresenius Medical Care is creating a new $2.4B company by combining its US value-based care division, Fresenius Health Partners, with nephrologist network InterWell Health, and digital-first kidney care startup Cricket Health. Cricket Health CEO Robert Sepucha is set to lead the new company, which will be named InterWell Health, assuming the deal closes in the second half of 2022 as expected.
The Gist: This move will enable Fresenius to move further up the renal care delivery chain, managing patients with earlier stage chronic kidney disease before they need dialysis. Fresenius says the new company will more than triple its total addressable market in the US, from $50B to around $170B.
Seeing an opportunity to disrupt the dialysis market, which has been dominated by for-profit giants Fresenius and DaVita, significant capital has been flowing to numerous disruptors in the kidney care space who aim to bring care closer to consumers. Medicare, which spends nearly $115B annually on chronic kidney disease, is testing new payment models aimed at delaying the need for dialysis, as well as moving care into patients’ homes.
But whether Fresenius’s latest moves will make a significant difference in lowering the cost of kidney care remains to be seen.






