
Author Archives: henrykotula
Cartoon – Waiting for the Perfect Situation
Cartoon – The Illusion of Strategy
Cartoon – Understanding Financial Statements
Cartoon – Market Consolidation
Cartoon – Consolidation
FTC sues to block Rhode Island’s largest health systems from merging

Dive Brief:
- The Federal Trade Commission is suing to block Rhode Island’s two largest health systems from merging, alleging the tie-up between Lifespan and Care New England would increase prices and diminish the quality of care.
- In the state’s own review, Rhode Island’s attorney general said the union would result in “extraordinary market power” and denied the merger application under state law that requires a review of such tie-ups. Rhode Island’s attorney general will join FTC’s federal lawsuit seeking to block the deal.
- The FTC alleges that, together, Lifespan and Care New England would control at least 70% of Rhode Island’s market for inpatient hospital services and also reduce competition in several nearby Massachusetts communities.
Dive Insight:
The union between Lifespan, the state’s largest health system, and Care New England, the second largest, quickly raised alarms in Rhode Island.
A 25-page report from the state’s insurance department found that the merger would “significantly alter” the state’s healthcare market, which currently enjoys a “relatively competitive” market. State regulators were also concerned about the control the new system would have over physician services. Given these risks, the state insurance commissioner proposed a set of conditions on the deal including price caps. Health system executives were open to working under certain conditions.
However, executives seemed surprise by Thursday’s announcement that the deal to create an integrated academic medical system with Brown University at the forefront would be blocked.
“On four separate occasions in prior years, the FTC reviewed the same proposed merger and allowed it to proceed,” a joint statement released Thursday said. The management teams said they offered up 30 conditions to regulators to satisfy antitrust concerns about the merger, “but neither the FTC or the AG ever discussed these conditions or others with the two systems prior to today’s decisions,” according to the statement.
After flirting with the idea of combining the systems for years, Lifespan and Care New England inked a deal to merge last February after the coronavirus pandemic revived talks.
The two touted the deal as a way to create an integrated academic health system with Brown University’s medical school in a central role. Brown University committed $125 million to the creation of the new system.
However, FTC commissioners voted unanimously to block the union over concerns it would extinguish competition between the two.
And although regulators have long leaned on the argument that hospital mergers lead to higher prices, a joint letter from FTC Chair Lina Khan and Commissioner Rebecca Kelly Slaughter points to the harmful effects consolidation has on labor markets, an argument growing in importance within the agency.
“Just as we want firms to compete with each other to sell goods and services to their customers, we want employers to compete with each other to attract and retain workers,” the letter states. “Indeed, there is a growing body of empirical research about the potential for competitive harm to labor markets from consolidation and concentration.”
The news follows reports that the Department of Justice is preparing to sue to stop UnitedHealth Group’s blockbuster acquisition of Change Healthcare, a healthcare technology firm. Concerned about the “massive consolidation” of healthcare data, the American Hospital Association urged antitrust regulators to thoroughly examine the proposed transaction in a letter sent to DOJ last spring.
After taking office, President Joe Biden has signaled his administration would take an aggressive antitrust stance, including getting tough on hospital mergers. Last summer, the president issued an executive order that called on antitrust regulators to “review and revise” merger guidelines to ensure patients are not harmed by proposed deals.
Biden specifically called out the healthcare industry, rife with consolidation and accompanying research that shows hospital unions lead to higher prices.
“Thanks to unchecked mergers, the ten largest healthcare systems now control a quarter of the market,” the release from the White House said.
Still, the FTC has become overwhelmed by the sheer number of proposed transactions. In August, the agency said it was hit by a “tidal wave” of merger filings and warned applicants it may not vet all submissions before the applicable deadlines. But in letters sent to merging companies, the FTC warned the delay should not be interpreted as a green light for any deal.
“Companies that choose to proceed with transactions that have not been fully investigated are doing so at their own risk,” the regulator said in a statement.
House Republicans press HHS to end COVID-19 emergency, but hospitals want extension

House Republicans are demanding the Biden administration starts winding down the COVID-19 public health emergency, while hospital lobbying groups are pressing it to do the opposite.
A group of more than 70 House Republicans wrote Thursday to Department of Health and Human Services (HHS) Secretary Xavier Becerra asking to start the process to wind down the COVID-19 public health emergency (PHE), which was recently extended until April. At the same time, several hospital advocacy groups are hoping the agency keeps the PHE beyond this spring and wants a 60-day notice as to when it will end.
“Although the PHE was certainly necessary at the outset of the pandemic, it was always meant to be temporary,” according to the GOP letter led by Rep. Cathy McMorris Rodgers, R-Washington, ranking member of the House Energy and Commerce Committee.
Republicans want HHS to release a concrete timeline for when the agency plans to exit the PHE.
“We recognize that the PHE cannot end overnight, and that certain actions must be taken to avoid significant disruption to patients and healthcare providers, including working with Congress to extend certain policies like maintaining access to telehealth services for our nation’s seniors,” the letter added.
The PHE granted major flexibilities for providers to get reimbursed by Medicare for telehealth, but those powers will go away after the PHE. It also gave flexibility on several reporting requirements and eased other regulatory burdens.
Another major issue is that states are going to be able to start eligibility redeterminations for Medicaid, which have been paused since the PHE went into effect in January 2020. State Medicaid directors are seeking a heads-up on when the emergency will go away, as states can start to disenroll ineligible beneficiaries after the PHE expires.
Republicans also want Becerra to cite any programs that should be made permanent, and they want “swift action” to lift all COVID-19 vaccine mandates.
The Supreme Court upheld the Biden administration’s healthcare worker vaccine mandate, overturning a lower court’s stay that affected half of the country. The Centers for Medicare & Medicaid Services has deadlines for states to comply with the vaccination mandate, and facilities that don’t fully comply could risk losing participation in Medicare and Medicaid.
The Republicans charge that the mandates have not “stopped the spread of COVID-19 but have alienated many Americans and have caused staff shortages at hospitals and other healthcare facilities.”
Key drivers of the staff shortages, however, have been a massive surge of the virus overwhelming facilities caused by the omicron variant along with increased expenses facilities have faced for temporary nursing staff. Those lingering expenses are the reason hospital groups are pressing for HHS to do the opposite and extend the PHE beyond April.
The Federation of American Hospitals (FAH) also wrote to Becerra Thursday (PDF) seeking to continue to extend the PHE “well beyond its current expiration date in April 2022.” Even though the omicron surge appears to be easing, the virus is still creating major operational challenges for providers, FAH said.
It also wants the administration to give hospitals a 60-day heads-up when it plans to end the PHE.
“Unwinding the complex web of PHE waiver-authorized operations, programs and procedures—which will have been in place and relied on for more than two years—is a major undertaking that, if rushed, risks destabilizing fragile healthcare networks that patients rely on for care,” the letter said.
The American Hospital Association also wrote to congressional leaders Tuesday seeking for more relief from Congress to help systems overcome staffing shortages that have exacerbated due to the omicron surge.
“The financial pressures hospitals and health systems faced at the beginning of the public health emergency continue, with, for example, ongoing delays in non-emergent procedures, in addition to increased expenses for supplies, medicine, testing and protective equipment,” the letter said.
FAH President Chip Kahn told Fierce Healthcare on Friday that the issues Republicans address in the letter are different from the priorities of the FAH, namely that the association doesn’t focus on mask or vaccine mandates.
“What we are saying is that the PHE has many aspects to it, and so … we think [it] should be extended, but if you don’t then we need to have a lengthy or carefully thought through transition,” Kahn said.
He added that Becerra’s predecessor, acting Secretary Eric Hargan, told providers that they would get a 60-day notice before the end of the PHE. That deadline for such a 60-day notice is Feb. 15.
Kahn said he understands the administration may be under political pressure to end the emergency, but prior notice is absolutely needed.
“I don’t know how they will respond but if they do choose to pull out, we just want to make sure that it doesn’t leave anything behind,” he said.
UnitedHealth was 2021’s most profitable payer
UnitedHealth Group was the most profitable payer in 2021, bringing in more than double the profit of its next-closest competitor with $17.3 billion in earnings.
CVS Health recorded the second-highest profit for the year among six major national insurers, earning $7.9 billion. CVS did bring in the highest revenue for the year, though, edging out UnitedHealth with $292.1 billion.
UHG reported $287.6 billion in revenue for 2021, according to the company’s earnings report.
Both healthcare giants expect to top $300 billion in revenue this year, according to their forecasts.
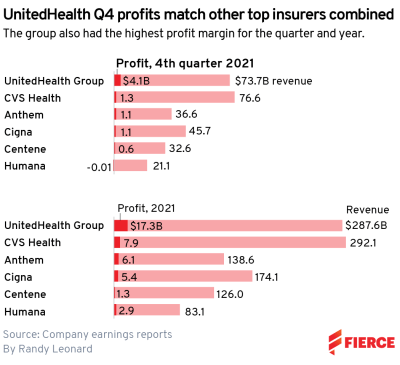
UnitedHealth was also the fourth quarter’s most profitable company, raking in $4.1 billion, which matched what its competitors earned combined, according to the filings.
UnitedHealth Group’s results represented significant growth over both the full-year and fourth quarter of 2020. According to its earnings report, this was driven in part by gains in Medicare Advantage and Medicaid at UnitedHealthcare as well as another quarter of double-digit growth at Optum.
CVS was also the next-highest earner in Q4, with $1.3 billion in profit on $76.6 billion in revenue. UHG was just behind on revenue with $73.7 billion.
CVS Health executives said that the retail business outperformed expectations in the fourth quarter amid increased demand for COVID-19 tests and booster shots.
The healthcare giant performed 32 million tests and 59 million vaccine doses over the course of the year, with 8 million tests and 20 million vaccinations reported in the fourth quarter alone.
While CVS and UnitedHealth duked it out for the top spot, all six of the big national payers were profitable for 2021, though Humana did post a $14 million loss for the fourth quarter.
Centene Corporation lands in sixth place for the year in profitability, bringing in $1.3 billion in profit on $126 billion in revenue. It also reported $599 million in profit for Q4.
Humana earned $2.9 billion for the year and $83.1 billion in revenue despite the Q4 loss, according to the company’s earnings report. Executives said the insurer braced for headwinds related to COVID-19 during the year and also saw disappointing growth in new Medicare Advantage members.
As a result, Humana has kicked off a $1 billion value creation effort to reinvest in its core MA business in hopes of bouncing back from the underwhelming enrollment during the annual period.
Centene has been conducting a similar project throughout the year in an effort to streamline its operations.
Anthem and Cigna fall in the middle of the pack, according to our review. They both reported about $1.1 billion in profit for Q4, though Cigna was ahead with $45.7 billion in revenue.
Cigna reported $174.1 billion in revenue and $5.4 billion in profit for the year, and on its earnings call noted that a major growth opportunity moving forward its Evernorth subsidiary, which includes a slew of businesses such as Express Scripts, Accredo and MDLive.
Anthem earned $6.1 billion in profit on $138.6 billion in revenue for the year, and executives shrugged off concerns about the Medicare Advantage market, saying its performance in open enrollment met expectations. In addition, it’s seeing growth at its in-house pharmacy benefit manager, IngenioRx, as it expands clientele.
34 states where child care costs more than college tuition

The annual expense of child care for an infant exceeds the annual cost of in-state tuition at a public four-year university in 34 states, according to the most recent data from the Economic Policy Institute.
At this point in the pandemic, healthcare is among the top three industries when it comes to people quitting or changing jobs. The quality and cost of child care is top of mind for healthcare decision-makers given its strength as a determining factor to push people from the U.S. labor force. Mothers continue to shoulder the majority of family caregiving responsibilities, making child care a heavier tip of the scale for healthcare, where women make up the majority of the front-line workforce (66 percent) and managers (59 percent), according to research from McKinsey.
Infant care expenses exceed college tuition in 34 states and Washington, D.C. Below is each state ranked by how much infant care costs exceed or compare to the cost of tuition at a four-year public university, along with the median family income in each state and infant care as a share of income.






